Medically Verified by Prof. Dr. Akram
Chief Medical Content Strategist & Senior Neurologist | 30+ Years Clinical Experience
The Neuro-Respiratory Matrix of Summer Breathing
I remember a scorching July afternoon in 1998. A 34-year-old patient named Sarah was rushed into my clinic, gasping for air. Her inhaler, left baking in the glovebox of her sedan, had failed her. As a neurologist, I don’t just look at the lungs; I look at the brain-lung axis. When extreme dry heat hits, the autonomic nervous system goes into overdrive. Your airways don’t just tighten; they panic. Navigating summer asthma and dust allergies requires far more than just carrying a rescue inhaler—it demands a strategic, environmental, and pharmacological master plan.

The paradox of summer is brutal. You escape the pollen of spring only to be trapped by the suffocating grip of dry heat, soaring ground-level ozone, and the invisible menace of indoor dust mites thriving in your air-conditioned sanctuaries. Addressing summer asthma & dust allergies effectively means hacking your environment and understanding the microscopic triggers that assault your respiratory epithelium.
Shareable Insight: “Managing summer asthma is a game of microscopic warfare; you must hydrate the airways while starving the allergens.”
Interactive Clinical Index
The Pathology of Dry Heat on Human Airways
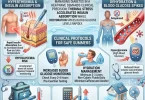
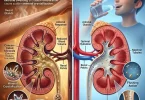
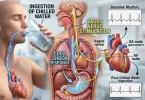
To defeat summer asthma & dust allergies, we must first understand the enemy. Inhaling hot, dry air forces the moisture within the mucosal lining of your bronchial tubes to evaporate rapidly. As a compensatory mechanism, your parasympathetic nervous system triggers a localized inflammatory cascade. Mast cells degranulate, releasing histamine, and the smooth muscles wrapping your airways contract violently. This is known as hyperosmolar-induced bronchoconstriction.
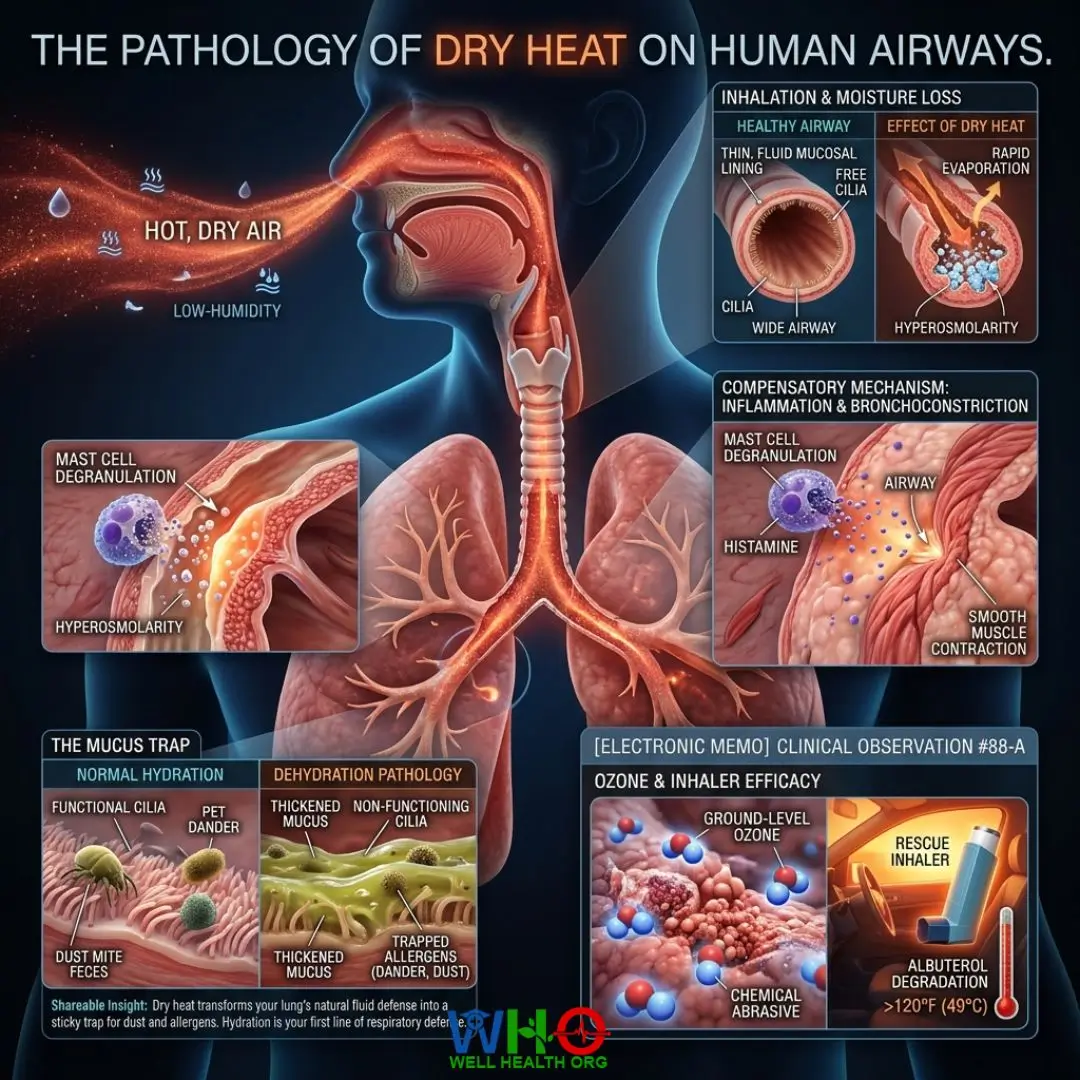
My “Eureka” moment in treating these seasonal exacerbations came when I began treating the lung’s environment rather than just the symptom. Hydration isn’t merely about drinking eight glasses of water; it is about maintaining the specific gravity of respiratory mucus. When mucus thickens due to dehydration, the cilia (the microscopic hairs lining the airways) cannot sweep away invading dust mite feces and pet dander. You become a walking trap for environmental debris.
Shareable Insight: “Dry heat transforms your lung’s natural fluid defense into a sticky trap for dust and allergens. Hydration is your first line of respiratory defense.”
[ELECTRONIC MEMO] CLINICAL OBSERVATION #88-A
Subject: Ozone and Inhaler Efficacy
Notes: High ambient temperatures combined with vehicular emissions create a spike in ground-level ozone, particularly between 11:00 AM and 4:00 PM. This ozone acts as a chemical abrasive on lung tissue. Furthermore, observed multiple patients experiencing rescue inhaler failure due to improper storage. Albuterol degradation occurs rapidly at temperatures above 120°F (easily reached in a parked vehicle). Always counsel patients on thermal medication protection.
The Allergen Matrix: The Hidden Life of Summer Dust Allergies
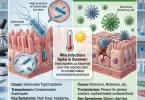
It is a common misconception that dust mites die off in the summer. While they require humidity to thrive, the micro-climates we create indoors to combat summer heat—specifically closed windows and recirculated air—provide a haven for Dermatophagoides pteronyssinus (the common dust mite). When battling summer asthma & dust allergies, understanding the biology of your mattress is mandatory.
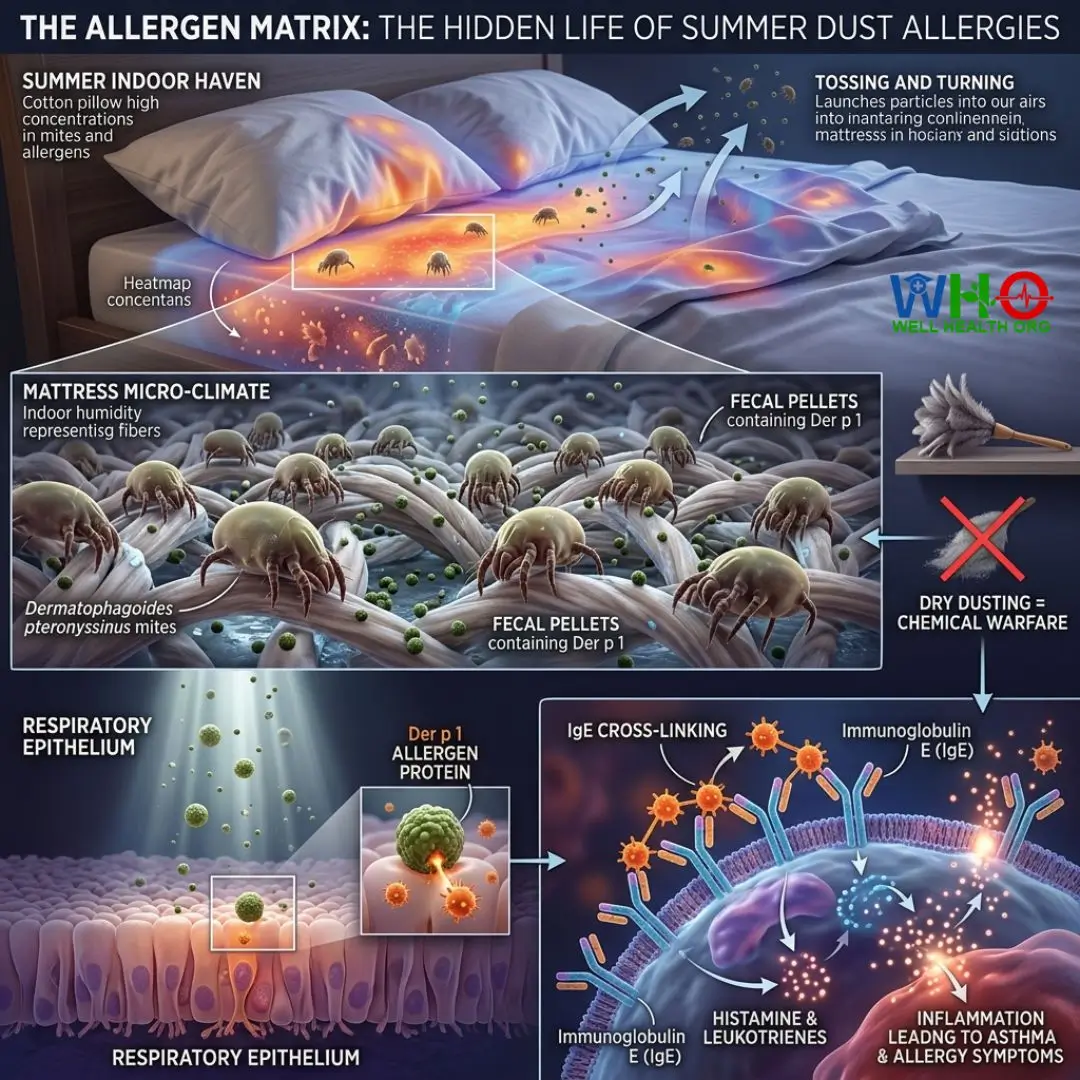
The allergic reaction is not to the mite itself, but to a specific protein (Der p 1) found in their fecal pellets. When you toss and turn in bed, these microscopic particles become airborne, settling directly onto your respiratory epithelium. Your immune system misidentifies this harmless protein as a lethal pathogen, initiating a cascade of Immunoglobulin E (IgE) cross-linking. The result? Wheezing, coughing, severe nasal congestion, and a tight chest.
Damp-dusting is non-negotiable. Dry dusting with a feather duster is essentially chemical warfare on your lungs, launching millions of microscopic allergen bombs directly into your breathing zone. We must transition from passive cleaning to active environmental medical containment.
Clinical Remedial Ecosystem
The following protocols form my proprietary strategy for combatting summer asthma & dust allergies. Treat these not merely as suggestions, but as precise medical directives to be executed with exactitude.
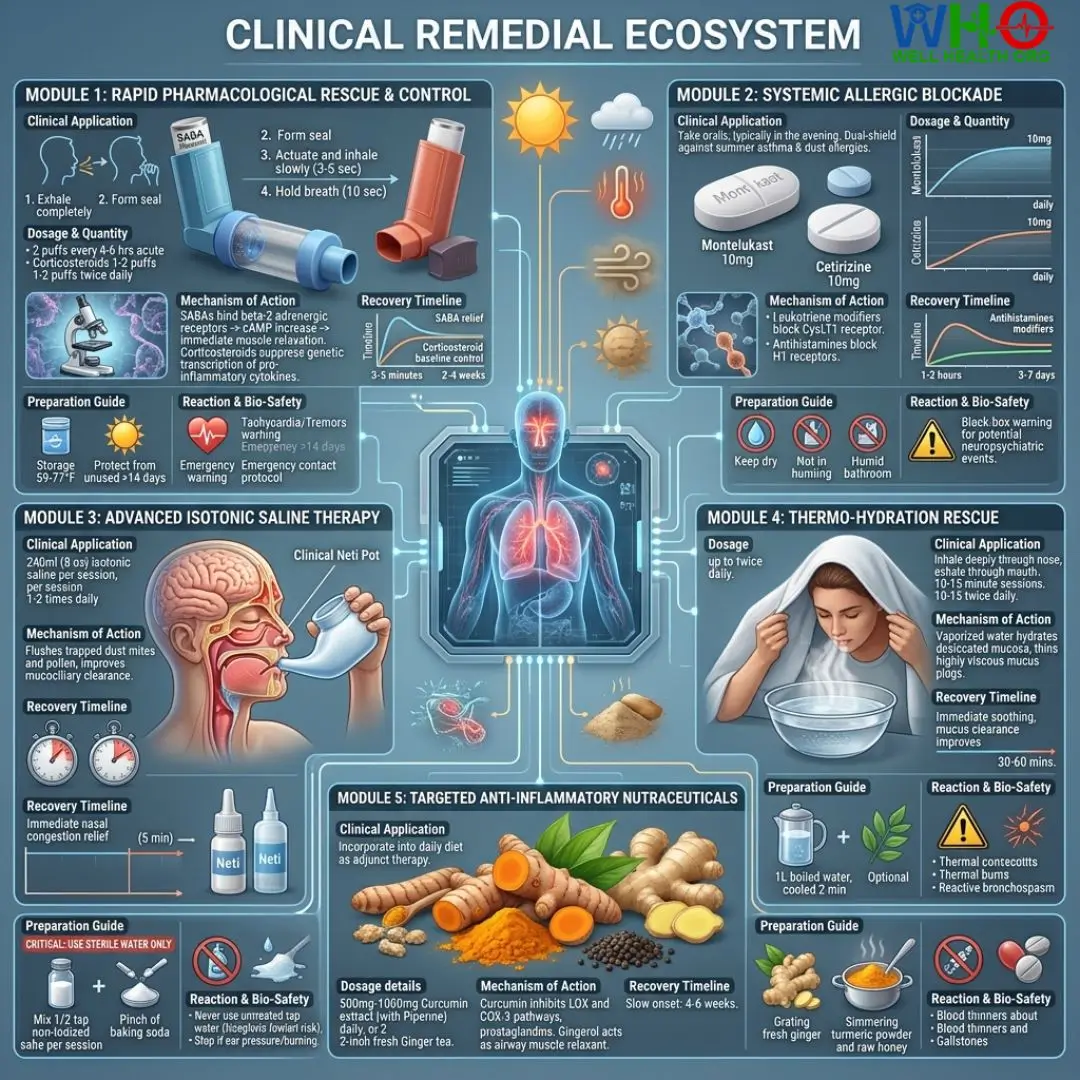
Module 1: Rapid Pharmacological Rescue & Control
Short-Acting Beta-Agonists (SABAs) & Inhaled Corticosteroids
- ⚡ How to Use (Clinical Application): Administer the SABA (e.g., Albuterol) at the first sign of chest tightness. Exhale completely, form a seal around the spacer, actuate the inhaler, and inhale slowly over 3-5 seconds. Hold breath for 10 seconds. Use inhaled corticosteroids daily as prescribed to maintain low baseline inflammation.
- ⚖️ Dosage & Quantity (Clinical Measurement): 2 puffs of SABA every 4-6 hours as needed for acute symptoms. Corticosteroids typically 1-2 puffs twice daily (follow specific physician dosing).
- 🔬 Mechanism of Action (Electronic Biological Mapping): SABAs bind to beta-2 adrenergic receptors on airway smooth muscle, activating adenylate cyclase, increasing cAMP, and forcing immediate muscle relaxation. Corticosteroids suppress genetic transcription of pro-inflammatory cytokines, reducing airway swelling over weeks.
- 📈 Recovery Timeline (Projected Outcome): SABA relief occurs within 3-5 minutes. Corticosteroid baseline control requires 2-4 weeks of uninterrupted adherence.
- 🛠️ Preparation Guide (Laboratory Method): Store devices between 59°F and 77°F (15°C–25°C). Keep away from direct summer sunlight. Prime inhalers if unused for more than 14 days by spraying 3-4 test bursts into the air.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): High doses of SABAs can cause tachycardia (rapid heart rate) and tremors. If symptoms do not resolve after use, or if peak expiratory flow drops below 50% of personal best, initiate emergency medical contact immediately.
Module 2: Systemic Allergic Blockade
Leukotriene Modifiers & 2nd-Gen Antihistamines
- ⚡ How to Use (Clinical Application): Take orally, typically in the evening. Montelukast is primarily used for both asthma and allergic rhinitis, creating a dual-shield against summer asthma & dust allergies. Combine with a non-drowsy antihistamine (e.g., Cetirizine) for comprehensive coverage.
- ⚖️ Dosage & Quantity (Clinical Measurement): Montelukast 10mg once daily for adults. Cetirizine 10mg once daily. Do not exceed these limits unless under direct specialist supervision.
- 🔬 Mechanism of Action (Electronic Biological Mapping): Leukotriene receptor antagonists block the CysLT1 receptor, preventing cysteinyl leukotrienes (released by mast cells) from causing bronchoconstriction and mucus hypersecretion. Antihistamines block H1 receptors from histamine binding.
- 📈 Recovery Timeline (Projected Outcome): Antihistamines reach peak efficacy in 1-2 hours. Leukotriene modifiers require 3-7 days to exhibit stable control over airway hyperresponsiveness.
- 🛠️ Preparation Guide (Laboratory Method): Swallow tablets whole with water. May be taken with or without food. Ensure they are kept in a dry environment, not in a humid bathroom cabinet.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): Montelukast has a black-box warning for potential neuropsychiatric events (agitation, vivid dreams, mood changes). Monitor closely. Discontinue and consult a physician if severe mood alterations occur.
Module 3: Advanced Isotonic Saline Therapy
Clinical Neti Pot Protocol for Upper Airway Clearance
- ⚡ How to Use (Clinical Application): Lean over a sink, tilt head 45 degrees. Pour solution into upper nostril, allowing it to flow out the lower nostril. Keep mouth open to breathe. This mechanically flushes trapped dust mites and pollen.
- ⚖️ Dosage & Quantity (Clinical Measurement): 240ml (8 oz) of isotonic saline per session. Perform 1-2 times daily during peak summer dust and heat waves.
- 🔬 Mechanism of Action (Electronic Biological Mapping): The saline washes away particulate matter and inflammatory mediators (prostaglandins, leukotrienes) from the nasal mucosa, while improving the beat frequency of mucociliary clearance.
- 📈 Recovery Timeline (Projected Outcome): Immediate relief of nasal congestion and sinus pressure within 5 minutes. Prevents downstream triggering of asthma over the long term.
- 🛠️ Preparation Guide (Laboratory Method): CRITICAL: Use only distilled, sterile, or previously boiled and cooled water. Mix with 1/2 teaspoon of non-iodized salt and a pinch of baking soda to buffer the pH to match the body.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): Never use untreated tap water due to the risk of Naegleria fowleri (brain-eating amoeba). If ear pressure or intense burning occurs, stop immediately and adjust the salt concentration.
Module 4: Thermo-Hydration Rescue
Clinical Steam Inhalation Therapy
- ⚡ How to Use (Clinical Application): Lean over a bowl of hot water with a towel draped over the head to form a tent. Inhale deeply through the nose and exhale through the mouth.
- ⚖️ Dosage & Quantity (Clinical Measurement): 10-15 minute sessions, up to twice daily when airways feel excessively dry from summer heat and AC usage.
- 🔬 Mechanism of Action (Electronic Biological Mapping): Vaporized water enters the upper and lower respiratory tracts, donating moisture to the desiccated mucosal lining. This thins highly viscous mucus plugs, allowing them to be expectorated easily.
- 📈 Recovery Timeline (Projected Outcome): Immediate soothing of raw, dry airways. Mucus clearance typically improves within 30-60 minutes post-therapy.
- 🛠️ Preparation Guide (Laboratory Method): Boil 1 liter of water. Let it cool for 2 minutes to prevent scalding the mucosal tissue. Optional: Add 1-2 drops of clinical-grade Eucalyptus essential oil (only if known not to trigger individual asthma phenotypes).
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): High risk of thermal burns. Keep eyes closed during inhalation. If steam causes reactive bronchospasm (tight chest), immediately discontinue; some asthmatics are triggered by extreme temperature shifts.
Module 5: Targeted Anti-Inflammatory Nutraceuticals
Biochemical Dietary Support (Curcumin & Gingerol)
- ⚡ How to Use (Clinical Application): Incorporate biologically active turmeric (curcumin) and fresh ginger into the daily diet as an adjunct therapy to reduce systemic inflammation driving summer asthma & dust allergies.
- ⚖️ Dosage & Quantity (Clinical Measurement): 500mg-1000mg of curcumin extract daily (with piperine for absorption), or a 2-inch thumb of fresh ginger brewed into tea daily.
- 🔬 Mechanism of Action (Electronic Biological Mapping): Curcumin inhibits the LOX and COX-2 enzymatic pathways, downregulating the synthesis of pro-inflammatory prostaglandins. Gingerol acts as a natural muscle relaxant on airway smooth muscle cells.
- 📈 Recovery Timeline (Projected Outcome): Slow onset. Requires 4-6 weeks of consistent daily intake to establish meaningful reductions in baseline systemic inflammation.
- 🛠️ Preparation Guide (Laboratory Method): For a potent extract: Simmer freshly grated ginger and 1 tsp of turmeric powder in hot water for 10 minutes. Add a crack of black pepper (increases curcumin bioavailability by 2000%) and a teaspoon of raw honey (soothes the throat).
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): High doses of turmeric can thin the blood. Consult your primary care physician before adding these if you are on anticoagulants (like Warfarin) or have a history of gallstones.
Neurological & Physiological Breathing Protocols
During an asthma flare-up triggered by dry summer heat or dust, patients naturally begin to panic. Hyperventilation ensues. As a neurologist, I continuously emphasize that anxiety and breathlessness form a destructive neuro-feedback loop. By breathing rapidly through the mouth, you bypass the nose’s vital filtration, humidification, and temperature-regulating systems. You deliver unconditioned, dust-laden hot air straight into your vulnerable lungs.
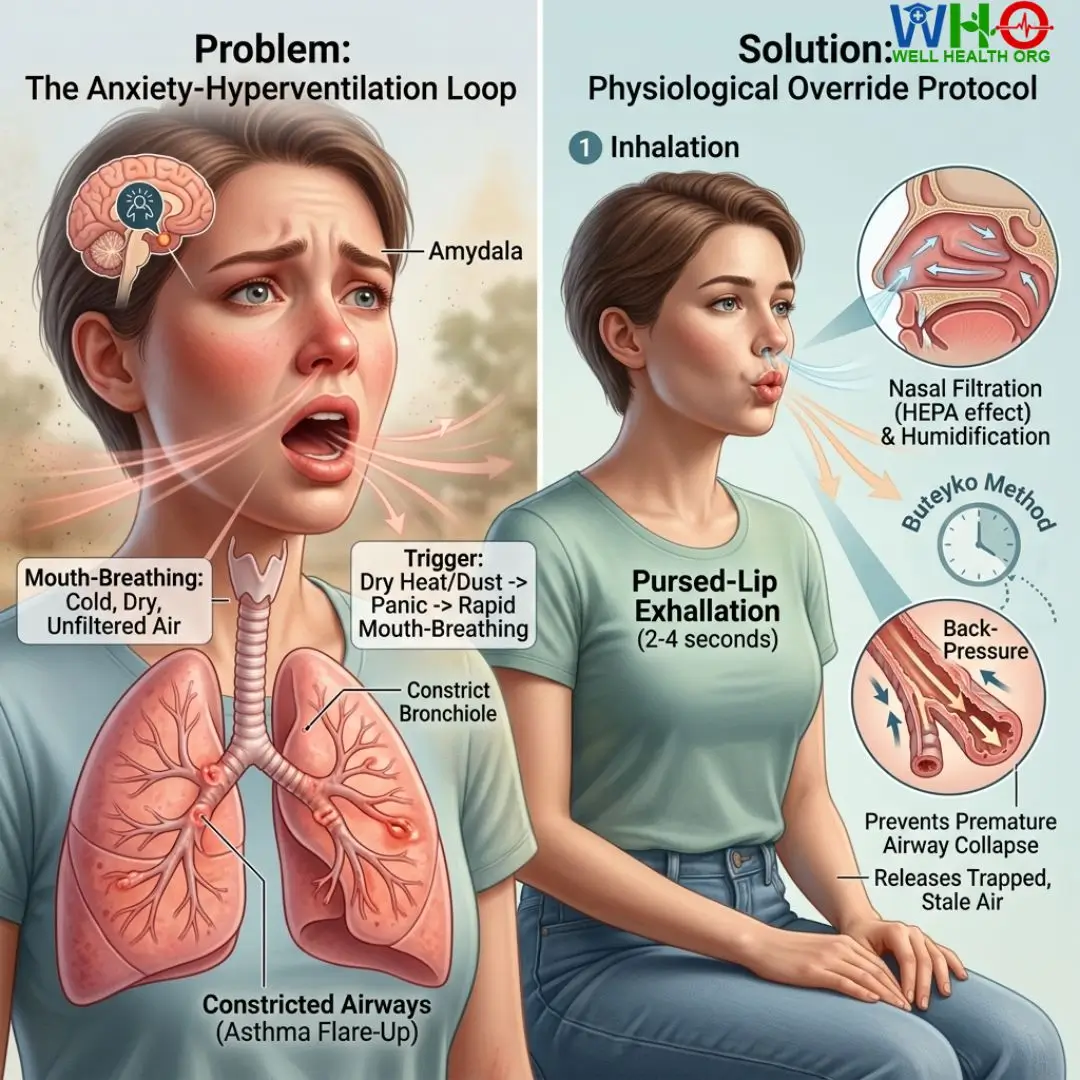
To break this loop, we utilize the Buteyko Breathing Method and Pursed-Lip Breathing. These are not merely relaxation techniques; they are physiological overrides for the nervous system.
Pursed-Lip Breathing Protocol: Inhale deeply through the nose for two seconds. Pucker your lips as if you are about to blow out a candle. Exhale slowly and forcefully through pursed lips for four to six seconds. This creates back-pressure in the airways, splinting them open and preventing premature airway collapse, allowing trapped, stale air to exit the lungs.
Shareable Insight: “When you panic and mouth-breathe during an asthma attack, you are bypassing your body’s natural HEPA filter—your nose. Slow down and close your mouth.”
Strategic Environmental Controls
Managing summer asthma & dust allergies is a 24/7 job of environmental engineering. The air inside your home can often be 2 to 5 times more polluted than the air outside. Let us break down the clinical parameters for maintaining a safe zone.

1. True HEPA Filtration Dynamics
You cannot fight microscopic dust mite feces with a standard vacuum. You require a True HEPA filter, capable of trapping 99.97% of particles that are 0.3 microns in size. When vacuuming, wear a well-fitted N95 mask, as the act of vacuuming aggressively agitates settled dust, throwing it into the breathing zone for up to two hours.
2. The Humidity Tightrope
This is where clinical precision is critical. If your air is too dry, your airways desiccate and spasm. If the humidity rises above 50%, dust mites breed exponentially. The optimal clinical target for an asthmatic in the summer is between 35% and 45% relative humidity. Purchase a digital hygrometer. Use a humidifier if the AC drops the air to 20%, but use a dehumidifier if swamp coolers push it past 50%.
3. Thermal Eradication of Bedding
Dust mites are resilient arthropods, but they have a fatal weakness: thermal shock. Washing sheets in warm or cold water only drowns a fraction of them. To eradicate dust mites, bedding must be washed weekly in water that is at least 130°F (54.4°C). Furthermore, utilizing zippered, allergen-proof encasements on mattresses and pillows creates an impenetrable barrier, starving the mites of their food source (your dead skin cells) and trapping the allergens inside.
Localized Clinical Summaries
🇮🇳 Hindi: Summer Asthma & Dust Allergies (15-Point Social Summary)
- 1. गर्मियों में सूखी हवा (Dry heat) सांस की नली को सिकोड़ देती है।
- 2. धूल के कण (Dust mites) गर्मियों में बंद घरों में तेजी से पनपते हैं।
- 3. शरीर और फेफड़ों को हाइड्रेटेड रखने के लिए दिन भर खूब पानी पिएं।
- 4. बाहर जाने से पहले हमेशा Air Quality Index (AQI) और ओजोन लेवल चेक करें।
- 5. दोपहर 11 बजे से शाम 4 बजे तक (Peak heat hours) घर के अंदर रहें।
- 6. खिड़कियां बंद रखें और हवा को साफ रखने के लिए AC का इस्तेमाल करें।
- 7. झाड़ू की जगह गीले कपड़े (Damp-dusting) से घर की सफाई करें।
- 8. वैक्यूम क्लीनर में True HEPA फ़िल्टर का ही उपयोग करें।
- 9. बिस्तर और चादरों को हर हफ्ते 130°F (गर्म पानी) में धोएं।
- 10. गद्दे और तकियों पर डस्ट-माइट प्रूफ कवर (Zippered covers) लगाएं।
- 11. अपने इनहेलर को कभी भी गर्म कार में न छोड़ें, यह खराब हो सकता है।
- 12. नाक की सफाई के लिए सलाइन वाटर (Neti pot) का इस्तेमाल करें।
- 13. पालतू जानवरों को बेडरूम से बाहर रखें क्योंकि उनके बालों में धूल चिपकती है।
- 14. बाहर आंधी या धूल हो तो अच्छी क्वालिटी का N95 मास्क पहनें।
- 15. पैनिक होने पर ‘Pursed-Lip Breathing’ करें, मुंह से सांस न लें।
🇮🇳 Hinglish: Summer Asthma Tips (15-Point Easy Summary)
- 1. Summer ki dry heat aapke airways ko dry aur tight kar deti hai.
- 2. Dust mites AC wale band kamro mein summer mein bhi survive karte hain.
- 3. Airways ko moist rakhne ke liye constantly pani peete rahein.
- 4. Outdoor activity se pehle phone par AQI aur pollen count zaroor check karein.
- 5. Peak pollution aur garmi ke time (11 AM to 4 PM) indoors hi rahein.
- 6. Windows closed rakhein aur indoor air ko clean rakhne ke liye air purifier use karein.
- 7. Dry dusting avoid karein; humesha damp (geele) cloth se surface saaf karein.
- 8. HEPA filter vacuum use karein taaki dust wapas hawa mein na ude.
- 9. Bedding aur pillow covers ko weekly garam pani (at least 130°F) mein wash karein.
- 10. Mattress aur pillows ke liye allergy-proof covers invest karein.
- 11. Rescue inhaler ko cool place par rakhein, hot car mein chhodne se wo asar nahi karega.
- 12. Dry nose ke liye Saline drops ya Neti pot ka use safe aur effective hai.
- 13. Pets ko bedroom ke andar allow na karein, unke dander se asthma trigger hota hai.
- 14. Ghar ki safai karte waqt ya windy days mein mask zaroor pehne.
- 15. Asthma attack ke time ghabrayein nahi, nose se saans lein aur Buteyko breathing try karein.
High-Engagement Clinical FAQs (25 Essential Directives)
1. What exactly triggers summer asthma & dust allergies?
Summer asthma is primarily triggered by a devastating combination of extreme heat desiccating the airways, elevated ground-level ozone causing chemical irritation, and indoor allergens like dust mites and mold thriving in recirculated, air-conditioned environments. The dry heat pulls moisture from your lungs, leading to rapid bronchospasm.
2. How does dry heat physiologically affect the lungs?
When you inhale extremely hot, dry air, the fluid lining your bronchial tubes evaporates. This hyperosmolar state triggers sensory nerves in the lung tissue. The brain interprets this as an attack, causing the airway smooth muscles to constrict to preserve moisture, leading directly to wheezing and shortness of breath.
3. Are dust mites really a problem during the summer?
Absolutely. While dust mites hate extreme dry heat outdoors, they thrive indoors. As people keep windows closed and run air conditioners or swamp coolers, the localized humidity in mattresses and carpets creates a perfect microclimate for them to feed, breed, and multiply, heavily exacerbating summer asthma & dust allergies.
4. What is the precise humidity level safe for asthmatics?
The clinical sweet spot is strictly between 35% and 45% relative humidity. If it drops below 30%, your airways become irritated and dry. If it rises above 50%, dust mites and mold spores reproduce rapidly. A digital hygrometer is essential for real-time monitoring of your indoor climate.
5. Are swamp coolers (evaporative coolers) safe for asthma?
They must be used with extreme caution. Swamp coolers add significant moisture to the air. While this helps dry airways, if left unchecked, it can easily push indoor humidity past 60%, turning your home into a breeding ground for mold and dust mites, ultimately worsening respiratory symptoms.
6. How does ground-level ozone interact with asthma?
Ground-level ozone, created when sunlight bakes vehicular and industrial emissions, is highly oxidative. When inhaled, it literally “sunburns” the respiratory epithelium. This aggressive cellular damage lowers your threshold for an asthma attack, meaning even tiny amounts of dust will trigger a severe asthmatic response.
7. When is the safest time to exercise outdoors during summer?
The safest window is early morning, strictly before 9:00 AM. During this time, temperatures are at their lowest, and morning breezes have dispersed overnight pollutants, meaning the Air Quality Index and ozone levels have not yet spiked from the midday solar radiation.
8. What happens if I leave my inhaler in a hot car?
This is a massive clinical error. Inside a parked car in summer, temperatures can exceed 140°F (60°C). Heat degrades the active medication (like Albuterol) and can warp the plastic housing or cause the pressurized canister to burst. Your rescue inhaler will fail you when you need it most.
9. Does washing bedding in cold water kill dust mites?
No. Cold or warm water simply gives dust mites a bath. To achieve thermal eradication and destroy the allergic proteins, you must wash all bedding in hot water that is at least 130°F (54.4°C). This is a critical step in managing summer asthma & dust allergies.
10. Do HEPA filters really make a difference for dust allergies?
Yes, provided they are ‘True HEPA’ (High-Efficiency Particulate Air). They capture 99.97% of particles down to 0.3 microns. Regular vacuums without HEPA filtration simply suck up dust and blast the invisible, microscopic allergens back into the air, drastically worsening your symptoms.
11. What is damp-dusting and why is it important?
Damp-dusting involves wiping hard surfaces with a damp microfiber cloth instead of a dry feather duster. Dry dusting launches allergen particles into the air where you inhale them. Damp-dusting traps the particulate matter onto the cloth, permanently removing it from your breathing zone.
12. Is using a Neti pot safe in the summer?
Yes, but strictly with distilled or previously boiled and cooled water. A Neti pot mechanically flushes out trapped pollen and dust mite debris from the nasal passages. Never use tap water, as the warming summer pipes increase the risk of dangerous amoebic infections.
13. Can pets make summer asthma worse even if they stay inside?
Yes. Dogs and cats shed dander (dead skin cells), which is a massive trigger. Furthermore, if they go outside, their fur acts like a sponge, bringing outdoor pollen and dust back inside. Keep pets entirely out of the asthmatic patient’s bedroom to maintain a sterile sleep zone.
14. Should an asthmatic wear a mask outdoors in summer?
On days when the AQI is in the red zone, or if it is highly windy and dusty, wearing a well-fitted N95 mask can act as a physical barrier. It pre-warms the air slightly and filters out massive amounts of particulate matter before it reaches your lower airways.
15. What is the fundamental difference between an allergy and asthma?
An allergy is an immune system overreaction in the upper respiratory tract (nose, eyes) to a harmless substance. Asthma is a chronic inflammatory disease of the lower respiratory tract (bronchial tubes). However, an allergic reaction can easily travel down the airway and trigger an asthma attack.
16. How do leukotriene modifiers (like Montelukast) work?
When exposed to an allergen, your immune cells release inflammatory chemicals called leukotrienes, which cause airway swelling and excessive mucus production. Montelukast blocks the receptors that these chemicals try to bind to, halting the inflammatory cascade at a cellular level.
17. Are OTC antihistamines safe to take daily all summer?
Second-generation antihistamines (like Cetirizine, Loratadine, Fexofenadine) are generally safe for daily use and do not cross the blood-brain barrier as aggressively, avoiding severe drowsiness. However, always consult your physician to ensure they don’t interact with other medications you are taking.
18. What is Immunotherapy for dust mites?
Immunotherapy (allergy shots or sublingual tablets) involves exposing your body to microscopic, gradually increasing amounts of the dust mite allergen over 3-5 years. This essentially rewires your immune system to build a natural tolerance, drastically reducing future severity of summer asthma & dust allergies.
19. Can Vitamin C really help with summer allergies?
Yes, Vitamin C is a powerful antioxidant that acts as a mild, natural antihistamine. Consuming foods high in Vitamin C (citrus, bell peppers, strawberries) helps stabilize mast cells, making them less likely to burst and release the histamine that causes severe allergic rhinitis and asthma exacerbations.
20. How exactly does Turmeric reduce asthma symptoms?
Turmeric contains curcumin, a potent bioactive compound that blocks specific inflammatory enzymes (LOX and COX-2) in the body. By reducing baseline systemic inflammation, your airways are less “twitchy” and less likely to spasm when exposed to summer heat and microscopic dust mites.
21. What is the Buteyko breathing method?
It is a clinical breathing protocol designed to reverse hyperventilation. It focuses on taking slow, shallow breaths exclusively through the nose and incorporating “control pauses” (holding the breath after exhaling). This restores carbon dioxide levels, which naturally dilates and relaxes smooth muscle in the airways.
22. How quickly does an Albuterol rescue inhaler work?
When administered correctly (preferably with a spacer), Albuterol binds to beta-2 receptors in the lungs within seconds. Noticeable relief from bronchospasm and chest tightness should occur within 3 to 5 minutes. If symptoms persist after two doses, emergency medical protocols must be initiated.
23. What are the signs of a true asthma emergency?
Critical warning signs include a rescue inhaler failing to provide relief after 15-20 minutes, extreme difficulty speaking more than brief phrases, cyanosis (bluish tint to lips or fingernails), and severe retractions (the skin sucking in around the ribs and neck when breathing). Seek ER intervention immediately.
24. Does air conditioning make asthma better or worse?
It is a double-edged sword. AC filters out outdoor pollen and lowers humidity, which is excellent. However, if the AC filters are dirty, or if it blasts freezing air directly onto your face, the abrupt temperature drop and recirculated dust can violently trigger an asthma attack.
25. Can stress from the summer heat worsen my asthma?
Absolutely. The brain-lung axis is very real. Physiological stress from extreme heat increases cortisol and adrenaline levels, which alters your respiratory rate. Anxiety about breathing makes you hyperventilate, creating a devastating cycle that exacerbates asthma symptoms drastically. Mental calmness is a medical necessity.
© 2026 Dr. Akram Medical Strategy Group. All Rights Reserved.
Medically Reviewed by Prof. Dr. Akram
Orthopedic Surgeon | Professor | Senior Medical Specialist
Prof. Dr. Akram is a distinguished surgeon with over 15 years of clinical expertise. Having served as a lead Emergency Specialist at Complex International Government Hospital, he currently leads a specialized team of 13 medical professionals at his private hospital. As a Professor at top medical universities, he ensures that every article on WellHealthOrg.com meets rigorous clinical standards.
Medical Disclaimer:
The information provided is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician for any medical concerns.
Our content is rigorously fact-checked by our 13-member Editorial Team under the clinical supervision of Prof. Dr. Akram.