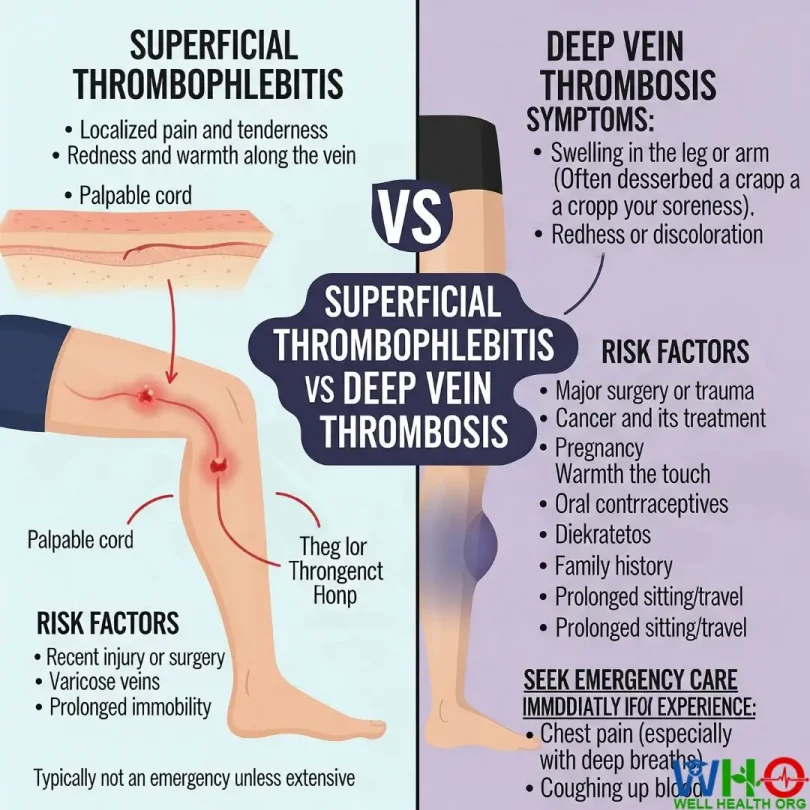
When you experience leg pain, swelling, or skin discoloration, it’s natural to worry. These symptoms can point to a variety of conditions — some relatively harmless, others potentially life-threatening. Among the most important to recognize are superficial thrombophlebitis vs deep vein thrombosis.
- Understanding the Basics: What Are These Conditions?
- Deep Vein Thrombosis (DVT)
- Superficial Thrombophlebitis (ST)
- Key Distinction
- Causes and Risk Factors: Why Do These Conditions Develop?
- Deep Vein Thrombosis (DVT) Risk Factors
- Superficial Thrombophlebitis (ST) Risk Factors
- Recognizing the Symptoms: When to Be Concerned
- Deep Vein Thrombosis (DVT) Symptoms
- Superficial Thrombophlebitis (ST) Symptoms
- Diagnostic Methods: How Doctors Tell the Difference
- 1. Clinical Examination
- 2. Ultrasound Imaging
- 3. D-dimer Blood Test
- 4. Additional Imaging (Rarely Needed)
- Treatment Approaches: Tailored Care for Each Condition
- Deep Vein Thrombosis (DVT) Treatment
- Superficial Thrombophlebitis (ST) Treatment
- Potential Complications: Understanding the Stakes
- Complications of Deep Vein Thrombosis (DVT)
- Complications of Superficial Thrombophlebitis (ST)
- Prevention Strategies: Reducing Your Risk
- Lifestyle Changes for Everyone
- Travel & Work-Related Prevention
- Medical Prevention for High-Risk Individuals
- When to Seek Medical Attention
- Seek Emergency Care Immediately If You Have:
- Contact Your Doctor Promptly If You Notice:
- Taking Action for Your Vascular Health
- FAQs About DVT vs ST
At first glance, these two vascular conditions may seem similar. Both involve blood clot formation in the veins, and both can cause swelling, redness, and discomfort. However, the severity, underlying risks, and treatment strategies differ significantly. While ST is usually a mild condition that resolves with conservative care, DVT requires urgent medical attention because it can lead to pulmonary embolism (PE) — a complication that can be fatal if left untreated.
This in-depth guide will break down the causes, risk factors, symptoms, diagnosis, treatments, and complications of each condition. By the end, you’ll not only understand the differences between ST and DVT, but also know when to seek medical care and how to protect your vascular health in the long term.
Understanding the Basics: What Are These Conditions?
Before comparing the two, let’s clearly define them.
Deep Vein Thrombosis (DVT)
DVT occurs when a blood clot (thrombus) forms in a deep vein, typically in the legs, thighs, or pelvis. These veins lie far beneath the skin’s surface and play a critical role in transporting blood back to the heart. A clot here can partially or completely block blood flow, creating serious risks. If a piece of the clot breaks off and travels to the lungs, it can cause a pulmonary embolism, a potentially deadly condition that requires immediate emergency care.
DVT is not rare — it affects hundreds of thousands of people each year, and because it sometimes develops without noticeable symptoms, it is often referred to as a “silent threat.”
Superficial Thrombophlebitis (ST)
By contrast, ST involves inflammation in veins located just beneath the skin’s surface. Unlike deep veins, superficial veins don’t carry large volumes of blood, which means clots here are far less likely to break loose and cause life-threatening complications.
In ST, the vein may become painful, hard, red, and cord-like to the touch. While often considered benign, it shouldn’t be dismissed completely. In certain cases, ST can extend into deeper veins or occur alongside DVT, which is why medical evaluation remains important.
Key Distinction
The main difference lies in location and risk:
- DVT = Deep veins, high risk, medical emergency
- ST = Superficial veins, lower risk, often self-limiting
However, since both can present with overlapping symptoms, it’s not always possible to self-diagnose. That’s why professional medical assessment is critical.
Causes and Risk Factors: Why Do These Conditions Develop?
Blood clot formation is rarely random. It usually happens when one or more elements of Virchow’s Triad — a classic medical concept — are present:
- Stasis of blood flow (when blood isn’t moving properly)
- Damage to vein walls
- Hypercoagulability (increased tendency of blood to clot)
Both DVT and ST are influenced by these factors, though specific triggers differ.
Deep Vein Thrombosis (DVT) Risk Factors
DVT typically develops in settings where circulation slows or vein damage occurs. The Centers for Disease Control and Prevention (CDC) highlights several key contributors:
- Injury or Surgery: Fractures, muscle trauma, or major operations can damage vein walls. Post-surgical immobility also heightens risk.
- Prolonged Inactivity: Sitting during long flights or car rides, extended bed rest, or paralysis slows venous return, giving blood more opportunity to clot.
- Hormonal Influences: High estrogen levels (from oral contraceptives, hormone replacement therapy, pregnancy, or postpartum changes) increase clotting potential.
- Medical Conditions: Cancer, chronic heart or lung disease, inflammatory bowel disease, and inherited clotting disorders (like Factor V Leiden) all raise DVT risk.
- Other Factors: Age, obesity, central venous catheters, smoking, family history of clots, or previous DVT/PE episodes make recurrence more likely.
⚠️ Importantly, having multiple risk factors multiplies your risk rather than adding to it. For instance, a sedentary, overweight smoker recovering from surgery is far more vulnerable than someone with just one isolated risk factor.
Superficial Thrombophlebitis (ST) Risk Factors
Superficial thrombophlebitis tends to arise from more localized issues affecting surface veins:
- Varicose Veins: These enlarged, twisted veins create areas of poor circulation where clots and inflammation can develop. ST is particularly common among people with longstanding varicose veins.
- IV Lines or Injections: Medical procedures involving cannulas, IV drips, or vein punctures can irritate the vein lining, leading to inflammation.
- Clotting Disorders: Inherited or acquired conditions that increase clotting risk (like thrombophilia) predispose individuals to both ST and DVT.
- Autoimmune Diseases: Conditions like Behçet’s disease or systemic vasculitis can inflame multiple blood vessels, including superficial ones.
- Other Contributors: Older age, obesity, pregnancy, cancer, or prior episodes of phlebitis all raise the likelihood of ST.
While ST is less likely than DVT to lead to severe outcomes, it is not always harmless. Studies show that some patients with ST also have silent DVT, which is why ultrasound testing is often recommended.
Recognizing the Symptoms: When to Be Concerned
One of the biggest challenges in distinguishing DVT from ST is that their symptoms often overlap. Both can cause pain, swelling, and redness in the affected limb. But there are subtle differences in severity, progression, and distribution that help doctors tell them apart.
Deep Vein Thrombosis (DVT) Symptoms
DVT can be tricky — some people develop large clots without any obvious signs. In fact, research suggests more than 50% of DVT cases may initially be “silent”. This makes it especially dangerous since the first noticeable symptom might actually be a pulmonary embolism.
When symptoms are present, they usually occur in the leg or thigh where the clot has formed:
- Persistent swelling: The affected leg (or arm, in rare cases) may appear noticeably larger than the other.
- Pain or tenderness: Often felt as a cramp-like sensation, heaviness, or throbbing that worsens when walking or standing.
- Skin changes: Redness, purplish discoloration, or a shiny appearance.
- Warmth: The skin over the clot may feel hotter than surrounding areas.
- Distended veins: Superficial veins may appear more visible or bulging due to blocked blood flow beneath.
🚨 Emergency Signs (Pulmonary Embolism): If a clot breaks off and travels to the lungs, symptoms may include:
- Sudden shortness of breath
- Chest pain that worsens with deep breathing
- Coughing (sometimes with blood-streaked sputum)
- Rapid heartbeat or lightheadedness
For some patients, these PE symptoms are the first sign of a hidden DVT, which is why any sudden leg swelling or pain should never be ignored.
Superficial Thrombophlebitis (ST) Symptoms
ST usually develops gradually and locally, affecting veins near the surface of the skin. Unlike DVT, symptoms are less likely to be life-threatening but can still cause significant discomfort.
Typical features include:
- Localized pain and tenderness: You can often pinpoint the exact vein that feels sore or hardened.
- Swelling along the vein: Unlike DVT, this swelling usually follows the path of a visible superficial vein.
- Redness and warmth: The skin above the inflamed vein may look red and feel warmer than the surrounding area.
- Cord-like texture: The affected vein may feel like a firm, rope-like structure under the skin.
- Mild itching or irritation: Some people describe a persistent itchiness near the inflamed vein.
Unlike DVT, ST does not usually cause extensive swelling of the entire leg. Instead, the discomfort stays confined to the surface vein involved. However, if symptoms spread or worsen quickly, it may signal that the condition is extending into deeper veins.
Diagnostic Methods: How Doctors Tell the Difference
Because DVT can mimic ST and vice versa, relying on symptoms alone isn’t enough. Doctors use a combination of clinical evaluation and imaging tests to make an accurate diagnosis.
1. Clinical Examination
A doctor will begin with a detailed medical history and physical assessment. They’ll ask about:
- Recent surgery, travel, or periods of immobility
- Use of birth control pills, hormone therapy, or pregnancy history
- Prior blood clot episodes or family history of clotting disorders
- Visible signs like swelling, redness, or palpable cord-like veins
Doctors sometimes use scoring systems such as the Wells Score for DVT, which assigns points based on symptoms and risk factors. A higher score suggests a stronger likelihood of DVT.
2. Ultrasound Imaging
The gold standard for both DVT and ST diagnosis is Doppler ultrasound. This painless, non-invasive test uses sound waves to:
- Visualize the clot inside the vein
- Determine whether blood flow is blocked or slowed
- Differentiate between superficial and deep vein involvement
Ultrasound is so effective that most guidelines recommend it for any patient suspected of having DVT or ST, especially since ST can sometimes overlap with DVT.
3. D-dimer Blood Test
This test measures a protein fragment released when clots break down. Elevated levels suggest that a clot may be present. While highly sensitive, it isn’t specific — meaning it can be elevated in other conditions like infections, recent surgery, or inflammation. For this reason, it’s often used in combination with imaging rather than as a standalone test.
4. Additional Imaging (Rarely Needed)
In unusual or complex cases, doctors may order:
- CT or MRI venography for detailed visualization of blood flow
- Contrast venography (less common today, as it’s more invasive)
⚠️ A critical point: Studies reveal that up to 25% of patients with superficial thrombophlebitis may also have an undiagnosed DVT. That’s why many vascular specialists insist on an ultrasound for all cases of ST, not just DVT.
Treatment Approaches: Tailored Care for Each Condition
The management of DVT and ST differs because their risks and outcomes are not the same. DVT requires aggressive treatment to prevent fatal complications, whereas ST can often be managed with conservative care and monitoring.
Deep Vein Thrombosis (DVT) Treatment
The goals of DVT treatment are to:
- Stop the clot from growing
- Prevent the clot from breaking loose and causing pulmonary embolism
- Reduce long-term complications like post-thrombotic syndrome
Common treatment strategies include:
- Anticoagulants (Blood Thinners):
The first-line therapy. Medications like heparin, warfarin, and direct oral anticoagulants (DOACs) help prevent new clots while allowing the body to gradually break down existing ones. Most patients require at least 3–6 months of therapy, sometimes longer if risk factors persist. - Thrombolytic Therapy:
In severe cases, doctors may use clot-busting drugs (like alteplase) that dissolve the clot quickly. This is usually reserved for massive DVTs or clots threatening limb survival, due to the higher bleeding risk. - Surgical or Interventional Options:
Procedures like thrombectomy (clot removal) or insertion of an IVC filter (to catch clots before they reach the lungs) may be considered if anticoagulants aren’t safe or effective. - Lifestyle and Supportive Care:
Wearing compression stockings, staying active, and elevating the affected leg help improve blood flow and reduce swelling.
Superficial Thrombophlebitis (ST) Treatment
ST is generally less dangerous and may resolve within 1–2 weeks without aggressive intervention. However, treatment depends on severity and risk of progression:
- Conservative Home Remedies:
- Warm compresses to soothe discomfort
- Leg elevation to reduce swelling
- Regular walking to keep blood circulating
- Over-the-counter pain relievers (when approved by a doctor)
- Compression Stockings:
Support circulation, reduce inflammation, and minimize discomfort. - Topical or Oral Anti-Inflammatories:
Creams, gels, or oral medications may help reduce pain and swelling. - Anticoagulants (for high-risk patients):
In cases where ST is extensive, recurrent, or close to deep veins, doctors may prescribe low-dose anticoagulants to prevent progression into DVT.
Potential Complications: Understanding the Stakes
Both DVT and ST can lead to complications, but the severity and long-term consequences differ greatly. Recognizing these risks is essential to motivate timely medical care and lifestyle adjustments.
Complications of Deep Vein Thrombosis (DVT)
DVT carries significant risks because the clot forms in major blood vessels. If untreated, it can cause:
- Pulmonary Embolism (PE):
- The most feared complication.
- Occurs when a piece of the clot breaks off and travels to the lungs, blocking blood flow.
- Symptoms include sudden chest pain, shortness of breath, dizziness, or coughing up blood.
- PE can be fatal within hours if not treated promptly.
- Post-Thrombotic Syndrome (PTS):
- A long-term complication caused by vein valve damage after a clot.
- Symptoms: chronic swelling, skin discoloration, heaviness, and even painful ulcers.
- About 1 in 3 DVT patients will develop PTS, sometimes years after the clot.
- Recurrent DVT:
- Once someone has had a DVT, the chance of another clot increases.
- Studies suggest about 30% of patients experience recurrence within 10 years.
- Preventive strategies and regular monitoring are critical.
- Chronic Venous Insufficiency:
- A condition where blood pools in the legs due to vein damage.
- Leads to varicose veins, swelling, and skin changes.
In short, DVT isn’t just a one-time emergency — it can cause lifelong vascular problems if not treated and monitored properly.
Complications of Superficial Thrombophlebitis (ST)
While ST is usually less serious, it can still cause issues, especially if ignored:
- Progression to DVT:
- In some cases, ST can extend into deeper veins, becoming a full-blown DVT.
- This risk is higher if the clot is close to the junction where superficial and deep veins meet.
- Recurrent ST:
- Patients with underlying risk factors, like varicose veins or clotting disorders, may develop repeated episodes.
- Chronic recurrence can affect quality of life and indicate deeper vascular issues.
- Secondary Infection (Thrombophlebitis Septica):
- Rare but possible when bacteria infect the inflamed vein.
- Leads to redness, pus, fever, and worsening pain.
- Requires antibiotics and sometimes drainage.
- Skin Damage:
- Prolonged inflammation can lead to hardening, discoloration, or thickened skin.
Although ST rarely poses immediate life-threatening danger, it should never be brushed off, especially in people with a history of clotting or vascular disease.
Prevention Strategies: Reducing Your Risk
The good news? Both DVT and ST can often be prevented with the right habits and medical guidance. Whether you’re recovering from surgery, traveling long distances, or managing chronic conditions, these steps can make a real difference.
Lifestyle Changes for Everyone
- Stay Active: Avoid sitting or standing for long periods. Simple leg movements, walking breaks, or stretching can keep blood flowing.
- Hydrate Well: Dehydration makes blood thicker, increasing clot risk. Drink enough water, especially during travel or hot weather.
- Maintain a Healthy Weight: Obesity is a major risk factor. Even modest weight loss improves circulation.
- Exercise Regularly: Activities like walking, swimming, or cycling strengthen leg muscles, which pump blood more effectively.
- Quit Smoking: Smoking damages blood vessels and makes clots more likely.
Travel & Work-Related Prevention
Long flights, car rides, or desk jobs can increase clot risk. Protect yourself with:
- Frequent Movement: Stand up and walk every 1–2 hours.
- Calf Exercises: Flex and extend your ankles while sitting.
- Compression Stockings: Especially recommended for frequent flyers or those with varicose veins.
Medical Prevention for High-Risk Individuals
Doctors may recommend preventive strategies if you are at increased risk:
- Blood-Thinning Medications: For patients after surgery, during hospitalization, or with clotting disorders.
- Compression Devices in Hospitals: Inflatable sleeves that massage the legs to improve circulation.
- Managing Underlying Conditions: Treating varicose veins, heart disease, or cancer can lower clotting risks.
When to Seek Medical Attention
Knowing when to seek help is just as important as prevention. Here’s a quick guide:
Seek Emergency Care Immediately If You Have:
- Sudden or unexplained swelling in one leg
- Severe leg pain or cramping
- Red or discolored skin with heat and tenderness
- Symptoms of pulmonary embolism: chest pain, shortness of breath, coughing blood, or fainting
These could signal DVT or PE, which require urgent hospital treatment.
Contact Your Doctor Promptly If You Notice:
- Painful, red, or hardened superficial veins (possible ST)
- Recurring vein inflammation or swelling
- ST symptoms that spread or worsen
- Fever or pus near an inflamed vein
While ST isn’t typically an emergency, evaluation is important to rule out hidden DVT.
Taking Action for Your Vascular Health
At the end of the day, the main difference between superficial thrombophlebitis and deep vein thrombosis lies in their severity and danger.
- ST often resolves on its own but should be checked to avoid complications.
- DVT is a serious condition that can lead to death within hours if ignored.
The most important takeaway? Never self-diagnose. If you notice unusual swelling, redness, or pain in your legs, don’t wait. Get checked by a doctor, because early detection and treatment can literally save your life.
Your veins work tirelessly for you every day — it’s time to return the favor by protecting them with smart lifestyle choices, awareness, and timely care.
FAQs About DVT vs ST
1. Can superficial thrombophlebitis turn into DVT?
Yes, especially if the clot is near the junction of deep veins. That’s why doctors often recommend ultrasound screening even for ST.
2. How long does it take for DVT to form?
A clot can develop in just hours of immobility, such as during a long flight or hospital stay.
3. Is walking good for DVT or ST?
For most patients, gentle walking improves circulation and aids recovery, but only after medical clearance.
4. Do compression stockings really help?
Yes. They reduce swelling, improve blood flow, and lower the risk of both DVT recurrence and ST symptoms.
5. Who is most at risk of DVT?
People over 60, those with recent surgery, cancer, obesity, prolonged immobility, or a family history of clotting disorders.
Medically Reviewed by Prof. Dr. Akram
Orthopedic Surgeon | Professor | Senior Medical Specialist
Prof. Dr. Akram is a distinguished surgeon with over 15 years of clinical expertise. Having served as a lead Emergency Specialist at Complex International Government Hospital, he currently leads a specialized team of 13 medical professionals at his private hospital. As a Professor at top medical universities, he ensures that every article on WellHealthOrg.com meets rigorous clinical standards.
Medical Disclaimer:
The information provided is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician for any medical concerns.
Our content is rigorously fact-checked by our 13-member Editorial Team under the clinical supervision of Prof. Dr. Akram.