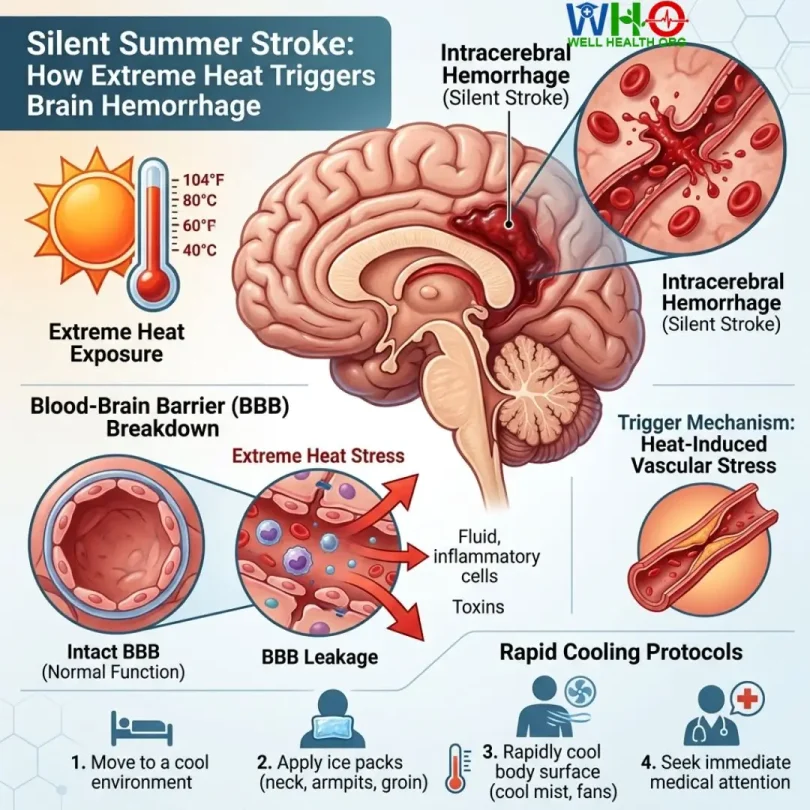
The Anatomy of a Silent Summer Stroke: When Heat Melts the Mind
The human brain is an exquisite, temperature-sensitive organ operating securely behind a physiological fortress known as the blood-brain barrier (BBB). But what happens when the ambient environment turns hostile? A Silent Summer Stroke occurs. We are no longer simply dealing with severe dehydration or basic heat exhaustion. Extreme heat melts the blood-brain barrier, triggering a catastrophic cascade of vascular failures, disseminated intravascular coagulation (DIC), and fatal brain hemorrhages.
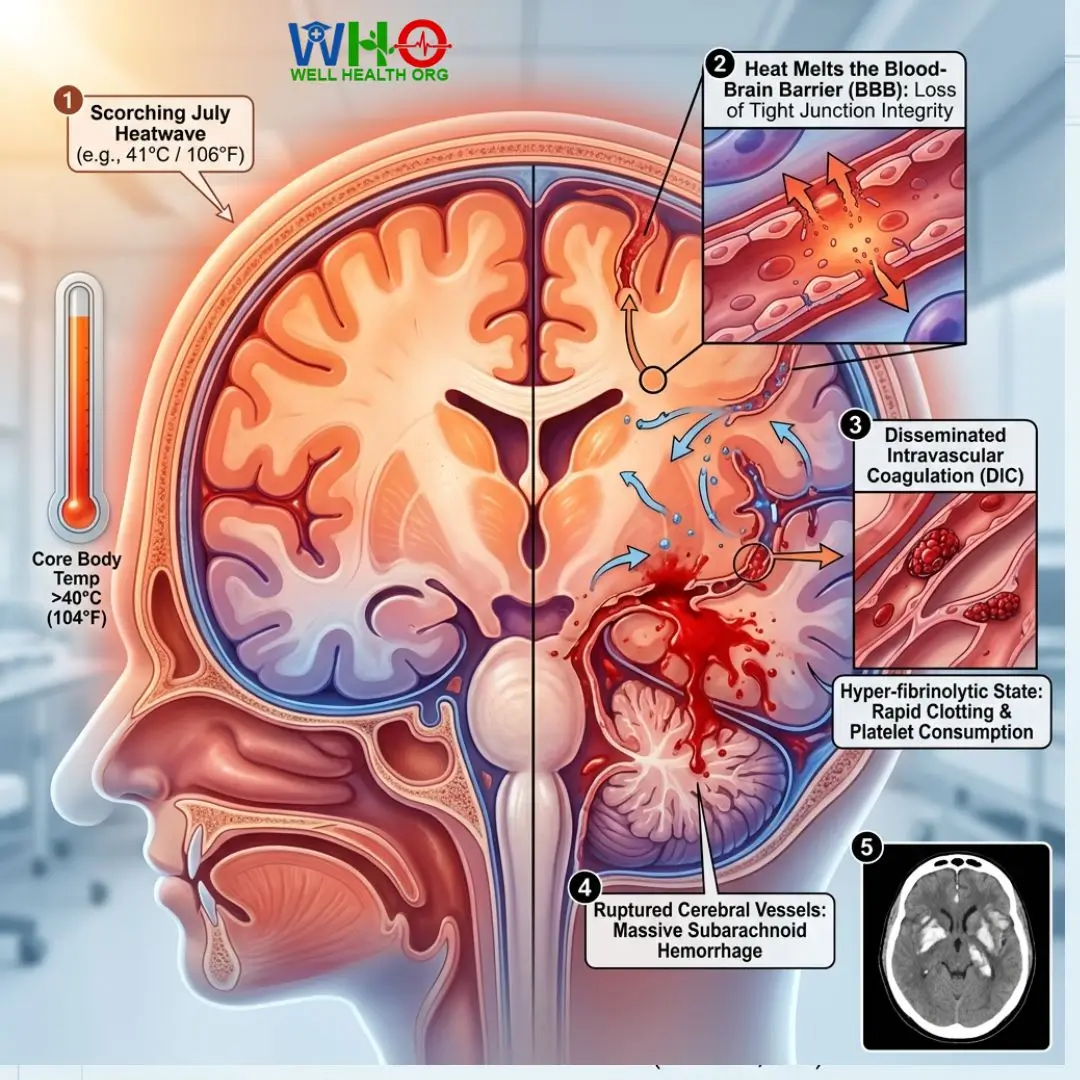
During my thirty years as a clinical neurologist, the most chilling cases I have witnessed did not happen in the dead of winter; they occurred during scorching July heatwaves. People underestimate the thermal limits of their own neurology. A Silent Summer Stroke is an insidious neurological emergency where prolonged exposure to extreme heat—driving the core body temperature above 40°C (104°F)—forces weakened capillaries in the brain to tear.
In the summer of 2018, a 55-year-old marathon runner was brought into my trauma bay. He had collapsed at the 18-mile mark in 41°C heat. The paramedics treated him for standard heatstroke. But his pupils were unequal, and his breathing was erratic. We rushed a cranial CT scan. The imaging revealed a massive subarachnoid hemorrhage. The heat had triggered a hyper-fibrinolytic state; his blood clotted rapidly, consumed all available platelets, and then his cerebral vessels ruptured. It was my clinical “Eureka” moment: Heat doesn’t just exhaust the body; it boils the vascular architecture of the mind.
Shareable Insight: “Heat doesn’t just exhaust the body; it boils the vascular architecture of the mind. Hydration is not just about quenching thirst; it is about preserving your brain’s structural integrity.” 🐦
Interactive Clinical Index
Mechanisms of a Silent Summer Stroke: The Biological Cascade
To understand a Silent Summer Stroke, we must look at the microscopic trauma occurring within the cerebral vasculature. When a patient experiences extreme heat, the body initiates massive vasodilation—widening the blood vessels to push heat to the skin for evaporative cooling. This mechanism is life-saving, but when it fails, it becomes lethal.
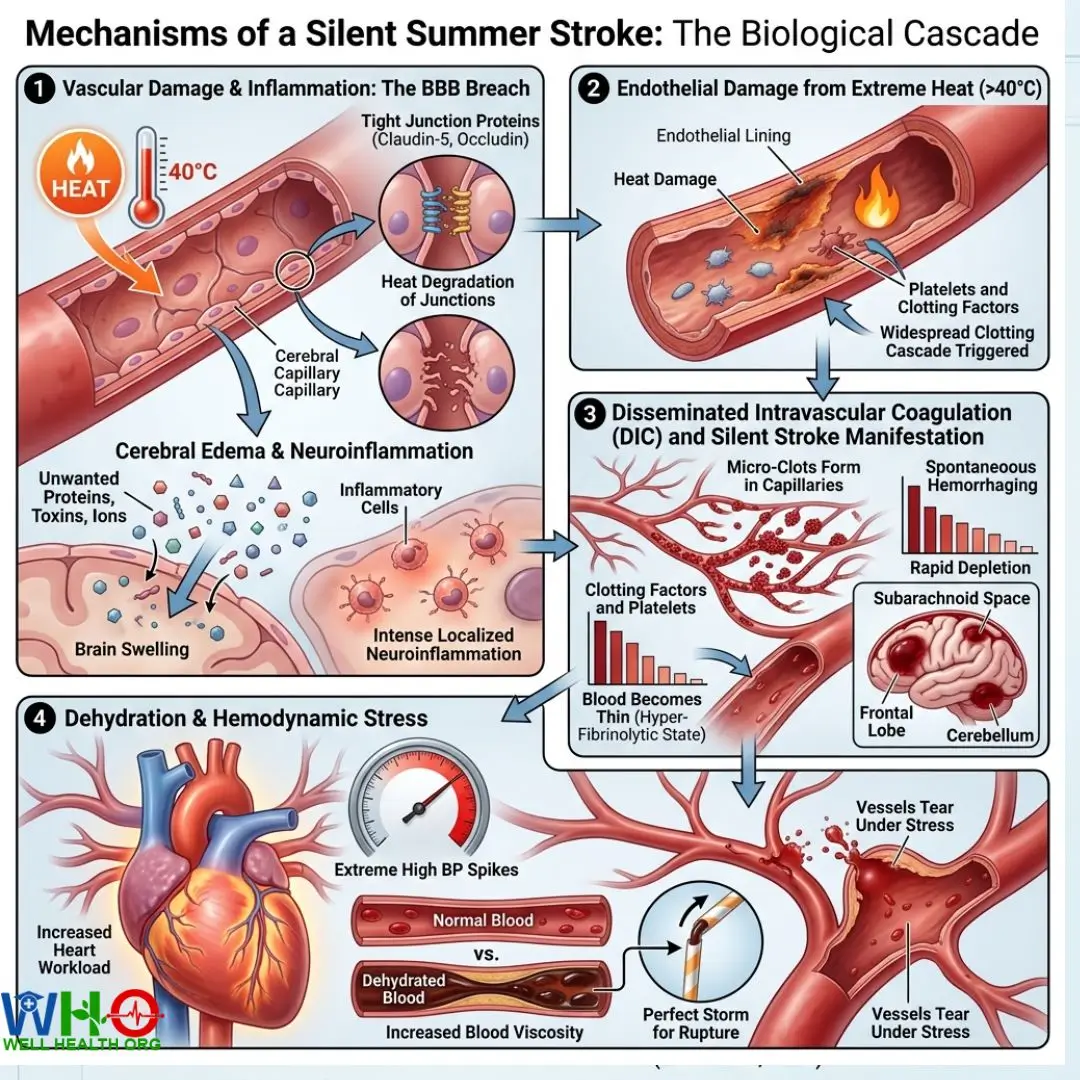
Vascular Damage & Inflammation: The BBB Breach
The blood-brain barrier (BBB) is tightly woven by endothelial cells. Thermal stress directly degrades the tight junction proteins (like Claudin-5 and Occludin) that hold these cells together. Extreme heat breaks down the blood-brain barrier, leading to immediate cerebral edema (brain swelling). Unwanted proteins, toxins, and ions flood into the brain tissue, triggering intense, localized neuroinflammation.
Coagulopathy and DIC (Disseminated Intravascular Coagulation)
As the core temperature climbs past the critical 40°C threshold, a terrifying phenomenon called DIC begins. The heat physically damages the endothelial lining of the body’s blood vessels. The immune system detects this widespread damage and mistakenly triggers massive clotting. Micro-clots form in millions of tiny capillaries. This hyper-fibrinolytic state consumes the body’s clotting factors and platelets at an unsustainable rate. Once the platelets are depleted, the blood becomes terrifyingly thin. At this exact moment, a Silent Summer Stroke manifests: spontaneous hemorrhaging occurs in the subarachnoid space, the frontal lobe, and the cerebellum.
Blood Thickening and Hemodynamic Stress
Dehydration from excessive sweating dramatically increases blood viscosity. Imagine trying to pump thick oil through a delicate paper straw. The heart must pump harder, resulting in extreme high blood pressure spikes. The combination of thick blood, intense hypertension, and weakened capillary walls provides the perfect storm for a cerebral rupture. The vessels literally tear under the pressure.
Coagulopathy: Disseminated Intravascular Coagulation (DIC)
A Silent Summer Stroke is frequently accompanied by a terrifying secondary condition known as Disseminated Intravascular Coagulation (DIC). The extreme heat essentially confuses the body’s coagulation system. Initially, it triggers a hypercoagulable state where thousands of microscopic blood clots form throughout the body’s vascular network. These clots act like tiny blockages, starving tissues of oxygen.
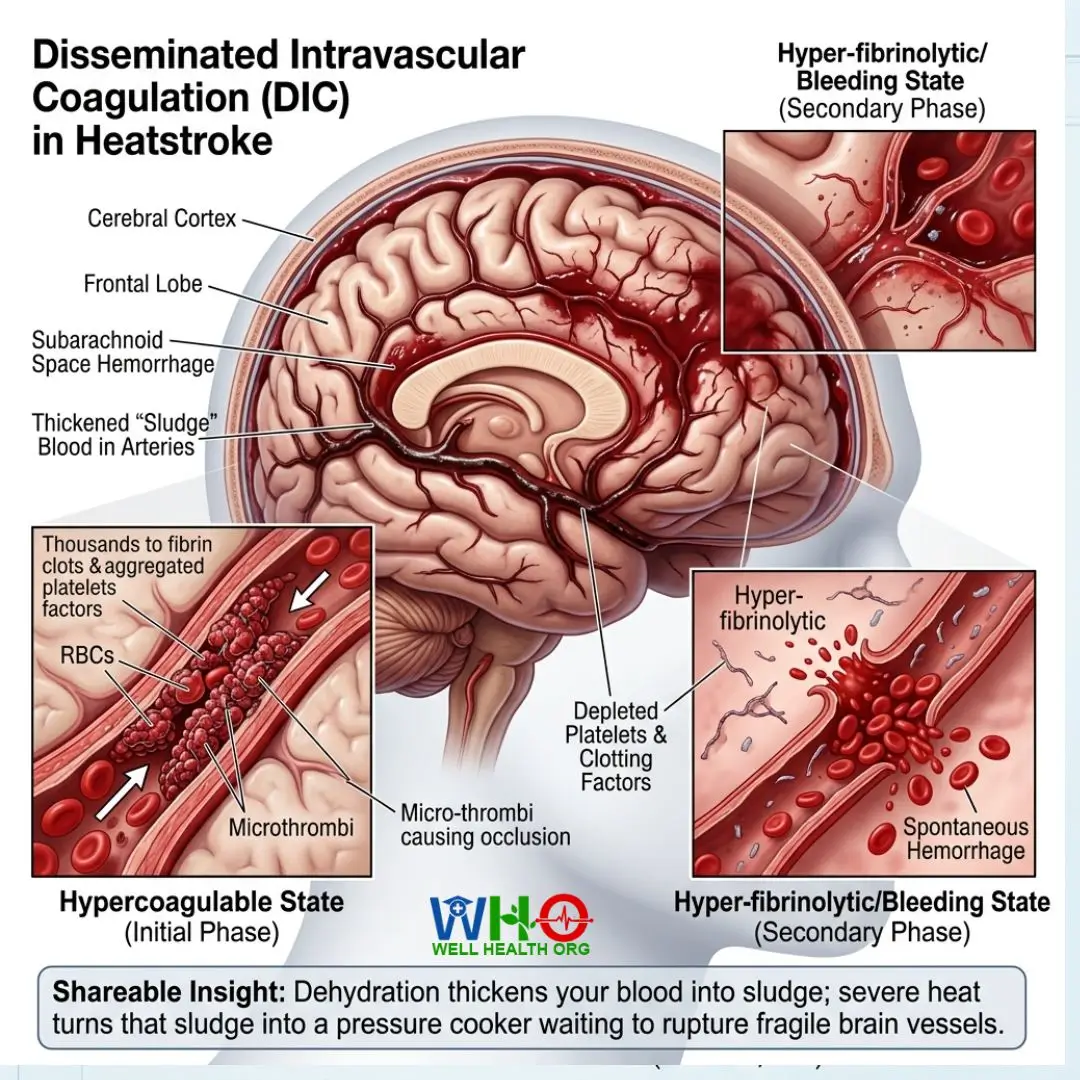
However, the human body realizes it is clotting inappropriately and attempts to break down these clots—a process known as a hyper-fibrinolytic state. The system burns through its entire supply of platelets and clotting factors. Suddenly, the patient’s blood cannot clot at all. When this state converges with the high blood pressure spikes induced by extreme dehydration and increased blood viscosity, the result is spontaneous bleeding. In a Silent Summer Stroke, this bleeding manifests mercilessly in the subarachnoid space and frontal lobes.
Shareable Insight: “Dehydration thickens your blood into sludge; severe heat turns that sludge into a pressure cooker waiting to rupture fragile brain vessels.”
Key Risk Factors: Identifying the Vulnerable
A Silent Summer Stroke does not discriminate, but it heavily favors specific biological environments.
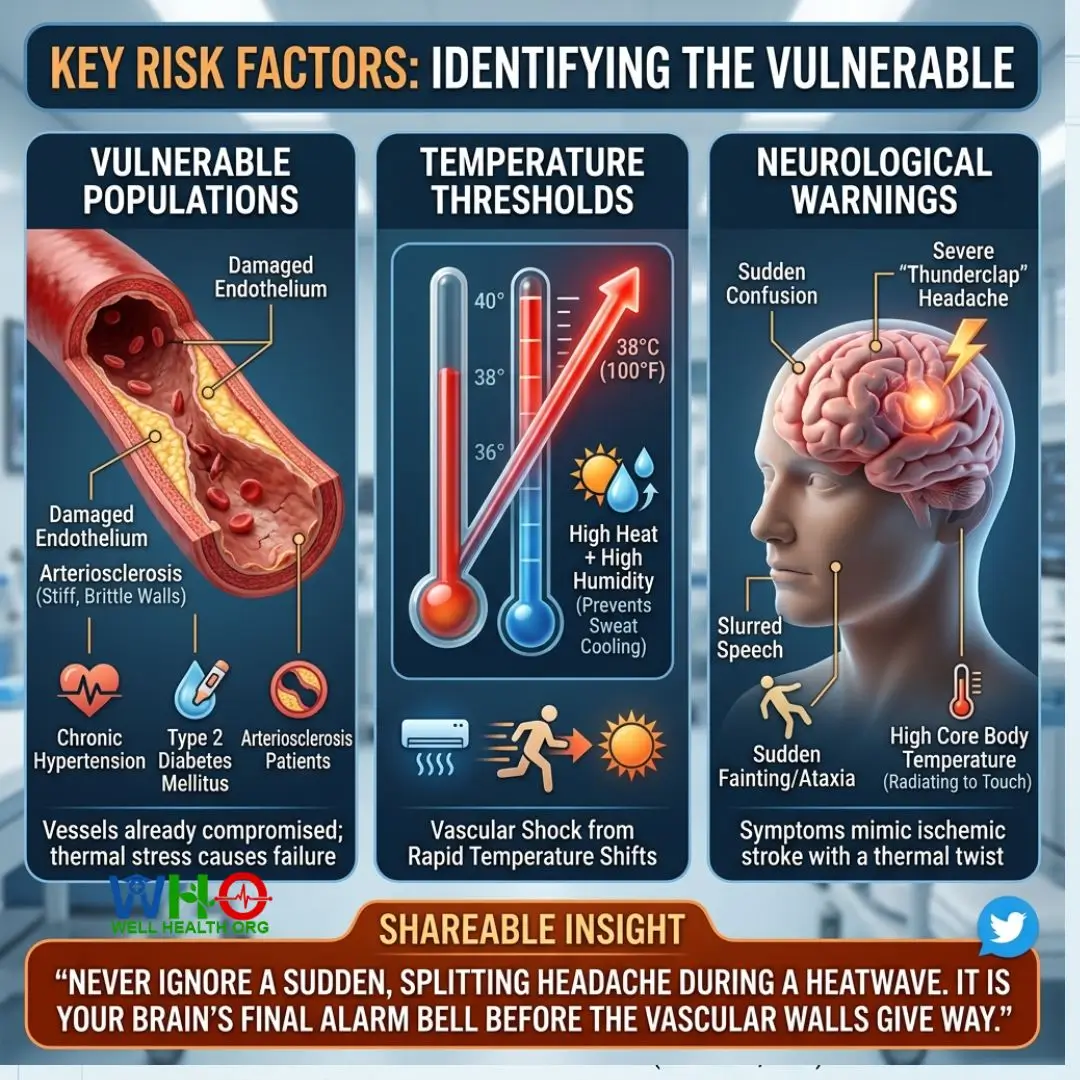
- Vulnerable Populations: Individuals with pre-existing endothelial damage are prime targets. This includes patients with chronic hypertension, type 2 diabetes mellitus, and arteriosclerosis. Their vessels are already stiff and brittle; the added thermal stress pushes them past the breaking point.
- Temperature Thresholds: The risk curve does not rise linearly; it spikes exponentially when ambient temperatures exceed 38°C (100°F) coupled with high humidity (which prevents evaporative sweat cooling). Rapid shifts from air-conditioned rooms to extreme outdoor heat can also shock the vascular system.
- Neurological Warnings: The signs to act upon mimic a traditional ischemic stroke but with a thermal twist. Look for sudden confusion, severe bursting headaches (often described as a “thunderclap”), slurred speech, sudden fainting, ataxia (loss of coordination), and a core body temperature that feels radiating to the touch.
Shareable Insight: “Never ignore a sudden, splitting headache during a heatwave. It is your brain’s final alarm bell before the vascular walls give way.” 🐦
Clinical Remedial Ecosystem: Actionable Interventions
Treating a Silent Summer Stroke requires military-grade precision. Every second the brain remains above 39°C, millions of neurons die, and the risk of irreversible hemorrhage expands. Below are the electronic remedy modules designed for immediate and long-term intervention.
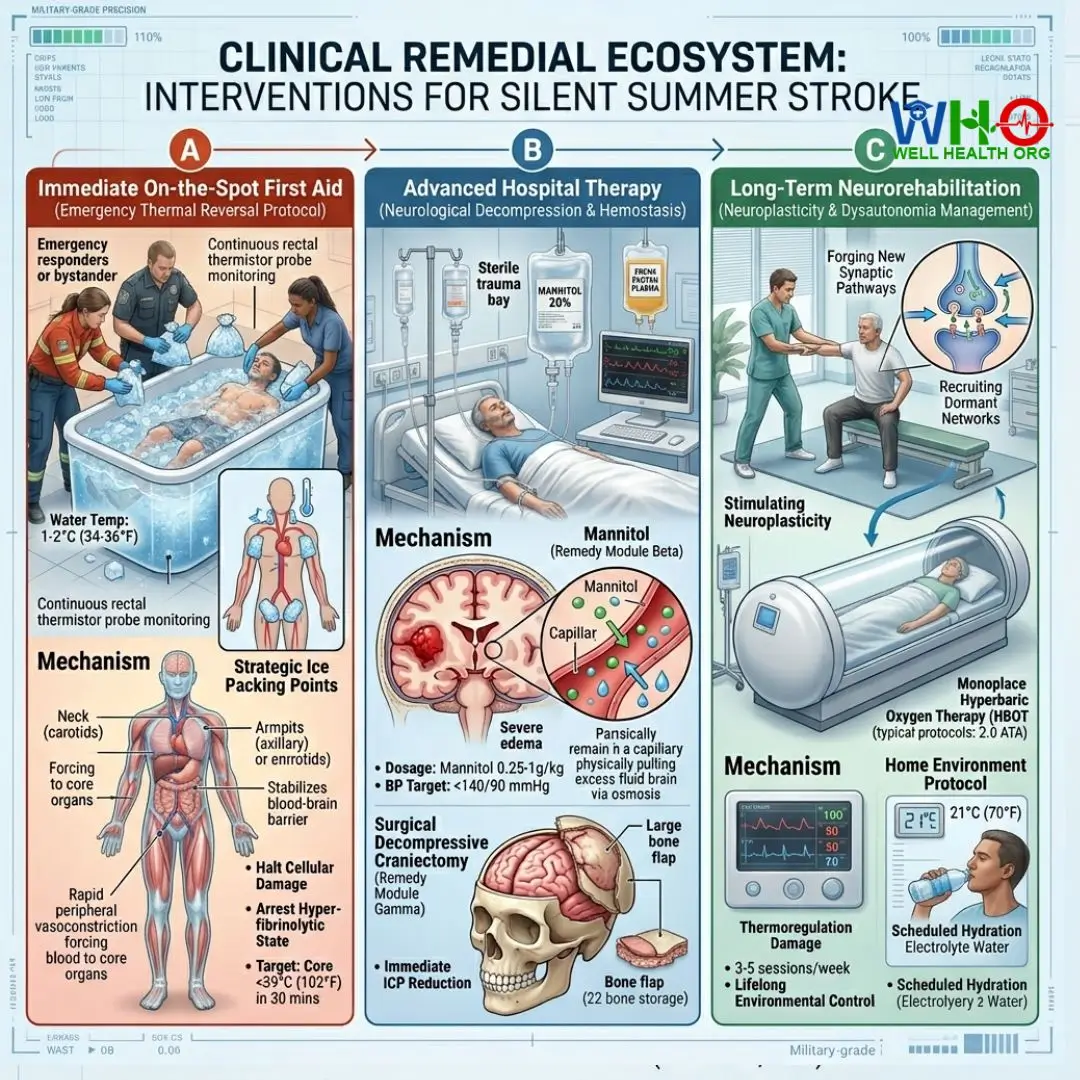
Module A: Immediate On-the-Spot First Aid
Emergency Thermal Reversal Protocol
The “Golden Hour” priority is to halt cellular damage and arrest the hyper-fibrinolytic state before full DIC onset.
- ⚡ How to Use (Clinical Application): Execute immediate rapid cooling. Do not wait for the ambulance to begin. Initiate Cold Water Immersion or Strategic Ice Packing immediately. Place the patient in the recovery position (lateral decubitus) to prevent airway aspiration if unconscious.
- ⚖️ Dosage & Quantity (Clinical Measurement): Continuous application. The absolute goal is to lower the core body temperature to below 39°C (102°F) within 30 minutes. If using ice packs, apply exactly to 4 key arterial points: bilateral neck (carotids), bilateral armpits (axillary), and bilateral groin (femoral).
- 🔬 Mechanism of Action (Electronic Biological Mapping): Rapid external cooling forces peripheral vasoconstriction, shunting blood back to the core organs. It stabilizes the blood-brain barrier lipid layers, preventing further tight-junction separation and halting the auto-immune cascade that leads to blood vessel rupture.
- 📈 Recovery Timeline (Projected Outcome): Vital signs should stabilize within 15 to 45 minutes of aggressive cooling. Failure to reduce temperature within this window increases the mortality rate of a heat-induced hemorrhage by 70%.
- 🛠️ Preparation Guide (Laboratory Method): If an ice bath is unavailable, create an “Evaporative Cooling Matrix.” Strip the patient, spray the skin continuously with cool water, and use a high-powered fan to generate artificial sweat evaporation.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): DO NOT administer fever reducers (Antipyretics). Aspirin or Acetaminophen (Tylenol) will not alter a heat-induced hypothalamic set-point. Worse, Aspirin will aggressively thin the blood, guaranteeing a catastrophic expansion of the brain hemorrhage. DO NOT give oral fluids to an altered patient due to severe aspiration risk.
Module B: Advanced Hospital Therapy
Neurological Decompression & Hemostasis
Once the patient arrives at the trauma bay, the objective shifts from cooling to pressure management and coagulation repair.
- ⚡ How to Use (Clinical Application): Intravenous Osmotic Therapy combined with strict Hemodynamic mapping. If the CT scan confirms a massive expanding hematoma, rapid Surgical Decompression (craniectomy) is initiated to relieve brainstem compression.
- ⚖️ Dosage & Quantity (Clinical Measurement): Mannitol 20% IV (0.5 to 1 g/kg) over 30 minutes, or Hypertonic Saline (3% to 23.4%) titrated to target serum sodium levels of 145-155 mEq/L. Blood pressure must be artificially clamped below 140/90 mmHg using IV Labetalol or Nicardipine.
- 🔬 Mechanism of Action (Electronic Biological Mapping): Osmotic diuretics like Mannitol create an osmotic gradient across the intact portions of the blood-brain barrier. This pulls interstitial fluid out of the swollen, edematous brain tissue and into the vascular space for renal excretion, instantly dropping intracranial pressure (ICP). Fresh Frozen Plasma (FFP) provides the specific clotting factors needed to reverse DIC.
- 📈 Recovery Timeline (Projected Outcome): ICP reduction occurs within 15-30 minutes of osmotic administration. Complete stabilization of the coagulation cascade via FFP takes 12 to 24 hours of intensive care monitoring.
- 🛠️ Preparation Guide (Laboratory Method): For extreme hyperthermic resistance, In-Vivo cooling is prepared. A gastric or Foley catheter is utilized to irrigate the stomach or bladder with sterile, ice-cold saline (4°C), actively extracting heat from the patient’s internal viscera.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): Monitor strictly for rebound intracranial hypertension once osmotic therapy wears off. Continuous arterial line monitoring is mandatory to prevent hypotensive shock, which would starve the surviving brain tissue of oxygen (secondary ischemia).
Module C: Long-Term Neurorehabilitation
Neuroplasticity & Dysautonomia Management
Surviving a Silent Summer Stroke leaves the brain highly sensitized. Recovery relies heavily on rewiring neural pathways and managing permanent temperature dysregulation.
- ⚡ How to Use (Clinical Application): Implement a customized, multi-disciplinary neurorehabilitation program. This includes Physical, Occupational, and Speech-Swallowing therapies designed to stimulate neuroplasticity—the brain’s inherent ability to forge new synaptic connections around the dead tissue.
- ⚖️ Dosage & Quantity (Clinical Measurement): Minimum of 3 to 5 therapy sessions per week, lasting 45-60 minutes each, for a continuous period of 6 to 12 months post-injury. Hyperbaric Oxygen Therapy (HBOT) protocols may involve 40 dives at 1.5 to 2.0 ATA.
- 🔬 Mechanism of Action (Electronic Biological Mapping): Repetitive physical and cognitive exercises force the brain to recruit dormant neuronal networks. HBOT supersaturates blood plasma with oxygen, forcing life-giving O2 into deep ischemic penumbra tissues, stimulating angiogenesis (new blood vessel growth) in the damaged cerebellum and hippocampus.
- 📈 Recovery Timeline (Projected Outcome): The steepest curve of neurological return occurs within the first 90 days. However, managing Post-Injury Heat Sensitivity (Dysautonomia) requires lifelong environmental control and hydration discipline.
- 🛠️ Preparation Guide (Laboratory Method): Create a rigid home environment. Set climate control strictly between 20°C and 22°C. Hydration must become scheduled, not reactive. Since the hypothalamus is damaged, the patient’s thirst mechanism is broken; they must consume 200ml of electrolyte-balanced water every two hours, regardless of thirst.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): Strict Medication Review is crucial. Survivors must be shielded from medications that inhibit sweating or alter thermoregulation, including certain anticholinergics, diuretics, and tricyclic antidepressants. Psychological screening for depression is mandatory, as cognitive fatigue frequently triggers severe emotional trauma.
Remedy Module Alpha: Rapid Cold Water Immersion (CWI)
- ⚡ How to Use (Clinical Application): Submerge the patient up to the neck in a clinical immersion tub. Constant agitation of the water is required to break the thermal barrier forming against the patient’s skin.
- ⚖️ Dosage & Quantity (Clinical Measurement): Water temperature strictly maintained between 1°C and 2°C (34°F – 36°F). Ice must be continuously added.
- 🔬 Mechanism of Action (Electronic Biological Mapping): Rapid conductive cooling extracts thermal energy directly from the skin. Peripheral vasoconstriction forces cooled blood back to the core, directly lowering brain temperature and halting the progression of the Silent Summer Stroke by stabilizing the BBB.
- 📈 Recovery Timeline (Projected Outcome): Core temperature drops at approximately 0.15°C to 0.35°C per minute. Target safe temp of 38.9°C (102°F) must be reached within 15 to 30 minutes.
- 🛠️ Preparation Guide (Laboratory Method): Prepare a standard medical tarp or portable ice bath. Stockpile minimum 40kg of medical-grade crushed ice. Insert continuous rectal thermistor for uncompromised core temperature data streaming.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): Risk of hypothermic overshoot. If core temp drops below 38°C during immersion, cardiac arrhythmias (ventricular fibrillation) may occur. Extract patient immediately upon reaching 38.9°C.
Remedy Module Beta: Intravenous Osmotic Therapy (Mannitol)
- ⚡ How to Use (Clinical Application): Administered via a dedicated central venous catheter. Used strictly when CT imaging confirms cerebral edema secondary to a heat-induced brain hemorrhage.
- ⚖️ Dosage & Quantity (Clinical Measurement): 0.25 to 1.0 g/kg body weight administered as a 20% solution infused intravenously over 20-30 minutes.
- 🔬 Mechanism of Action (Electronic Biological Mapping): Mannitol does not cross the intact blood-brain barrier. It creates an osmotic gradient in the intravascular space, physically drawing excess trapped water out of the swollen brain tissue and back into the bloodstream to be excreted by the kidneys.
- 📈 Recovery Timeline (Projected Outcome): Intracranial pressure reduction begins within 15 minutes of infusion and peaks at 60-90 minutes.
- 🛠️ Preparation Guide (Laboratory Method): Must be drawn up in the pharmacy using an inline filter (typically 5 microns) because Mannitol has a high propensity to crystallize at room temperature. Use a fluid warmer if crystallization is observed.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): Rebound intracranial hypertension can occur if administered too rapidly. Extreme caution required as it can worsen dehydration; strict electrolyte and renal function monitoring is mandatory.
Remedy Module Gamma: Surgical Decompressive Craniectomy
- ⚡ How to Use (Clinical Application): Emergency neurosurgery utilized when medical management fails to control rising intracranial pressure from the Silent Summer Stroke hemorrhage.
- ⚖️ Dosage & Quantity (Clinical Measurement): Removal of a large bone flap (typically >12cm in diameter) from the affected cranial vault.
- 🔬 Mechanism of Action (Electronic Biological Mapping): By physically removing a portion of the rigid skull and opening the dura mater, the swelling brain is given physical space to expand outward rather than compressing downward into the fatal brainstem (herniation).
- 📈 Recovery Timeline (Projected Outcome): Immediate drop in intracranial pressure on the operating table. The bone flap is stored subcutaneously in the patient’s abdomen or a medical freezer for reimplantation 3-6 months later.
- 🛠️ Preparation Guide (Laboratory Method): Absolute sterility required. Pre-operative mapping of the hematoma via 3D MRI reconstruction to determine the exact surgical trajectory.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): High risk of post-operative infection, hydrocephalus, or “syndrome of the trephined” (neurological deterioration due to atmospheric pressure on the unprotected brain).
The Long Road Back: Neurorehabilitation Strategies
Surviving a Silent Summer Stroke is only the first battle. A heat-induced brain hemorrhage leaves behind microscopic scars, particularly in the cerebellum (which governs balance) and the hippocampus (which governs memory). Once the patient is neurologically stabilized, aggressive neurorehabilitation must commence.
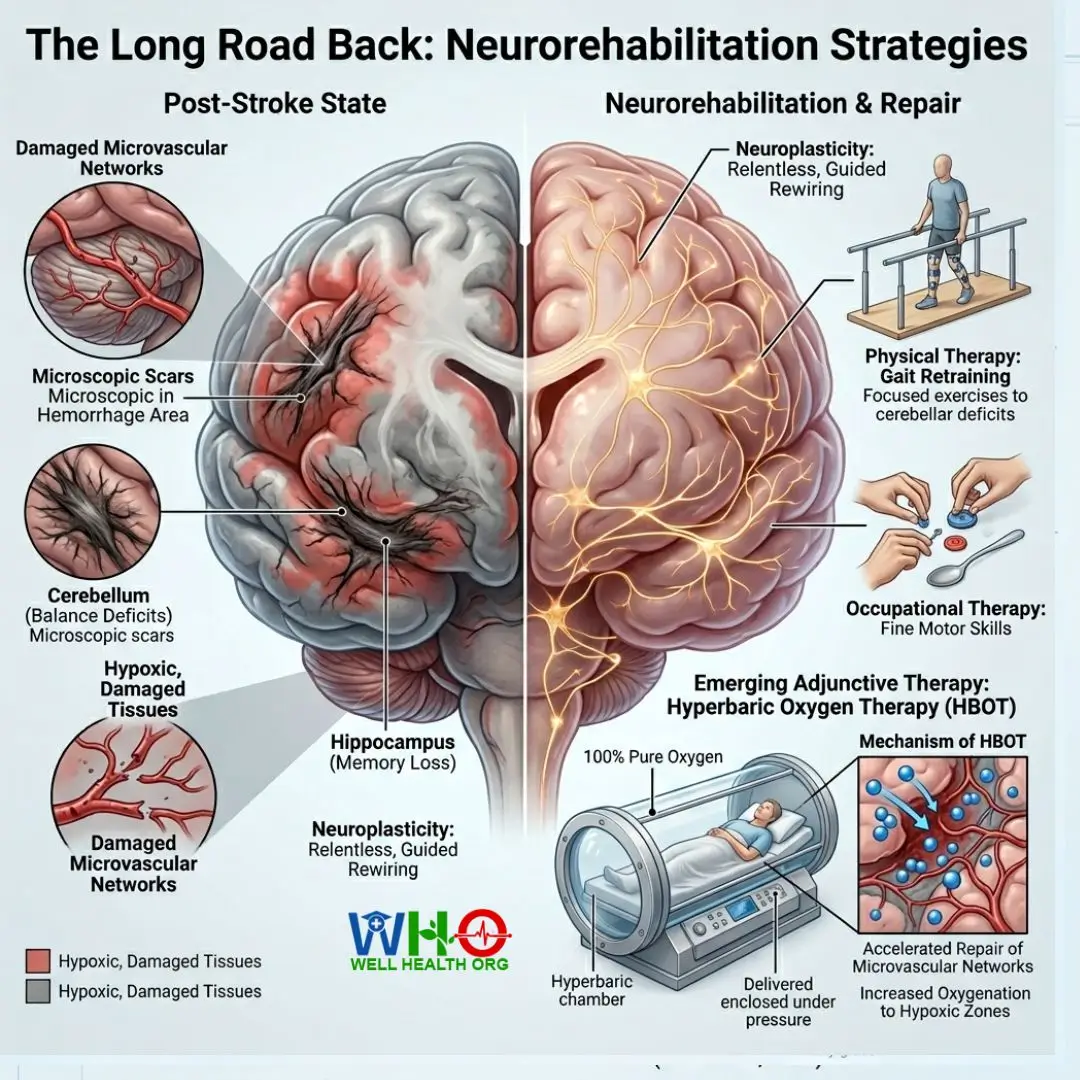
Neuroplasticity is our greatest ally here. The brain possesses an astonishing ability to rewire itself, but it requires relentless, guided stimulation. Physical therapy focuses on gait retraining and fall prevention, heavily targeting cerebellar deficits. Occupational therapy is crucial for regaining fine motor skills, allowing survivors to navigate daily life tasks like dressing and cooking.
One emerging adjunctive therapy we frequently monitor is Hyperbaric Oxygen Therapy (HBOT). By placing the survivor in a pressurized chamber breathing 100% pure oxygen, we can force oxygen deeper into the damaged, hypoxic brain tissues surrounding the hemorrhage site, theoretically accelerating the repair of the microvascular networks damaged by the heatstroke.
Managing Post-Injury Dysautonomia
One of the most frustrating, chronic side effects of surviving a Silent Summer Stroke is the onset of Dysautonomia. The autonomic nervous system—the brain’s internal thermostat—is permanently altered. Survivors lose their natural ability to properly regulate body temperature, sweat efficiently, or sense thirst accurately.

Hydration discipline must become a mechanical habit, untethered from the biological sensation of thirst. Survivors are instructed to consume fluids on a strict schedule. Environmental control is paramount; outdoor exposure during peak thermal hours (11 AM to 4 PM) must be entirely avoided. Additionally, a rigorous medication review is required. Many common drugs, including diuretics, antihistamines, and certain antidepressants, further inhibit sweating and blood flow, turning an ordinary sunny day into an immediate relapse risk.
Shareable Insight: “After a heat-induced stroke, thirst is a broken alarm bell. You must hydrate by the clock, not by feeling.”
Regional Patient Summaries
🇮🇳 Quick Summary in Hindi (हिंदी में सारांश)
- साइलेंट समर स्ट्रोक एक जानलेवा स्थिति है जो अत्यधिक गर्मी के कारण होती है।
- यह केवल डिहाइड्रेशन नहीं है, बल्कि गर्मी मस्तिष्क की रक्त वाहिकाओं (blood vessels) को पिघला देती है।
- शरीर का तापमान 40°C से ऊपर जाने पर ब्लड-ब्रेन बैरियर टूट जाता है।
- गर्मी के कारण खून गाढ़ा हो जाता है, जिससे ब्लड प्रेशर अचानक बढ़ जाता है।
- DIC नामक स्थिति पैदा होती है, जिसमें शरीर के अंदर खून के थक्के (clots) बनने लगते हैं।
- थक्के बनने के बाद खून अत्यधिक पतला हो जाता है, जिससे ब्रेन हेमरेज (brain hemorrhage) हो जाता है।
- हाई ब्लड प्रेशर और डायबिटीज के मरीजों को इसका सबसे ज्यादा खतरा होता है।
- लक्षणों में अचानक भयंकर सिरदर्द, भ्रम (confusion), और बोलने में दिक्कत शामिल हैं।
- यह एक इमरजेंसी है; 39°C से नीचे तापमान लाना सबसे पहली प्राथमिकता है।
- मरीज को तुरंत ठंडे पानी या बर्फ के टब में रखें।
- गर्दन, कांख (armpits) और जांघों पर बर्फ की पट्टियां लगाएं।
- मरीज को एस्पिरिन (Aspirin) या पैरासिटामोल बिल्कुल न दें, इससे ब्लीडिंग का खतरा बढ़ जाता है।
- बेहोशी की हालत में मरीज को पानी पिलाने की कोशिश न करें, पानी फेफड़ों में जा सकता है।
- अस्पताल में डॉक्टर ऑस्मोटिक थेरेपी और जरूरत पड़ने पर सर्जरी का उपयोग करते हैं।
- रिकवरी के लिए लंबे समय तक फिजियोथेरेपी और तापमान नियंत्रण की आवश्यकता होती है।
🇮🇳 Quick Summary in Hinglish (Hinglish Summary)
- Silent Summer Stroke ek extreme aur life-threatening condition hai jo severe heatwave mein hoti hai.
- Yeh sirf dehydration nahi hai, extreme heat brain ki blood vessels ko damage kar deti hai.
- Jab core body temperature 40°C cross karta hai, blood-brain barrier break ho jata hai.
- Paseene ki wajah se body ka blood thick ho jata hai, jisse BP achanak shoot up karta hai.
- Is condition mein DIC trigger hota hai, jisme puri body mein micro-clots banne lagte hain.
- Clotting factors khatam hone par blood ekdum patla ho jata hai, leading to massive brain hemorrhage.
- Hypertension aur diabetes ke patients iske liye sabse zyada vulnerable hote hain.
- Warning signs mein sudden severe headache (thunderclap headache), confusion, aur slurred speech aate hain.
- Yeh ek medical emergency hai; Golden Hour mein temperature ko 39°C se niche lana zaroori hai.
- Patient ko turant cold water immersion ya ice bath dein.
- Neck, armpits, aur groin area par ice packs strategically place karein.
- Bhool kar bhi Aspirin ya fever reducers na dein, isse brain bleeding aur badh jayegi.
- Agar patient unconscious hai, toh use muh se liquid na dein (aspiration risk).
- Hospital mein doctors IV osmotic therapy aur surgical decompression use karte hain brain swelling kam karne ke liye.
- Long-term recovery ke liye strict hydration discipline, neuro-rehab aur AC environments zaroori hain.
Comprehensive Silent Summer Stroke FAQ Database
To further map the clinical contours of a Silent Summer Stroke, I have compiled twenty-five of the most critical queries I encounter from emergency residents, patients, and families regarding this devastating heat-induced phenomenon.
1. What exactly is a Silent Summer Stroke?
A Silent Summer Stroke is a severe neurological emergency triggered by extreme heat. Unlike a traditional ischemic stroke caused by a cholesterol plaque, this stroke occurs when severe heatstroke induces a breakdown of the blood-brain barrier, causing coagulopathy (DIC) and resulting in spontaneous, fatal brain hemorrhages.
2. How does extreme heat cause the brain to bleed?
Extreme heat damages the endothelial cells lining your blood vessels. This damage triggers widespread, abnormal blood clotting (DIC). The body uses up all its platelets trying to fix the micro-damage. Once platelets are depleted, the blood becomes artificially thin, and the weakened cerebral vessels tear under high blood pressure, leaking blood into the brain.
3. What is Disseminated Intravascular Coagulation (DIC)?
DIC is a pathological disruption of the blood’s coagulation system. In a Silent Summer Stroke, hyperthermia triggers a hyper-fibrinolytic state where micro-clots form uncontrollably throughout the body. This paradoxical condition rapidly consumes clotting factors, leaving the patient simultaneously suffering from blockages and massive spontaneous bleeding.
4. Why is it called “Silent”?
It is termed “silent” because the initial symptoms—fatigue, sweating, and dizziness—are often dismissed as everyday summer exhaustion. The internal vascular destruction happens quietly until the moment a massive hemorrhage triggers a sudden collapse, seizure, or coma.
5. What are the earliest warning signs?
Neurological warnings include sudden and severe confusion, slurred speech, ataxia (a lack of muscle coordination making walking difficult), a sudden “thunderclap” headache, and the cessation of sweating despite an extremely high core body temperature.
6. Why shouldn’t I give Aspirin to someone with a heat stroke?
Aspirin and other antipyretics lower fevers caused by infection (altering the hypothalamic set-point). They do absolutely nothing for environmental hyperthermia. Critically, Aspirin is a blood thinner. If the patient is suffering from a Silent Summer Stroke, giving them Aspirin will exponentially worsen the brain hemorrhage, often making it fatal.
7. How quickly does brain damage occur at 40°C?
Cellular death and protein denaturation begin almost immediately once the core body temperature surpasses 40°C (104°F). Every minute spent above this threshold exponentially increases the severity of the blood-brain barrier breach and subsequent cerebral edema.
8. What is the absolute best first aid measure?
Rapid cold water immersion. Submerging the patient in an ice bath up to their neck provides the fastest heat extraction. If a bath is unavailable, aggressive evaporative cooling (spraying with water and using fans) combined with ice packs on the neck, armpits, and groin is the alternative.
9. How does dehydration contribute to a stroke?
Massive fluid loss via sweating decreases your overall blood plasma volume. This drastically increases blood viscosity (thickness). Thick blood requires the heart to pump with much higher pressure, stretching and stressing cerebral capillaries until they physically rupture under the strain.
10. Who is most at risk for a heat-induced hemorrhage?
Patients with pre-existing vascular compromises are highly vulnerable. This includes people with uncontrolled hypertension, arteriosclerosis, chronic kidney disease, and diabetes. Elderly populations, whose bodies have naturally weakened thermoregulatory responses, face the highest mortality rates.
11. Can medications increase the risk of a Silent Summer Stroke?
Yes. Diuretics (water pills) cause deliberate dehydration. Beta-blockers impair the heart’s ability to increase output for skin cooling. Anticholinergics and certain psychiatric medications actively suppress the body’s ability to sweat, trapping the heat internally.
12. What happens in the hospital for a heat-induced hemorrhage?
Trauma teams utilize an aggressive multi-pronged approach: Intravenous osmotic therapy (Mannitol) to pull fluid out of the swollen brain, Fresh Frozen Plasma to fix the DIC clotting failure, strict blood pressure clamping with IV medications, and potentially surgical craniectomy to relieve skull pressure.
13. Is recovery from a heat-induced brain hemorrhage possible?
Yes, but it requires intensive, long-term neurorehabilitation. Through physical, cognitive, and speech therapy, the brain relies on neuroplasticity to reroute functions around the dead tissue. However, permanent deficits in motor function and thermoregulation are common.
14. What is dysautonomia post-stroke?
Dysautonomia involves a malfunction of the autonomic nervous system. Survivors of a Silent Summer Stroke often suffer localized damage to the hypothalamus, permanently impairing their ability to regulate their own body temperature, heart rate, and blood pressure in the future.
15. How should survivors manage future heat exposure?
Survivors must practice strict environmental control. They should remain in climate-controlled (air-conditioned) environments, absolutely avoid outdoor exposure between 11 AM and 4 PM, and adhere to rigid, scheduled hydration routines rather than relying on natural thirst indicators.
16. Why is Hyperbaric Oxygen Therapy (HBOT) used?
HBOT places the patient in a pressurized chamber breathing 100% oxygen. This supersaturates the blood plasma, allowing oxygen to bypass damaged capillaries and penetrate deep into ischemic brain tissues, which promotes the healing of injured neurons and the growth of new blood vessels.
17. Are children at risk for this?
Yes. Children, particularly infants left in hot cars, are at extreme risk. Their surface-area-to-mass ratio is different, causing them to absorb heat much faster than adults. Their immature thermoregulatory systems fail rapidly, leading to rapid-onset cerebral edema.
18. Does drinking alcohol increase the risk?
Tremendously. Alcohol is a potent diuretic, accelerating dehydration. It also impairs judgment (causing people to stay out in the heat) and artificially dilates peripheral blood vessels initially, confusing the body’s natural thermal regulation processes.
19. What is the recovery position and why use it?
The recovery position involves rolling an unconscious patient onto their side with their top knee bent. In the event of a severe brain injury, vomiting is highly common. This position prevents the patient from aspirating (inhaling) their own vomit, which causes fatal chemical pneumonitis.
20. How do doctors measure brain pressure?
In an intensive care unit setting, neurosurgeons will drill a small burr hole through the skull to insert an external ventricular drain (EVD) or an intracranial pressure (ICP) monitor. This directly measures the pressure exerted by the hemorrhage against the inside of the skull.
21. Can physical exertion trigger this even without extreme weather?
Yes, this is known as Exertional Heatstroke. Highly motivated individuals like marathon runners, military recruits, or football players generating massive internal metabolic heat can push their core temperatures above 40°C even on mildly warm days, triggering the exact same hemorrhagic cascade.
22. What role do electrolytes play in prevention?
Sweat depletes massive amounts of sodium, potassium, and magnesium. Drinking only plain water can lead to hyponatremia (low blood sodium), which actively exacerbates cerebral edema. Electrolyte solutions maintain the osmotic balance, protecting brain cells from severe swelling.
23. Is a CT scan or MRI better for diagnosing this?
In an emergency setting, a non-contrast Head CT scan is the gold standard. It is incredibly fast and highly sensitive to acute blood (which shows up bright white on the scan). Once the patient is stabilized, an MRI may be used later to map exact tissue damage and neuroinflammation.
24. Can recurrent minor heat exhaustion lead to long-term damage?
Repeated thermal stress without adequate recovery can cause cumulative micro-vascular damage and chronic low-grade neuroinflammation. Over time, this steadily weakens the integrity of the blood-brain barrier, drastically increasing the likelihood of a major rupture during a subsequent severe heat exposure.
25. How do I help an elderly relative survive heatwaves?
Check on them twice daily. Ensure they have functioning air conditioning, as fans are insufficient above 35°C (they essentially act as convection ovens). Provide ready-to-drink electrolyte beverages, review their medications with a doctor, and keep them indoors during peak solar radiation hours.
© 2026 Dr. Akram Medical Strategy Group. All Rights Reserved.
Medically Reviewed by Prof. Dr. Akram
Orthopedic Surgeon | Professor | Senior Medical Specialist
Prof. Dr. Akram is a distinguished surgeon with over 15 years of clinical expertise. Having served as a lead Emergency Specialist at Complex International Government Hospital, he currently leads a specialized team of 13 medical professionals at his private hospital. As a Professor at top medical universities, he ensures that every article on WellHealthOrg.com meets rigorous clinical standards.
Medical Disclaimer:
The information provided is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician for any medical concerns.
Our content is rigorously fact-checked by our 13-member Editorial Team under the clinical supervision of Prof. Dr. Akram.