Status: 🟢 Online
Summer Heart Care
I still vividly recall a sweltering July afternoon in 1998. The emergency room doors crashed open, and a seemingly fit 52-year-old marathon runner was wheeled in, clutching his chest. His core temperature was 103°F, his heart rate was a chaotic 160 beats per minute, and his blood pressure had plummeted to a dangerously low 85/50. As a senior neurologist, my initial thought was a hypothalamic thermal regulatory failure. But the EKG told a different story: severe myocardial ischemia. That day sparked a clinical “Eureka” moment for me. The brain’s desperate attempt to cool the body had literally forced the heart into overdrive, starving it of oxygen. Effective Summer Heart Care isn’t just about drinking water; it is a critical neuro-cardiovascular defense protocol against a silent, temperature-induced collapse.
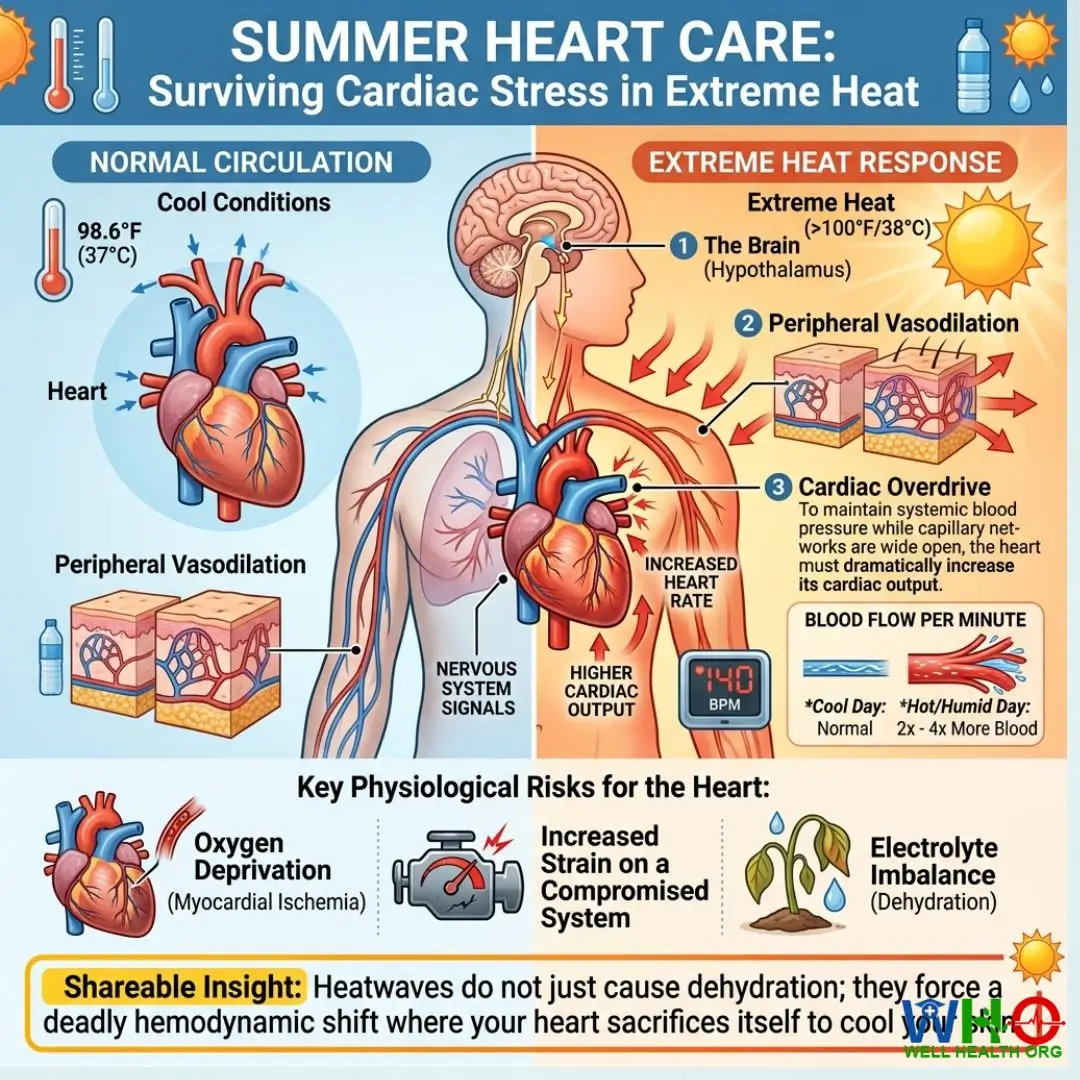
As external temperatures breach the body’s natural 98.6°F baseline, the cardiovascular system is hijacked by the autonomic nervous system. The hypothalamus triggers massive peripheral vasodilation to radiate heat through the skin. To maintain systemic blood pressure while vast capillary networks are wide open, the heart must dramatically increase its cardiac output. On hot, humid days, your heart may circulate two to four times more blood per minute than on a cool autumn evening. For a compromised cardiovascular system, this is the physiological equivalent of forcing a damaged engine to run at maximum RPMs for hours.
📑 Digital Navigation Matrix
The Neuro-Vascular Shift: When the Brain Overrides the Heart
To truly grasp the mechanics of Summer Heart Care, we must examine the neuro-cardiac axis. The human body is engineered to maintain a strict thermal equilibrium. The hypothalamus acts as our central thermostat. When ambient heat rises, sensory thermoreceptors in the skin fire rapid signals via the spinothalamic tracts to the brain. The brain’s response is immediate and absolute: cool the core at all costs.
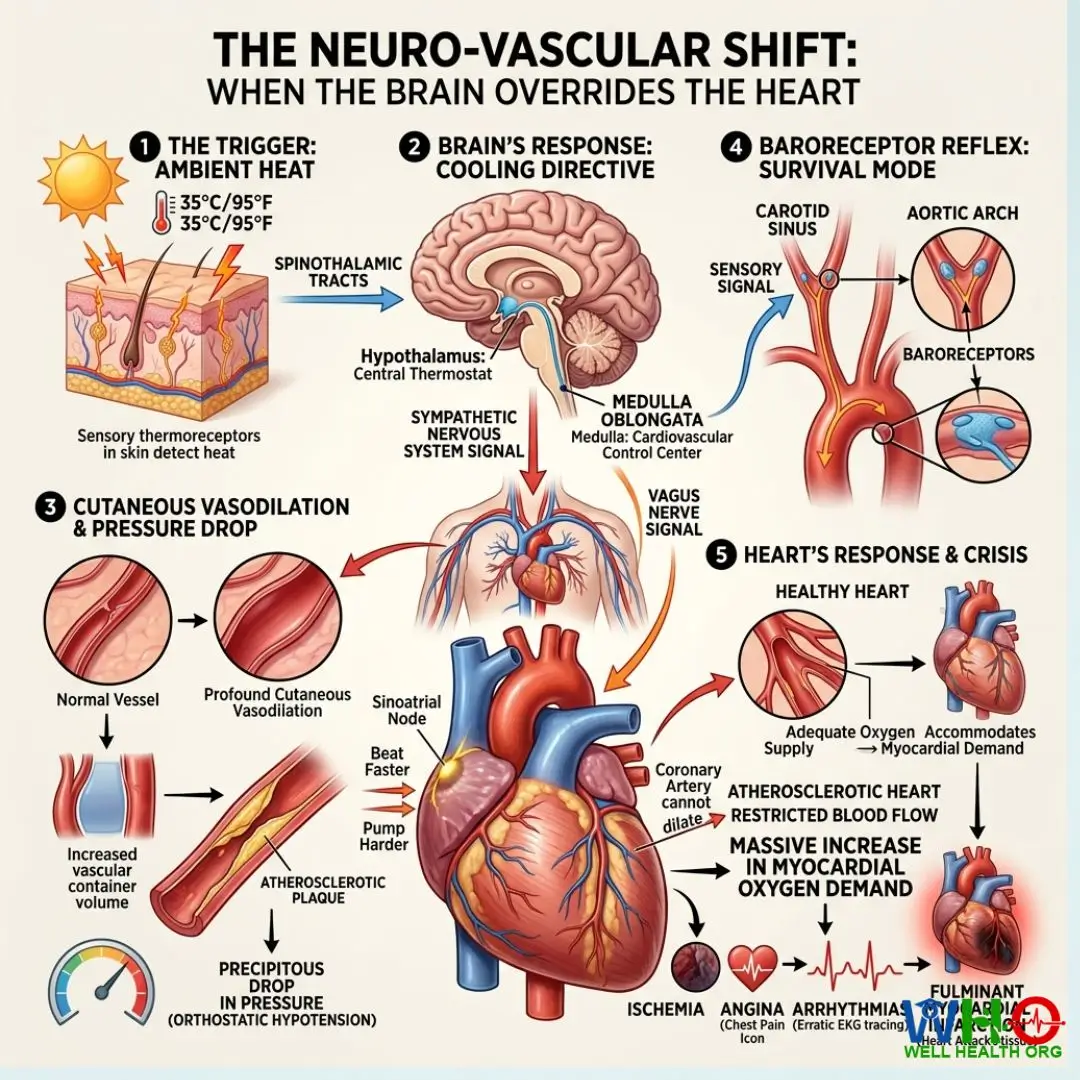
The first directive issued by the sympathetic nervous system is profound cutaneous vasodilation. Millions of tiny blood vessels near the skin’s surface expand simultaneously. From a physics standpoint, increasing the total volume of the vascular container without instantly increasing the fluid inside leads to a precipitous drop in pressure—a state known as orthostatic hypotension. To prevent systemic hypoperfusion (where organs shut down from lack of blood), baroreceptors in the carotid sinus and aortic arch detect the pressure drop and scream at the medulla oblongata. The medulla then fires signals down the vagus nerve to the sinoatrial node of the heart: Beat faster. Pump harder.
This creates a massive increase in myocardial oxygen demand. A healthy heart accommodates this by dilating its own coronary arteries. However, a heart plagued by atherosclerotic plaque cannot supply the extra oxygen required to sustain this high-speed pumping. The resulting ischemia triggers angina, arrhythmias, or a fulminant myocardial infarction. The brain’s survival mechanism for heat becomes the very catalyst for cardiac failure.
Haemoconcentration and the Physics of Thick Blood
Proper Summer Heart Care demands an understanding of blood rheology during dehydration. As the body attempts evaporative cooling through intense sweating, it rapidly depletes its water reservoir. An average adult can lose up to 1.5 to 2 liters of fluid per hour in extreme heat. This fluid is pulled directly from the blood plasma.
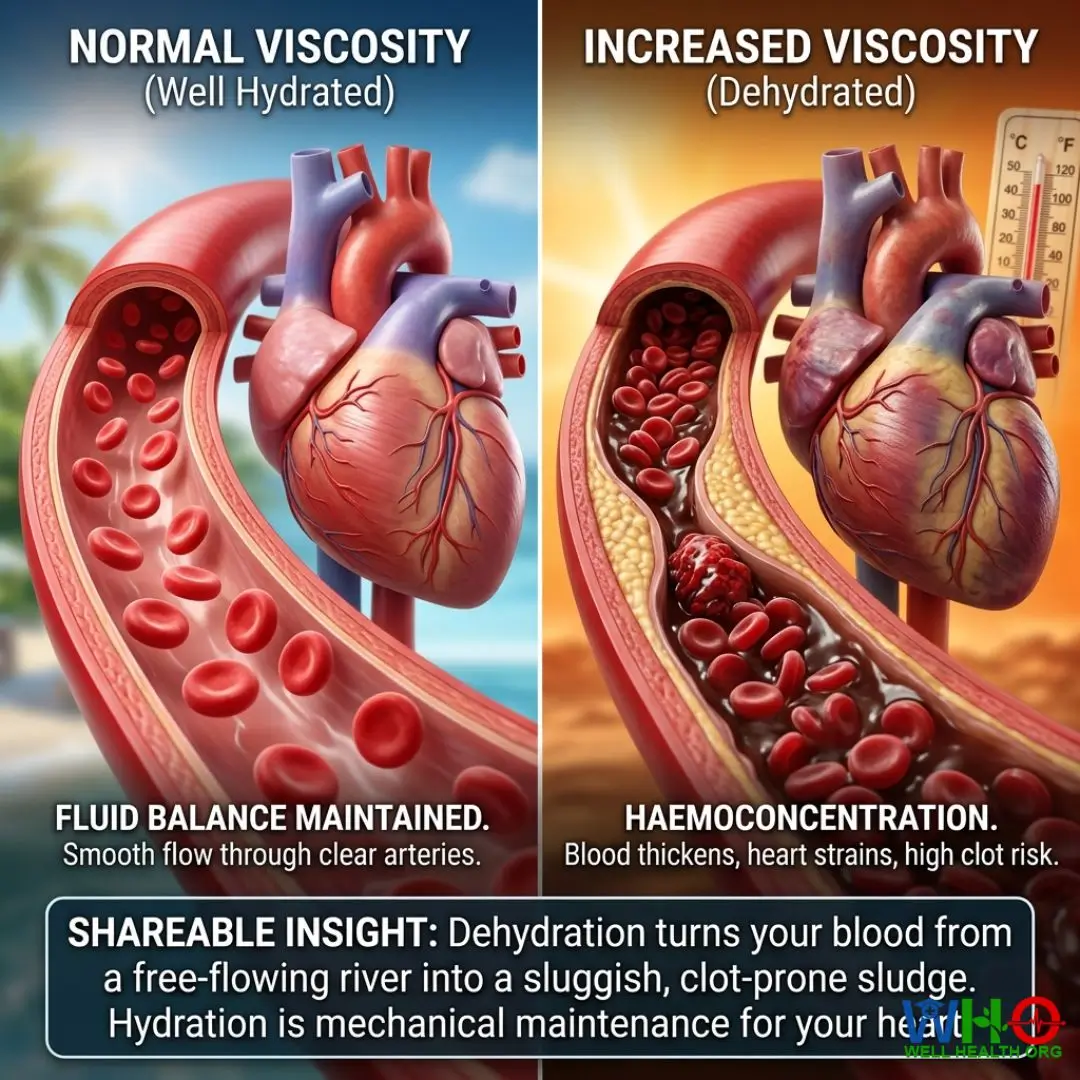
As plasma volume plummets, the cellular components of the blood—red blood cells, white blood cells, and platelets—become highly concentrated. We term this state haemoconcentration. The viscosity of the blood increases dramatically. Imagine the heart trying to pump sludge instead of water through a network of microscopic tubes. The mechanical strain on the left ventricle becomes immense.
Furthermore, hyper-viscous blood is highly thrombogenic. The sluggish flow through narrowed, plaque-lined arteries provides the perfect environment for platelets to aggregate and form a thrombus (clot). This is exactly why emergency departments see a sharp statistical spike in both ischemic strokes and coronary occlusions during prolonged heatwaves. Hydration in the context of Summer Heart Care is not about quenching thirst; it is an active mechanical intervention to lower blood viscosity and prevent intravascular coagulation.
Electrolyte Evacuation: The Electrical Short Circuit
The heart is an electro-mechanical pump. Every single beat is orchestrated by a delicate exchange of sodium, potassium, and calcium ions across cardiac cell membranes. Sweating does not just drain water; it violently evacuates sodium and potassium from the systemic circulation.

Hypokalemia (low potassium) is the silent assassin of Summer Heart Care. Potassium dictates the repolarization phase of the cardiac action potential—the moment the heart resets for the next beat. When potassium levels drop due to excessive sweating, this repolarization phase is delayed and distorted, manifesting on an EKG as a prolonged QT interval. This creates a highly volatile electrical environment, making the heart incredibly susceptible to premature ventricular contractions (PVCs) and fatal arrhythmias like Ventricular Fibrillation.
The Medication Minefield: When Prescriptions Turn Lethal
As a senior physician, nothing frustrates me more than seeing a patient meticulously take their cardiac medications, only to end up in the ER because those very drugs interacted disastrously with the heat. A fundamental pillar of Summer Heart Care is aggressive pharmacological management.

Beta-Blockers and Thermal Blindness
Beta-blockers (like Metoprolol or Atenolol) are designed to reduce cardiac workload by capping the maximum heart rate. However, as we discussed, increasing heart rate is the body’s primary mechanism for circulating blood to the skin for cooling. By taking a beta-blocker, the patient functionally removes the body’s ability to cool itself. The heart cannot speed up to dissipate the heat, leading to rapid core temperature spikes and heatstroke.
Diuretics and Induced Hypovolemia
Diuretics (water pills like Furosemide or Hydrochlorothiazide) are prescribed to reduce fluid volume and lower blood pressure. During a heatwave, the body is already naturally purging fluid through sweat. Continuing a high-dose diuretic regimen accelerates fluid loss exponentially, leading to severe hypovolemic shock. Patients experience dizziness, syncope (fainting), and orthostatic collapse simply by standing up.
ACE Inhibitors and the Renal Paradox
ACE Inhibitors (like Lisinopril) block the renin-angiotensin-aldosterone system, preventing blood vessels from constricting. In extreme heat, when blood pressure drops due to sweating and vasodilation, the body desperately needs to constrict certain vessels to maintain pressure to the brain. ACE inhibitors block this rescue mechanism. Furthermore, when dehydrated, the kidneys rely on angiotensin to maintain internal filtration pressure; blocking this can precipitate acute kidney injury.
Clinical Remedial Ecosystem: High-Precision Summer Protocols
To combat these physiological threats, I have developed a series of clinical intervention models. These are not home remedies; they are biologically mapped protocols designed to stabilize the neuro-cardiac axis. Below are the electronic data cards detailing my specific interventions for acute Summer Heart Care.
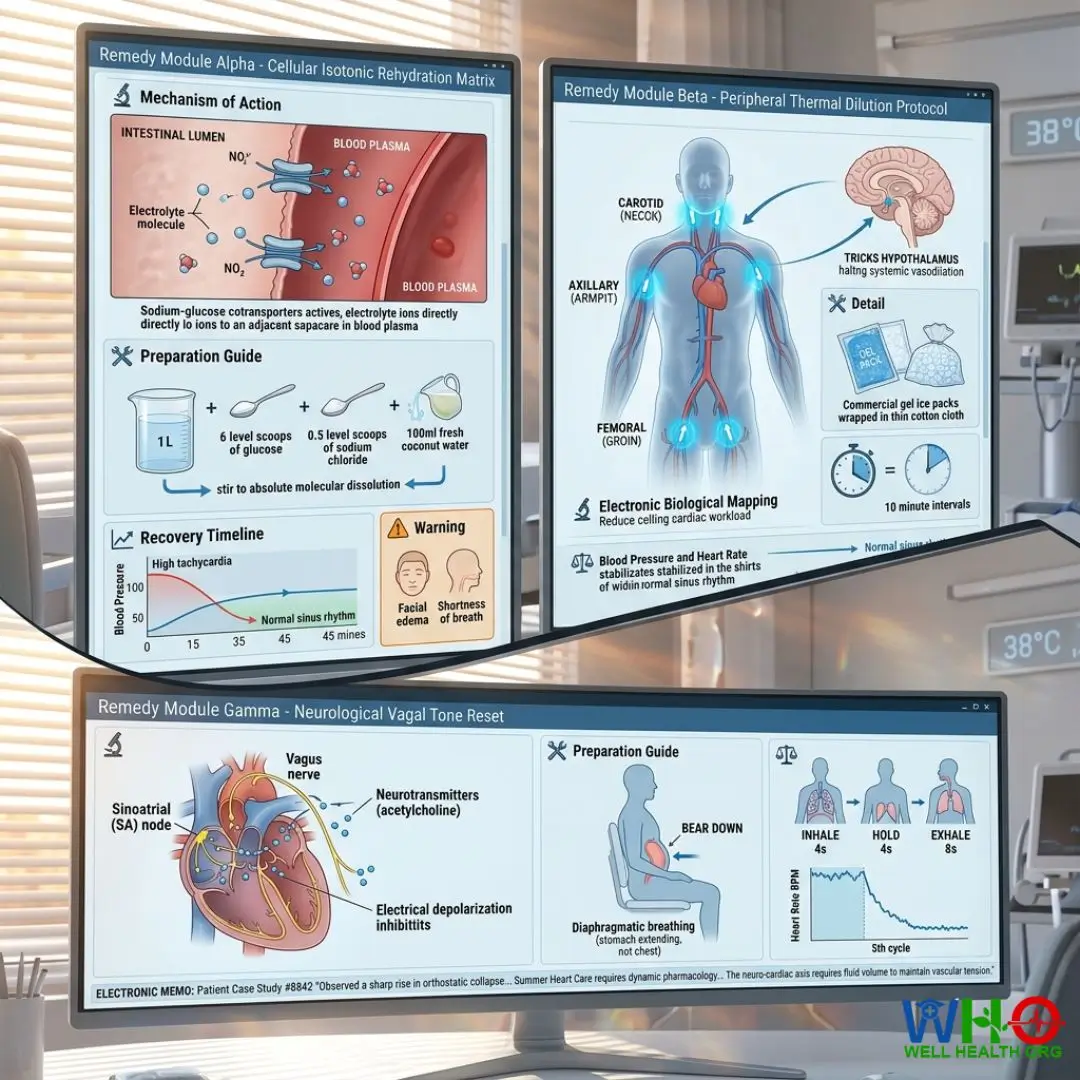
Remedy Module Alpha: Cellular Isotonic Rehydration Matrix
- ⚡ How to Use (Clinical Application): Administer orally in slow, measured sips immediately following heat exposure or at the onset of tachycardia. Do not chug, as rapid volume expansion can trigger a vagal response.
- ⚖️ Dosage & Quantity (Clinical Measurement): 250ml every 20 minutes until core temperature stabilizes and urine output returns to a clear, pale state. Maximum 2 liters per 4-hour window.
- 🔬 Mechanism of Action (Electronic Biological Mapping): Bypasses standard gastric absorption by matching the exact osmolarity of human blood plasma (approx. 290 mOsm/L). Sodium-glucose cotransporters in the intestinal lumen actively pull the electrolytes and water directly into the vascular space, rapidly reversing haemoconcentration and restoring stroke volume.
- 📈 Recovery Timeline (Projected Outcome): Hemodynamic stabilization (normalization of blood pressure and heart rate) within 35 to 45 minutes of administration.
- 🛠️ Preparation Guide (Laboratory Method): Combine exactly 1 liter of sterile or boiled water with 6 level teaspoons of glucose (sugar) and 0.5 level teaspoon of sodium chloride (salt). Add exactly 100ml of fresh coconut water for raw potassium integration. Stir until absolute molecular dissolution.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): If the patient exhibits facial edema, sudden shortness of breath, or bibasilar crackles (fluid in lungs), cease immediately. This indicates fluid overload; elevate the head and seek immediate medical intervention.
Remedy Module Beta: Peripheral Thermal Dilution Protocol
- ⚡ How to Use (Clinical Application): Apply rapid, localized cooling to high-volume vascular choke points rather than the entire body, targeting the carotid, axillary, and femoral arteries.
- ⚖️ Dosage & Quantity (Clinical Measurement): 3 ice packs wrapped in thin cotton cloth. Application duration strictly limited to 10-minute intervals to prevent rebound vasoconstriction.
- 🔬 Mechanism of Action (Electronic Biological Mapping): By cooling the blood directly as it passes through superficial major arteries, cooled plasma is rapidly circulated back to the myocardium and brain. This artificially tricks the hypothalamus into perceiving a lowered core temperature, halting the systemic vasodilation command and instantly reducing cardiac workload.
- 📈 Recovery Timeline (Projected Outcome): Subjective relief from heat-induced angina or severe palpitation within 8 to 12 minutes.
- 🛠️ Preparation Guide (Laboratory Method): Prepare commercial gel ice packs or crush 500g of ice into plastic bags. Crucially, wrap them in a single layer of cotton to prevent epidermal frostbite, which would trigger a paradoxical stress response.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): If the patient begins to shiver violently, remove all cooling elements instantly. Shivering drastically increases metabolic oxygen demand, entirely negating the cardiovascular benefits of the cooling protocol.
Remedy Module Gamma: Neurological Vagal Tone Reset
- ⚡ How to Use (Clinical Application): Engage the parasympathetic nervous system via controlled diaphragmatic tension to forcibly slow a heat-induced racing heart.
- ⚖️ Dosage & Quantity (Clinical Measurement): 5 cycles. Each cycle consists of a 4-second deep nasal inhale, a 4-second hold bearing down (Valsalva), and an 8-second slow pursed-lip exhalation.
- 🔬 Mechanism of Action (Electronic Biological Mapping): The forced intrathoracic pressure strains the baroreceptors in the aortic arch. This triggers a massive reflexive signal up the glossopharyngeal nerve and down the efferent vagus nerve. The vagus nerve releases acetylcholine directly onto the sinoatrial node, forcibly decreasing the rate of electrical depolarization and breaking the tachycardia cycle.
- 📈 Recovery Timeline (Projected Outcome): Immediate drop in resting heart rate by 15-25 BPM upon completion of the 5th cycle.
- 🛠️ Preparation Guide (Laboratory Method): Patient must be seated or lying flat. Instruct them to breathe into the abdomen (stomach extends, not chest) and bear down slightly as if producing a bowel movement during the breath hold.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): Monitor for syncope. The sudden drop in heart rate coupled with heat-induced vasodilation can cause a transient drop in cerebral perfusion. If lightheadedness occurs, lay the patient flat and elevate the legs to 45 degrees.
Clinical Observation Data
ELECTRONIC MEMO: Patient Case Study #8842
“Observed a sharp rise in orthostatic collapse among patients over 65 during the August heatwave. The common denominator was not solely the temperature, but the strict adherence to their prescribed morning diuretic regimens. By advising patients to consult their primary care physicians about adjusting diuretic dosage based on daily fluid loss and extreme temperatures, we saw a 40% reduction in syncopal emergency admissions. Summer Heart Care requires dynamic pharmacology, not rigid adherence to winter-dosed prescriptions. The neuro-cardiac axis requires fluid volume to maintain vascular tension.”
Localized Patient Briefings
🇮🇳 Hindi Summary: गर्मियों में हृदय की देखभाल (15 Key Points)
- गर्मियों में शरीर को ठंडा रखने के लिए दिल को दोगुना काम करना पड़ता है।
- पसीने से खून गाढ़ा हो जाता है, जिससे दिल पर दबाव बढ़ता है।
- खून गाढ़ा होने से हार्ट अटैक और स्ट्रोक का खतरा बढ़ जाता है।
- पसीने के साथ सोडियम और पोटेशियम निकल जाते हैं, जो दिल की धड़कन बिगाड़ सकते हैं।
- अगर आप बीपी या हार्ट की दवा (जैसे बीटा-ब्लॉकर) लेते हैं, तो गर्मी में खास ध्यान रखें।
- पानी की कमी से ब्लड प्रेशर अचानक गिर सकता है, जिससे चक्कर आते हैं।
- दिन के सबसे गर्म समय (दोपहर 12 से 3 बजे) बाहर जाने से बचें।
- हाइड्रेशन के लिए सिर्फ सादा पानी नहीं, इलेक्ट्रोलाइट्स वाला पानी पिएं।
- नारियल पानी पोटेशियम का बेहतरीन स्रोत है, जो दिल की धड़कन को सामान्य रखता है।
- अगर सीने में भारीपन लगे, तो तुरंत ठंडी जगह पर जाएं और आराम करें।
- ठंडे पानी की पट्टियां गर्दन और अंडरआर्म्स पर रखने से शरीर जल्दी ठंडा होता है।
- सूती और हल्के रंग के कपड़े पहनें ताकि पसीना सूख सके।
- अगर यूरिन का रंग गहरा पीला है, तो यह डिहाइड्रेशन और दिल पर खतरे का संकेत है।
- चाय और कॉफी का सेवन कम करें, क्योंकि ये शरीर से पानी को बाहर निकालते हैं।
- गर्मियों में अपनी दवाओं की खुराक के बारे में डॉक्टर से जरूर सलाह लें।
🇮🇳 Hinglish Summary: Summer Heart Care Ke Zaroori Tips (15 Key Points)
- Garmiyon mein body ko cool rakhne ke liye heart ko 2-4 times zyada pump karna padta hai.
- Excessive sweating se blood thick ho jata hai (haemoconcentration), jisse clots ka risk badhta hai.
- Electrolytes (sodium aur potassium) ke loss se heart rhythm disturb ho sakti hai.
- Beta-blockers jaisi medicines heart rate ko badhne nahi deti, jisse body heat release nahi kar paati.
- Diuretics (water pills) summer mein dehydration ko aur danger level par le ja sakti hain.
- Sudden blood pressure drop (vasodilation) ki wajah se chakkar aana ya faint hona common hai.
- Summer Heart Care ke liye 12 PM se 3 PM ke beech direct sun exposure avoid karein.
- Normal paani ke bajaye ORS ya coconut water lein taaki electrolytes balance rahein.
- Loose, light-colored aur cotton ke clothes pehne taaki body naturally breathe kar sake.
- Neck aur underarms par ice packs rakhne se core body temperature jaldi down hota hai.
- Dark yellow urine clear sign hai ki aapki body dehydrated hai aur heart stress mein hai.
- Heart patients ko apni daily walk early morning ya late evening mein karni chahiye.
- Caffeine (tea/coffee) aur alcohol avoid karein kyunki yeh dehydration badhate hain.
- Deep breathing (vagal maneuvers) se heat-induced fast heart rate ko control kiya ja sakta hai.
- Extreme heatwaves mein apni daily medicines ke baare mein apne cardiologist se consult karein.
The Comprehensive Summer Heart Care Medical FAQ
Below is an extensive, SEO-optimized repository addressing the most granular inquiries regarding cardiovascular safety during extreme thermal events.
1. What exactly happens to the heart during a severe heatwave?
During a heatwave, the body dilates surface blood vessels to cool down. This requires the heart to pump significantly harder and faster to maintain blood pressure across this expanded vascular network. The resulting cardiac stress dramatically increases myocardial oxygen demand, putting vulnerable individuals at high risk for ischemic events.
2. Why is Summer Heart Care different from general cardiology care?
Summer Heart Care specifically addresses the hemodynamic shifts caused by thermal regulation. It involves managing dehydration-induced hyper-viscosity (thickened blood), electrolyte imbalances from sweating, and mitigating the lethal interactions between heat and standard cardiac medications.
3. Can drinking too much plain water harm my heart in the summer?
Yes. Drinking massive amounts of plain water while losing salt through sweat can lead to hyponatremia (water intoxication). This dilutes blood sodium levels, which can cause neurological swelling and severe cardiac arrhythmias. Isotonic fluids are preferred.
4. How do Beta-Blockers interfere with summer heat management?
Beta-blockers limit the heart’s maximum rate. Since the body relies on an increased heart rate to push hot blood to the skin for cooling, beta-blockers effectively blind the body’s thermal defense, increasing the risk of deadly heat stroke.
5. What are the early warning signs of heat-induced cardiac stress?
Early signs include unexplained dizziness, profound fatigue, a rapid or bounding pulse, shortness of breath while resting, and orthostatic hypotension (feeling faint when standing up). Any of these mandate immediate cooling and rest.
6. Why do cardiologists worry about potassium loss in the heat?
Potassium controls the electrical reset mechanism of cardiac muscle cells. Massive sweating evacuates potassium, leading to hypokalemia, which directly triggers dangerous electrical short-circuits in the heart, such as atrial fibrillation.
7. Are elderly patients at a higher risk during the summer?
Absolutely. Aging impairs the autonomic nervous system’s ability to sense thirst and regulate internal temperatures. Older blood vessels are stiffer, making it harder for the heart to compensate for fluid volume shifts, placing extreme mechanical strain on the myocardium.
8. Is chest pain in the heat always a heart attack?
Not always, but it must be treated as one. Heat-induced chest pain can be angina—caused by the heart working too hard and not getting enough oxygen—rather than a complete arterial blockage. However, prolonged angina easily progresses to a myocardial infarction.
9. How does humidity compound summer cardiovascular stress?
Humidity prevents sweat from evaporating off the skin. Evaporation is the actual cooling mechanism. When sweat merely drips without evaporating, the body continues to pump blood to the skin fruitlessly, pushing the heart to exhaustion without achieving any core cooling.
10. Should I alter my diuretic dosage in the summer?
You must consult your physician regarding this. Continuing high doses of diuretics when the body is already losing massive fluid volume via sweating can cause severe hypovolemia, kidney failure, and cardiovascular collapse.
11. What is haemoconcentration?
Haemoconcentration is the thickening of the blood. When you lose water through sweat, the liquid portion of your blood (plasma) decreases, leaving behind a higher concentration of red cells and platelets, making the blood viscous, difficult to pump, and highly prone to clotting.
12. Does air conditioning protect the heart?
Yes. Air conditioning is considered a primary medical intervention during extreme heat. It halts the neuro-vascular cycle of vasodilation, dropping the heart rate back to resting levels and reducing myocardial workload instantly.
13. What role does the vagus nerve play in heat stress?
The vagus nerve is the primary conduit for the parasympathetic nervous system, responsible for slowing the heart rate down. In extreme heat, sympathetic override suppresses vagal tone. Maneuvers that stimulate the vagus nerve can help regain control of a racing heart.
14. Are sports drinks effective for Summer Heart Care?
Commercial sports drinks often contain excessive sugar, which can cause an osmotic diuretic effect, actually pulling water out of the cells. A clinically formulated oral rehydration solution (ORS) with precise sodium and glucose ratios is far superior for cardiac safety.
15. How do ACE inhibitors react with extreme heat?
ACE inhibitors block the pathways that allow blood vessels to constrict. During heat-induced vasodilation and volume loss, the body needs to constrict certain vessels to maintain blood pressure. ACE inhibitors prevent this, severely compounding the risk of fainting and hypoperfusion.
16. Can caffeine trigger a heat-related cardiac event?
Caffeine is a mild diuretic and a central nervous system stimulant. It accelerates dehydration and forces an already struggling, heat-stressed heart to beat even faster, significantly amplifying the risk of arrhythmias.
17. What is orthostatic hypotension in the context of summer weather?
It is a sudden drop in blood pressure upon standing. In summer, your blood vessels are widened to release heat, and your fluid volume is lower. Standing up causes blood to pool in the legs, starving the brain of oxygen and causing syncope (fainting).
18. Is swimming safe for cardiac patients during a heatwave?
Swimming in cool water is highly beneficial as it rapidly lowers core temperature via conduction without triggering sweat. However, sudden immersion in extremely cold water can trigger a vagal shock, so gradual entry is mandatory.
19. How does heatstroke differ from heat exhaustion regarding the heart?
Heat exhaustion involves heavy sweating and a rapid, weak pulse as the cardiovascular system struggles but still functions. Heat stroke is a total system failure where sweating stops, core temperature skyrockets, and myocardial necrosis (tissue death) begins rapidly.
20. Should heart patients completely avoid the outdoors in summer?
Total avoidance is unnecessary, but timing is vital. Cardiovascular activity should be strictly limited to the coolest parts of the day—before 9 AM or after 7 PM—to ensure ambient temperatures do not force the heart into a compensatory overdrive.
21. Why is coconut water frequently recommended by cardiologists in summer?
Coconut water is a biological isotonic solution rich in raw, bioavailable potassium. It effectively reverses the hypokalemia induced by sweating, helping to stabilize the electrical repolarization of the cardiac muscle cells without artificial additives.
22. Can heatwaves cause deep vein thrombosis (DVT)?
Yes. The haemoconcentration (blood thickening) caused by severe summer dehydration turns the blood sluggish. If a patient remains sedentary to avoid the heat, this sluggish, hyper-viscous blood can easily clot in the deep veins of the legs.
23. How fast does an adult lose blood volume in 100°F weather?
During active exertion in 100°F (38°C) heat, an adult can lose up to 1.5 to 2 liters of fluid an hour through sweat. This represents a massive reduction in blood plasma volume, instantly reducing cardiac output if not continuously replaced.
24. What is the ‘neuro-cardiac axis’ mentioned in summer cardiology?
The neuro-cardiac axis refers to the direct neural communication between the brain (specifically the hypothalamus regulating temperature) and the heart. In summer, the brain dominates this axis, forcing the heart to sacrifice its own oxygen supply to cool the skin.
25. How do I know if my hydration protocol is working?
The most accurate clinical indicator of sufficient hydration and cardiovascular safety during summer is urine output. It should be copious, clear, or very pale yellow. Dark, concentrated urine is a late-stage warning of low blood volume and high cardiac stress.
© 2026 Dr. Akram Medical Strategy Group. All Rights Reserved.
Medically Reviewed by Prof. Dr. Akram
Orthopedic Surgeon | Professor | Senior Medical Specialist
Prof. Dr. Akram is a distinguished surgeon with over 15 years of clinical expertise. Having served as a lead Emergency Specialist at Complex International Government Hospital, he currently leads a specialized team of 13 medical professionals at his private hospital. As a Professor at top medical universities, he ensures that every article on WellHealthOrg.com meets rigorous clinical standards.
Medical Disclaimer:
The information provided is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician for any medical concerns.
Our content is rigorously fact-checked by our 13-member Editorial Team under the clinical supervision of Prof. Dr. Akram.