● Status: Online | Chief Medical Content Strategist & Senior Neurologist
Summer Food Poisoning: How to Identify and Treat Stomach Infections at Home
Summer food poisoning strikes fast when the mercury rises, triggering a cascade of gastrointestinal distress that demands rapid, strategic hydration. As the temperature crosses the critical 90°F threshold, an innocent potato salad left on a picnic table becomes a microscopic battlefield. Bacterial replication rates explode, doubling every twenty minutes.

I remember a sweltering July afternoon during my third year as an attending physician. A young marathon runner was wheeled into the ER. His heart rate was 130 BPM, and his blood pressure was crashing. He hadn’t been running; he had attended a family barbecue. He assumed his severe abdominal cramps and relentless vomiting were just a “stomach bug” and tried to sleep it off. He was entering hypovolemic shock due to acute summer food poisoning. That case cemented a clinical truth in my mind: gastroenteritis in the heat is a neurological and vascular emergency masquerading as a simple stomach ache.
Shareable Insight: “Vomiting is not a stomach defect; it is a brilliant neurological defense mechanism. Your brain is aggressively purging neurotoxins before they can breach the blood-brain barrier.”
As a neurologist, my perspective on summer food poisoning differs from a standard gastroenterologist. When you ingest a pathogen like Staphylococcus aureus or Salmonella, the bacteria release enterotoxins. Your enteric nervous system—often called the second brain—detects these toxins immediately. It fires high-voltage electrical signals up the vagus nerve directly to the medulla oblongata, specifically targeting the area postrema (the brain’s vomiting center). The resulting emesis (vomiting) is your brain prioritizing your survival over your comfort.
Interactive Clinical Index
The Neuro-Gut Axis of Intoxication
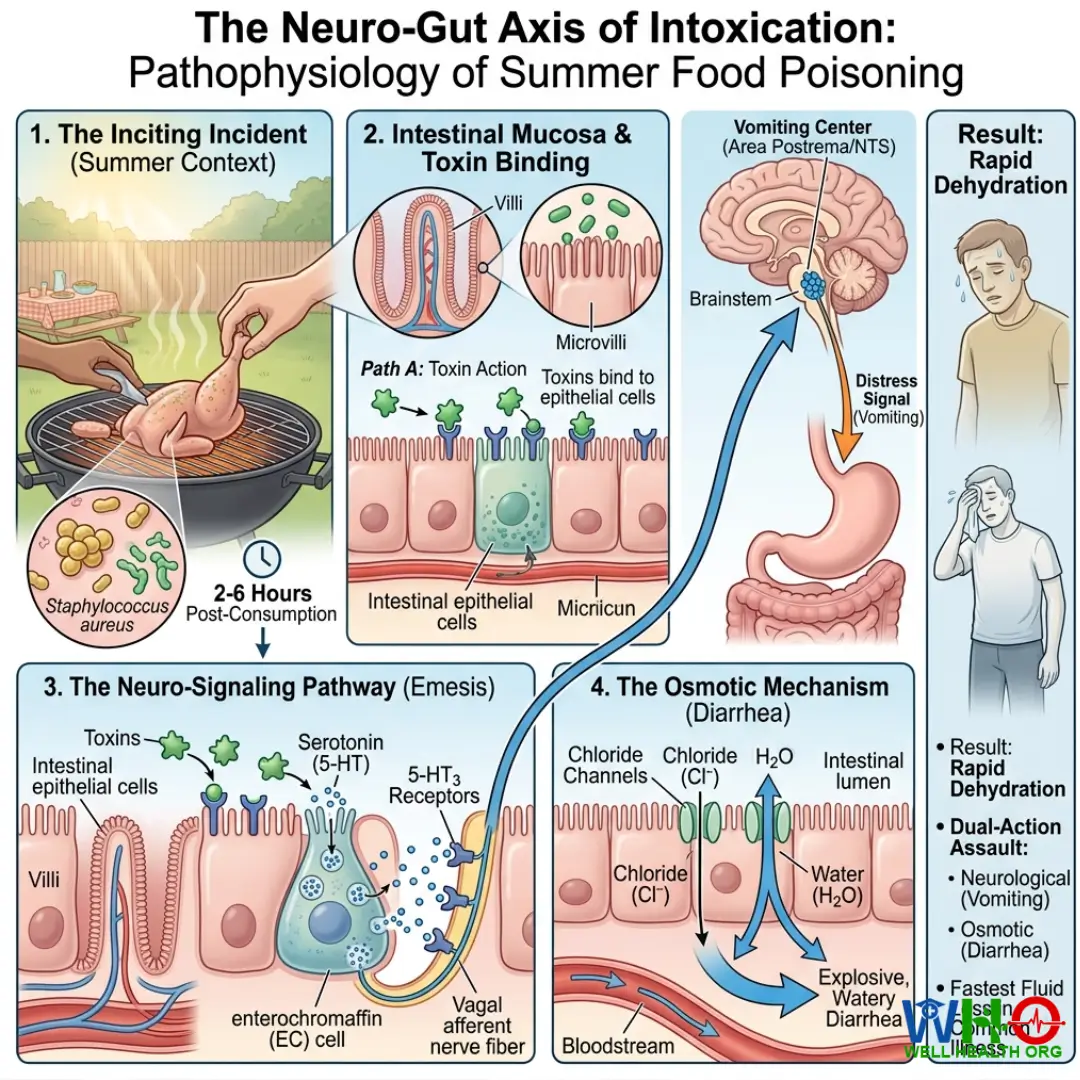
To effectively treat summer food poisoning, we must understand the pathophysiology. When temperatures soar, the protective barriers in our food chain weaken. Let us dissect the timeline of a typical infection. You consume a tainted piece of undercooked meat. Within two to six hours, the pre-formed toxins bind to the epithelial cells of your intestinal mucosa. This binding triggers the release of serotonin (5-HT) from enterochromaffin cells. The serotonin binds to 5-HT3 receptors on vagal afferent nerve fibers, sending a massive distress signal to the brainstem.
Simultaneously, the toxins force open chloride channels in your intestinal lining. Water follows salt. Fluid is rapidly pulled from your bloodstream into your bowels, causing explosive, watery diarrhea. This dual-action assault—neurological vomiting and osmotic diarrhea—is why summer food poisoning causes dehydration faster than almost any other common illness.
Pathogen Profiling: The “Danger Zone”
Bacteria thrive in the “Danger Zone”—temperatures between 40°F (4°C) and 140°F (60°C). During summer, outdoor ambient temperatures sit squarely in the upper quadrant of this zone. A dish left out at 90°F provides the perfect incubator. Let us review the primary culprits of summer food poisoning:

- Staphylococcus aureus: This bacteria produces toxins rapidly in mayo-based salads and dairy. Symptoms (intense nausea and vomiting) appear incredibly fast, often within 30 minutes to 6 hours.
- Salmonella: Found in undercooked poultry and raw eggs. The incubation period is 6 hours to 6 days. It causes severe abdominal cramps, fever, and diarrhea.
- Campylobacter: Frequently linked to raw chicken. It can trigger a secondary neurological complication known as Guillain-Barré syndrome if left unchecked.
- E. coli (STEC): Contracted from undercooked beef or contaminated raw produce (like lettuce). It is notorious for causing bloody diarrhea and requires immediate medical observation.
Differential Diagnosis: Summer Food Poisoning vs. Norovirus (Stomach Flu)
Patients constantly ask me how to tell the difference. Summer food poisoning presents with intense, sudden gastrointestinal distress localized strictly to the gut, highly correlated with a specific meal. The “stomach flu” (Norovirus), while causing similar GI symptoms, is systemic. Norovirus is highly contagious person-to-person and frequently presents with generalized muscle aches (myalgia), chills, and a low-grade fever before the vomiting even begins.
Clinical Remedial Ecosystem
Treating summer food poisoning at home is an exercise in precise fluid mechanics and targeted symptom management. The following interventions are designed to stop hypovolemia, soothe the inflamed enteric nervous system, and restore electrolyte balance safely.

MODULE 01: High-Osmolarity Oral Rehydration Therapy (ORS)
Clinical Objective: Reverse vascular fluid depletion and correct cellular sodium-potassium imbalance caused by sudden emesis and diarrhea.
- ⚡ How to Use (Clinical Application): Do not chug fluids. The inflamed stomach will instantly reject large volumes. Administer via the “micro-dosing” method: 1 tablespoon (15 ml) every 5 minutes.
- ⚖️ Dosage & Quantity (Clinical Measurement): Aim for 2 liters of ORS solution over a 12-hour period for adults. For children, follow weight-based pediatric guidelines (typically 50 ml per kg of body weight over 4 hours).
- 🔬 Mechanism of Action (Electronic Biological Mapping): Pure water lacks the sodium required to open the sodium-glucose cotransporter (SGLT1) in the intestinal lining. ORS provides precise ratios of glucose and sodium, forcing the cellular gates open and pulling water back into the bloodstream via osmosis.
- 📈 Recovery Timeline (Projected Outcome): Urine should transition from dark amber to pale yellow within 6 to 8 hours of consistent ORS administration.
- 🛠️ Preparation Guide (Laboratory Method): Dissolve 6 level teaspoons of sugar and 1/2 level teaspoon of salt into 1 liter of safe, sterile drinking water. Stir until completely dissolved.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): If the patient vomits the ORS immediately upon ingestion three times consecutively, abandon oral hydration and seek intravenous (IV) fluids at an emergency department.
MODULE 02: The Modified BRAT Protocol
Clinical Objective: Reintroduce caloric load without triggering the hyper-reactive gastrocolic reflex.
- ⚡ How to Use (Clinical Application): Initiate this protocol strictly after a minimum of 4 hours of zero emesis. Begin with a single bite of toast or mashed banana.
- ⚖️ Dosage & Quantity (Clinical Measurement): 1/4 cup of bland food material every 2 to 3 hours. Do not force consumption.
- 🔬 Mechanism of Action (Electronic Biological Mapping): Bananas provide vital potassium lost during diarrhea. Rice and Toast offer simple, low-fiber carbohydrates that require minimal enzymatic breakdown, giving the pancreatic and biliary systems time to rest. Applesauce contains pectin, a soluble fiber that adds bulk to liquid stools.
- 📈 Recovery Timeline (Projected Outcome): Stool consistency should begin to normalize within 24 to 48 hours of starting the protocol.
- 🛠️ Preparation Guide (Laboratory Method): Mash one ripe banana until smooth. Serve with plain white rice boiled in clear chicken or vegetable broth to maximize electrolyte retention. Avoid all butter, dairy, or spices.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): If introducing solid food triggers severe, doubling-over abdominal cramps, revert to a strictly liquid diet for another 12 hours. The mucosal lining is not yet ready for mechanical digestion.
MODULE 03: Targeted Bismuth Subsalicylate Intervention
Clinical Objective: Chemical binding of enterotoxins and reduction of gut mucosal inflammation.
- ⚡ How to Use (Clinical Application): Administer orally using standard over-the-counter preparations (e.g., Pepto-Bismol) to combat active, non-bloody diarrhea.
- ⚖️ Dosage & Quantity (Clinical Measurement): For adults: 524 mg (two tablets or 30 mL liquid) every 30 to 60 minutes as needed, up to a maximum of 8 doses in 24 hours.
- 🔬 Mechanism of Action (Electronic Biological Mapping): The bismuth compound exhibits mild antimicrobial properties, actively binding to enterotoxins produced by E. coli and Salmonella. The subsalicylate component acts as a potent local anti-inflammatory, slowing hyper-motility in the intestines.
- 📈 Recovery Timeline (Projected Outcome): Noticeable reduction in bowel movement frequency within 2 to 4 hours.
- 🛠️ Preparation Guide (Laboratory Method): Ensure the bottle is shaken vigorously to distribute the suspension evenly before pouring the exact measured dose into a medical cup.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): NEVER administer to children or teenagers due to the risk of Reye’s Syndrome (associated with salicylates). Expect the tongue and stool to turn harmlessly black. DO NOT USE if the patient has a high fever (>101.5°F) or bloody diarrhea—halting motility in these cases traps invasive bacteria inside the body.
MODULE 04: Gingerol Extract Therapy (Anti-Emetic)
Clinical Objective: Down-regulation of serotonin-induced vagal nerve firing to suppress nausea naturally.
- ⚡ How to Use (Clinical Application): Sip slowly as a warm tea. The heat relaxes stomach muscles while the active compounds neutralize nerve signaling.
- ⚖️ Dosage & Quantity (Clinical Measurement): 1 cup of concentrated ginger tea every 4 to 6 hours.
- 🔬 Mechanism of Action (Electronic Biological Mapping): Gingerol and shogaol (active phytochemicals) act as competitive 5-HT3 receptor antagonists. They literally block the serotonin molecules in your gut from attaching to the vagus nerve, short-circuiting the vomit reflex before it reaches the brain.
- 📈 Recovery Timeline (Projected Outcome): Nausea should abate noticeably 20 to 30 minutes post-consumption.
- 🛠️ Preparation Guide (Laboratory Method): Grate 1 inch of fresh ginger root. Steep in 8 ounces of boiling water for 10 minutes. Strain the fibrous matter. Add a minimal drop of honey (glucose aids in absorption).
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): High doses of ginger can cause mild heartburn. If esophageal burning occurs, dilute the tea further or discontinue use.
Diagnostic Red Flags: When Summer Food Poisoning Becomes a Hospital Emergency
While most cases of summer food poisoning resolve within 24 to 72 hours through rigorous at-home management, complications can be fatal. The line between a manageable infection and a systemic crisis is thin. As a physician, I look for specific biological markers. You must bypass home care and proceed immediately to the emergency room if you observe any of the following:
- Bloody Diarrhea (Hematochezia or Melena): If stool is bright red or black and tarry, it indicates the bacteria have destroyed the intestinal mucosal wall and are causing gastrointestinal bleeding.
- Neurological Decline: Dizziness upon standing, extreme lethargy, confusion, or inability to answer simple questions. This means hypovolemic shock is restricting oxygenated blood flow to the brain.
- Anuria (Lack of Urination): If the patient has not produced urine in 8 hours, their kidneys are shutting down to conserve water.
- Hyperpyrexia: A stubborn fever exceeding 102°F (38.9°C) points to an invasive bacterial infection that has breached the gut barrier and entered the bloodstream (bacteremia).
- Intractable Vomiting: The absolute inability to keep even small sips of water down for more than 12 hours.
Preventive Protocol: Securing the Summer Kitchen

The best treatment for summer food poisoning is absolute avoidance. The rules of food safety bend aggressively under the weight of summer heat.
First, respect the two-hour rule, which becomes the one-hour rule when ambient temperatures exceed 90°F. Potato salads, mayonnaise-based slaws, and raw meats must be kept in coolers submerged in ice. Cold foods must stay below 40°F, and hot foods must be held above 140°F.
Second, sanitize cooking surfaces with militant precision. Cross-contamination is the silent vector of summer food poisoning. Using the same cutting board for raw chicken and watermelon ensures that Campylobacter transfers directly into the porous fruit, which is then eaten raw. Always use separate boards and wash utensils in scalding, soapy water immediately after handling raw protein.
Localized Medical Summaries
🇮🇳 Hindi Summary: Summer Food Poisoning (Quick Social-Ready Guide)
- 1. गर्मियों में खाने में बैक्टीरिया बहुत तेजी से बढ़ते हैं (Summer food poisoning).
- 2. मुख्य लक्षण: अचानक उल्टी, दस्त, पेट में ऐंठन और बुखार।
- 3. यह “Stomach Flu” से अलग है; इसमें भोजन खाने के कुछ ही घंटों बाद लक्षण दिखते हैं।
- 4. सबसे जरूरी कदम: शरीर में पानी की कमी (Dehydration) को रोकना।
- 5. ORS का घोल (Oral Rehydration Solution) पिएं; सिर्फ सादा पानी काफी नहीं है।
- 6. उल्टी होने के बाद 2-4 घंटे तक पेट को आराम दें, कुछ ठोस न खाएं।
- 7. जब भूख लगे, तो BRAT डाइट लें: केला (Banana), चावल (Rice), सेब की चटनी (Applesauce), और टोस्ट (Toast)।
- 8. मसालेदार, तला हुआ खाना और डेयरी उत्पाद (दूध, पनीर) बिल्कुल बंद कर दें।
- 9. वयस्क लोग दस्त रोकने के लिए दवा (जैसे Imodium) ले सकते हैं, लेकिन बच्चों को न दें।
- 10. अगर दस्त में खून आए या तेज बुखार हो, तो दस्त रोकने वाली दवाएं न लें।
- 11. अदरक की चाय (Ginger tea) पीने से उल्टी और मतली में आराम मिलता है।
- 12. खतरे के संकेत: 8 घंटे तक पेशाब न आना या चक्कर आना।
- 13. अगर लक्षण 3 दिन से ज्यादा रहें, तो तुरंत डॉक्टर से मिलें।
- 14. बचाव: गर्मी में बाहर रखा खाना 1-2 घंटे के भीतर फ्रिज में रख दें।
- 15. कच्चा मांस और सलाद को हमेशा अलग-अलग काटें।
🇮🇳 Hinglish Summary: Summer Food Poisoning (Easy-to-Read Guide)
- 1. Garmiyon mein khana jaldi kharab hota hai, jisse summer food poisoning ka khatra badh jata hai.
- 2. Symptoms: Sudden vomiting, loose motions (diarrhea), stomach cramps, aur fever.
- 3. Khana khane ke 2-6 ghante baad hi iske asar dikhne lagte hain.
- 4. Sabse bada risk dehydration ka hai, isliye fluids lagatar lete rahein.
- 5. Khali pani peene se behtar hai ORS (electrolytes) ya nariyal pani thoda-thoda piyein.
- 6. Ulti (vomiting) ke turant baad solid food avoid karein, stomach ko rest dein.
- 7. Diet mein BRAT protocol follow karein: Banana, Rice, Applesauce, Toast.
- 8. Milk, cheese, spicy food, aur alcohol ko poori tarah avoid karein.
- 9. Adults non-bloody diarrhea ke liye OTC meds le sakte hain, par baccho ko na dein.
- 10. Agar fever 102°F se upar ho ya stool mein blood aaye, toh meds mat lein.
- 11. Adrak (ginger) ko boil karke peene se nausea mein quick relief milta hai.
- 12. ER Red Flag: Agar 8 hours se urine pass na hua ho, ya extreme weakness ho.
- 13. Agar 3 din baad bhi symptoms theek na hon, toh clinic visit zaroori hai.
- 14. Prevention: Bahar rakha khana 1 ghante mein fridge mein daal dein agar garmi zyada ho.
- 15. Chopping boards hamesha clean rakhein taaki cross-contamination na ho.
25+ High-Yield Clinical FAQs: Summer Food Poisoning
Patients present with myriad questions regarding their symptoms. Below is a comprehensive diagnostic Q&A designed to eliminate confusion surrounding summer food poisoning.
1. How long does summer food poisoning usually last?
Most acute episodes of summer food poisoning resolve within 24 to 72 hours. The intensive vomiting phase typically burns out after 12 hours, followed by 1-2 days of residual diarrhea and fatigue as the intestinal lining repairs itself.
2. Can I drink plain water to rehydrate?
Plain water is inadequate during severe summer food poisoning. Because you are losing vast amounts of sodium and potassium, drinking plain water can dilute your blood sodium further (hyponatremia). You must consume oral rehydration solutions (ORS) to replenish lost electrolytes.
3. Is it safe to take Imodium for diarrhea?
Loperamide (Imodium) is safe for healthy adults experiencing watery diarrhea WITHOUT a high fever or bloody stool. If blood or a high fever is present, taking anti-motility drugs will trap the dangerous bacteria inside your intestines, exacerbating the infection.
4. Why does food poisoning happen more often in the summer?
Ambient temperatures in the summer fall directly into the bacterial “Danger Zone” (40°F to 140°F). Combined with outdoor activities like picnics and barbecues where refrigeration is scarce, pathogens like Salmonella and E. coli multiply at exponential rates.
5. What is the BRAT diet?
The BRAT diet consists of Bananas, Rice, Applesauce, and Toast. These are low-fiber, bland, easily digestible carbohydrates that help bulk up loose stools while providing the gastrointestinal tract an opportunity to rest and recover.
6. How soon after eating contaminated food do symptoms start?
It depends on the pathogen. Staphylococcal food poisoning can strike within 30 minutes. Salmonella may take 6 to 48 hours to manifest. Generally, summer food poisoning presents faster than viral gastroenteritis.
7. Is milk bad for food poisoning?
Yes. Summer food poisoning temporarily damages the tips of your intestinal villi where lactase (the enzyme that digests lactose) is produced. Consuming dairy will result in undigested lactose drawing more water into the bowel, worsening diarrhea.
8. When should I take a child to the hospital?
Pediatric cases escalate quickly. Seek emergency care if a child exhibits a sunken fontanelle (soft spot), cries without producing tears, has a dry mouth, lethargy, or has not produced a wet diaper in over 4 to 6 hours.
9. Does coffee help with stomach cramps?
Absolutely not. Caffeine is a gastric irritant and a mild diuretic. It will increase intestinal motility (worsening abdominal cramps and diarrhea) and accelerate fluid loss, deepening dehydration.
10. Can I get food poisoning from watermelon?
Yes. If the exterior rind of a melon is not washed, the knife used to slice it drags soil-based bacteria (like Listeria or Salmonella) directly into the flesh. Once sliced and left in the summer heat, the sugar-rich fruit breeds bacteria rapidly.
11. What does bloody diarrhea mean?
Bloody diarrhea indicates invasive bacterial action. Pathogens like E. coli O157:H7 or Shigella are actively eroding the vascular lining of your colon. This is a red flag requiring immediate emergency room evaluation and potential antibiotic therapy.
12. Should I induce vomiting if I suspect I ate bad food?
No. Inducing vomiting can cause esophageal tearing (Mallory-Weiss tears) and aspiration of gastric contents into the lungs. Let your body’s enteric nervous system dictate if emesis is necessary.
13. Is chicken the most common cause?
While raw poultry (carrying Campylobacter and Salmonella) is a massive vector, leafy greens, sprouts, and mayonnaise-based side dishes left in the heat are statistically responsible for vast numbers of summer food poisoning outbreaks.
14. Are antibiotics necessary for summer food poisoning?
Rarely. Most cases are self-limiting, and the body flushes the toxins out naturally. In fact, giving antibiotics for certain E. coli infections can trigger a deadly kidney complication called Hemolytic Uremic Syndrome (HUS).
15. Can pregnant women take Pepto-Bismol?
No. Bismuth subsalicylate is contraindicated during pregnancy as the salicylates can absorb into the bloodstream and affect fetal circulation. Pregnant women should rely on ORS and consult an obstetrician immediately.
16. Why do I feel dizzy when I stand up?
This is called orthostatic hypotension. Because summer food poisoning causes massive fluid loss via vomiting and diarrhea, your overall blood volume drops. When you stand, gravity pulls blood down, and there isn’t enough pressure to pump it quickly to your brain.
17. Are sports drinks as good as ORS?
No. Sports drinks are formulated to replace sweat, not diarrheal fluid. They contain high amounts of sugar (which can worsen osmotic diarrhea) and vastly insufficient amounts of critical sodium and potassium required for clinical rehydration.
18. How do probiotics help after food poisoning?
The acute infection and mechanical purging strip your gut of its native, beneficial microbiome. Taking clinically studied probiotics (like Lactobacillus rhamnosus GG or Saccharomyces boulardii) after the vomiting stops helps recolonize the gut flora and shorten the duration of diarrhea.
19. Can I get food poisoning from ice?
Yes. Freezing does not kill bacteria; it only renders them dormant. If ice is made from contaminated water or handled with unwashed hands, the bacteria will reactivate as soon as the ice melts in your digestive tract.
20. Does alcohol kill food poisoning bacteria?
No. The concentration of alcohol in a beverage is vastly insufficient to act as an internal sterilizing agent. Furthermore, alcohol severely irritates the gastric mucosa and exacerbates dehydration.
21. Why does my stomach still hurt a week later?
Post-infectious irritable bowel syndrome (PI-IBS) is a common aftermath. The severe inflammation during the acute phase can leave the nerves in the gut hyper-sensitive, causing ongoing mild cramps and irregular bowel habits for several weeks.
22. Can smelling bad food make me sick?
No. Pathogens causing summer food poisoning must be ingested and enter the gastrointestinal tract to establish an infection and release enterotoxins. Smelling spoiled food may induce nausea, but it will not cause true food poisoning.
23. Is coconut water effective for rehydration?
Coconut water is an excellent source of natural potassium and is better than plain water. However, it lacks the high sodium content found in a true ORS, which is the primary electrolyte lost during massive diarrheal purging.
24. Can I use activated charcoal?
While activated charcoal is used in clinical toxicology for certain poisonings, its efficacy for bacterial food poisoning is debated. It may bind to some toxins, but it can also induce vomiting and bind to useful medications. Consult a physician before use.
25. How do I clean my kitchen after a food poisoning incident?
Discard all suspected food. Wash all cutting boards, knives, and countertops with hot, soapy water, followed by a sanitizing solution of 1 tablespoon of unscented liquid bleach per gallon of water. Let surfaces air dry.
26. Is it safe to fast during summer food poisoning?
Yes, an initial liquid-only fast for the first 12 to 24 hours is highly recommended. Forcing your inflamed gastrointestinal tract to mechanically process solid food will inevitably trigger the gastrocolic reflex, leading to immediate vomiting and further discomfort.
© 2026 Dr. Akram Medical Strategy Group. All Rights Reserved.
Medically Reviewed by Prof. Dr. Akram
Orthopedic Surgeon | Professor | Senior Medical Specialist
Prof. Dr. Akram is a distinguished surgeon with over 15 years of clinical expertise. Having served as a lead Emergency Specialist at Complex International Government Hospital, he currently leads a specialized team of 13 medical professionals at his private hospital. As a Professor at top medical universities, he ensures that every article on WellHealthOrg.com meets rigorous clinical standards.
Medical Disclaimer:
The information provided is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician for any medical concerns.
Our content is rigorously fact-checked by our 13-member Editorial Team under the clinical supervision of Prof. Dr. Akram.







