Chief Medical Content Strategist & Senior Neurologist | 30+ Years Clinical Experience
Status: Online
The Neurology of Summer Syncope: Reclaiming Your Mornings
In my three decades walking the neurology wards, the arrival of July has consistently signaled a specific wave of admissions: the “gravity casualties.” I have seen countless patients—from marathon runners to retired schoolteachers—brought into the ER completely bewildered because they stood up from their beds and collapsed. The culprit is rarely a catastrophic cardiac event; rather, it is a predictable failure of the autonomic nervous system to fight the dual forces of gravity and heat. Establishing the best morning routine to prevent low blood pressure in summer is not just a matter of wellness; it is a neurological imperative.

During the warmer months, our bodies deploy a survival mechanism known as vasodilation. Blood vessels expand to release core heat through the skin. While this keeps you from overheating, it drastically increases the total “container space” of your circulatory system. When you suddenly transition from lying flat for eight hours to standing upright, gravity aggressively pulls that blood into your legs. A healthy autonomic nervous system instantly tightens those vessels and ramps up your heart rate. But with summer heat blunting that response, you experience orthostatic hypotension—a rapid drop in blood pressure that robs your brain of oxygen, leading to lightheadedness, blurred vision, and syncope (fainting).
📋 Clinical Observation Memo: Case #402-B
“Eureka moments in medicine rarely happen in a laboratory; they happen at the bedside. I recall treating a 45-year-old architect who experienced debilitating morning dizziness exclusively between June and August. Extensive cardiac workups were entirely clear. The breakthrough occurred when we mapped her exact morning movements. She was jumping out of a warm bed, walking straight to a hot shower, and skipping breakfast. Her routine was a perfect storm for peripheral vasodilation. By simply introducing an isotonic drink on her nightstand, instituting a two-minute staged rise, and swapping the hot shower for tepid water, her symptoms vanished completely in 48 hours. The architecture of waking up matters.” – Dr. Akram
Interactive Diagnostic Index
Understanding the Enemy: Heat-Induced Vasodilation
To master the best morning routine to prevent low blood pressure during summer, we must first analyze the precise mechanics of waking up in a warm environment. When you sleep, your blood pressure naturally dips—a phenomenon known as “nocturnal dipping.” Concurrently, you lose fluid through respiration and mild perspiration, leading to subtle dehydration by dawn.
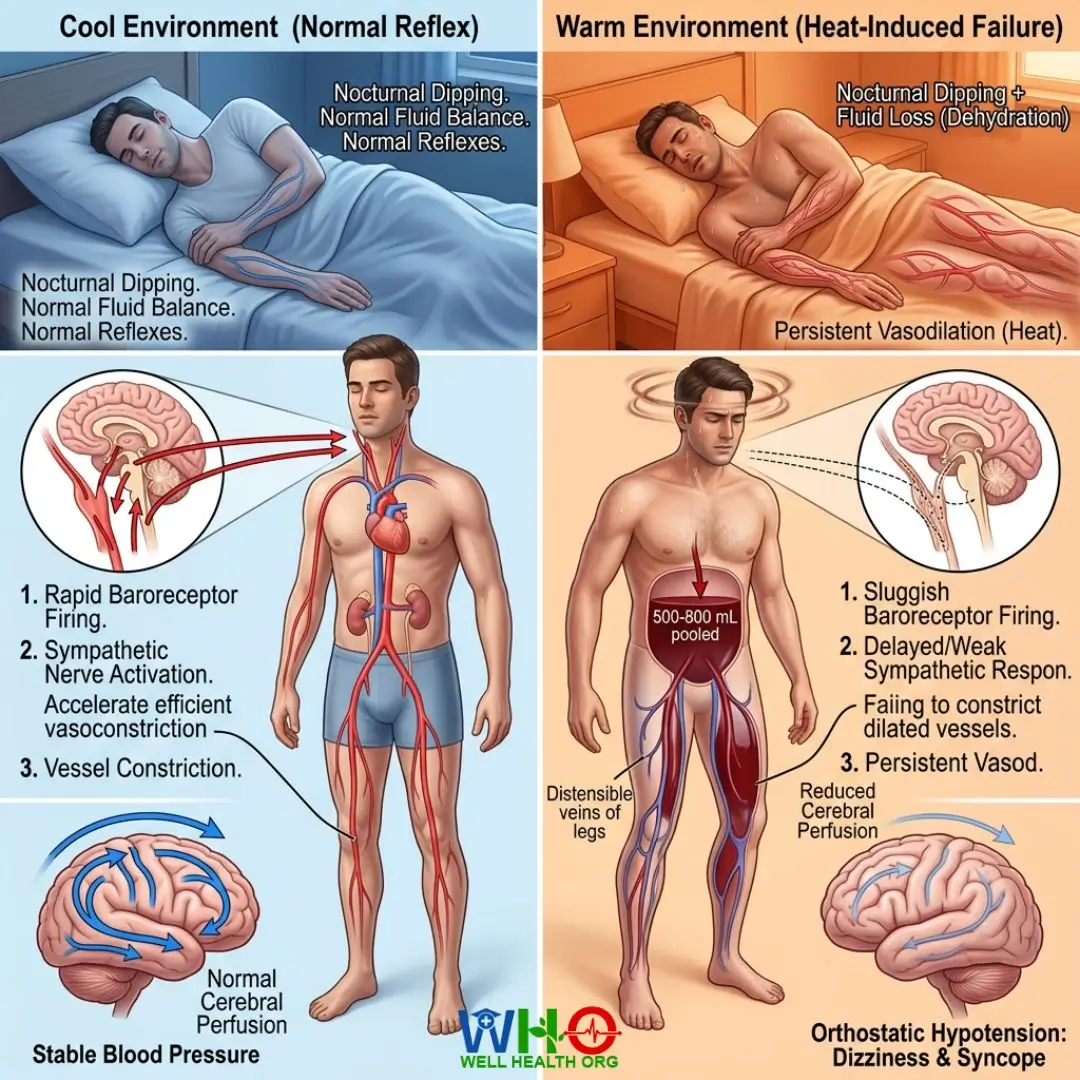
If you sleep in a room that is too warm, your body keeps the peripheral blood vessels wide open. When your alarm rings and you stand up suddenly, gravity pulls approximately 500 to 800 milliliters of blood downward into the distensible veins of the legs and splanchnic (abdominal) bed. In a cooler climate or a well-hydrated state, the baroreceptors in your carotid arteries immediately detect this drop and fire signals via the sympathetic nervous system to clamp down the blood vessels and accelerate the heart. In the summer heat, this reflex is tragically sluggish. The blood remains pooled, cerebral perfusion drops, and the room begins to spin.
This is why intentional, staged mornings are non-negotiable for those prone to hypotension.
Clinical Remedial Ecosystem
Below, I have codified the precise interventions necessary to build the best morning routine to prevent low blood pressure during summer. These are not mere lifestyle suggestions; they are targeted physiological modulators designed to intercept vascular collapse before it begins.
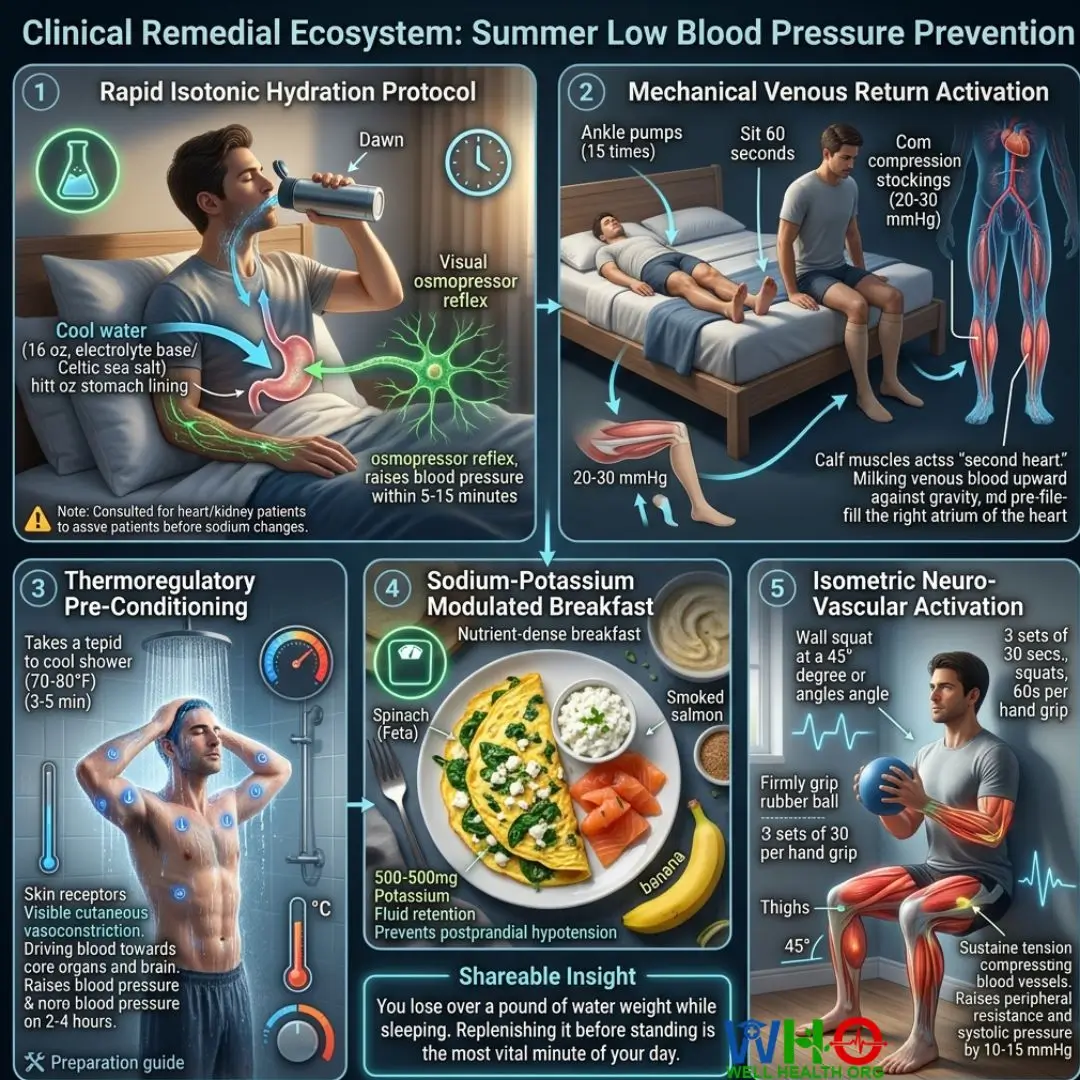
Remedy Module 1: Rapid Isotonic Hydration Protocol
⚡ How to Use (Clinical Application): Place an insulated flask on your nightstand. Upon waking, before your feet touch the floor, consume the entire volume over 2 to 3 minutes while sitting propped up on your pillows.
⚖️ Dosage & Quantity (Clinical Measurement): 16 ounces (approx. 500 ml) of cool water mixed with an electrolyte base (or a pinch of Celtic sea salt).
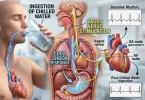
🔬 Mechanism of Action (Electronic Biological Mapping): Initiates the “osmopressor reflex.” Water hitting the stomach lining triggers sympathetic nerve activity that raises blood pressure independently of fluid volume expansion. The added sodium helps retain this fluid within the intravascular space.
📈 Recovery Timeline (Projected Outcome): Hemodynamic stabilization within 5 to 15 minutes of ingestion.
🛠️ Preparation Guide (Laboratory Method): Before bed, fill a flask with 16 oz of chilled water. Add 1/8 teaspoon of quality salt and an optional squeeze of lemon for flavor.
⚠️ Reaction & Bio-Safety (Emergency Protocol): Nausea can occur if consumed too fast on a sensitive stomach. If nausea presents, reduce volume to 8 oz and sip slowly. Patients with heart failure or severe kidney disease must consult their physician before modifying sodium intake.
Remedy Module 2: Mechanical Venous Return Activation
⚡ How to Use (Clinical Application): Perform the “Staged Rise.” Lying flat, flex your calves and pump your ankles 15 times. Roll to your side, push up to a seated position on the edge of the bed. Wait 60 seconds. Apply compression garments if prescribed, then stand slowly.
⚖️ Dosage & Quantity (Clinical Measurement): 15 ankle pumps per leg; 60 seconds of seated pausing; 20-30 mmHg medical-grade compression stockings.
🔬 Mechanism of Action (Electronic Biological Mapping): The calf muscle acts as a “second heart.” Contracting these muscles actively milks pooled venous blood upward against gravity, pre-filling the right atrium of the heart and ensuring adequate stroke volume when you finally stand.
📈 Recovery Timeline (Projected Outcome): Immediate mitigation of postural dizziness upon standing.
🛠️ Preparation Guide (Laboratory Method): Keep compression stockings within arm’s reach of the bed so they can be donned before gravity allows blood to pool in the lower extremities.
⚠️ Reaction & Bio-Safety (Emergency Protocol): If lightheadedness occurs while seated, immediately lie back down and elevate legs above the heart using pillows (Trendelenburg position) to force cerebral perfusion.
Remedy Module 3: Thermoregulatory Pre-Conditioning
⚡ How to Use (Clinical Application): Replace the traditional morning hot shower with a tepid to cool shower.
⚖️ Dosage & Quantity (Clinical Measurement): Water temperature should be around 70-80°F (21-26°C), lasting 3 to 5 minutes.
🔬 Mechanism of Action (Electronic Biological Mapping): Cool water stimulates cutaneous cold receptors, causing sudden peripheral vasoconstriction. This physically shrinks the blood vessels in the skin, driving blood back toward the core organs and brain, acutely raising blood pressure.
📈 Recovery Timeline (Projected Outcome): Sustained alertness and stable blood pressure for 2-4 hours post-shower.
🛠️ Preparation Guide (Laboratory Method): Start with lukewarm water to avoid a severe shock, gradually turning the dial to cool over 30 seconds.
⚠️ Reaction & Bio-Safety (Emergency Protocol): Avoid ice-cold water if you have a history of cardiac arrhythmias, as the sudden cold shock can trigger vagal nerve overstimulation. Warm the water slightly if shivering occurs.
Remedy Module 4: Sodium-Potassium Modulated Breakfast
⚡ How to Use (Clinical Application): Consume a nutrient-dense, slightly saltier breakfast within 60 minutes of waking, paired with high-quality proteins and complex carbohydrates.
⚖️ Dosage & Quantity (Clinical Measurement): Target 500-1000mg of sodium for the morning meal (for diagnosed hypotensive patients), balanced with 300-500mg of potassium (e.g., half a banana or spinach).
🔬 Mechanism of Action (Electronic Biological Mapping): Sodium retains fluid volume. Complex carbs and protein prevent “postprandial hypotension” (where blood rushes to the digestive tract after a heavy, simple-carb meal, causing subsequent dizziness).
📈 Recovery Timeline (Projected Outcome): Prevents the mid-morning crash commonly seen at 10:00 AM.
🛠️ Preparation Guide (Laboratory Method): Prepare an omelet with spinach and feta cheese, or cottage cheese topped with smoked salmon. Ensure portions are small to moderate to avoid massive splanchnic blood pooling.
⚠️ Reaction & Bio-Safety (Emergency Protocol): If profound lethargy occurs after eating, lay down for 15 minutes. Ensure you are not over-consuming carbohydrates, which require massive blood flow to digest.
Remedy Module 5: Isometric Neuro-Vascular Activation
⚡ How to Use (Clinical Application): Engage in static muscle contractions before starting your commute or active day.
⚖️ Dosage & Quantity (Clinical Measurement): 3 sets of 30-second wall squats, or firmly gripping a rubber ball for 60 seconds per hand.
🔬 Mechanism of Action (Electronic Biological Mapping): Sustained muscle tension without joint movement (isometrics) temporarily compresses blood vessels in the active muscles, raising peripheral resistance and forcing blood pressure to climb steadily.
📈 Recovery Timeline (Projected Outcome): Elevates systolic pressure by 10-15 mmHg during and immediately following the exercise.
🛠️ Preparation Guide (Laboratory Method): Find a sturdy wall. Slide down until knees are bent at a 45-degree angle. Hold while breathing evenly.
⚠️ Reaction & Bio-Safety (Emergency Protocol): Never hold your breath during isometrics (the Valsalva maneuver), as this can paradoxically crash your blood pressure when you release. Breathe rhythmically. Stop if chest pain occurs.
The Danger Zone: Summer Morning “Don’ts”
Building the best morning routine to prevent low blood pressure during summer is as much about omission as it is about action. The morning environment is full of hidden triggers that sabotage vascular tone.

1. The Hot Shower Trap: We touched on this in our remedial module, but it bears repeating. Standing in a steaming shower creates massive cutaneous vasodilation. Blood rushes to the surface of the skin. Combining heat, standing still, and raising your arms above your head to wash your hair removes a massive percentage of blood from cerebral circulation. Fainting in the shower is a primary cause of head trauma during summer months.
2. Skipping the Morning Meal: Fasting might be a current dietary trend, but for the hypotensive patient, it is disastrous. Skipping breakfast denies your system the glucose and fluid retention needed to stabilize energy and vascular pressure. A fasted, dehydrated morning guarantees mid-day fatigue.
3. The Caffeine Paradox: Many reach for three cups of strong black coffee to combat the morning brain fog of hypotension. While caffeine acts as a mild vasoconstrictor (temporarily raising BP), it is also a powerful diuretic. In the heat of summer, massive caffeine intake accelerates fluid loss through urine. The initial spike in blood pressure is inevitably followed by a severe dehydration-induced crash by early afternoon.
The Duality of Blood Pressure: Regulating the Autonomic Pendulum
It is clinically fascinating to observe how morning routines impact the opposite end of the spectrum: hypertension (high blood pressure). When examining the literature, we see that practices designed to lower high blood pressure often intersect beautifully with practices that stabilize low blood pressure. The ultimate goal is autonomic homeostasis—balancing the sympathetic (fight-or-flight) and parasympathetic (rest-and-digest) systems.
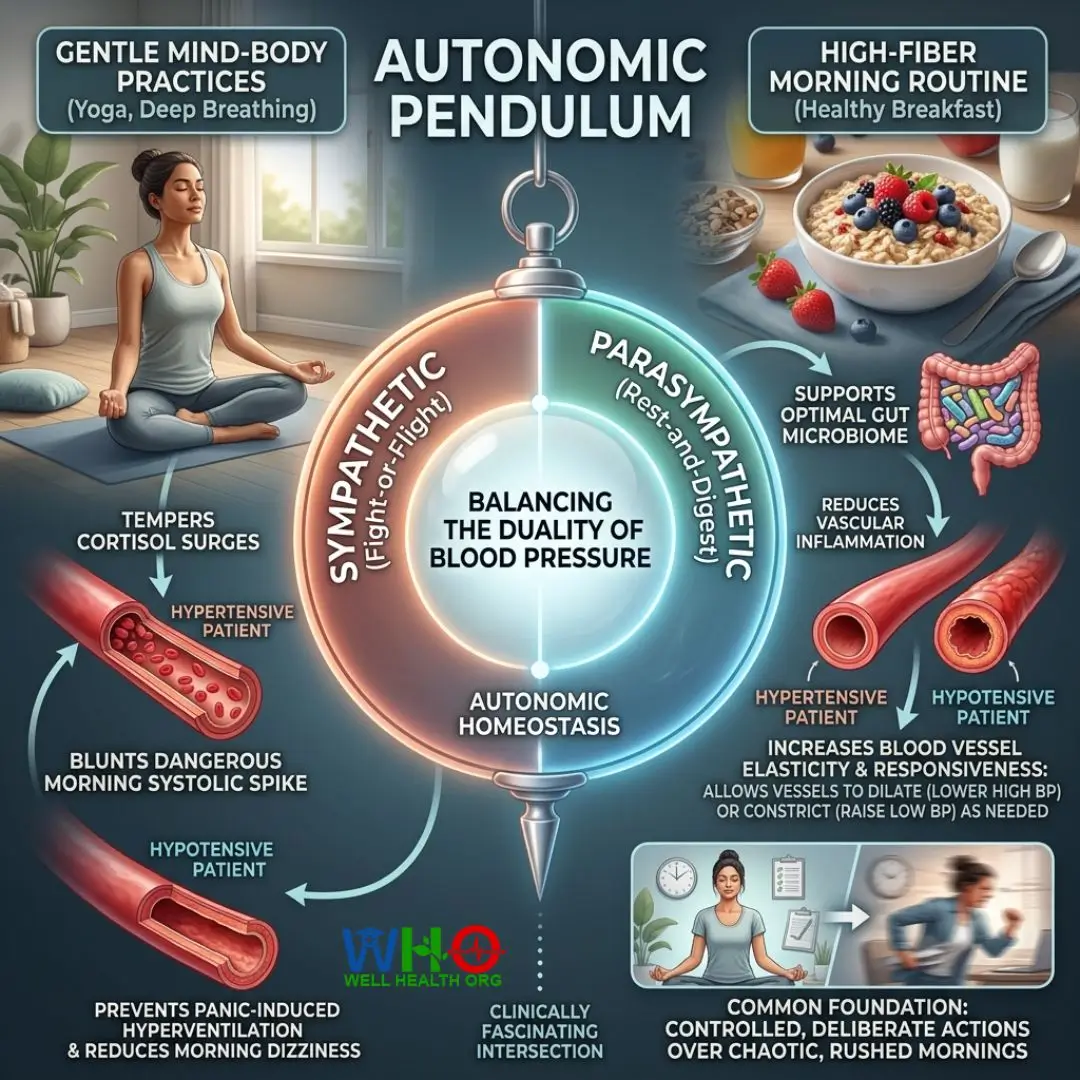
For instance, incorporating mind-body practices like gentle yoga or deep diaphragmatic breathing helps temper the extreme surges of cortisol upon waking. For a hypertensive patient, this blunts the dangerous morning spike in systolic pressure. For a hypotensive patient, mindful breathing prevents the panic-induced hyperventilation that often accompanies morning dizziness.
Similarly, adding high-fiber foods to your morning routine supports an optimal gut microbiome. Fiber reduces vascular inflammation, making blood vessels more elastic and responsive. Whether those vessels need to dilate to lower pressure or constrict to raise it, a healthy, inflammation-free endothelial lining is critical for both populations. The best morning routine to prevent low blood pressure during summer shares a common foundation with general cardiovascular longevity: controlled, deliberate actions over chaotic, rushed mornings.
Localized Protocols for Rapid Reading
🇮🇳 Hindi Social Summary: गर्मियों में लो ब्लड प्रेशर से बचने के 15 टिप्स
- 1. सुबह उठते ही बिस्तर से तुरंत न कूदें।
- 2. रात को सिरहाने पानी का फ्लास्क रखें।
- 3. बिस्तर छोड़ने से पहले 1-2 गिलास पानी पिएं।
- 4. लेटे हुए ही पैरों और पंजों को 15 बार हिलाएं।
- 5. करवट लें और 1 मिनट तक बिस्तर के किनारे बैठें।
- 6. जरूरत हो तो लेटे-लेटे ही कम्प्रेशन मोज़े (Compression stockings) पहनें।
- 7. गर्म पानी से नहाने से बचें, यह ब्लड प्रेशर और कम करता है।
- 8. सुबह ठंडे या हल्के गुनगुने पानी से नहाएं।
- 9. नाश्ता कभी न छोड़ें, यह ऊर्जा और प्रेशर को स्थिर रखता है।
- 10. नाश्ते में थोड़ा नमक और प्रोटीन जरूर शामिल करें (जैसे पनीर या अंडे)।
- 11. ज्यादा कैफीन या चाय-कॉफी न पिएं, यह डिहाइड्रेशन बढ़ाता है।
- 12. अगर व्यायाम करना हो, तो सुबह जल्दी ठंडे मौसम में करें।
- 13. भारी एक्सरसाइज के बजाय हल्की स्ट्रेचिंग या योग करें।
- 14. चक्कर आने पर तुरंत बैठ जाएं या लेटकर पैर ऊंचे कर लें।
- 15. सुबह की दिनचर्या को शांत और बिना जल्दबाजी का बनाएं।
📱 Hinglish Social Summary: Summer Low BP Prevent Karne Ke 15 Tips
- 1. Bed se achanak khade mat ho, aaram se utho.
- 2. Nightstand par hamesha ek glass pani rakhein.
- 3. Uthte hi sabse pehle 500ml pani piyein.
- 4. Lete huye calves stretch karein aur ankles pump karein.
- 5. Bed ke edge par 1-2 minute sit karein blood flow balance karne ke liye.
- 6. Agar prescribed hai toh bed mein hi compression stockings pehan lein.
- 7. Hot showers completely avoid karein, blood vessels dilate hoti hain.
- 8. Body temperature maintain karne ke liye cool shower lein.
- 9. Breakfast skip bilkul na karein.
- 10. Breakfast mein thoda salty aur nutrient-dense food khayein.
- 11. Excess tea/coffee avoid karein kyunki yeh diuretics hote hain.
- 12. Morning workout karna hai toh early morning lower temperatures mein karein.
- 13. Intense gym sessions ki jagah gentle walking ya yoga karein.
- 14. Agar dizziness feel ho, toh turant “get low” — baith jayein ya legs elevate karein.
- 15. Apne morning routine mein stress aur jaldbazi kam karein.
Extensive Medical FAQ Database: Navigating Summer Hypotension
1. What exactly constitutes the best morning routine to prevent low blood pressure during summer?
The best morning routine to prevent low blood pressure during summer integrates rapid fluid volume expansion (drinking 16oz of electrolyte water upon waking), mechanical vascular pumping (ankle flexing), staged rising, and thermoregulation (cool showers). It prevents the massive pooling of blood in the lower extremities caused by summer heat.
2. Why does summer heat make my blood pressure drop specifically in the morning?
Heat forces your peripheral blood vessels to dilate (open wide) to cool the body. While asleep, you become mildly dehydrated. When you stand up in the morning with widened vessels and lower fluid volume, gravity pulls the blood into your legs, causing a rapid drop in cerebral blood pressure.
3. Can drinking coffee first thing help raise my low blood pressure?
While caffeine provides a temporary vasoconstrictive spike in blood pressure, it acts as a diuretic, causing you to lose fluids through urination. In summer heat, this accelerates dehydration and often leads to a more severe blood pressure crash by mid-day. Hydrate with water first.
4. Is it safe to eat saltier foods in the morning if I suffer from hypotension?
Yes, for patients clinically diagnosed with chronic hypotension or conditions like POTS (Postural Orthostatic Tachycardia Syndrome), moderately increasing morning sodium intake helps the body retain intravascular fluid, directly boosting blood volume. Always consult your physician first, especially if you have kidney issues.
5. What is “staged rising” and how do I do it?
Staged rising involves transitioning from lying down to standing over a span of minutes rather than seconds. Wake up, pump your ankles to push blood to the heart, sit on the edge of the bed for 60-120 seconds, and then stand slowly. This gives your autonomic nervous system time to react to gravity.
6. Why should I avoid hot showers in the morning during summer?
Hot water causes immediate and widespread vasodilation. When combined with standing up, it aggressively shifts blood away from your brain and core toward the skin’s surface. This is a primary trigger for morning syncope (fainting) in hypotensive individuals.
7. Do compression stockings really work for low blood pressure?
Absolutely. Medical-grade compression stockings (20-30 mmHg) worn thigh-high or waist-high mechanically prevent blood from pooling in the distensible veins of the legs. They should be put on while you are still lying in bed, before gravity affects your blood pooling.
8. How does potassium fit into a low blood pressure diet?
While hypotensive individuals need sodium to retain fluid, potassium is essential for proper cellular signaling, muscle contraction (including the heart), and preventing the negative side effects of excessive sodium. A balanced ratio is required for optimal autonomic nervous system function.
9. What is “postprandial hypotension”?
Postprandial hypotension is a drop in blood pressure occurring 30 to 75 minutes after eating a meal. Digesting a heavy, carbohydrate-rich breakfast requires massive blood flow to the stomach and intestines, pulling blood away from the brain. Small, protein-rich meals are safer.
10. If I feel dizzy, what is the emergency protocol?
Immediately “get low.” Sit on the floor or lie down flat. If possible, elevate your legs above the level of your heart (Trendelenburg position) using a chair or pillows. This uses gravity to instantly return pooled blood from your legs directly to your brain.
11. Can morning workouts cause my blood pressure to crash?
Yes, if they are overly intense or done in high heat. Vigorous exercise diverts blood to skeletal muscles and dilates skin vessels for sweating. After stopping, blood pressure can drop dangerously low. Gentle movement, like walking or yoga in a cool room, is much safer.
12. Does drinking water before bed help morning blood pressure?
It can help maintain overnight hydration, but drinking too much will disrupt sleep by forcing you to wake up to urinate. The best approach is moderate evening hydration combined with immediate, aggressive hydration the moment you wake up.
13. Are there specific medications that worsen morning hypotension in summer?
Yes. Alpha-blockers, beta-blockers, diuretics, and certain antidepressants can blunt the autonomic response. When combined with summer heat, their effects are magnified. Never stop medication abruptly, but consult your doctor regarding summer dose adjustments.
14. What role does fiber play in blood pressure regulation?
Fiber supports a healthy gut microbiome, which reduces systemic inflammation and improves the elasticity of the vascular endothelium. Healthy blood vessels are better able to constrict rapidly upon standing, improving overall autonomic responsiveness.
15. Can anxiety about fainting make blood pressure worse?
Anxiety usually spikes heart rate and blood pressure initially due to adrenaline. However, it can trigger a vagal response—a sudden reflex that crashes both heart rate and blood pressure—leading to vasovagal syncope. Stress management is a vital part of the morning routine.
16. Are sports drinks good for morning hydration?
Commercial sports drinks contain electrolytes, but often come with excessive refined sugars that can trigger postprandial blood pooling or energy crashes. Medical oral rehydration salts (ORS) or water with a pinch of sea salt are superior choices.
17. How long should I elevate my legs if I feel dizzy?
Elevate your legs above heart level for at least 5 to 10 minutes, or until the dizziness completely subsides. Afterward, do not stand up suddenly; perform the staged rising protocol to safely return to an upright posture.
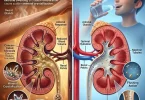
18. Can sleeping with my head elevated prevent morning dizziness?
Paradoxically, yes. Elevating the head of the bed by 4 to 6 inches reduces kidney perfusion at night, which slightly decreases nocturnal urine production. This helps you retain fluid volume overnight, leading to higher blood pressure upon waking.
19. Is alcohol the night before related to morning hypotension?
Alcohol is a potent vasodilator and diuretic. Drinking it the night before ensures you wake up with relaxed, widened blood vessels and a depleted fluid volume—the perfect recipe for severe morning orthostatic hypotension.
20. How do isometric exercises help before I get out of bed?
Isometrics, like clenching your fists or tightening your glutes and leg muscles without moving joints, physically squeeze the blood vessels inside the muscles. This increases total peripheral resistance and safely forces blood pressure upward before you stand.
21. Can spending time in nature morning help autonomic function?
Yes, gentle morning walks in green spaces stabilize the autonomic nervous system. By shifting the body into a relaxed, parasympathetic state, the regulatory centers in the brain are better equipped to handle baroreceptor reflexes smoothly throughout the day.
22. Does age affect summer morning blood pressure?
As we age, baroreceptors (the sensors that detect blood pressure drops) become less sensitive, and blood vessels lose elasticity. Elderly individuals are highly susceptible to orthostatic hypotension, making a strict morning routine a critical fall-prevention strategy.
23. What is the “osmopressor reflex”?
It is a physiological response where drinking a bolus of water (about 16 oz) rapidly stimulates sympathetic nerve fibers in the stomach lining. This triggers widespread blood vessel constriction, raising blood pressure within minutes, even before the water enters the bloodstream.
24. Should I avoid carbohydrates at breakfast?
You do not need to eliminate them, but avoid large quantities of simple, refined carbs (like pastries or sugary cereals). These digest rapidly, pulling excessive blood to the gut. Opt for complex carbs paired with proteins and healthy fats to slow digestion and stabilize vascular volume.
25. If my blood pressure is low, am I at risk for heart disease?
Chronic low blood pressure in healthy individuals is often linked to longevity and a lower risk of stroke and heart attack. The primary danger of hypotension is not organ damage, but physical trauma resulting from fainting episodes (syncope) caused by postural drops.
© 2026 Dr. Akram Medical Strategy Group. All Rights Reserved.
Disclaimer: The protocols outlined herein are for educational purposes. Always consult a board-certified physician before modifying your clinical regimens, specifically concerning cardiovascular functionality.
Medically Reviewed by Prof. Dr. Akram
Orthopedic Surgeon | Professor | Senior Medical Specialist
Prof. Dr. Akram is a distinguished surgeon with over 15 years of clinical expertise. Having served as a lead Emergency Specialist at Complex International Government Hospital, he currently leads a specialized team of 13 medical professionals at his private hospital. As a Professor at top medical universities, he ensures that every article on WellHealthOrg.com meets rigorous clinical standards.
Medical Disclaimer:
The information provided is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician for any medical concerns.
Our content is rigorously fact-checked by our 13-member Editorial Team under the clinical supervision of Prof. Dr. Akram.