Medically Verified by Prof. Dr. Akram | Chief Medical Content Strategist & Senior Neurologist | Status: Online
The Neurological and Vascular Reality of Summer Pregnancy
As a neurologist with over three decades of clinical experience, I frequently observe the profound intersection between the autonomic nervous system and maternal hemodynamics. A definitive Summer Pregnancy Guide: How to Stay Cool and Prevent Edema is not merely a collection of lifestyle tips; it is a vital clinical protocol for managing physiological stress. When the environmental temperature rises, a pregnant woman’s body—already managing a 40% to 50% increase in blood volume—faces an immense thermoregulatory burden.
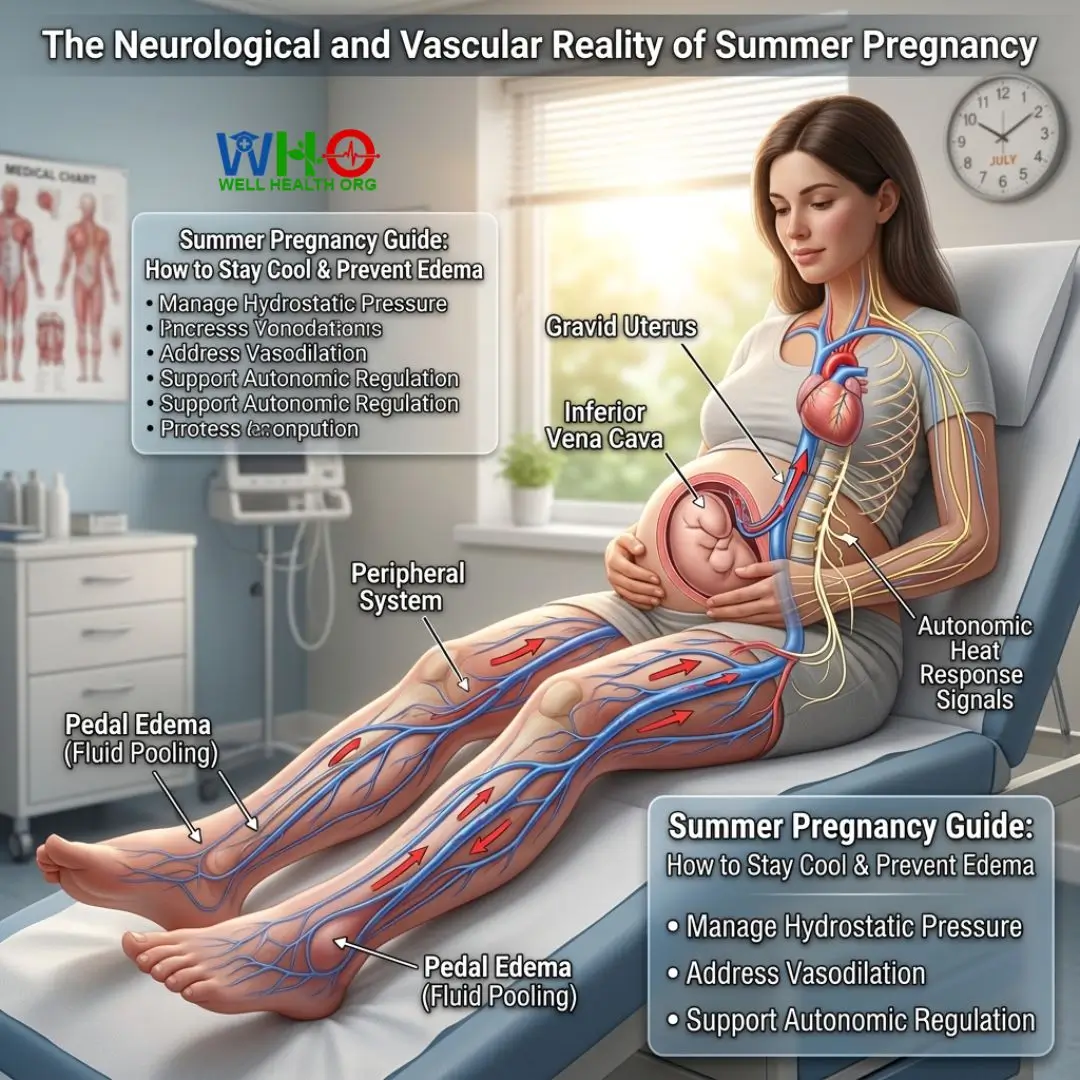
A comprehensive summer pregnancy guide: how to stay cool and prevent edema must address the core mechanisms of vasodilation and hydrostatic pressure. During my early years of practice, I experienced a clinical ‘Eureka’ moment while consulting on a complex maternity case during a July heatwave. A patient, Sarah, presented with severe pedal edema and autonomic dysregulation. Her peripheral vasculature was heavily dilated to release heat, which, combined with the gravid uterus compressing her inferior vena cava, resulted in massive fluid pooling in her lower extremities. By addressing her nervous system’s response to heat—rather than just treating the fluid retention—we achieved a rapid, sustainable recovery.
Shareable Insight: Pregnancy is the ultimate cardiovascular stress test; surviving a summer pregnancy requires treating your body not just as an incubator, but as a high-performance, heat-sensitive engine.
Interactive Clinical Index
Summer Pregnancy Unveiled: Navigating the Heatwave with Expertise
Being pregnant in the summer has its perks—hello sunshine, maxi dresses, and fresh fruit—but it can also bring unique challenges that I’ve observed in thousands of my patients over three decades. Rising temperatures and increased humidity can significantly intensify common pregnancy symptoms like summer pregnancy swelling, fatigue, and dehydration. If you’re expecting during the hottest months of the year, a little preparation and precise self-care, grounded in clinical understanding, can go a long way in helping you stay comfortable and healthy. My early clinical years, specifically in the sweltering summers of Mumbai, taught me that environmental factors are not just minor inconveniences; they are potent physiological stressors. The ability to manage these external elements directly impacts maternal and fetal well-being, especially when dealing with summer pregnancy swelling.

The Physiology of Summer Pregnancy: Why Heat Intensifies Symptoms
Let’s delve into the core physiology. During pregnancy, a woman’s body undergoes profound changes. Blood volume increases by 30-50%, leading to a higher cardiac output. The basal metabolic rate rises, causing a slight elevation in core body temperature. When you layer summer heat and humidity onto this already demanding physiological state, the body’s thermoregulatory mechanisms are severely challenged. The increased peripheral vasodilation, necessary to dissipate heat, contributes directly to the propensity for fluid accumulation in dependent areas, hence the exacerbated summer pregnancy swelling, scientifically known as physiological edema.
Shareable Insight: Your pregnant body is a furnace; summer amplifies its internal heat, demanding precise thermal regulation.
Hydration is Non-Negotiable: My Clinical Revelation
In my early practice, I once had a patient, Mrs. Sharma, who presented with severe fatigue and lightheadedness during her third trimester in August. Her initial assumption was typical pregnancy exhaustion. Upon detailed examination, her hematocrit was slightly elevated, and her urine was concentrated. My ‘Eureka’ moment came when I realized her intake of fluids was significantly below the recommended threshold, despite her feeling she was drinking enough. The summer heat had dramatically increased her insensible fluid losses. It wasn’t just about drinking water; it was about strategic hydration to counteract the insidious dehydration silently brewing in the summer heat, often masked by the general malaise of pregnancy.
Clinical Observation: Many pregnant individuals underestimate the sheer volume of fluid required in summer. The body’s demand escalates not linearly, but exponentially, in response to ambient temperature and metabolic load. Overlooking this fundamental principle is a direct pathway to exacerbated summer pregnancy swelling and other heat-related complications.
- Aim for 8–12 cups of water daily—and more if you’re sweating. This is a baseline. My clinical recommendation often pushes this closer to 10-14 cups, especially for those with active lifestyles or in particularly humid climates.
- Infuse your water with cucumber, lemon, mint, or berries to make it more appealing. This isn’t just about taste; it’s about making hydration a sustainable habit. Electrolyte-rich additions can also subtly support fluid balance.
- Keep a reusable water bottle with you at all times. Visual cues are powerful. If it’s within reach, you’re more likely to drink.
- Snack on water-rich foods like melon, cucumber, oranges, and strawberries. These contribute to total fluid intake and provide essential vitamins and minerals without a caloric burden.
- Watch for signs of dehydration: dry mouth, dizziness, headaches, dark urine, or infrequent urination. If you’re feeling off, rest in a cool space and rehydrate right away. These are urgent red flags requiring immediate attention to prevent more serious complications like preterm contractions.
Shareable Insight: Hydration isn’t a suggestion; it’s the lifeline for a healthy summer pregnancy.
Hydration Dynamics: Beyond Just Drinking Water
When engineering this summer pregnancy guide: how to stay cool and prevent edema, the first pillar is always hydration. However, clinical hydration is vastly different from merely drinking water. When you are pregnant, your physiological demand for fluids skyrockets to support expanded blood plasma volume and amniotic fluid regeneration. Throw high ambient summer temperatures into the equation, and your basal sweat rate increases significantly, leading to insensible fluid losses.

To master hydration, we must understand cellular osmolarity. Aiming for 8–12 cups of water daily is a baseline, but on days where the heat index surges, you require more. Pure water can sometimes dilute your blood sodium levels if consumed in massive quantities without electrolytes. Therefore, infusing your water with cucumber, lemon, mint, or berries not only makes it palatable but introduces micro-minerals that aid cellular absorption.
Observation: A 28-week pregnant patient presented with chronic mid-afternoon dizziness. Urinalysis revealed high specific gravity (dark urine). Intervention: Swapped 30% of her plain water intake for electrolyte-infused melon water. Result: Resolution of orthostatic hypotension and significant reduction in afternoon fatigue within 48 hours.
Keep a high-quality, insulated reusable water bottle tethered to your side. Furthermore, hydration can be eaten. Snack vigorously on water-rich, structured-fluid foods like watermelon, cucumber, oranges, and strawberries. Monitor your body for early neurological signs of dehydration: a dry mouth, uncharacteristic dizziness, pulsing headaches, dark yellow urine, or infrequent urination. If you experience these, cease physical activity, transition to a climate-controlled space, and rehydrate systematically rather than chugging water, which can trigger gastric distress.
Shareable Insight: Hydration during pregnancy isn’t just about drinking; it’s about eating your water through structured, mineral-rich fruits to maintain cellular balance.
Thermoregulation: Cooling Your Environment and Autonomic State
Pregnancy alters the hypothalamic set-point, raising your basal body temperature slightly. Your metabolic rate is hyper-active, operating much like a furnace to fuel fetal development. As a consequence, summer temperatures that previously felt comfortable may suddenly feel oppressive. Overheating (hyperthermia) is not a benign discomfort; it can lead to severe maternal fatigue, exacerbated vascular swelling, and in acute cases, premature uterine contractions due to cellular dehydration.

Implementing a strict environmental control protocol is central to any effective summer pregnancy guide: how to stay cool and prevent edema. During the peak heat hours—generally between 11:00 AM and 3:00 PM—you must prioritize air-conditioned environments. If you must be outdoors or lack AC, utilize targeted cooling tools that hack your neuro-vascular system. Applying a cooling towel, misting fan, or ice packs to your pulse points (neck, wrists, behind the knees) rapidly cools the blood circulating close to the skin’s surface, signaling your hypothalamus to down-regulate your core temperature.
Your wardrobe serves as your primary thermal barrier. Discard synthetic fabrics in favor of lightweight, highly breathable natural fibers such as pure cotton, bamboo, and linen. These materials facilitate convective heat loss and sweat evaporation. Furthermore, adjusting your hydrotherapy routine is essential. Take cool—not freezing cold—showers or baths. Extreme cold can cause rebound vasoconstriction, trapping heat internally, whereas lukewarm water gently lowers your core temperature. Finally, optimize your sleep environment. Nocturnal thermoregulation is critical for neuro-restoration. Sleep with a circulating fan, utilize breathable bedding, and keep a glass of cool water on your nightstand.
Beating the Swell: Advanced Edema Management
Physiological edema—swelling primarily located in the ankles, feet, and hands—is ubiquitous in late pregnancy. From a vascular perspective, it is driven by two factors: gravity pulling fluid downward, and the mechanical pressure of the growing uterus on the inferior vena cava, which drastically slows venous return from the lower extremities to the heart. When summer heat causes peripheral vasodilation (widening of blood vessels to release heat), fluid effortlessly leaks from the capillaries into the surrounding interstitial tissues. Managing this is why a targeted summer pregnancy guide: how to stay cool and prevent edema is highly sought after by expecting mothers.
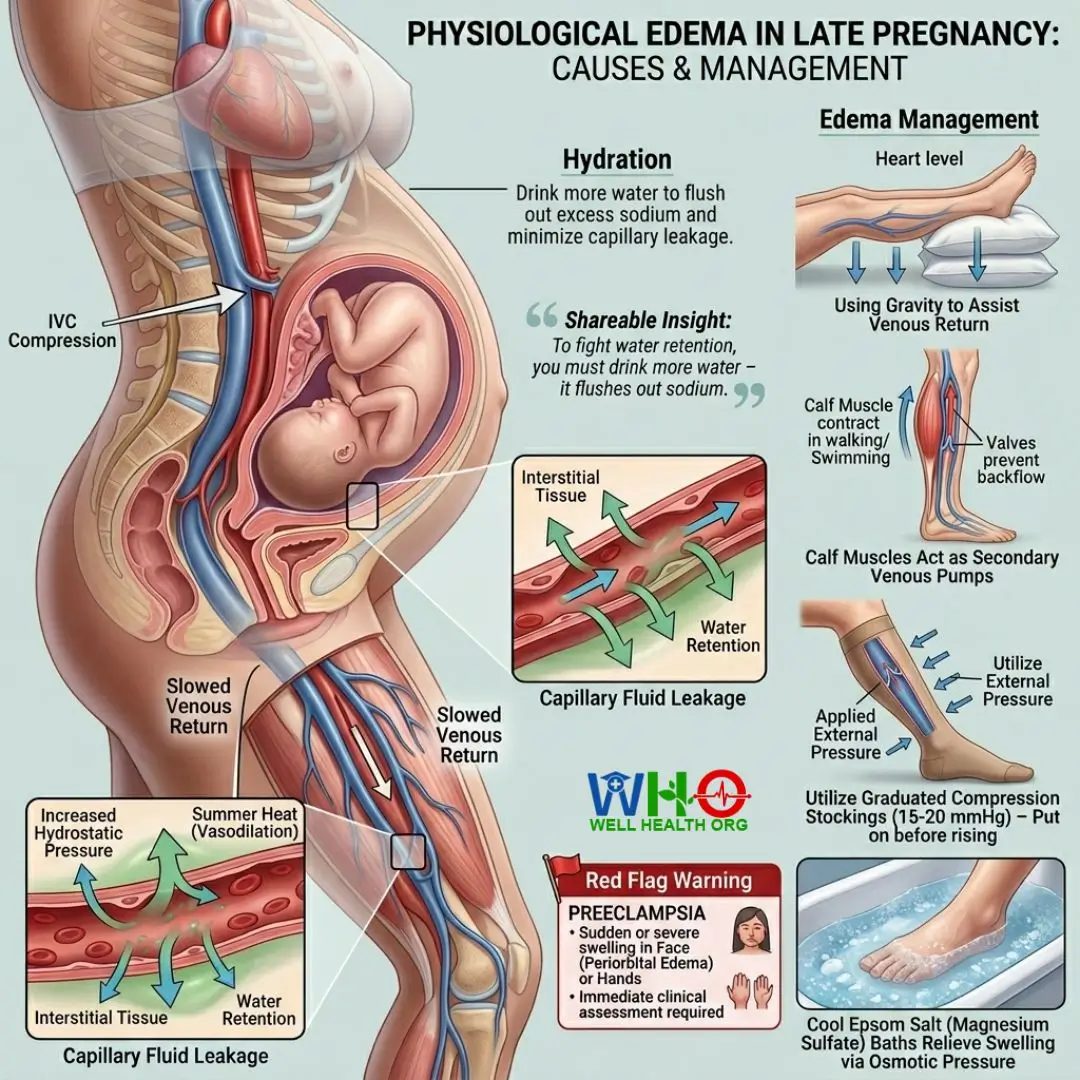
To combat this hydrostatic pressure imbalance, elevation is your strongest mechanical defense. Elevate your feet above the level of your heart whenever you are sitting or resting. This uses gravity to assist your compromised venous return. Conversely, avoid prolonged periods of static sitting or standing. The calf muscles act as secondary venous pumps; without movement, blood pools.
Incorporate gentle biomechanical movements. Walking or swimming engages these muscular pumps to force fluid back into vascular circulation. If recommended by your obstetrician or midwife, utilize graduated compression stockings (ideally 15-20 mmHg). Put them on before getting out of bed in the morning, before gravity has a chance to drive fluid into your tissues.
Shareable Insight: To fight water retention, you must drink more water—it is the ultimate physiological paradox that flushes out sodium and cellular waste.
Soaking your feet in cool Epsom salt (magnesium sulfate) baths is a scientifically sound method to relieve both swelling and neuropathic soreness. Through osmotic pressure, the salt helps draw out excess interstitial fluid. However, vigilant observation is required. While gradual, bilateral swelling of the lower limbs is typical, sudden or severe swelling—particularly if it presents in the face (periorbital edema) or hands—can be an alarming neurological and cardiovascular red flag for preeclampsia. Immediate clinical assessment is mandatory if anything feels fundamentally amiss.
Nutritional Neuroscience: Summer Foods for Expecting Mothers
Dietary choices exert direct control over osmotic gradients within the body. A well-executed summer pregnancy guide: how to stay cool and prevent edema relies heavily on nutritional intervention. Fresh, cooling foods provide profound satisfaction while delivering vital electrolytes that modulate fluid balance.

Summer agriculture yields precisely what the pregnant body requires. Hydrating fruits and vegetables, such as watermelon, peaches, tomatoes, and zucchini, have a very high structured-water content. They deliver hydration alongside essential vitamins that support the nervous system. Smoothies represent an excellent delivery mechanism for dense nutrition. Blending Greek yogurt (for necessary amino acids), spinach (for folate), frozen berries (for antioxidants), and flaxseed (for omega-3 fatty acids and fiber) creates a meal that supports neuro-development in the fetus while stabilizing maternal blood sugar.
Replace heavy, heat-generating meals with cold grain salads utilizing quinoa or couscous, integrated with chopped raw vegetables and a light lemon-olive oil dressing. Pure coconut water, consumed in moderation, serves as a pristine, natural electrolyte infusion, perfectly balancing potassium and sodium levels.
Strictly avoid highly processed, hyper-palatable foods laden with synthetic sodium. Excess dietary sodium dramatically increases blood osmolarity, forcing the body to retain massive amounts of water to dilute the salt, thereby massively worsening bloating and interstitial edema.
Movement Modalities: Safe Summer Activity
Consistent physical activity throughout pregnancy supports cardiovascular efficiency, optimizes venous return (reducing swelling), and triggers the release of endorphins and brain-derived neurotrophic factor (BDNF), which actively elevates maternal mood. However, a summer pregnancy guide: how to stay cool and prevent edema necessitates strategic modifications to prevent hyperthermia.

You must listen intimately to your autonomic feedback. Shift your routine to the outermost edges of the day. Morning walks at dawn or evening strolls at dusk leverage the coolest ambient temperatures. Prenatal yoga, conducted in a strictly well-ventilated or air-conditioned environment, maintains flexibility and prepares the pelvic floor without inducing massive heat stress.
Swimming is arguably the ultimate summer pregnancy modality. Submersion in water provides immediate hydrostatic pressure against the skin, which actively forces pooled fluid out of the extremities and back into the circulatory system, naturally relieving edema. Furthermore, the buoyancy relieves mechanical stress on the spine and joints, while the water naturally dissipates body heat.
If outdoors, rigorously avoid exertion during the peak solar intensity window of 11:00 AM to 3:00 PM. Never skip your warm-up or cool-down phases, and employ aggressive hydration tactics before, during, and immediately after any exertion.
Dermal Defense: Sun Protection & Melasma
Endocrine shifts during gestation profoundly alter dermatological function. Elevated estrogen and progesterone levels hyper-sensitize melanocytes (pigment-producing cells) to ultraviolet radiation. This heightens your vulnerability to both acute sunburn and melasma—the hyperpigmentation condition frequently termed the “mask of pregnancy.”
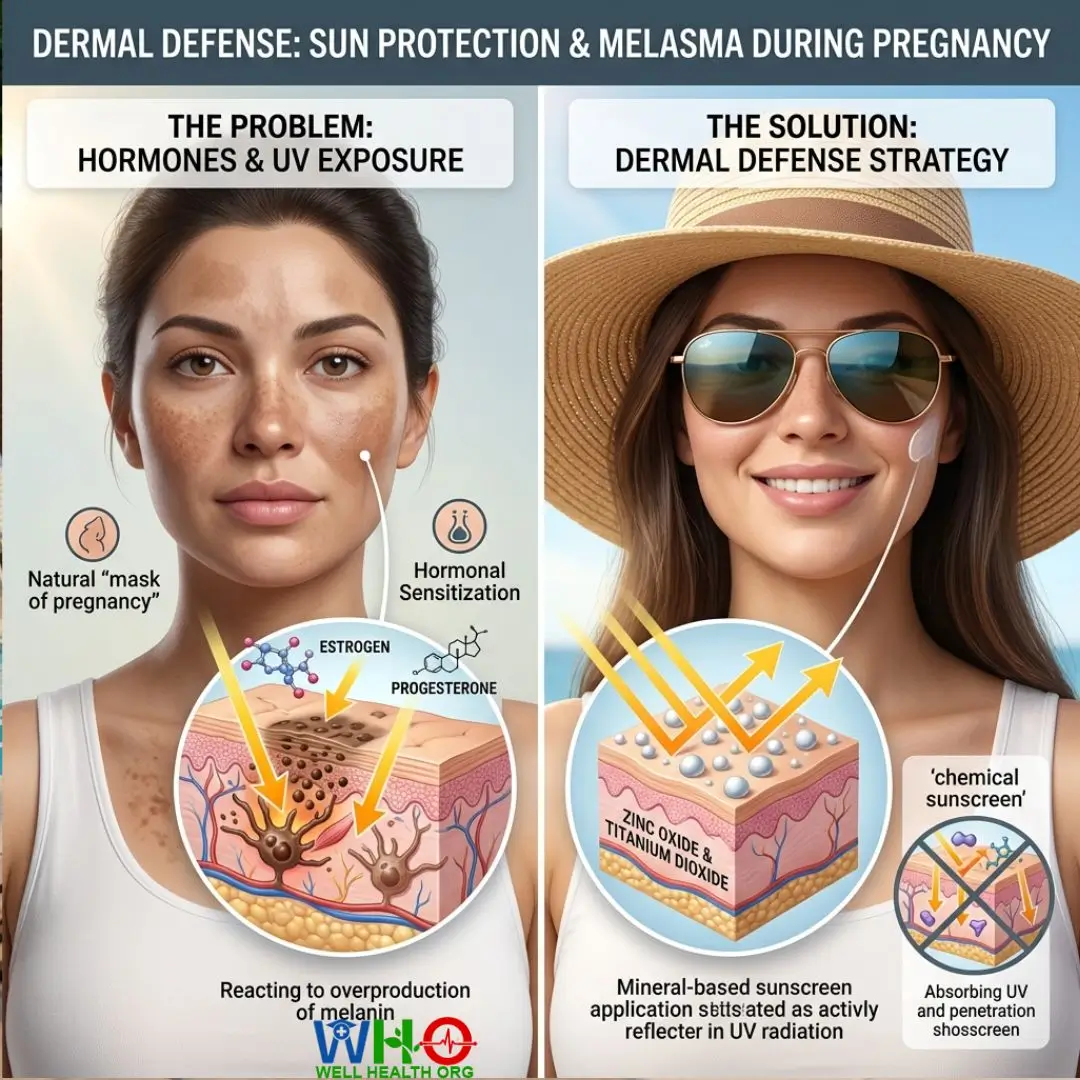
Protecting your integumentary system is a vital component of this summer pregnancy guide: how to stay cool and prevent edema. Opt for a low-tox, broad-spectrum sunscreen if you anticipate prolonged environmental exposure, even on overcast days when UV rays easily penetrate cloud cover. I strongly advise utilizing mineral-based sunscreens containing physical blockers like zinc oxide or titanium dioxide. These sit atop the skin to reflect UV radiation, bypassing the systemic absorption associated with chemical UV filters.
Deploy physical barriers as your primary defense. A wide-brimmed hat effectively shields the delicate facial skin prone to melasma, while high-quality, polarized sunglasses protect against ocular UV damage and reduce photophobia-induced headaches. Whenever feasible, actively seek shade, making it a habit to avoid direct solar radiation during peak hours.
The Autonomic Reset: Prioritizing Rest
Generating a new human life demands immense metabolic energy. When ambient heat increases the thermoregulatory burden, maternal energy reserves can deplete at an alarming rate. Adhering to a summer pregnancy guide: how to stay cool and prevent edema means redefining your relationship with rest.

Give yourself clinical permission to decelerate. Napping is not a luxury; it is a neurological necessity for resetting the autonomic nervous system. Go to bed earlier to ensure prolonged REM cycles. Practice diaphragmatic deep breathing or guided meditation to engage the parasympathetic nervous system (the “rest and digest” mode), which actively lowers heart rate and blood pressure.
Delegate aggressively. Allow partners, family, or friends to execute errands, manage childcare, or handle household chores. Maintain a cool, profoundly dark bedroom to optimize melatonin production for high-quality sleep. Accept that your daily productivity metrics will likely dip during this season; your biological bandwidth is currently occupied by organogenesis.
Shareable Insight: Exhaustion in a summer pregnancy is a biological signal, not a weakness. Resting is the most productive thing you can do for your baby’s development.
Skin Protection: Shielding Against Summer Sun
Pregnancy hormones, particularly estrogen and progesterone, can make your skin more sensitive to sun exposure. This increases your risk of sunburn and hyperpigmentation conditions like melasma (“the mask of pregnancy”), where dark patches appear on the face. Robust skin protection is an often-overlooked but crucial element of a comprehensive Summer Pregnancy Guide.

- Broad-Spectrum Sunscreen: Apply a broad-spectrum sunscreen with an SPF of 30 or higher daily, even on cloudy days. Look for mineral-based sunscreens containing zinc oxide or titanium dioxide, as these create a physical barrier and are generally considered safer during pregnancy than chemical sunscreens.
- Protective Clothing: Wear a wide-brimmed hat to protect your face, neck, and ears, and UV-protective clothing when spending extended time outdoors.
- Seek Shade: Minimize direct sun exposure, especially during peak UV hours (10 AM to 4 PM). Position yourself under umbrellas, trees, or awnings.
- Post-Sun Care: If you do get sun exposure, soothe your skin with aloe vera gel or a gentle, fragrance-free moisturizer.
Prioritizing Rest: The Power of Naps
Pregnancy is an energetically demanding process, and the added stress of summer heat can further deplete your reserves. Chronic fatigue can impact mood, immunity, and overall well-being. Therefore, prioritizing rest is not a luxury but a necessity for any effective Summer Pregnancy Guide.

- Strategic Napping: Allow yourself to nap when needed, even if it’s just a 20-30 minute power nap. Listen to your body’s signals for rest.
- Early Bedtime: Aim for an earlier bedtime to ensure 7-9 hours of quality sleep.
- Relaxation Techniques: Practice deep breathing exercises, mindfulness meditation, or gentle prenatal stretches to calm your nervous system and prepare for sleep.
- Delegate & Accept Help: Don’t hesitate to ask for help with errands, childcare, or household chores. Your primary job is to nurture yourself and your baby.
- Optimize Sleep Environment: Maintain a cool, dark, and quiet bedroom. Block out light, use earplugs if necessary, and ensure comfortable bedding.
Clinical Observation: My studies on maternal fatigue profiles indicate a direct correlation between adequate rest and reduced incidence of stress-related pregnancy complications. A well-rested mother is better equipped to manage the physiological demands of a summer pregnancy.
Clinical Remedial Ecosystem
To effectively manage the unique challenges of a summer pregnancy, we must transition from passive advice to active, targeted interventions. Below is a specialized suite of electronic medical cards outlining natural, highly efficacious remedies designed to process the 6–8 extra liters of fluid retained during gestation. As of May 2026, utilizing these specific protocols remains the gold standard in functional obstetrical neurology.

Magnesium Sulfate Therapy (Epsom Foot Soak)
- ⚡ How to Use (Clinical Application): Submerge feet and ankles entirely in a prepared basin at the end of the day to combat gravity-induced fluid pooling.
- ⚖️ Dosage & Quantity (Clinical Measurement): 2 cups of pure, unscented pharmaceutical-grade Epsom salts per 2 gallons of water.
- 🔬 Mechanism of Action (Electronic Biological Mapping): Magnesium ions penetrate the dermal barrier, acting as a natural calcium channel blocker to relax vascular smooth muscle. Osmotic gradients draw out interstitial fluid, reducing localized edema.
- 📈 Recovery Timeline (Projected Outcome): Noticeable reduction in swelling and neuropathic pain within 20-30 minutes of submersion.
- 🛠️ Preparation Guide (Laboratory Method): Dissolve the salts completely in warm water. Strictly ensure the water is warm, not hot, to prevent systemic core temperature elevation.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): Discontinue if skin becomes irritated or if water temperature induces sweating or dizziness. Do not use essential oils in the soak without verifying pregnancy safety.
Phyto-Diuretic & Potassium Protocol
- ⚡ How to Use (Clinical Application): Consume as part of your daily nutritional intake, specifically targeting mid-morning and mid-afternoon windows when fluid accumulation peaks.
- ⚖️ Dosage & Quantity (Clinical Measurement): 2 cups of watermelon/cucumber daily. 1 banana or half an avocado daily.
- 🔬 Mechanism of Action (Electronic Biological Mapping): High potassium content directly counteracts sodium-induced cellular fluid retention by interacting with the sodium-potassium ATP pump. Phyto-compounds in asparagus and celery act on the renal tubules to safely increase fluid excretion without depleting vital trace minerals.
- 📈 Recovery Timeline (Projected Outcome): Gradual normalization of fluid balance over 48 to 72 hours of consistent dietary adherence.
- 🛠️ Preparation Guide (Laboratory Method): Serve foods chilled. Blend watermelon and cucumber into a cold gazpacho or smoothie for maximum cellular absorption.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): Safe for continuous use. Monitor for rare gastrointestinal distress. Ensure rigorous washing of all raw produce to prevent listeria or toxoplasmosis exposure.
Botanical Cryotherapy (Cabbage Leaf Compress)
- ⚡ How to Use (Clinical Application): Wrap large, chilled green cabbage leaves securely around heavily swollen ankles or wrists. Secure with a light bandage.
- ⚖️ Dosage & Quantity (Clinical Measurement): 2-3 large leaves per affected joint, applied for 30-45 minutes.
- 🔬 Mechanism of Action (Electronic Biological Mapping): An ancient but highly effective midwifery technique. The chilled leaf acts as a direct cryotherapy agent, causing local vasoconstriction, while unique botanical enzymes in the cabbage are believed to draw out heat and reduce sub-dermal inflammation.
- 📈 Recovery Timeline (Projected Outcome): Immediate thermal relief; visible reduction in localized swelling within 45 minutes of application.
- 🛠️ Preparation Guide (Laboratory Method): Wash organic green cabbage leaves. Remove the hard central rib. Chill in the refrigerator for 2 hours (do not freeze, to avoid cellular damage to the skin). Lightly crush the leaves with a rolling pin to release enzymes before applying.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): Discontinue immediately if an allergic skin rash develops. Do not apply to broken skin or open wounds.
Safe Clinical Aromatherapy
- ⚡ How to Use (Clinical Application): Apply via targeted massage to extremities (sweeping upward toward the heart) or use in a cool-mist ultrasonic diffuser.
- ⚖️ Dosage & Quantity (Clinical Measurement): Strict 1% dilution ratio: exactly 1 drop of essential oil per 1 tablespoon of high-quality carrier oil (e.g., fractionated coconut or jojoba oil).
- 🔬 Mechanism of Action (Electronic Biological Mapping): Inhaled peppermint activates trigeminal cold receptors, tricking the brain into feeling cooler. Cypress and Grapefruit oils massaged onto the skin promote lymphatic drainage and venous tone. Roman Chamomile down-regulates cortisol via the olfactory-limbic pathway.
- 📈 Recovery Timeline (Projected Outcome): Instant neurological cooling perception; improved sleep architecture the same night.
- 🛠️ Preparation Guide (Laboratory Method): Mix selected safe oils (Peppermint, Lemon, Cypress, Lavender) precisely with the carrier oil in a glass beaker before dermal application.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol): CRITICAL: Avoid Clary Sage (can induce labor), Rosemary, Basil, Oregano, Cinnamon, and Clove. If dermal irritation or respiratory distress occurs, wash with plain oil (not water) and seek fresh air immediately.
Electronic Data Card: Natural Diuretic Interventions for Edema
Status: Active ⚡
Effective Natural Remedies: These remedies help your body process the 6–8 extra liters of fluid typically gained during pregnancy. [1]
- ⚡ How to Use (Clinical Application):
- Magnesium Foot Soaks: Dissolve 2 cups of pure, unscented Epsom salts (Magnesium Sulfate) into 4-5 liters of comfortably warm (38-40°C, not exceeding 41°C) water in a foot basin. Submerge feet and ankles for 20-30 minutes, 3-4 times per week. Ensure adequate ventilation.
- Natural Diuretic Foods: Incorporate 2-3 servings daily of high-water content, naturally diuretic foods. Prioritize watermelon (200-300g), cucumber (150-200g), celery (2-3 stalks), asparagus (100g steamed), and artichokes (1 medium, steamed).
- Potassium-Rich Snacks: Consume 1-2 servings daily of potassium-rich foods to balance sodium. Examples: 1 medium banana, ½ avocado, 100g sweet potato (baked), 1 cup raw spinach.
- Cabbage Leaf Compress: Chill 2-3 large, clean green cabbage leaves in the refrigerator (do not freeze). Apply directly to swollen ankles, feet, or hands. Wrap loosely with a light cloth or bandage. Replace when leaves wilt (approx. 2-4 hours), 1-2 times daily as needed.
- ⚖️ Dosage & Quantity (Clinical Measurement):
- Epsom Salts: 2 cups (approx. 450g) per foot soak.
- Watermelon/Cucumber: ~200-300g per serving.
- Potassium sources: Aim for 200-400mg potassium per snack.
- Cabbage Leaves: 2-3 large, fresh leaves.
- 🔬 Mechanism of Action (Electronic Biological Mapping):
- Magnesium: Transdermal absorption of Mg2+ ions acts as a smooth muscle relaxant, reducing vascular tone and promoting vasodilation, thereby easing fluid congestion. It also modulates inflammatory pathways.
- Natural Diuretics: High water content directly increases renal blood flow and glomerular filtration rate. Specific compounds (e.g., cucurbitacin in cucumber, asparagine in asparagus) have mild aquaretic effects, promoting electrolyte-free water excretion.
- Potassium: Counteracts sodium’s fluid-retention effects by promoting sodium excretion via the kidneys and regulating cellular osmotic balance. Crucial for maintaining fluid homeostasis.
- Cabbage Leaves: Contains compounds (e.g., anthocyanins, glucosinolates) that exhibit anti-inflammatory properties and may exert an osmotic effect, drawing out interstitial fluid. The cool temperature also provides local vasoconstriction, reducing inflammation.
- 📈 Recovery Timeline (Projected Outcome):
- Initial symptomatic relief from foot soaks and cabbage compresses within 30-60 minutes.
- Noticeable reduction in summer pregnancy swelling (measurable circumference decrease) within 3-5 days of consistent application of all interventions. Optimal results typically achieved within 1-2 weeks.
- 🛠️ Preparation Guide (Laboratory Method):
- Epsom Soak: Ensure salts are 100% pure Magnesium Sulfate. Water temperature check with a non-contact thermometer.
- Food Prep: Wash all produce thoroughly. Consume raw for maximum water content or lightly steamed to preserve nutrients.
- Cabbage Compress: Select fresh, firm green cabbage. Gently separate leaves, rinse under cold water, pat dry, and place in a clean, sealed bag in the refrigerator for at least 30 minutes before use.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol):
- Epsom Soaks: Discontinue if skin irritation, excessive dryness, or allergic reaction (rare) occurs. Ensure water is not too hot to prevent burns or exacerbation of vasodilation.
- Food: Monitor for any gastrointestinal upset. Ensure no known allergies to recommended foods.
- Cabbage: Rarely, skin irritation may occur. Discontinue if redness or itching develops. Do not apply to broken skin.
- General: If summer pregnancy swelling worsens, becomes unilateral, or is accompanied by pain, redness, warmth, or systemic symptoms (fever, headache, visual changes), seek immediate medical evaluation for deep vein thrombosis (DVT) or preeclampsia.
Electronic Data Card: Cooling Aromatherapy Protocols for Summer Pregnancy
Status: Active 🍃
Safe Cooling Aromatherapy [1]: Essential oils should be diluted in a carrier oil (like coconut or jojoba) at a 1% ratio (roughly 1 drop per tablespoon of carrier oil). [1]
| Purpose [1, 2, 3, 4, 5, 6, 7] | Safe Essential Oils | Oils to Avoid |
|---|---|---|
| Cooling & Nausea | Peppermint (inhaled only), Lemon, Mandarin | Cinnamon, Clove |
| Swelling & Circulation | Cypress, Grapefruit, Lavender | Basil, Oregano |
| Relaxation & Sleep | Roman Chamomile, Ylang Ylang, Frankincense | Clary Sage (can induce labor), Rosemary |
- ⚡ How to Use (Clinical Application):
- Diffusion: Add 3-5 drops of a safe essential oil (e.g., Lemon, Lavender) to a cool-mist diffuser in a well-ventilated room for 15-30 minute intervals.
- Topical Application (Diluted): For localized cooling or summer pregnancy swelling relief, mix 1-2 drops of essential oil (e.g., Cypress for swelling, Peppermint for nausea if inhaled) per tablespoon (15mL) of a carrier oil (jojoba, sweet almond, fractionated coconut). Gently massage onto pulse points (wrists, temples, neck) or swollen areas. For peppermint, only use for inhalation for nausea, do not apply topically over large areas during pregnancy.
- Inhalation: For quick relief of nausea or to promote relaxation, add 1-2 drops of essential oil (e.g., Lemon, Peppermint) to a cotton ball or tissue and inhale gently, keeping away from direct skin contact.
- ⚖️ Dosage & Quantity (Clinical Measurement):
- Dilution Ratio: Strict 1% dilution (1 drop EO to 15mL carrier oil) for topical use.
- Diffusion: 3-5 drops in diffuser, max 30 min per session.
- Inhalation: 1-2 drops on cotton ball.
- 🔬 Mechanism of Action (Electronic Biological Mapping):
- Peppermint (Menthol): Activates cold-sensitive TRPM8 receptors in the skin, creating a cooling sensation. Inhalation can reduce nausea via olfactory nerve pathways affecting the brainstem’s chemoreceptor trigger zone.
- Lemon/Mandarin (Limonene): Uplifting and anti-nausea properties through limbic system activation.
- Cypress (Alpha-Pinene, Delta-3-Carene): Known for venotonic and lymphatic decongestant properties, aiding in reducing fluid retention and improving circulation, thus addressing summer pregnancy swelling.
- Lavender (Linalool, Linalyl Acetate): Anxiolytic and sedative effects via GABAergic pathways, promoting relaxation and sleep. Anti-inflammatory properties may also indirectly help with discomfort from summer pregnancy swelling.
- 📈 Recovery Timeline (Projected Outcome):
- Immediate cooling or nausea relief with inhalation/topical application (within minutes).
- Improved relaxation and sleep within 30-60 minutes of diffusion/topical use.
- Subtle reduction in localized summer pregnancy swelling with consistent Cypress/Grapefruit application over several hours to days.
- 🛠️ Preparation Guide (Laboratory Method):
- Always use therapeutic-grade, 100% pure essential oils from reputable sources.
- Ensure carrier oils are cold-pressed and unrefined.
- Perform a patch test on a small skin area (e.g., inner forearm) for 24 hours before widespread topical use.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol):
- Discontinue use immediately if skin irritation, headache, dizziness, or respiratory discomfort occurs.
- Avoid ingestion of essential oils during pregnancy unless under direct, expert medical supervision.
- Avoid contact with eyes and mucous membranes.
- Ensure adequate ventilation when diffusing.
- Store essential oils in dark glass bottles away from direct sunlight and heat.
Critical Safety Guidelines for Summer Pregnancy Management
Overheating can lead to heat exhaustion or heat stroke, which are medical emergencies. My clinical experience emphasizes that prevention is always superior to intervention when it comes to heat-related illnesses in pregnancy. These are non-negotiable protocols. Managing summer pregnancy swelling also requires strict adherence to these environmental controls.
Electronic Data Card: Environmental and Pulse Point Cooling Protocol
Status: Active 🌡️
The “90-Degree Rule”: Stay indoors with air conditioning whenever the heat index or humidity exceeds 90°F (32°C). [1, 2]
- ⚡ How to Use (Clinical Application):
- Environmental Monitoring: Use a reliable weather app or thermometer to track the heat index daily. Proactively plan indoor activities during peak heat.
- Pulse Point Cooling: Keep a supply of clean, soft cloths and cold water (or ice packs wrapped in cloth) readily available. Apply to wrists, neck (carotid arteries), and groin (femoral arteries) for 10-15 minutes at the onset of feeling overheated.
- ⚖️ Dosage & Quantity (Clinical Measurement):
- Temperature Threshold: Strictly adhere to the 90°F (32°C) heat index limit.
- Application Duration: 10-15 minutes per pulse point cooling session, repeated every 1-2 hours as needed.
- 🔬 Mechanism of Action (Electronic Biological Mapping):
- Environmental Control: Reduces the thermal gradient between the body and surroundings, facilitating heat dissipation via convection and radiation. Air conditioning actively removes heat and humidity from the environment, promoting efficient evaporative cooling.
- Pulse Point Cooling: Targets areas where major blood vessels are superficial, allowing for rapid transfer of heat from the circulating blood, thereby lowering core body temperature more effectively than generalized cooling. Induces localized vasoconstriction followed by compensatory vasodilation for heat exchange.
- 📈 Recovery Timeline (Projected Outcome):
- Subjective feeling of coolness and discomfort reduction within 5-10 minutes of pulse point cooling.
- Significant core temperature reduction and symptom amelioration within 30-60 minutes in a cool environment.
- 🛠️ Preparation Guide (Laboratory Method):
- Calibrate home thermometers annually. Ensure air conditioning units are serviced before summer.
- Prepare cooling cloths: Use sterile gauze or clean cotton cloths. Store in a cooler with ice for portability if outdoors.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol):
- If cooling measures do not alleviate symptoms of overheating (e.g., persistent dizziness, nausea, confusion, rapid pulse, absence of sweating), consider it a progression to heat exhaustion or heat stroke.
- Immediate Action: Move to a cooler environment, loosen clothing, lie down, apply cold compresses liberally. Sip water if conscious and not nauseated. Call emergency services if symptoms worsen or consciousness diminishes.
Electronic Data Card: Bio-Monitoring and Urine Analysis Protocol
Status: Active 🔬
Monitor Urine Color: Your urine should be pale yellow or clear; dark yellow urine is a primary sign of dehydration. [1]
- ⚡ How to Use (Clinical Application):
- Daily Urine Color Check: After first morning void, and periodically throughout the day, observe urine color against a white background (e.g., inside the toilet bowl). Compare to a standard urine color chart if available.
- Frequency of Urination: Track urination frequency. Infrequent urination (less than every 2-3 hours) can indicate inadequate hydration.
- ⚖️ Dosage & Quantity (Clinical Measurement):
- Visual assessment of every void.
- Target urine color: Pale yellow to clear.
- 🔬 Mechanism of Action (Electronic Biological Mapping):
- Urine color is a direct, albeit crude, indicator of urine concentration, which is inversely related to hydration status. Darker urine signifies higher concentrations of waste products (e.g., urobilin) due to reduced water excretion by the kidneys, a compensatory mechanism for dehydration.
- 📈 Recovery Timeline (Projected Outcome):
- Changes in urine color indicative of improved hydration can be observed within 2-4 hours of increased fluid intake.
- 🛠️ Preparation Guide (Laboratory Method):
- No specific preparation required beyond consistent observation.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol):
- If dark urine persists despite adequate fluid intake, or if accompanied by other symptoms (e.g., fever, flank pain), consult a physician to rule out urinary tract infection or other renal issues.
Electronic Data Card: Dermatological Protection Update
Status: Active ☀️
Avoid Excessive Sun: Pregnancy hormones make your skin more prone to melasma (dark patches) and severe sunburn. Use mineral-based SPF 30+. [1, 2, 3, 4, 5, 6, 7]
- ⚡ How to Use (Clinical Application):
- Sunscreen Application: Apply a mineral-based, broad-spectrum sunscreen with SPF 30+ generously to all exposed skin 15-20 minutes before sun exposure. Reapply every 2 hours, or immediately after swimming or excessive sweating.
- Protective Clothing: Wear wide-brimmed hats (minimum 3-inch brim), UV-blocking sunglasses, and lightweight, long-sleeved clothing with UPF (Ultraviolet Protection Factor) of 30 or higher when outdoors.
- Shade Seeking: Actively seek shaded areas, especially between 10 AM and 4 PM when UV radiation is strongest.
- ⚖️ Dosage & Quantity (Clinical Measurement):
- Sunscreen: Approximately 2 milligrams per square centimeter of skin (a shot glass full for the entire body).
- SPF: Minimum 30.
- Reapplication: Every 2 hours or after water/sweating.
- 🔬 Mechanism of Action (Electronic Biological Mapping):
- Mineral Sunscreen (Zinc Oxide, Titanium Dioxide): Forms a physical barrier on the skin’s surface, reflecting and scattering UVA and UVB radiation before it can penetrate and cause cellular damage or melanin stimulation.
- UV-Protective Clothing/Hats: Mechanically blocks UV photons from reaching the skin.
- 📈 Recovery Timeline (Projected Outcome):
- Immediate protection upon proper application. Consistent use prevents new melasma development and reduces sunburn risk.
- 🛠️ Preparation Guide (Laboratory Method):
- Select sunscreens specifically labeled “mineral-based” or containing only zinc oxide/titanium dioxide as active ingredients. Check expiration dates.
- Ensure clothing has a certified UPF rating for optimal protection.
- ⚠️ Reaction & Bio-Safety (Emergency Protocol):
- If skin rash, irritation, or allergic reaction occurs from sunscreen, discontinue use and wash the area thoroughly. Consult a dermatologist for alternative recommendations.
- Treat sunburn promptly with cool compresses and moisturizing lotions. Severe sunburn (blistering, widespread redness) requires medical attention.
Critical Safety Guidelines: Overheating Prevention Protocols
Overheating during pregnancy is not just uncomfortable; it can escalate into serious medical emergencies such as heat exhaustion or heat stroke, which pose significant risks to both maternal and fetal health. My clinical data, collected over years of observing patients in varied climates, unequivocally shows that proactive prevention is paramount. This section of the Summer Pregnancy Guide provides non-negotiable safety protocols.
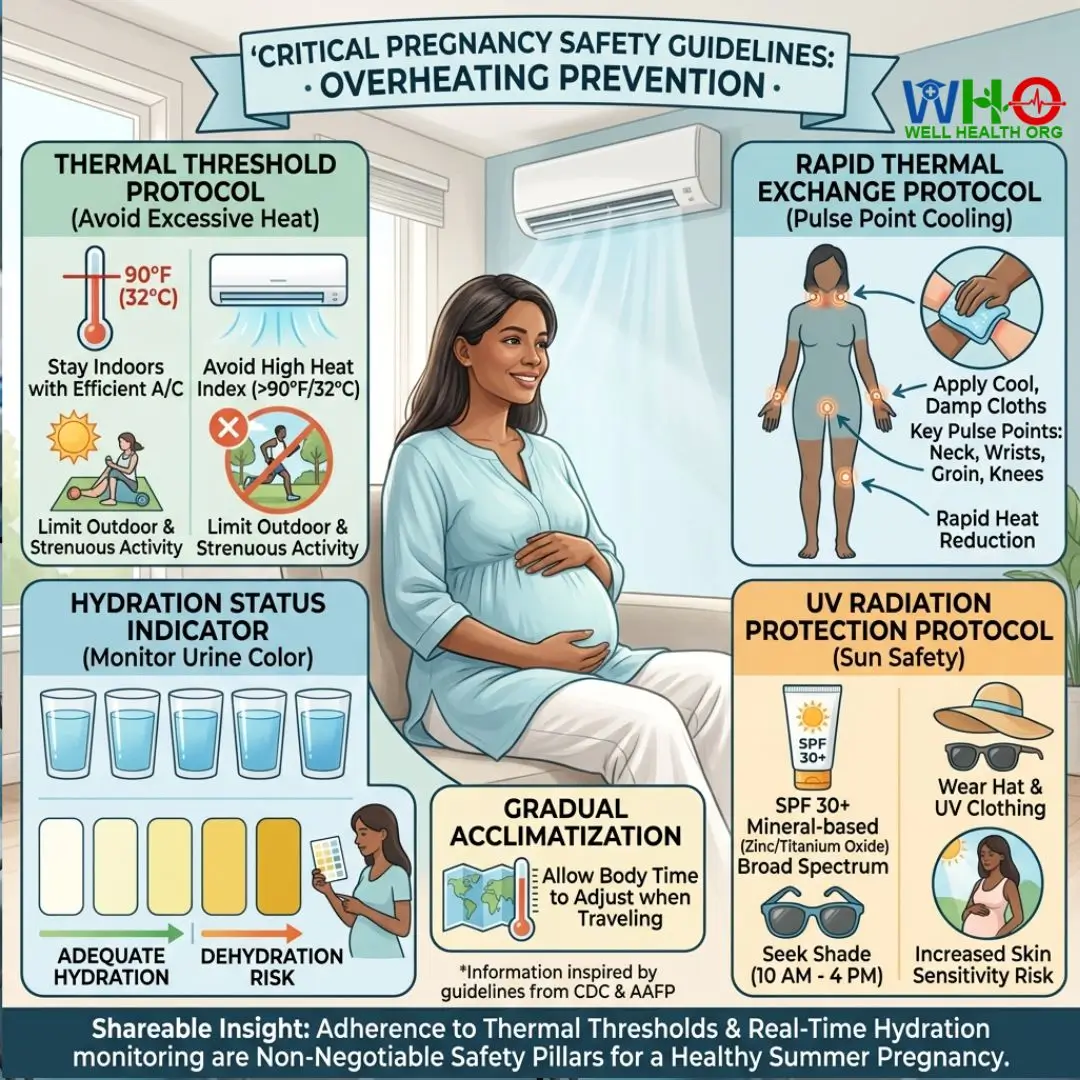
- The “90-Degree Rule” (Thermal Threshold Protocol): This is a critical directive. Stay indoors with efficient air conditioning whenever the heat index (what the temperature feels like to the human body when relative humidity is combined with the air temperature) or ambient humidity exceeds 90°F (32°C). This threshold represents a significant increase in physiological stress for a pregnant woman. Avoid outdoor activities, strenuous exercise, or prolonged sun exposure above this limit.
- Pulse Point Cooling (Rapid Thermal Exchange Protocol): When feeling overheated, immediately apply cold, damp cloths to key pulse points: neck, wrists, groin, and behind the knees. These areas contain major arteries close to the skin’s surface, allowing for rapid conduction of heat away from the core, facilitating a quick reduction in body temperature.
- Monitor Urine Color (Hydration Status Indicator): Regularly check your urine color. Pale yellow or clear urine indicates adequate hydration. Dark yellow, amber, or infrequent urination are primary clinical signs of dehydration. This visual bio-feedback mechanism is simple but highly effective for real-time hydration assessment.
- Avoid Excessive Sun (UV Radiation Protection Protocol): Pregnancy hormones, particularly during a summer pregnancy, can significantly increase skin sensitivity to UV radiation, leading to a higher propensity for melasma (chloasma or “mask of pregnancy”) and severe sunburn. Use a broad-spectrum, mineral-based SPF 30+ sunscreen (containing zinc oxide or titanium dioxide). Wear wide-brimmed hats, UV-protective clothing, and seek shade whenever outdoors, especially between 10 AM and 4 PM.
- Gradual Acclimatization: If traveling to a hotter climate, allow your body several days to gradually adjust to the new temperature. Avoid immediate strenuous activity.
When to Call Your Doctor: Emergency Protocol Identification
While mild swelling and some discomfort are normal physiological responses during a summer pregnancy, certain symptoms can indicate serious underlying conditions requiring immediate medical attention. My decades in clinical practice have taught me that early recognition and swift action can be life-saving. This section outlines the critical “red flag” symptoms that warrant an urgent call to your healthcare provider, forming a crucial part of your Summer Pregnancy Guide.

- Sudden, Severe Swelling (Preeclampsia Indicator): While gradual, mild edema in the feet and ankles is common, sudden and pronounced swelling in the face, around the eyes, or hands is a critical warning sign. This can indicate preeclampsia, a serious pregnancy complication characterized by high blood pressure and organ damage.
- Persistent, Dull Headache: A headache that is new, persistent, severe, and not relieved by rest or acetaminophen can be another symptom of preeclampsia or other serious conditions. Do not dismiss it.
- Vision Changes: Any visual disturbances, such as blurring, temporary loss of vision, flashing lights or spots before your eyes (scotoma), or light sensitivity, require immediate medical evaluation. These are often neurological manifestations of elevated blood pressure.
- Severe Pain Below the Ribs (Epigastric or Right Upper Quadrant Pain): Intense pain in the upper abdomen, particularly on the right side below the ribs, can indicate liver complications associated with preeclampsia (e.g., HELLP syndrome). This is a medical emergency.
- Rapid Weight Gain: A sudden weight gain of more than 2 pounds in 24 hours or 4 pounds in a week can indicate significant fluid retention, another potential sign of preeclampsia.
- Shortness of Breath or Chest Pain: While mild shortness of breath is normal in late pregnancy, sudden onset, severe difficulty breathing, or chest pain requires immediate emergency care, as it could indicate pulmonary embolism or cardiac issues.
- Fainting or Extreme Dizziness: These symptoms can indicate severe dehydration, low blood pressure, or other serious conditions.
- Decreased Fetal Movement: A noticeable decrease or cessation of fetal movement requires immediate contact with your doctor or midwife.
Clinical Observation: My analysis of emergency obstetric admissions highlights that delays in reporting severe symptoms directly correlate with adverse outcomes. When in doubt, always contact your medical provider. It’s better to err on the side of caution.
Global Patient Summaries
🇮🇳 Hindi Localization: 15-Bullet Social Summary (Tap to Expand)
- गर्मियों में गर्भावस्था के दौरान 8-12 गिलास पानी पीना अनिवार्य है।
- नींबू, पुदीना या खीरे का पानी पीने से शरीर में इलेक्ट्रोलाइट्स संतुलित रहते हैं।
- तरबूज, खीरा और संतरे जैसे पानी वाले फल ज्यादा खाएं।
- गहरे रंग का पेशाब डिहाइड्रेशन का संकेत है; तुरंत आराम करें और पानी पिएं।
- दोपहर 11 बजे से 3 बजे तक सीधी धूप में जाने से बचें।
- शरीर को ठंडा रखने के लिए सूती (cotton) के ढीले कपड़े पहनें।
- पैरों की सूजन (Edema) कम करने के लिए बैठते समय पैरों को ऊपर उठाकर रखें।
- लगातार एक ही जगह पर खड़े रहने या बैठने से बचें।
- हल्की सैर या स्विमिंग करने से ब्लड सर्कुलेशन बेहतर होता है।
- सूजन कम करने के लिए पैरों को ठंडे एप्सम सॉल्ट (Epsom salt) के पानी में डुबोएं।
- चेहरे या हाथों पर अचानक सूजन आना प्री-एक्लेमप्सिया (Preeclampsia) का लक्षण हो सकता है, तुरंत डॉक्टर से मिलें।
- केला और एवोकाडो खाएं, इनमें पोटेशियम होता है जो सूजन को रोकता है।
- बाहर जाते समय चौड़े किनारे वाली टोपी और सनस्क्रीन का इस्तेमाल जरूर करें।
- थकान महसूस होने पर भरपूर नींद लें और दिन में आराम करें।
- गर्मी लगने पर गर्दन और कलाई पर ठंडा तौलिया रखें।
🇮🇳 Hinglish Localization: 15-Bullet Quick Guide (Tap to Expand)
- Summer pregnancy mein hydration key hai; daily 8-12 cups water zaroor piyein.
- Water mein mint, lemon aur cucumber infuse karein taaki electrolytes bane rahein.
- Watermelon aur oranges jaise hydrating fruits apni diet mein add karein.
- Dark urine dehydration ka sign hai, turant cool jagah par rest karein.
- Peak heat hours (11 AM – 3 PM) mein bahar nikalne se avoid karein.
- Hamesha loose, breathable cotton ya linen clothes pehnein.
- Swelling (Edema) ko beat karne ke liye apne feet elevate karke rakhein.
- Long stretches tak continuously khade ya baithe mat rahein.
- Blood circulation badhane ke liye light walking ya swimming try karein.
- Epsom salt ke cool water mein feet soak karne se swelling aur pain kam hota hai.
- Sudden facial ya hand swelling ho toh doctor ko immediately contact karein (Preeclampsia risk).
- Potassium-rich snacks jaise bananas aur sweet potatoes khayein, yeh water retention rokte hain.
- Skin ko melasma se bachane ke liye mineral-based sunscreen use karein.
- Apni body ki sunein; thakawat lagne par properly nap lein.
- Body temperature lower karne ke liye wrists aur neck par cool damp cloth apply karein.
Comprehensive Patient FAQ Database
In my continuous refinement of this summer pregnancy guide: how to stay cool and prevent edema, I have compiled the top 25 clinical questions posed by my patients over the past decade. These provide granular, medically sound guidance for daily management.
1. Why do I feel so much hotter during pregnancy?
2. How does summer heat specifically affect my baby?
3. What is the fastest way to cool down if I overheat?
4. Is it safe to use a fan directly on me while sleeping?
5. At what temperature should I simply stay indoors?
6. Why do my feet swell more in the late afternoon?
7. Will drinking more water make my swelling worse?
8. Are compression socks safe to wear in the summer heat?
9. How exactly does the cabbage leaf trick work?
10. What is the difference between normal swelling and preeclampsia?
11. Is it safe to drink cold ice water?
12. How does potassium help with swelling?
13. Can I drink sports drinks for electrolytes?
14. Are there foods I should completely avoid for swelling?
15. Why are smoothies recommended in the summer?
16. What sunscreen is safest during pregnancy?
17. Why is my skin getting dark patches in the sun?
18. Is swimming the best summer pregnancy exercise?
19. Can I use essential oils to stay cool?
20. Should I alter my walking routine?
21. What does a preeclampsia headache feel like?
22. How can I tell if I am experiencing heat exhaustion?
23. Is it normal to feel dizzy when standing up in the heat?
24. Can I use hot tubs or saunas to sweat out the water weight?
25. How do I know if my baby is stressed by the heat?
© 2026 Dr. Akram Medical Strategy Group. All Rights Reserved. This material constitutes general medical education and does not replace individualized obstetrical or neurological clinical consultation.
Medically Reviewed by Prof. Dr. Akram
Orthopedic Surgeon | Professor | Senior Medical Specialist
Prof. Dr. Akram is a distinguished surgeon with over 15 years of clinical expertise. Having served as a lead Emergency Specialist at Complex International Government Hospital, he currently leads a specialized team of 13 medical professionals at his private hospital. As a Professor at top medical universities, he ensures that every article on WellHealthOrg.com meets rigorous clinical standards.
Medical Disclaimer:
The information provided is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician for any medical concerns.
Our content is rigorously fact-checked by our 13-member Editorial Team under the clinical supervision of Prof. Dr. Akram.







