Chief Medical Content Strategist & Senior Neurologist | 30+ Years Clinical Experience
The Neurological Tipping Point: Decoding Hyperthermia
In my three decades as a neurologist, I have observed the human body endure extraordinary stress. Yet, few systemic failures are as rapid and devastating as acute hyperthermia. When comparing heatstroke vs heat exhaustion, the difference is literally life and death. Learn the life-saving warning signs to protect your brain and body before the biological thermostat shatters.
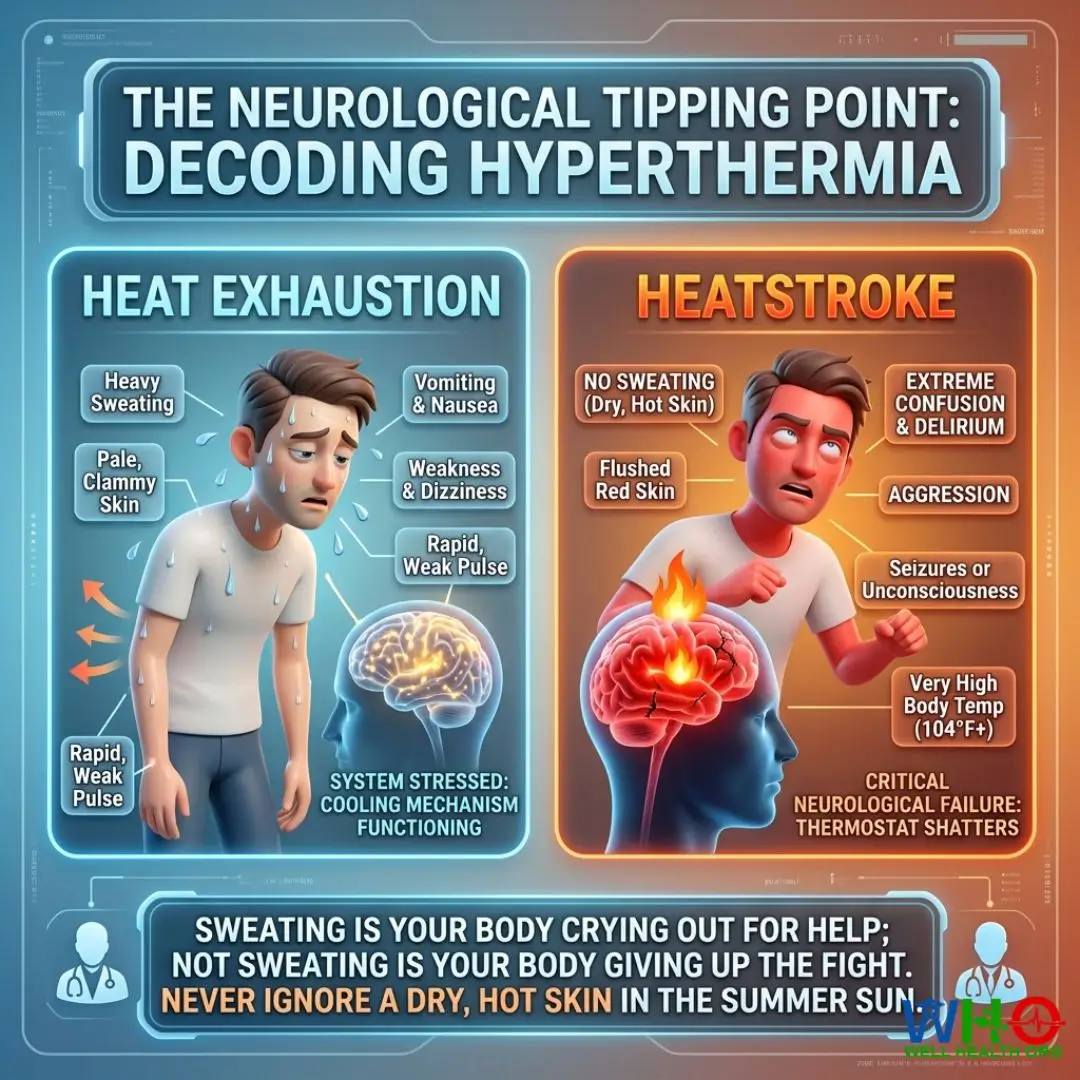
I recall a blistering July afternoon in the ER, early in my career. Two patients arrived simultaneously. Patient A was drenched in sweat, pale, and vomiting. Patient B was entirely dry, skin flushed bright red, completely delirious, and fighting the nurses. The untrained eye might assume Patient A, violently ill, was in worse shape. As a neurologist, I knew instantly that Patient B was minutes away from irreversible brain damage. Patient A was experiencing heat exhaustion; Patient B was suffering a full-blown heatstroke.
Understanding heatstroke vs heat exhaustion is not just a matter of first aid—it is a matter of neurological preservation. As the weather warms and global temperatures rise, your ability to recognize these life-saving warning signs will dictate your survival.
Shareable Insight: “Sweating is your body crying out for help; not sweating is your body giving up the fight. Never ignore a dry, hot skin in the summer sun.”
Interactive Clinical Directory (Jump-to-Section)
Brain Mechanics: How the Hypothalamus Fails
To truly grasp the severity of heatstroke vs heat exhaustion, we must look inside the brain—specifically at a tiny, almond-sized structure called the hypothalamus. This is your biological thermostat. When your internal body temperature rises, the hypothalamus sends electrical signals across your central nervous system to dilate blood vessels near the skin and activate sweat glands.
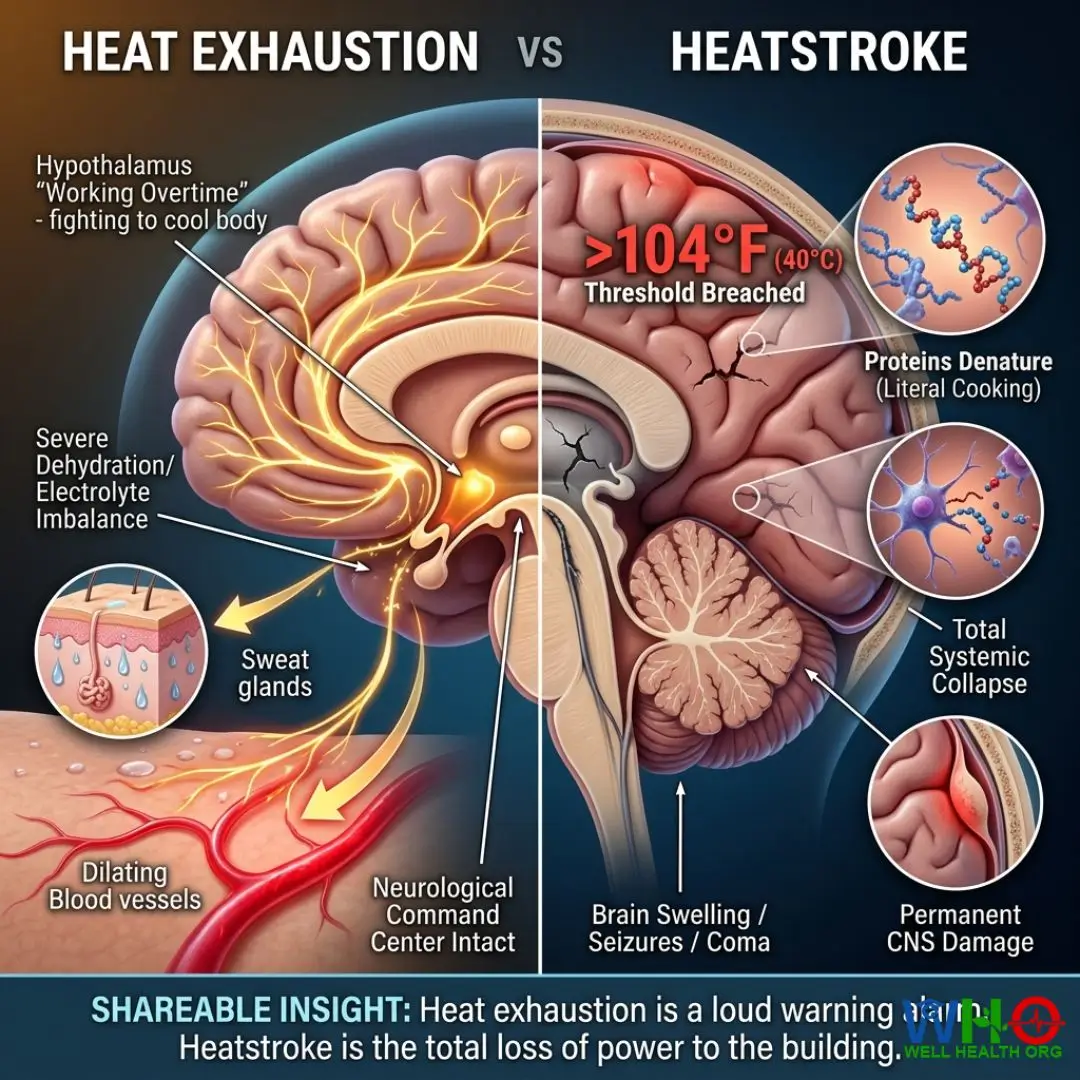
In heat exhaustion, your hypothalamus is working overtime. It is desperately pushing water and salt out of your pores to create evaporative cooling. You feel terrible—weak, nauseous, dizzy—but this is actually a sign that your brain is still fighting to keep you alive. You are experiencing severe dehydration and an electrolyte imbalance, but the neurological command center is intact.
In a heatstroke, we see total systemic collapse. The internal body temperature breaches 104°F (40°C). At this threshold, the proteins inside your brain cells begin to denature—literally cooking. The hypothalamus crashes. The sweating stops. The brain swells. Without immediate emergency medical care, the central nervous system damage becomes permanent, leading to seizures, coma, and multi-organ failure.
Shareable Insight: “Heat exhaustion is a loud warning alarm. Heatstroke is the total loss of power to the building.”
Differentiating the Symptoms: A Life-Saving Matrix
Let us dissect the exact warning signs. The clinical matrix below separates the localized struggle of exhaustion from the systemic emergency of a stroke. When analyzing heatstroke vs heat exhaustion, look for the following defining features:
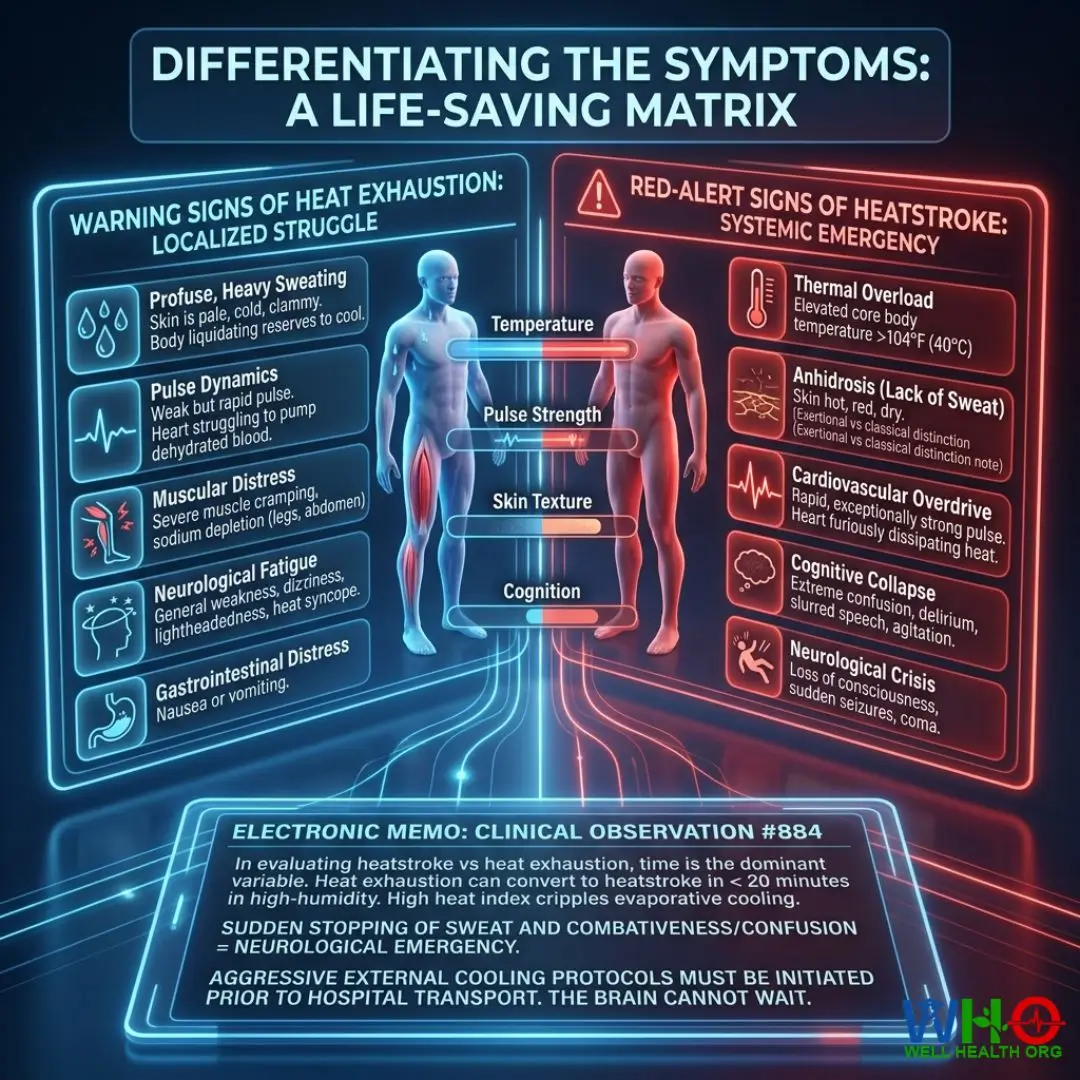
Warning Signs of Heat Exhaustion
- Profuse, Heavy Sweating: The skin is pale, cold, and clammy. The body is liquidating its reserves to cool down.
- Pulse Dynamics: A weak but rapid pulse or heart rate. The heart is struggling to pump thickened, dehydrated blood.
- Muscular Distress: Severe muscle cramping, often starting in the legs or abdomen, signaling massive sodium depletion.
- Neurological Fatigue: General weakness, dizziness, lightheadedness, and potential fainting (heat syncope).
- Gastrointestinal Distress: Nausea or vomiting.
Red-Alert Signs of Heatstroke
- Thermal Overload: Elevated core body temperature above 104°F (40°C).
- Anhidrosis (Lack of Sweat): The skin becomes hot, red, and dry. (Note: Exertional heatstroke may still present with moist skin, but non-exertional classical heatstroke results in bone-dry skin).
- Cardiovascular Overdrive: A rapid, exceptionally strong pulse. The heart is furiously trying to dissipate heat.
- Cognitive Collapse: Extreme confusion, delirium, slurred speech, or agitation.
- Neurological Crisis: Loss of consciousness, sudden seizures, and potential coma.
Electronic Memo: Clinical Observation #884
“In evaluating heatstroke vs heat exhaustion, time is the dominant variable. I have watched heat exhaustion convert to heatstroke in less than 20 minutes in a high-humidity environment. The heat index—factoring humidity with ambient temperature—cripples the body’s evaporative cooling mechanism. If a patient presenting with exhaustion suddenly stops sweating and becomes combative or confused, their condition has escalated to a neurological emergency. At this juncture, aggressive external cooling protocols must be initiated prior to hospital transport. The brain cannot wait.”
The Complete Clinical Remedial Ecosystem for Hyperthermia
In the emergency room, we do not view heat-related illness as a single event; we view it as a cascading spectrum of neurological and cellular failures. To halt this cascade, you must apply the correct biological intervention at the exact right time. Using a heatstroke protocol for a minor heat cramp is overkill, but using a heat cramp protocol for a heatstroke is a fatal error.
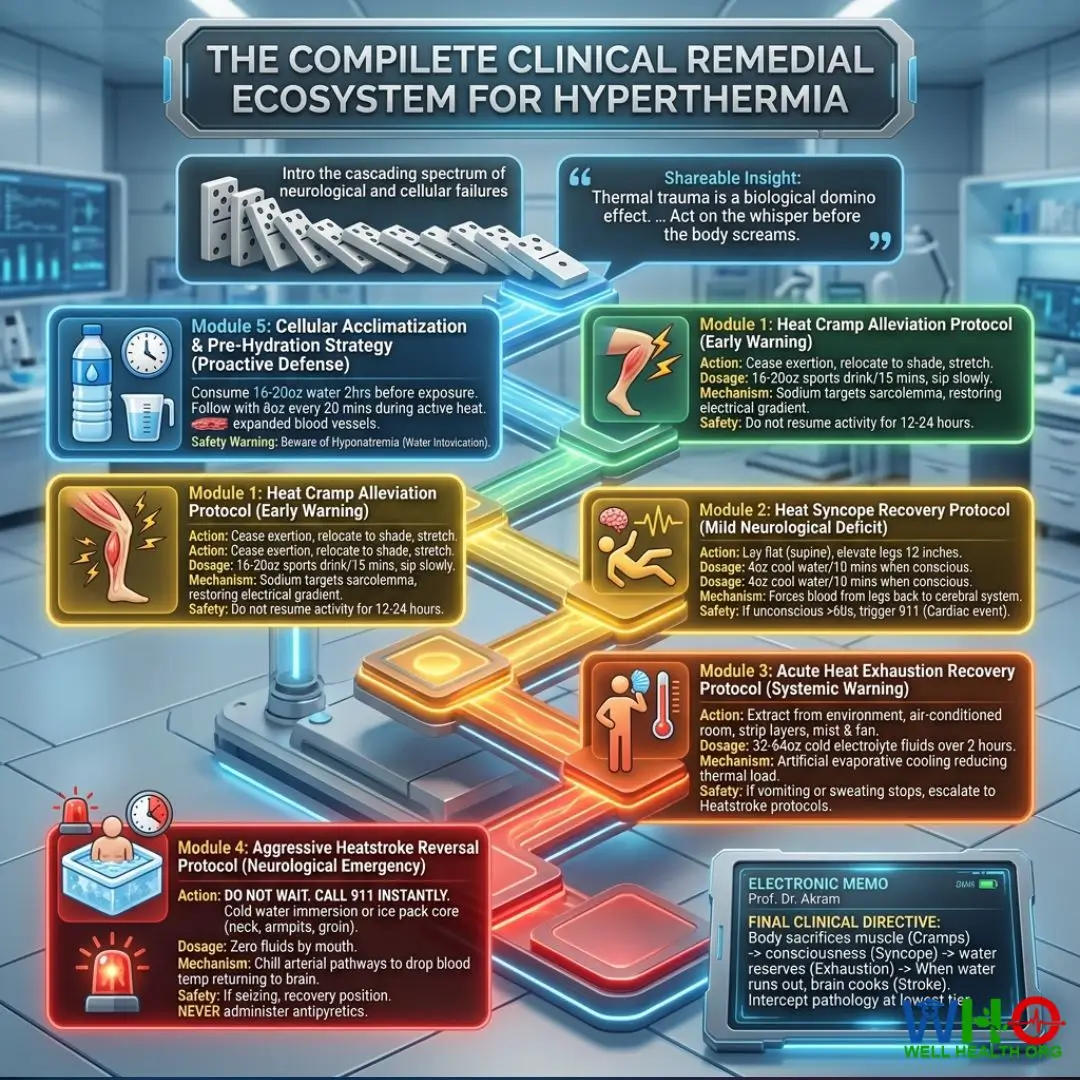
Below is my complete, unredacted clinical library of electronic remedy cards covering the entire spectrum of thermal trauma—from early muscular warnings to full-blown central nervous system collapse. Treat these protocols as your absolute medical baseline.
Shareable Insight: “Thermal trauma is a biological domino effect. If you stop the muscle cramp, you prevent the exhaustion. If you stop the exhaustion, you prevent the stroke. Act on the whisper before the body screams.”
Module 1: Heat Cramp Alleviation Protocol
Clinical Status: Early Warning (Muscular Distress)
- ⚡ How to Use (Clinical Application): Immediately cease all physical exertion. Relocate to a shaded area. Apply firm, sustained pressure and gentle stretching to the affected muscle groups (typically calves, hamstrings, or abdomen).
- ⚖️ Dosage & Quantity (Clinical Measurement): Consume 16 to 20 ounces of a carbohydrate-electrolyte beverage (sports drink) over a 15-minute window. Do not gulp; sip continuously.
- 🔬 Mechanism of Action (Electronic Biological Mapping): The sudden influx of sodium directly targets the sarcolemma (muscle cell membrane), restoring the cellular electrical gradient. This rapidly halts the involuntary fasciculations (spasms) caused by excessive sodium loss through sweat.
- 📈 Recovery Timeline (Projected Outcome): Muscular spasms should release entirely within 15 to 30 minutes.
- 🛠️ Preparation Guide (Laboratory Method): If commercial electrolyte solutions are absent, create an immediate saline-dextrose mix: 1 liter of water, 1/2 teaspoon of table salt, and a splash of fruit juice for glucose transporter activation.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): Do not resume strenuous activity for at least 12 to 24 hours after a severe cramp episode. Returning to the heat immediately will reliably trigger rapid-onset heat exhaustion.
Module 2: Heat Syncope (Fainting) Recovery Protocol
Clinical Status: Mild Neurological Deficit (Blood Pressure Drop)
- ⚡ How to Use (Clinical Application): Catch the individual if falling. Lay them flat on their back (supine position) in a cool environment. Elevate their legs 12 inches above the level of their heart. Loosen any tight collars, belts, or restrictive gear.
- ⚖️ Dosage & Quantity (Clinical Measurement): Once fully conscious and able to swallow safely, administer 4 ounces of cool water every 10 minutes.
- 🔬 Mechanism of Action (Electronic Biological Mapping): Heat syncope is caused by cutaneous vasodilation—blood rushing to the skin to cool the body, leaving the brain deprived of oxygen. Leg elevation physically forces pooled venous blood from the lower extremities back into the cerebral vascular system.
- 📈 Recovery Timeline (Projected Outcome): Consciousness should return within seconds of falling. Complete neurological clarity and stabilized blood pressure take 10 to 20 minutes.
- 🛠️ Preparation Guide (Laboratory Method): Use a cool, damp cloth applied directly to the forehead and back of the neck to stimulate the vagus nerve and promote parasympathetic nervous system recovery.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): If the patient remains unconscious for more than 60 seconds, or if they wake up experiencing chest pain, this is no longer a heat issue—it is a cardiac event. Trigger 911 immediately.
Module 3: Acute Heat Exhaustion Recovery Protocol
Clinical Status: Systemic Warning (Pre-Emergency)
- ⚡ How to Use (Clinical Application): Immediately extract the individual from the thermal environment. Relocate to an air-conditioned room. Strip off heavy outer layers. Induce active external cooling by misting the skin with water and placing them in front of a high-speed fan.
- ⚖️ Dosage & Quantity (Clinical Measurement): Target fluid intake is 32 to 64 ounces over a two-hour window. Serve cold, but not freezing, electrolyte-rich fluids.
- 🔬 Mechanism of Action (Electronic Biological Mapping): Misting the skin while fanning creates artificial evaporative cooling, drastically reducing the thermal load on the over-taxed hypothalamus. Oral fluids restore lost intravascular volume, thickening the blood pressure back to survival baseline.
- 📈 Recovery Timeline (Projected Outcome): Nausea, headache, and extreme fatigue should visibly dissipate within 45 to 60 minutes. Core temperature should drop below 100°F (37.7°C).
- 🛠️ Preparation Guide (Laboratory Method): Create cold compresses by soaking towels in ice water. Wring them out and apply directly to the axillae (armpits) and nape of the neck. Rotate towels every 5 minutes as they absorb body heat.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): If the patient begins vomiting, they cannot retain oral fluids, leading to inevitable dehydration. If vomiting occurs, or if heavy sweating suddenly stops, escalate to Module 4 (Heatstroke) protocols immediately.
Module 4: Aggressive Heatstroke Reversal Protocol
Clinical Status: Neurological Emergency (Life-Threatening)
- ⚡ How to Use (Clinical Application): DO NOT WAIT. Call emergency services (911) instantly. While waiting, bypass the patient’s failed internal cooling system. Immerse the patient in a cold water bath, or pack their core (neck, armpits, groin) with ice.
- ⚖️ Dosage & Quantity (Clinical Measurement): Zero fluids by mouth. Apply maximum possible external cold load. If using ice packs, use at least 6 to 8 large packs targeting the major arterial pathways.
- 🔬 Mechanism of Action (Electronic Biological Mapping): Extreme hyperthermia denatures brain proteins. By chilling the carotid, axillary, and femoral arteries, you physically drop the temperature of the blood returning to the brain, halting cellular destruction and preventing coma.
- 📈 Recovery Timeline (Projected Outcome): The absolute clinical mandate is to drop the core body temperature below 102°F (38.9°C) within the first 30 minutes. Survival rates plummet exponentially after this window.
- 🛠️ Preparation Guide (Laboratory Method): In athletic or military settings, the gold standard is “Cold Water Immersion.” Fill a tub with water and ice (50/50 mix). Submerge the patient up to their chest. Vigorously stir the water to disrupt the warm thermal layer that forms around their skin.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): Heatstroke causes severe neurological misfiring. If the patient begins seizing, do not restrain them forcefully. Protect their head from concrete or hard surfaces. Roll them onto their side (recovery position) to prevent them from drowning in their own saliva. NEVER administer antipyretics (Aspirin/Tylenol)—they will destroy the already failing liver.
Module 5: Cellular Acclimatization & Pre-Hydration Strategy
Clinical Status: Proactive Defense (Thermoregulatory Conditioning)
- ⚡ How to Use (Clinical Application): This protocol must be executed *before* stepping into a high-heat environment. It conditions the hypothalamus to expect thermal stress and arms the body with the necessary vascular volume to sweat efficiently.
- ⚖️ Dosage & Quantity (Clinical Measurement): Consume exactly 16 to 20 ounces of water 2 hours before extreme heat exposure. Follow this with 8 ounces of water or sports drink every 20 minutes during active heat exposure.
- 🔬 Mechanism of Action (Electronic Biological Mapping): Pre-hydration expands blood plasma volume. A higher plasma volume ensures the heart does not have to work as hard to pump blood to the skin (for cooling) and to the muscles (for movement) simultaneously. It keeps the biological cooling reservoir fully stocked.
- 📈 Recovery Timeline (Projected Outcome): Over a period of 7 to 14 days of gradual heat exposure combined with this hydration protocol, the body “acclimatizes.” Sweat glands adapt to produce more sweat, faster, while actively hoarding vital sodium instead of sweating it out.
- 🛠️ Preparation Guide (Laboratory Method): Weigh yourself before and after rigorous outdoor activity. For every pound of body weight lost during the activity, you have lost roughly 16 ounces of fluid. Consume 20 to 24 ounces of fluid to replace each lost pound to achieve cellular equilibrium.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): Beware of “Water Intoxication” (Hyponatremia). If you consume massive amounts of plain water (over 1 liter per hour) without consuming any sodium or food, you will dilute your blood sodium to fatal levels, causing brain swelling that mimics heatstroke. Always balance heavy water intake with electrolyte replacement.
Electronic Memo: Final Clinical Directive
“I instruct all my medical students to memorize this progression: The body will sacrifice the muscle to save the blood volume (Cramps). It will sacrifice consciousness to reset blood pressure (Syncope). It will sacrifice all internal water reserves to cool the brain (Exhaustion). When the water runs out, the brain cooks (Stroke). Your job is to intercept the pathology at the lowest possible tier using the precise remedial module above.”
— Prof. Dr. Akram
Regional Medical Intelligence (Localized Dropdowns)
To ensure this life-saving data reaches across linguistic barriers, I have formatted the heatstroke vs heat exhaustion protocols into localized, easily shareable summary components.
🇮🇳 Hindi (हिंदी): Heatstroke vs Heat Exhaustion Summary
- 1. हीट एग्जॉशन (Heat Exhaustion) में बहुत ज्यादा पसीना आता है।
- 2. हीटस्ट्रोक (Heatstroke) में पसीना आना बंद हो जाता है, त्वचा लाल और सूखी हो जाती है।
- 3. हीट एग्जॉशन एक चेतावनी है, जबकि हीटस्ट्रोक एक जानलेवा मेडिकल इमरजेंसी है।
- 4. चक्कर आना, उल्टी होना और कमजोरी हीट एग्जॉशन के लक्षण हैं।
- 5. बेहोशी, भ्रम और दौरे पड़ना हीटस्ट्रोक के संकेत हैं।
- 6. हीट एग्जॉशन होने पर तुरंत ठंडी जगह पर जाएं।
- 7. पैरों को दिल के स्तर से ऊपर उठाकर लेट जाएं।
- 8. ओआरएस (ORS) या इलेक्ट्रोलाइट्स वाला पानी पिएं।
- 9. यदि लक्षण 30 मिनट में ठीक न हों, तो डॉक्टर को बुलाएं।
- 10. हीटस्ट्रोक के मरीज को भूलकर भी कुछ पीने को न दें, सांस नली में पानी जा सकता है।
- 11. हीटस्ट्रोक में तुरंत एम्बुलेंस (911/108) को कॉल करें।
- 12. मरीज के कपड़े ढीले करें और गर्दन, बगल, और जांघों पर बर्फ लगाएं।
- 13. बुखार कम करने वाली दवाइयां (जैसे पेरासिटामोल) हीटस्ट्रोक में न दें।
- 14. शराब और कैफीन का सेवन गर्मी में शरीर को डिहाइड्रेट करता है।
- 15. बाहर निकलते समय ढीले, हल्के रंग के सूती कपड़े पहनें।
🇮🇳 Hinglish: Quick Shareable Summary
- 1. Heat exhaustion aur heatstroke ke beech ka farq jaan bachane wala hai.
- 2. Exhaustion mein body se bahut sweat nikalta hai, skin thandi aur clammy hoti hai.
- 3. Heatstroke mein sweating ruk jati hai, skin red, dry aur garam ho jati hai.
- 4. Agar kisi ko confusion ho raha hai ya faint ho raha hai, toh yeh stroke hai.
- 5. Exhaustion wale ko turant AC room ya shade mein le jayein.
- 6. Thanda pani ya sports drink sips mein pilayein.
- 7. Patient ke legs ko thoda upar elevate karke litayein blood flow ke liye.
- 8. Agar patient ulti (vomit) kar raha hai, toh use fluids mat dein.
- 9. Heatstroke ek absolute medical emergency hai. Turant ambulance bulayein.
- 10. Ambulance aane tak, patient ki neck, armpits aur groin par ice packs lagayein.
- 11. Heatstroke patient ko pani peene ko NA dein, choking ho sakti hai.
- 12. Aspirin ya Paracetamol fever kam karne ke liye bilkul use mat karein.
- 13. Bachon aur bujurgon (65+) ko extreme heat se sabse zyada khatra hota hai.
- 14. Bahar nikalte waqt light-colored cotton clothes aur wide-brimmed hat pehnein.
- 15. High humidity mein sweat evaporate nahi hota, isliye aur alert rahein.
Advanced Hospital Diagnostics
Once a patient transitions from the field to the Emergency Department, our clinical protocols shift from stabilization to investigation. Diagnosing the exact severity of heatstroke vs heat exhaustion requires high-resolution biological data.
As a specialist, I look beyond the external thermometer. We execute rapid blood panels to assess sodium and potassium levels. Severe dehydration creates massive electrolyte imbalances that threaten cardiac rhythm. We analyze the patient’s urine; a dark amber output indicates profound kidney strain, while the presence of myoglobin points to rhabdomyolysis—a terrifying complication where cooked muscle tissue breaks down and clogs the renal filters.
Furthermore, muscle function tests and internal imaging (X-rays, ultrasounds) are mandated if the core temperature remained above 104°F for a sustained period. Heatstroke literally melts cellular walls. We must rule out hepatic (liver) and renal (kidney) failure.
Prevention & Acclimatization Protocols
The truest cure for heat-related illnesses is aggressive prevention. The body is an adaptable machine, but it requires strategic conditioning.
Cellular Hydration Mechanics
Do not wait for the sensation of thirst. Thirst is a lagging indicator—by the time your brain signals you to drink, you are already 1-2% dehydrated. Drink 2 to 4 cups of water every hour when exposed to high temperatures. Avoid alcohol and heavy caffeine. Both are powerful diuretics that command your kidneys to flush water out of your system, sabotaging your body’s attempt to build an internal coolant reservoir.
Demographic Vulnerabilities
Understand that your risk profile dictates your required vigilance.
- Age Dynamics: Infants under 4 and adults over 65 have compromised central nervous systems that process thermal regulation inefficiently.
- Pharmacology: Prescription medications like beta-blockers, diuretics, and certain psychiatric drugs severely impair the body’s ability to sweat or regulate blood flow.
- Adipose Tissue (Obesity): Excess body fat acts as deep insulation, trapping core heat and making rapid cooling incredibly difficult.
Shareable Insight: “Never leave a human or pet in a parked vehicle. Ambient heat can spike the internal car temperature to fatal levels in under 10 minutes, triggering acute heatstroke.”
25 High-Yield Clinical FAQs: Mastering Heatstroke vs Heat Exhaustion
Below, I have meticulously curated the 25 most critical questions patients ask regarding heatstroke vs heat exhaustion. Each answer is anchored in clinical neurology and emergency medicine protocols.
1. What is the single biggest difference between heatstroke vs heat exhaustion?
The defining difference is the body’s ability to cool itself. In heat exhaustion, the body sweats profusely to regulate temperature. In heatstroke, the cooling mechanism fails entirely, sweating stops, and the core temperature skyrockets to fatal levels.
2. At what temperature does heat exhaustion turn into heatstroke?
A core body temperature reading of 104°F (40°C) or higher is the clinical threshold for heatstroke. Above this temperature, cellular damage begins in the brain and vital organs.
3. Can you have heatstroke while still sweating?
Yes, in cases of “exertional heatstroke” (usually seen in athletes or laborers working intensely in heat), the skin may still feel moist. However, classical “non-exertional heatstroke” typically presents with completely dry, hot skin.
4. Why shouldn’t I give water to someone suffering a heatstroke?
A heatstroke compromises the central nervous system, meaning the patient’s swallowing reflex is impaired. Giving them water creates a high risk of aspiration, where the fluid goes into their lungs instead of their stomach.
5. How quickly can heat exhaustion escalate?
In high heat and extreme humidity, heat exhaustion can cascade into full heatstroke in under 30 to 60 minutes if the person is not removed from the environment and cooled down.
6. What is the primary cause of muscle cramps in the heat?
Heat cramps are caused by immense sodium and electrolyte depletion through sweat. Muscles require precise electrical signals to contract and relax; without sodium, the muscles spasm violently.
7. Are children more at risk for these conditions?
Absolutely. Children under 4 possess a smaller body mass to surface area ratio, meaning they absorb heat faster than adults, and their hypothalamic temperature regulation is immature.
8. How does high humidity affect body temperature regulation?
Sweating cools you down only when the sweat evaporates off your skin. High humidity heavily saturates the air with moisture, preventing your sweat from evaporating, thereby disabling your cooling system.
9. Can I use Tylenol or Aspirin to lower a heatstroke fever?
No. Fever-reducing medications target the hypothalamus during an infection. They do absolutely nothing for environmental hyperthermia and can actually trigger rapid liver or kidney failure in a heatstroke patient.
10. What is “heat syncope”?
Heat syncope is a fainting episode or severe dizziness caused by standing too long in the heat. Blood pools in the lower extremities, causing a temporary drop in blood flow to the brain.
11. Why do we apply ice to the armpits and groin during emergency care?
The axillary (armpit) and femoral (groin) arteries are massive blood vessels located very close to the surface of the skin. Cooling these areas rapidly cools the blood returning to the heart and brain.
12. Does drinking alcohol increase my risk of heat-related illness?
Yes. Alcohol is a diuretic, forcing the body to excrete fluids through urine. It also impairs judgment, making individuals less likely to notice early warning signs of heat exhaustion.
13. Is permanent brain damage possible from a heatstroke?
Tragically, yes. If the core temperature remains above 104°F for a prolonged period, proteins in the brain denature, leading to irreversible neurological deficits, persistent vegetative states, or death.
14. What color should my urine be to ensure adequate hydration?
Your urine should be a pale, translucent yellow (like lemonade). Dark yellow, amber, or brown urine is a severe warning sign of deep dehydration and potential kidney strain.
15. Why do certain medications make me more susceptible to heat?
Drugs like antihistamines, beta-blockers, and diuretics alter blood flow or suppress the sweat glands. If you take medication for blood pressure or psychiatric conditions, consult your doctor regarding heat exposure.
16. What is the role of the hypothalamus in hyperthermia?
The hypothalamus acts as the body’s internal thermostat. In heat exhaustion, it triggers sweating. In a stroke, the extreme heat causes the hypothalamus to crash, halting all self-cooling mechanisms.
17. How should I dress to prevent these conditions outdoors?
Wear lightweight, loose-fitting, and light-colored clothing. Dark colors absorb radiant solar heat, while tight clothing prevents air circulation necessary for sweat evaporation.
18. What is heat acclimatization?
Acclimatization is the biological process of slowly adapting to a hotter environment. Over 7 to 14 days of gradual exposure, your body learns to sweat earlier, sweat more, and lose fewer electrolytes.
19. Should I drink sports drinks or just plain water?
If you are sweating profusely for over an hour, sports drinks containing electrolytes (sodium, potassium) are vastly superior to plain water, as they replace the critical salts lost through the pores.
20. How long does it take to fully recover from heat exhaustion?
With immediate resting and rehydration, core symptoms dissipate in an hour. However, clinical fatigue and heat sensitivity can linger for 24 to 48 hours, requiring extended rest.
21. If someone is seizing from heatstroke, what do I do?
Ensure their airway is clear, roll them onto their side to prevent choking on saliva, protect their head from striking the ground, and actively cool their body. Do not put anything in their mouth.
22. What is rhabdomyolysis in relation to extreme heat?
Rhabdomyolysis occurs when thermal trauma breaks down muscle tissue, releasing a protein called myoglobin into the blood. This protein heavily damages the kidneys, often turning urine dark tea-colored.
23. Can indoor heat cause these conditions?
Absolutely. Poorly ventilated factories, kitchens, and homes lacking air conditioning during a heatwave routinely generate life-threatening hyperthermia, particularly among the elderly.
24. Why is elevating the legs helpful for heat exhaustion?
Elevating the legs harnesses gravity to push pooled blood from the lower extremities back to the heart and brain, rapidly resolving lightheadedness and maintaining blood pressure.
25. Once I survive a heatstroke, am I more sensitive to heat in the future?
Yes. A severe heatstroke causes micro-damage to the hypothalamus. Clinical studies suggest survivors often experience a lowered tolerance for high temperatures and must remain permanently hyper-vigilant.
© 2026 Dr. Akram Medical Strategy Group. All Rights Reserved.
Medically Reviewed by Prof. Dr. Akram
Orthopedic Surgeon | Professor | Senior Medical Specialist
Prof. Dr. Akram is a distinguished surgeon with over 15 years of clinical expertise. Having served as a lead Emergency Specialist at Complex International Government Hospital, he currently leads a specialized team of 13 medical professionals at his private hospital. As a Professor at top medical universities, he ensures that every article on WellHealthOrg.com meets rigorous clinical standards.
Medical Disclaimer:
The information provided is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician for any medical concerns.
Our content is rigorously fact-checked by our 13-member Editorial Team under the clinical supervision of Prof. Dr. Akram.







