⚕️ Medically Verified by Prof. Dr. Akram
Chief Medical Content Strategist & Senior Neurologist | 🟢 Status: Online
Over 30 years of clinical expertise decoding complex neurological and endocrine interactions.
The Invisible Threat: Managing Diabetes in a Heatwave
Summer brings an entirely different clinical paradigm for metabolic health. Managing diabetes in a heatwave is not just about finding shade; it is an active clinical battle against accelerated insulin absorption, silent dehydration, and erratic glucose fluctuations. I vividly recall a July afternoon years ago when a seasoned patient of mine—let us call him David—collapsed in his garden. He had taken his normal morning basal insulin dose. What he did not account for was the 98-degree heat. The thermal stress caused his peripheral blood vessels to dilate rapidly, sweeping the subcutaneous insulin into his bloodstream at twice the normal rate. He plummeted into severe hypoglycemia before he even felt thirsty.
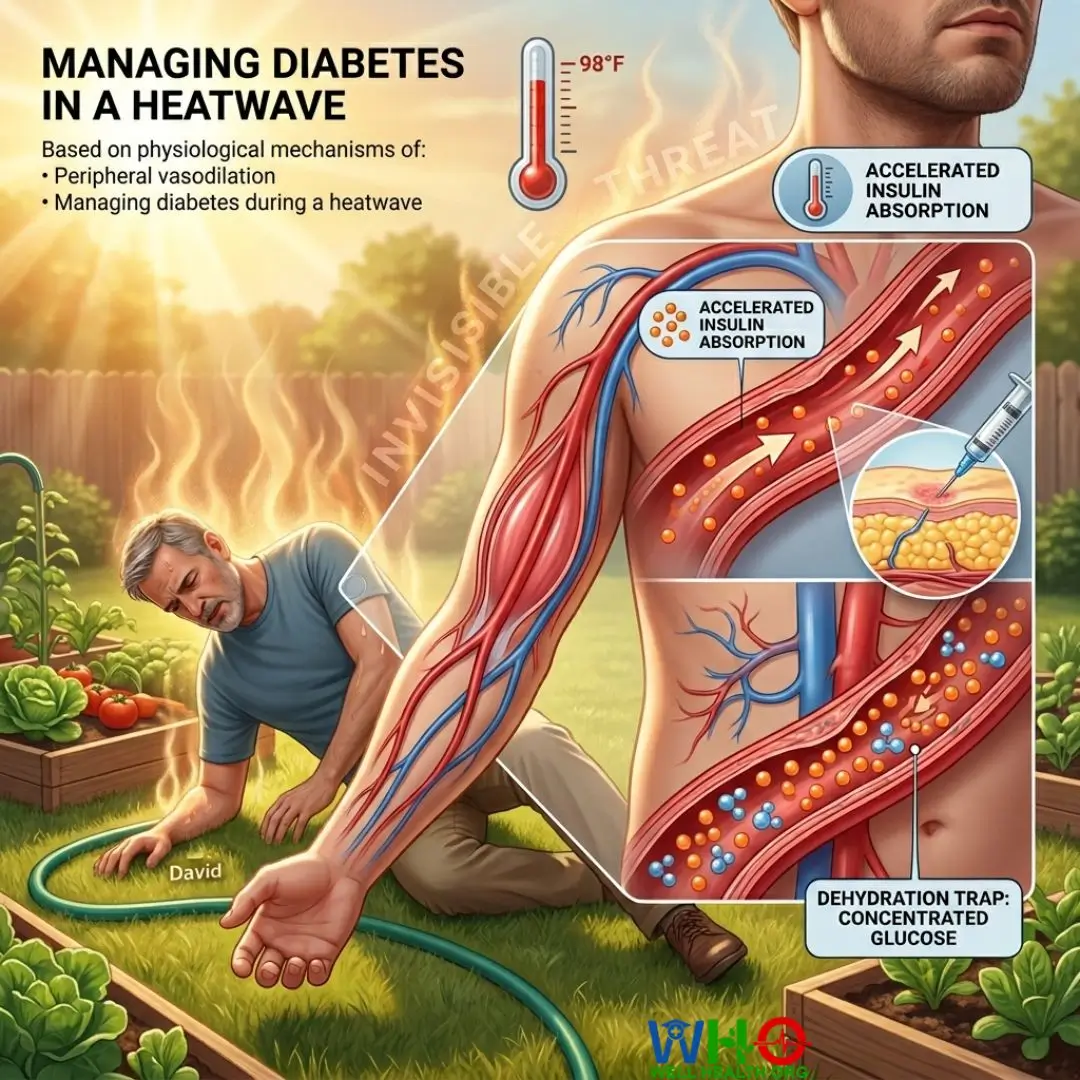
The human body operates like an intricate biochemical thermostat. When ambient temperatures rise, the body diverts blood to the skin’s surface to sweat and cool down. For a person without metabolic impairment, this is routine. For someone relying on exogenous insulin or oral hypoglycemics, this physiological shift alters the pharmacokinetics of every medication in their system.
Shareable Insight: “Dehydration in diabetes is a mathematical trap: less water equals highly concentrated blood glucose. Hydrate before you calculate.”
To master managing diabetes in a heatwave, we must move beyond basic advice and understand the underlying vascular and cellular mechanics at play. We must differentiate between heat exhaustion and a hypoglycemic crash, as their symptoms overlap dangerously. In this medical dossier, I will walk you through exact emergency protocols, biological mechanisms, and the clinical toolkit required to navigate thermal extremes safely.
Social Index & Clinical Navigation
The Biological Impact: Why High Temperatures Alter Glycemic Control
Every biological process in the human body is temperature-dependent. Managing diabetes in a heatwave requires recognizing that external heat forces internal physiological adaptations. Let me break down exactly what happens beneath the skin when the mercury rises.
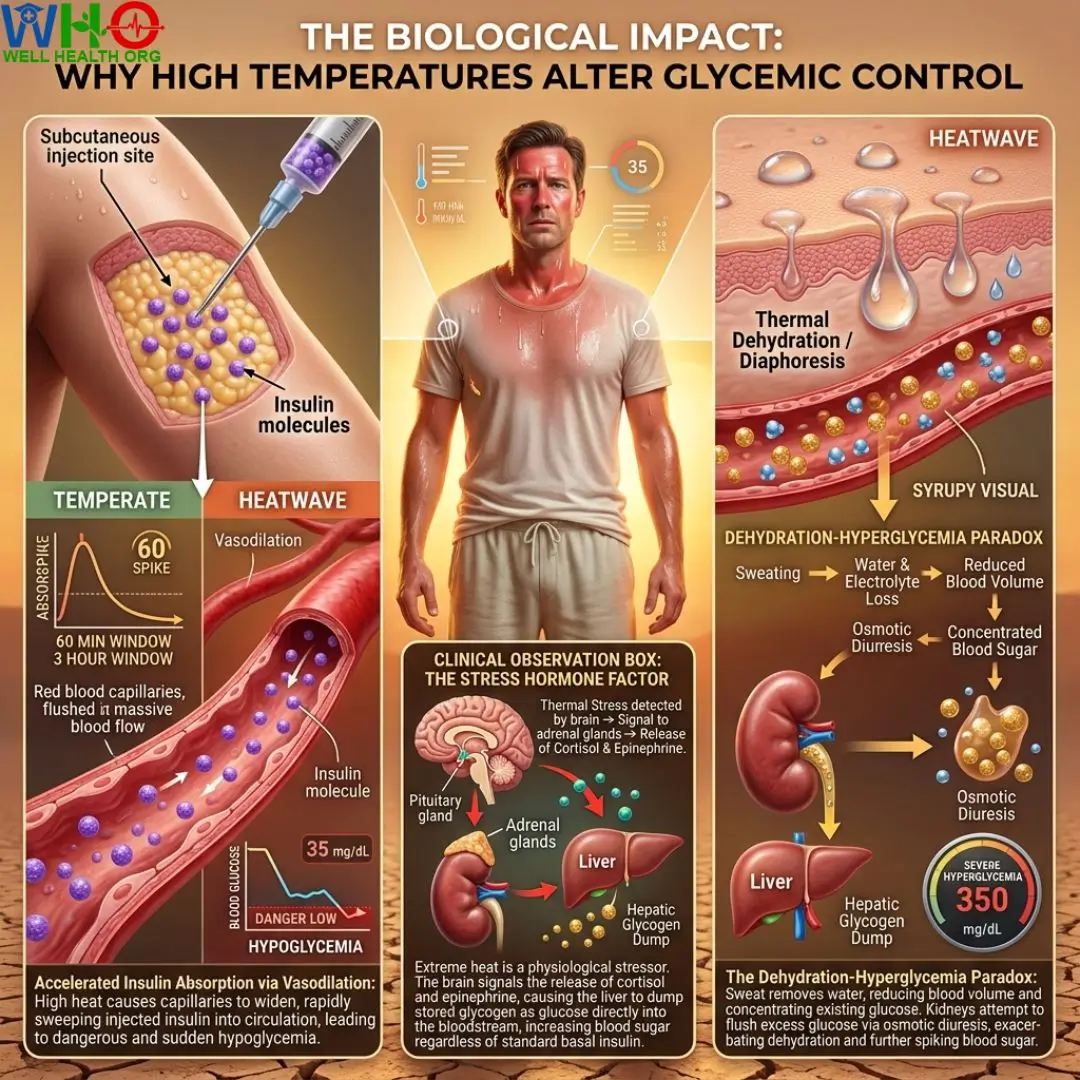
Accelerated Insulin Absorption via Vasodilation
Insulin is typically injected subcutaneously—into the layer of fat just beneath the skin. In a temperate environment, this insulin is absorbed into the bloodstream at a predictable rate, establishing your basal or bolus curve. However, high heat triggers a process called vasodilation. The endothelial cells lining your blood vessels release nitric oxide, causing the smooth muscles of the vessel walls to relax and widen.
This expansion pushes more blood toward the skin’s surface to dissipate heat. Consequently, the capillary beds surrounding your insulin injection site are suddenly flushed with massive blood flow. The injected insulin is swept into systemic circulation much faster than intended. What was supposed to be a slow, steady three-hour absorption window condenses into a rapid 60-minute spike. This sudden influx of insulin clears glucose from the blood too quickly, precipitating dangerous and sudden hypoglycemia.
The Dehydration-Hyperglycemia Paradox
While vasodilation pulls you toward low blood sugar, thermal dehydration yanks you violently in the opposite direction. Heat causes profound diaphoresis (sweating). Sweating removes both water and essential electrolytes from your vascular system. When your blood volume decreases due to water loss, the concentration of glucose remaining in the blood spikes. Imagine a glass of water with two spoons of sugar; if half the water evaporates, the remaining liquid becomes incredibly sweet and syrupy.
The kidneys sense this hyperosmolar state and attempt to flush the excess glucose out via urine (osmotic diuresis). This creates a vicious cycle: high blood sugar forces you to urinate, which exacerbates dehydration, which further concentrates blood sugar. Managing diabetes in a heatwave means actively intercepting this dehydration loop before it escalates into Diabetic Ketoacidosis (DKA) or Hyperosmolar Hyperglycemic State (HHS).
📝 Clinical Observation Box: The Stress Hormone Factor
Patient records often show inexplicable glucose spikes during heatwaves, even in patients who remain indoors but lack air conditioning. Extreme heat is a physiological stressor. The brain perceives prolonged thermal stress as a threat, signaling the adrenal glands to release cortisol and epinephrine. These counter-regulatory hormones signal the liver to dump stored glycogen directly into the bloodstream as glucose, preparing the body for a “fight or flight” response to the heat. This hepatic glucose release defies standard basal insulin regimens.
Recognizing the Red Flags: Heat Exhaustion vs. Hypoglycemia
One of the most profound dangers of managing diabetes in a heatwave is symptomatological overlap. The physical signs of heat exhaustion are nearly identical to the signs of severe hypoglycemia. Misdiagnosing yourself in the moment can lead to administering the wrong treatment, which can be fatal.

Decoding the Symptoms
When my patients ask how to tell the difference, I teach them to look for the nuances. Both conditions will cause profound diaphoresis (sweating), tachycardia (rapid heartbeat), extreme fatigue, dizziness, and shaking. However:
- Hypoglycemia specific indicators: Profound cognitive confusion, irritability, sudden hunger, tingling around the lips or tongue, and visual disturbances (blurred or double vision).
- Heat Exhaustion specific indicators: Muscle cramping in the abdomen or legs, nausea or vomiting, a mild headache that feels like a tight band, and cool, clammy skin despite the heat.
The Clinical Directive: Never guess. If you feel faint, shaking, or sweating excessively in the heat, the immediate first step is to check your blood glucose. Treating heat exhaustion when you are actually hypoglycemic means your brain continues to starve of glucose. Treating hypoglycemia when you actually have heat exhaustion means you are delaying critical cooling measures while needlessly spiking your blood sugar.
Clinical Remedial Ecosystem
Theory is only useful when translated into actionable therapeutics. The following section contains precise medical protocols. Think of these as your emergency deployment strategies when managing diabetes in a heatwave fails to prevent a crisis.
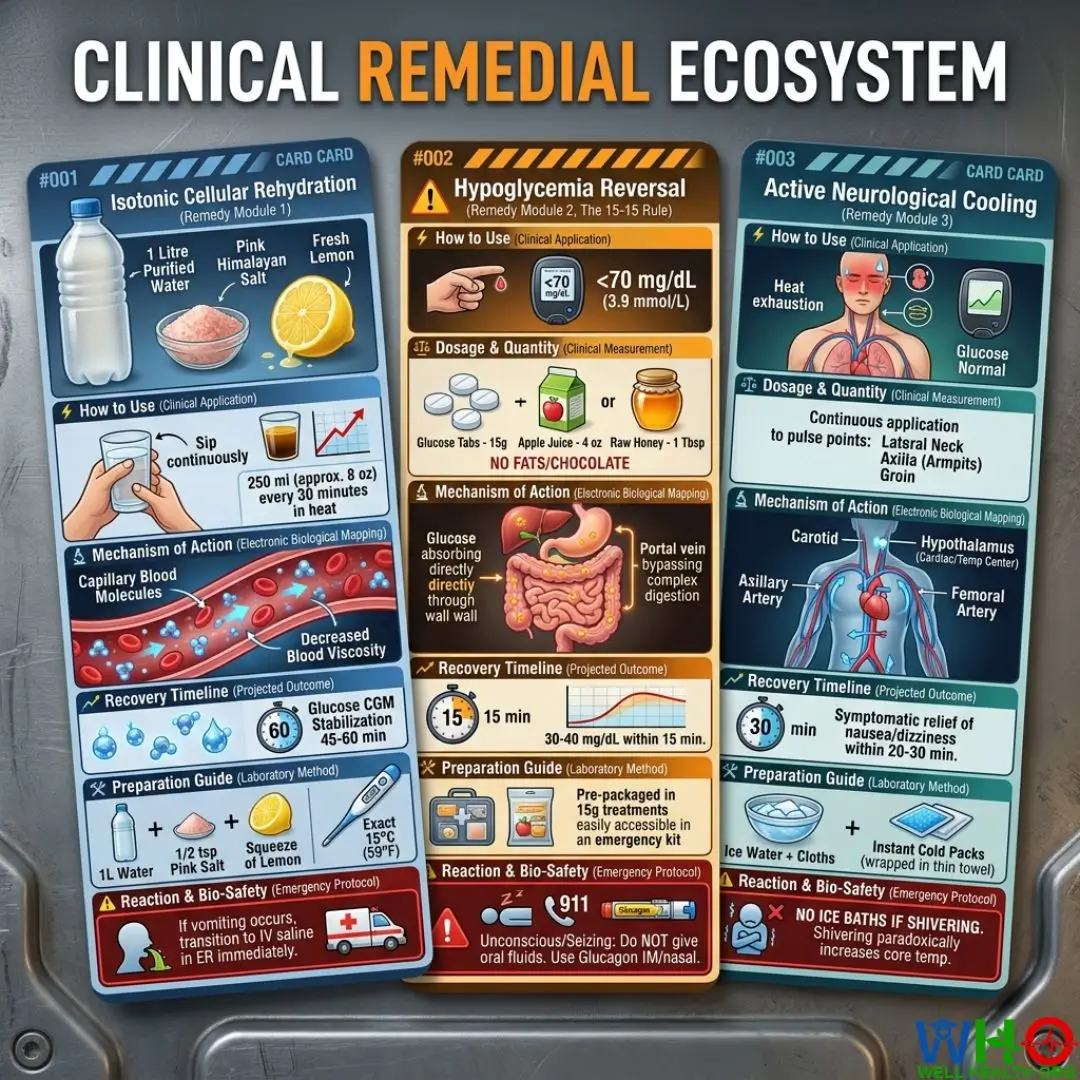
Remedy Module 1: Rapid Hyper-Hydration Protocol
Card #001: Isotonic Cellular Rehydration
⚡ How to Use (Clinical Application): Initiate this protocol immediately upon noting concentrated, dark urine or a creeping rise in baseline blood glucose during high ambient temperatures. Sip continuously rather than gulping to prevent gastric distension and vomiting.
⚖️ Dosage & Quantity (Clinical Measurement): 250 ml (approximately 8 oz) of cool, sugar-free electrolyte water every 30 minutes while exposed to heat. Ensure the fluid contains sodium and potassium but strictly zero simple carbohydrates (unless treating a simultaneous low).
🔬 Mechanism of Action (Electronic Biological Mapping): Reintroduces hypotonic fluid into the vascular space, decreasing blood viscosity. This dilutes the serum glucose concentration back to physiological norms and provides the kidneys with the necessary hydraulic pressure to filter out excess ketones and glucose without taxing the renal tubules.
📈 Recovery Timeline (Projected Outcome): Cellular rehydration begins within 15-20 minutes of ingestion. Blood glucose concentration stabilization should be observable on a continuous glucose monitor (CGM) within 45 to 60 minutes.
🛠️ Preparation Guide (Laboratory Method): Combine 1 liter of purified water with 1/2 teaspoon of pink Himalayan salt (for sodium/trace minerals) and a squeeze of fresh lemon (potassium). Chill to exactly 15°C (59°F)—this specific temperature maximizes gastric emptying rates.
⚠️ Reaction & Bio-Safety (Emergency Protocol): If the patient begins vomiting and cannot keep fluids down, oral rehydration has failed. Immediate transition to an emergency room for intravenous (IV) normal saline is required to prevent hyperosmolar coma.
Remedy Module 2: Fast-Acting Glucose Intervention
Card #002: Hypoglycemia Reversal (The 15-15 Rule)
⚡ How to Use (Clinical Application): Administer the moment a blood glucose check reads below 70 mg/dL (3.9 mmol/L) accompanied by vasodilation-induced insulin rushing.
⚖️ Dosage & Quantity (Clinical Measurement): Exactly 15 grams of pure, simple, fast-acting carbohydrates. Do not use chocolate or fat-heavy snacks, as lipid chains delay gastric emptying and slow glucose absorption.
🔬 Mechanism of Action (Electronic Biological Mapping): Simple monosaccharides bypass complex digestive breakdown in the duodenum. They diffuse directly across the intestinal mucosa into the portal vein, rapidly traveling to the liver and central circulation, actively raising serum glucose and shutting off the adrenal panic response.
📈 Recovery Timeline (Projected Outcome): Glucose levels should rise by 30-40 mg/dL within 15 minutes. Re-test at the 15-minute mark.
🛠️ Preparation Guide (Laboratory Method): Pre-package precise interventions: 4 chewable glucose tablets, 4 ounces (1/2 cup) of apple or grape juice, or 1 tablespoon of raw honey. Keep these accessible on the outer layer of your emergency kit.
⚠️ Reaction & Bio-Safety (Emergency Protocol): If the patient becomes unconscious or seizes, do NOT administer oral fluids or food due to aspiration risk. Administer emergency Glucagon (intramuscular injection or nasal powder like Baqsimi) immediately and contact paramedics.
Remedy Module 3: Cutaneous Thermal Regulation
Card #003: Active Neurological Cooling
⚡ How to Use (Clinical Application): Deploy when a patient exhibits signs of heat exhaustion (dizziness, profound fatigue, tight headache) but blood sugar confirms normal glycemic ranges.
⚖️ Dosage & Quantity (Clinical Measurement): Continuous application to the major arterial pulse points: the lateral neck (carotid arteries), the axilla (armpits), and the groin (femoral arteries).
🔬 Mechanism of Action (Electronic Biological Mapping): Placing cold compresses on areas where major arteries run close to the skin surface acts as a biological radiator. The chilled blood circulates back to the cardiac center and hypothalamus, actively lowering core body temperature and downregulating the hyperactive sympathetic nervous system.
📈 Recovery Timeline (Projected Outcome): Core body temperature reduction should yield symptomatic relief of nausea and dizziness within 20 to 30 minutes. Vasodilation will reverse, normalizing insulin absorption rates.
🛠️ Preparation Guide (Laboratory Method): Soak clean cotton cloths in ice water, wring out the excess, and apply. Alternatively, use instant chemical cold packs wrapped in a thin towel to prevent cryogenic tissue damage (frostbite).
⚠️ Reaction & Bio-Safety (Emergency Protocol): Do not submerge a patient in an ice bath if they are shivering. Shivering creates muscular friction that paradoxically increases internal core temperature, worsening the heatstroke trajectory.
Pharmacological & Environmental Shielding
Managing diabetes in a heatwave extends far beyond bodily physiology. The molecular integrity of your medications and the integrity of your sensory feedback systems are equally at risk. I have seen countless cases where patients maintained perfect hydration, yet still ended up hospitalized because their insulin simply stopped working.
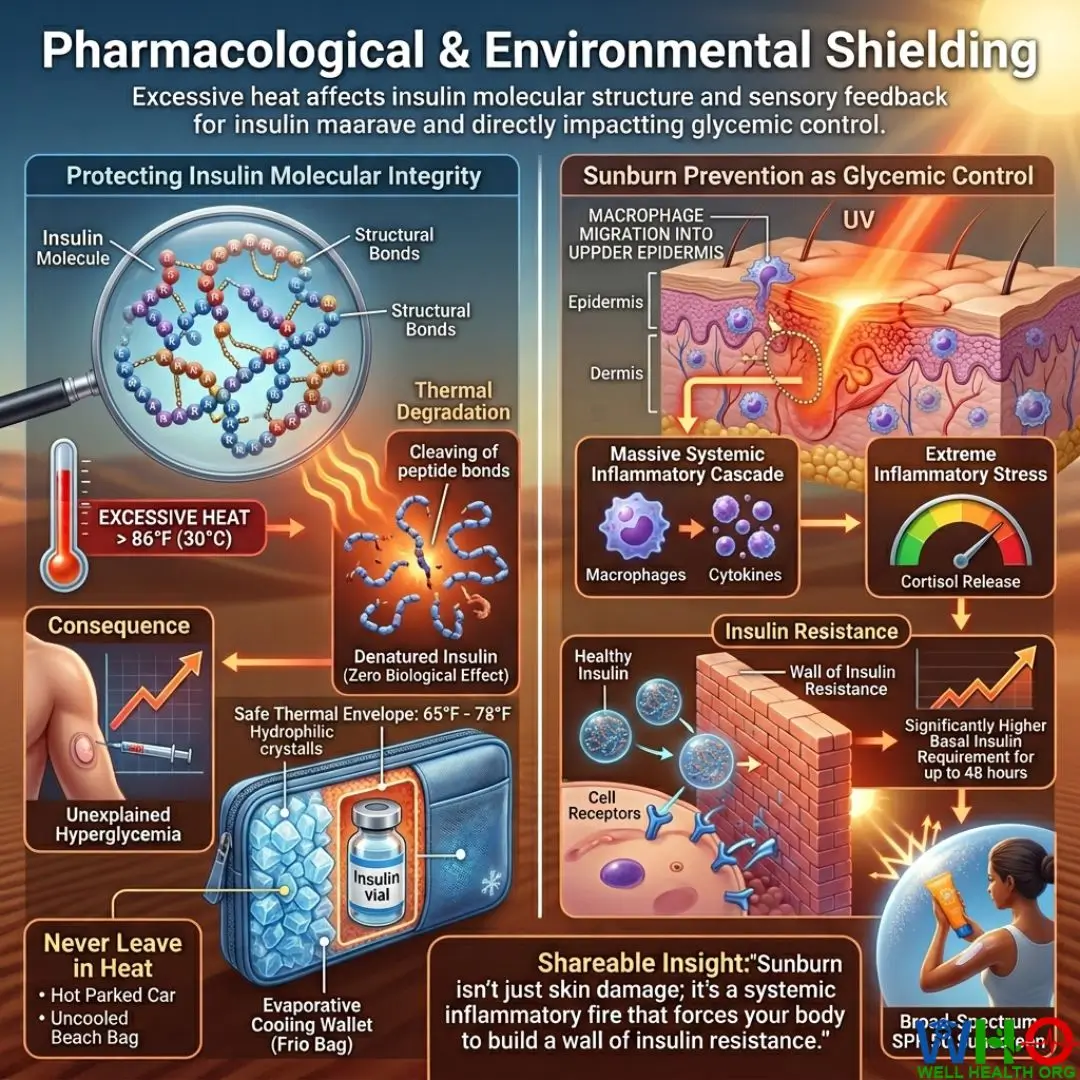
Protecting Insulin Molecular Integrity
Insulin is a polypeptide hormone. It consists of delicate chains of amino acids held together by specific structural bonds. When exposed to temperatures exceeding 86°F (30°C), thermal degradation occurs. The heat actively cleaves these peptide bonds, denaturing the protein structure. Once insulin is denatured, it is permanently destroyed. It may look perfectly clear in the vial, but injecting it will yield zero biological effect, leading to catastrophic, unexplained hyperglycemia.
Never leave insulin, GLP-1 agonists, or test strips in a parked car, directly under sunlight, or in an uncooled beach bag. Utilizing an evaporative cooling wallet (like a Frio bag) is medically essential. These wallets utilize hydrophilic crystals that swell with water and cool the insulin through prolonged evaporation, keeping the medication within a safe thermal envelope of 65°F to 78°F, even in a desert environment.
Sunburn Prevention as Glycemic Control
It is a clinical reality often overlooked: sunburn directly elevates blood sugar. The skin is your largest organ. When ultraviolet (UV) radiation damages the epidermal layers, it triggers a massive systemic inflammatory cascade. Macrophages and cytokines flood the burn site. This extreme inflammatory stress triggers cortisol release and insulin resistance. You will find that an untreated sunburn requires significantly more basal insulin for up to 48 hours to maintain glycemic control. Applying broad-spectrum SPF 50 sunscreen is, therefore, an active blood sugar management technique.
Shareable Insight: “Sunburn isn’t just skin damage; it’s a systemic inflammatory fire that forces your body to build a wall of insulin resistance.”
Neuropathy and Thermal Foot Safety
Diabetic peripheral neuropathy damages the sensory nerves in the lower extremities. In my neurology practice, I frequently treat patients who have sustained third-degree burns on the soles of their feet simply from walking barefoot on hot beach sand or concrete pool decks. Because the thermal pain receptors are non-functional due to chronic hyperglycemia, the patient feels no pain while the tissue literally cooks. Always wear specialized, protective water shoes or sandals. Inspect your feet nightly for blisters or erythema (redness).
Building the Ultimate Diabetes Heat Safety Kit
Preparedness dictates survival. Managing diabetes in a heatwave necessitates carrying a specialized, portable logistical kit. I advise my patients to assemble a waterproof, insulated medical go-bag specifically for the summer months. Here is the clinical inventory required:

- Insulated Cooling Pouches: Do not rely on direct ice, which can freeze and destroy insulin. Use gel-based evaporative cooling bags for all pens, vials, and oral medications.
- Redundant Testing Equipment: Extreme heat causes Continuous Glucose Monitors (CGMs) to lose adhesion due to sweat, and can fry the internal sensors of traditional glucometers. Carry a backup capillary blood meter, extra test strips (stored in a cool place), and spare batteries.
- Tiered Fast-Acting Carbohydrates: Carry solid glucose (tablets) which will not melt, and liquid glucose (juice boxes) which can be consumed easily even if heat exhaustion makes chewing difficult.
- Osmotic Regulators: Pack sugar-free electrolyte sachets containing sodium, magnesium, and potassium to mix instantly with bottled water.
- Clinical Documentation: A laminated card stating “I have diabetes. If I am confused or unconscious, call emergency services immediately.” Include current basal/bolus ratios and emergency contact numbers.
Regional Medical Summaries
To ensure this crucial medical data crosses linguistic barriers seamlessly, I have organized the primary directives into accessible regional formats.
🇮🇳 Hindi Summary: गर्मी में डायबिटीज का प्रबंधन (15 Key Points)
- 1. गर्मी और इंसुलिन: तेज गर्मी में इंसुलिन शरीर में बहुत तेजी से घुलता है।
- 2. लो ब्लड शुगर का खतरा: इंसुलिन के तेजी से घुलने से शुगर अचानक कम (Hypoglycemia) हो सकती है।
- 3. पानी की कमी (Dehydration): पसीना अधिक आने से शरीर में पानी की कमी होती है, जिससे खून में शुगर गाढ़ा हो जाता है।
- 4. लगातार जांच: गर्मी के मौसम में सामान्य से अधिक बार ब्लड शुगर चेक करें।
- 5. दवाओं का बचाव: इंसुलिन को हमेशा ठंडी जगह या कूलिंग बैग (Frio bag) में रखें।
- 6. धूप में कार: अपनी दवाइयां या शुगर नापने की मशीन कभी भी बंद कार में न छोड़ें।
- 7. सही कपड़े: हल्के रंग के सूती कपड़े पहनें ताकि पसीना सूख सके।
- 8. हाइड्रेशन: प्यास न लगने पर भी हर आधे घंटे में पानी या बिना शक्कर का इलेक्ट्रोलाइट पिएं।
- 9. सनबर्न से बचाव: सनबर्न शरीर में तनाव पैदा करता है, जिससे शुगर बढ़ सकती है; हमेशा सनस्क्रीन लगाएं।
- 10. पैरों की सुरक्षा: नंगे पैर कभी न चलें, गर्म जमीन से पैर जल सकते हैं और न्यूरोपैथी के कारण आपको दर्द महसूस नहीं होगा।
- 11. एक्सरसाइज का समय: व्यायाम केवल सुबह जल्दी या शाम को करें जब मौसम ठंडा हो।
- 12. इमरजेंसी किट: अपने साथ हमेशा ग्लूकोज टैबलेट या जूस रखें।
- 13. हीट एग्जॉशन: चक्कर आना, कमजोरी, और मतली होना गर्मी लगने के लक्षण हैं।
- 14. शुगर लो होने के लक्षण: घबराहट, पसीना, और भ्रम होना शुगर कम होने का संकेत है।
- 15. डॉक्टर की सलाह: गर्मी में इंसुलिन की मात्रा (डोज़) बदलने के लिए हमेशा अपने डॉक्टर से बात करें।
🇮🇳 Hinglish Summary: Heatwave mein Diabetes Management (15 Key Points)
- 1. Fast Insulin Absorption: High heat mein blood vessels expand hoti hain, jisse insulin body mein bahut jaldi absorb ho jata hai.
- 2. Hypoglycemia Risk: Is fast absorption ki wajah se blood sugar achanak low ho sakta hai.
- 3. Dehydration Trap: Pasina aane se body ka water level girta hai, jisse blood mein sugar concentrate ho kar high ho jati hai.
- 4. Frequent Monitoring: Garmiyo mein outdoor activities ke time apna blood glucose zyada frequent check karein.
- 5. Insulin Protection: Insulin protein se bana hota hai, heat se ye kharab ho sakta hai. Isko hamesha cool bag mein rakhein.
- 6. Hot Car Danger: Glucometer aur test strips ko kabhi dhoop mein park ki hui car mein na chodein; readings galat aayengi.
- 7. Stay Hydrated: Pyas na lagne par bhi water aur sugar-free electrolytes sip karte rahein.
- 8. Clothing: Loose, breathable, light-colored cotton clothes pehnein taaki body ka temperature maintain rahe.
- 9. Sunscreen is Must: Sunburn body mein inflammation badhata hai, jisse insulin resistance hoti hai aur sugar badhti hai.
- 10. Foot Safety: Beach ya pool ke paas nange pair na chalein. Neuropathy ke chalte jalne ka ehsas nahi hota.
- 11. Workout Timings: Intense workout ya gardening sirf early morning ya late evening mein karein.
- 12. Rule of 15: Low sugar feel hone par 15g fast-acting carbs (jaise glucose tablets) lein aur 15 min baad check karein.
- 13. Emergency Kit: Hamesha ek waterproof pouch mein extra strips, insulin, aur juice box carry karein.
- 14. Identify Symptoms: Confusion aur shakiness low sugar ka sign hai, jabki muscle cramps aur nausea heat exhaustion ka.
- 15. Medical Help: Agar severe dizziness ho ya sugar control na ho raha ho, toh turant doctor se dose adjustment ke liye consult karein.
Exhaustive Clinical FAQs: Managing Diabetes in a Heatwave
In my clinical practice, patient education forms the bedrock of preventive medicine. Below are the most critical inquiries I field regarding maintaining metabolic homeostasis during summer thermal events.
1. Does extreme heat cause false Continuous Glucose Monitor (CGM) readings?
Yes. Extreme temperatures can compromise the interstitial fluid dynamics surrounding the sensor filament. Furthermore, excessive sweating can cause the sensor adhesive to loosen, slightly pulling the filament out of the correct tissue depth, leading to erratic or falsely low readings. Always verify suspicious CGM alerts with a capillary fingerstick using a traditional blood glucose meter during a heatwave.
2. How does dehydration specifically spike my blood sugar?
The mechanism is volume depletion. Your blood volume is primarily water. When you sweat out that water, the volume of blood decreases, but the absolute amount of glucose in your bloodstream remains the same. This results in a higher concentration of glucose per deciliter of blood. Managing diabetes in a heatwave means understanding that rehydrating literally dilutes this concentration back to safe levels.
3. Can I store my insulin directly on ice in a cooler?
Never. Placing insulin directly against ice risks freezing the peptide structure. Once insulin freezes, the molecular bonds shatter, rendering it permanently biologically inactive, just as if it had been boiled. Use a barrier layer (like a towel) between the ice and the medication, or preferably, use a specialized gel-based evaporative cooling wallet designed strictly for medical use.
4. Why do I feel suddenly exhausted when my blood sugar is perfectly fine in the heat?
This is thermoregulatory fatigue. Your heart is pumping massively to dilate peripheral blood vessels and produce sweat. This requires a tremendous amount of cellular ATP (energy). The exhaustion you feel is your cardiovascular system working overtime, which mimics the lethargy of hyperglycemia. Rest in the shade and hydrate.
5. How much water should I drink while outdoors in the summer?
The standard medical recommendation for a diabetic patient exposed to high heat is approximately 250 ml (8 ounces) every 30 minutes. Do not wait for the thirst mechanism to trigger, as thirst is a lagging indicator. By the time your brain registers thirst, you are already mildly dehydrated and your blood glucose concentration has likely begun to rise.
6. Can I exercise outside during a heatwave?
It is highly discouraged during peak thermal hours (10 AM to 4 PM). Exercise already sensitizes cells to insulin. Combining exercise-induced insulin sensitivity with heat-induced vasodilation creates a synergistic effect that almost guarantees sudden, severe hypoglycemia. Limit activity to early dawn or indoor, air-conditioned environments.
7. What happens if I use insulin that has been degraded by heat?
Denatured insulin loses its ability to bind to cellular insulin receptors. If you inject it, your blood sugar will simply continue to rise as if you had injected saline. You will face unexplained, refractory hyperglycemia, risking Diabetic Ketoacidosis (DKA) if not quickly corrected with a fresh, intact vial of insulin.
8. Will sweating lower my blood sugar?
Sweating itself does not utilize glucose; it utilizes water and electrolytes. However, the cardiovascular effort required to cool the body burns calories, and the heat accelerates insulin absorption. Therefore, the *conditions* causing the sweat often result in lowered blood sugar, even though the sweat itself is not exuding glucose.
9. Does drinking ice-cold water help cool the body faster?
Counterintuitively, chugging ice-cold water can trigger a vagus nerve response that causes stomach cramping and slows gastric emptying. Cool water (around 15°C or 59°F) is absorbed by the gastrointestinal tract much more efficiently, restoring vascular volume without causing gastrointestinal distress.
10. How does sunburn affect diabetes control?
Sunburn is profound systemic inflammation. The body reacts to damaged skin by releasing stress hormones like cortisol and inflammatory cytokines, which induce significant insulin resistance. Managing diabetes in a heatwave means understanding that a bad sunburn might require your doctor to temporarily increase your basal insulin doses for days.
11. What is the difference between heat exhaustion and heatstroke?
Heat exhaustion involves heavy sweating, dizziness, and a rapid pulse—your body is struggling but still regulating its temperature. Heatstroke is a medical emergency where the thermoregulatory system completely fails; sweating stops, the skin becomes hot and dry, and severe neurological confusion or unconsciousness sets in.
12. Should I adjust my basal insulin dosage before going into the heat?
This requires a deeply personalized clinical assessment. Many patients find they need a slight reduction (e.g., 10-20%) in their background basal insulin during extreme heatwaves to prevent vasodilation-induced lows. You must consult your endocrinologist before making proactive adjustments to your basal rates.
13. Is it safe to consume sports drinks for hydration?
Standard sports drinks are densely packed with high-fructose corn syrup, which will induce massive hyperglycemic spikes. Diabetics must strictly use zero-sugar, zero-carbohydrate electrolyte formulations designed specifically for hydration without caloric impact, unless they are actively treating a hypoglycemic event.
14. Why do my feet swell in the heat, and is it related to diabetes?
Heat causes vasodilation, allowing fluid to leak into the interstitial spaces of the lower extremities due to gravity. While anyone can experience heat edema, diabetic patients with compromised vascular elasticity or early-stage peripheral artery disease (PAD) are particularly susceptible to severe lower limb swelling.
15. What are the signs that my test strips have gone bad from heat?
Test strips contain delicate biological enzymes (like glucose oxidase) that react with your blood. If exposed to heat over 86°F (30°C), these enzymes degrade. The primary sign is erratic, completely illogical readings—such as testing 400 mg/dL, retesting a minute later, and getting 120 mg/dL. Always keep strips at room temperature.
16. Does high humidity make managing diabetes harder?
Absolutely. High humidity prevents sweat from evaporating off the skin. Evaporation is the actual mechanism that cools the blood. Without it, your core temperature rises faster, forcing even more extreme vasodilation, which pushes insulin absorption into overdrive and severely increases the risk of heat exhaustion.
17. Can I drink caffeine during a heatwave?
Caffeine is a mild diuretic. While a morning cup of coffee is generally acceptable, heavily consuming caffeinated beverages or energy drinks in extreme heat will exacerbate fluid loss through increased urination. This accelerates the dehydration-hyperglycemia cycle. Stick primarily to plain water or electrolyte infusions.
18. What should I do if my insulin turns cloudy?
If clear insulin (like rapid-acting aspart or lispro) becomes cloudy, yellowish, or develops stringy crystalline clumps, it has suffered irreversible thermal degradation. Discard the vial immediately. Do not attempt to use it, as it will lack any physiological efficacy and jeopardize your glycemic stability.
19. Are Type 2 diabetics as affected by heat as Type 1 diabetics?
Yes, though the mechanisms slightly differ. Type 1 diabetics face severe risks regarding exogenous insulin absorption rates. Type 2 diabetics, especially those on oral medications like Sulfonylureas or SGLT2 inhibitors (which induce diuresis), are incredibly vulnerable to profound dehydration and acute hyperosmolar events in the heat.
20. Why do my hands shake when I get too hot?
Tremors in the heat can be caused by two distinct pathways: either a rapid drop in blood glucose (hypoglycemia triggering an adrenaline release), or a severe depletion of central nervous system electrolytes (sodium and potassium) due to heavy diaphoresis. A quick glucose check will instantly differentiate the two.
21. Should I inject insulin into a different site during summer?
It is clinically advisable to avoid injecting insulin into limbs that are about to be heavily utilized (e.g., injecting your thigh before a summer hike). Muscular contraction combined with thermal vasodilation will maximize the absorption speed. The abdomen generally provides a more stable absorption rate, though it is still accelerated by heat.
22. Is a cooling vest helpful for diabetics?
Yes. For patients who must work outdoors (construction, agriculture), active cooling vests containing gel packs worn over the torso keep the core body temperature stable. This mitigates the central nervous system’s need to trigger massive vasodilation, thereby keeping insulin pharmacokinetics much closer to their normal baseline.
23. What is the best fast-acting carb to carry that won’t melt?
Pharmaceutical-grade glucose tablets are the gold standard. They do not melt, spoil, or freeze. Hard candies (like LifeSavers) or medical glucose gels are excellent secondary options. Never carry chocolate or gummy snacks in a heatwave, as they will melt into a lipid-rich paste that delays glucose absorption.
24. Can certain blood pressure medications make heat worse for diabetics?
Yes. Many diabetics take diuretics (like Hydrochlorothiazide) or ACE inhibitors for cardiovascular protection. Diuretics intentionally deplete fluid volume and sodium. When combined with excessive sweating from a heatwave, the patient is at critical risk for severe dehydration, orthostatic hypotension (fainting), and hyper-concentrated blood glucose.
25. How do I handle a sick day with a fever during a heatwave?
A physiological fever combined with environmental heat is a metabolic crisis. Fever induces massive insulin resistance, while external heat induces vasodilation. You must enforce strict indoor temperature control (AC), hydrate aggressively with electrolytes, monitor for ketones every 4 hours, and follow your endocrinologist’s advanced sick-day insulin protocols.
Medically Reviewed by Prof. Dr. Akram
Orthopedic Surgeon | Professor | Senior Medical Specialist
Prof. Dr. Akram is a distinguished surgeon with over 15 years of clinical expertise. Having served as a lead Emergency Specialist at Complex International Government Hospital, he currently leads a specialized team of 13 medical professionals at his private hospital. As a Professor at top medical universities, he ensures that every article on WellHealthOrg.com meets rigorous clinical standards.
Medical Disclaimer:
The information provided is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician for any medical concerns.
Our content is rigorously fact-checked by our 13-member Editorial Team under the clinical supervision of Prof. Dr. Akram.





