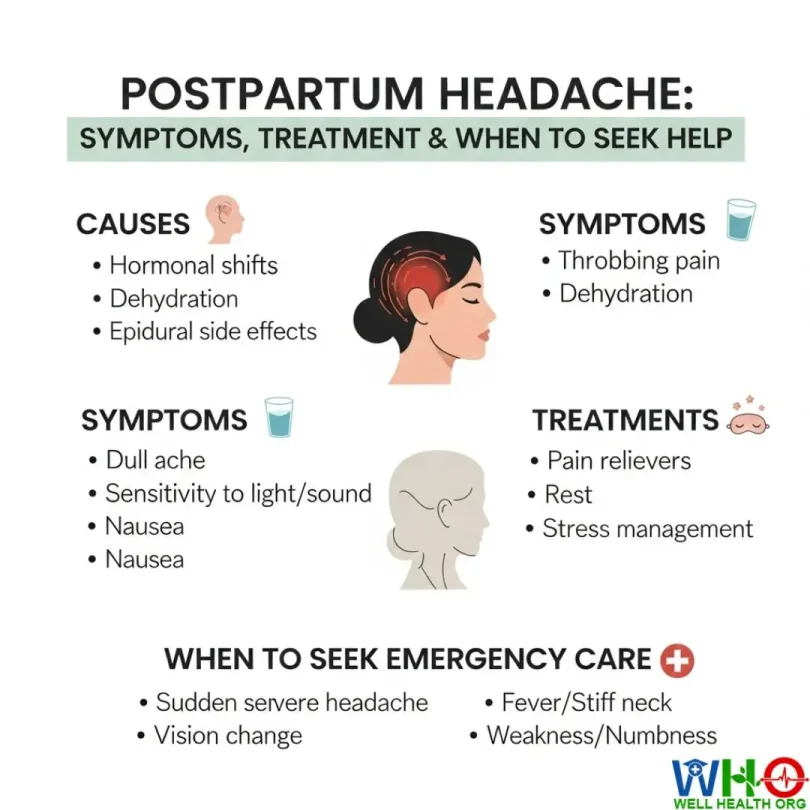
Bringing a child into the world is a life-changing milestone filled with joy, challenges, and profound adjustments. While many new mothers expect sleepless nights and physical recovery, fewer anticipate the discomfort of postpartum headaches. Yet, studies suggest that nearly 40% of women experience headaches after childbirth, ranging from mild tension headaches to severe, potentially life-threatening conditions.
- Understanding Postpartum Headache Symptoms
- Common Headache Symptoms After Childbirth
- Warning Signs That Require Immediate Medical Attention
- Causes and Risk Factors for Postpartum Headaches
- Primary Headache Disorders
- Hormonal Fluctuations
- Post-Dural Puncture Headaches
- Life-Threatening Causes
- When to Contact Your Healthcare Provider
- Routine Medical Consultation
- Emergency Medical Care
- Treatment Options for Postpartum Headaches
- Medication Management
- Managing Post-Dural Puncture Headaches
- Emergency Treatments
- Preventive Measures and Lifestyle Adjustments
- Sleep Optimization
- Nutritional Support
- Stress Management
- Gradual Return to Physical Activity
- Creating Your Recovery Plan
- Identifying Your Risk Factors
- Developing a Care Routine
- Long-Term Health Considerations
- The Importance of Early Medical Intervention
- Why Early Help Matters
- Overcoming Barriers to Care
- The Fourth Trimester: Why It Deserves Equal Attention
- A Period of Intense Change
- Holistic Care Approach
- Emotional Impact of Postpartum Headaches
- Link to Postpartum Depression
- Breaking the Stigma
- Practical Tips for Managing Postpartum Headaches at Home
- Hydration and Nutrition Hacks
- Relaxation and Pain Relief Methods
- Environmental Adjustments
- Partner and Family Support in Postpartum Recovery
- Ways Partners Can Help
- Role of Extended Family and Friends
- Long-Term Outlook for Postpartum Headaches
- Short-Term Outlook
- When Headaches Persist
- Positive Recovery Outcomes
- Frequently Overlooked Triggers of Postpartum Headaches
- Hormonal Birth Control
- Breastfeeding Posture
- Caffeine Dependence
- Emotional Exhaustion
- Empowering Mothers Through Education and Awareness
- Shifting the Narrative
- Healthcare Providers’ Role
- Mothers Supporting Mothers
These headaches can strike unexpectedly, sometimes interfering with a mother’s ability to bond with her baby, care for herself, or manage daily responsibilities. Because the postpartum period is already overwhelming—physically, mentally, and emotionally—understanding the causes, warning signs, and treatment options for postpartum headaches is essential.
This comprehensive guide explores everything new mothers and their families need to know: the common symptoms, when to seek urgent medical care, risk factors, management strategies, and preventive measures. By the end, you’ll feel more confident navigating postpartum headaches and advocating for your health during this important stage of recovery.
Understanding Postpartum Headache Symptoms
Not all headaches are the same, and in the postpartum period, they can vary widely in severity, duration, and triggers. Some headaches are mild annoyances, while others may signal an urgent medical issue. Being able to recognize the differences early helps ensure appropriate treatment and prevents dangerous complications.
Common Headache Symptoms After Childbirth
Most women who report postpartum headaches describe symptoms that resemble tension headaches or migraines. These headaches typically present with:
- Throbbing or pulsating pain that worsens with activity such as bending, lifting, or walking.
- Nausea and vomiting, which can further interfere with hydration and nutrition—two things already compromised in new mothers.
- Sensitivity to light (photophobia), making it difficult to stay in bright rooms or go outside during the day.
- Sensitivity to sound (phonophobia), where even routine noises like a crying baby, a running dishwasher, or a ringing phone feel unbearable.
- Visual disturbances or aura, such as flashing lights, zigzag patterns, or temporary blind spots.
For some mothers, these headaches mirror the migraines or tension headaches they may have experienced before pregnancy, but postpartum hormonal changes, sleep deprivation, and stress can make them worse or more frequent.
Warning Signs That Require Immediate Medical Attention
While mild headaches are common, certain symptoms can point to serious, potentially life-threatening conditions. It’s vital to call your doctor or emergency services immediately if headaches are accompanied by:
- A sudden, severe headache often described as “the worst headache of my life.”
- Fever, chills, or neck stiffness, which may suggest infection such as meningitis.
- Confusion, difficulty speaking, or memory problems.
- Seizures or convulsions, even if they last only a few seconds.
- High blood pressure readings, especially combined with vision changes.
- Weakness, numbness, or tingling in one side of the body.
- Severe headaches that wake you from sleep or worsen with coughing, sneezing, or exertion.
Additional red flags include swelling in the legs, decreased urination, blurred vision, or overactive reflexes. These may signal preeclampsia—a dangerous condition that can occur even after childbirth.
Recognizing these symptoms quickly can be life-saving. Always trust your instincts—if something feels wrong, don’t wait.
Causes and Risk Factors for Postpartum Headaches
Understanding why postpartum headaches happen is key to prevention and effective treatment. While some headaches are related to lifestyle changes, others are tied to serious medical conditions.
Primary Headache Disorders
For many women, postpartum headaches are a continuation—or worsening—of pre-existing conditions like:
- Migraines: Characterized by pulsating pain, nausea, and sensitivity to light or sound.
- Tension headaches: A band-like pressure around the head, often linked to stress and poor posture.
- Cluster headaches: Severe pain around one eye, though less common in postpartum women.
The postpartum period creates a “perfect storm” for these headaches due to:
- Sleep deprivation from nighttime feedings and baby care.
- Dehydration, especially for breastfeeding mothers who need extra fluids.
- Nutritional deficiencies, since many mothers skip meals or eat irregularly.
- Stress and anxiety related to adjusting to motherhood.
Hormonal Fluctuations
Hormonal changes after delivery play a huge role in headache development. Key shifts include:
- Estrogen crash: Estrogen levels drop rapidly after birth, which can trigger migraines.
- Serotonin imbalance: Affects both mood and pain perception, making mothers more sensitive to pain.
- Oxytocin fluctuations: Linked to breastfeeding and bonding but can also impact vascular changes in the brain.
Because hormones remain in flux for weeks—or longer if breastfeeding—headaches may persist during the “fourth trimester.”
Post-Dural Puncture Headaches
Women who receive epidural anesthesia or spinal anesthesia during labor face an additional risk. If the needle punctures the dura mater (the protective layer around the spinal cord), cerebrospinal fluid may leak, causing what’s called a post-dural puncture headache (PDPH).
These headaches typically:
- Worsen when sitting or standing but improve when lying flat.
- Are often accompanied by neck stiffness or shoulder pain.
- Usually develop within 24–48 hours after delivery.
Up to 50% of women with a puncture experience PDPH, making it one of the most common postpartum complications linked to epidurals.
Life-Threatening Causes
Though less frequent, certain postpartum headaches stem from serious medical emergencies, including:
- Preeclampsia or eclampsia: High blood pressure and organ stress.
- Stroke: Blood clots or bleeding in the brain.
- Cerebral venous sinus thrombosis (CVST): Clotting in brain veins.
- Meningitis: Infection of the brain or spinal cord lining.
- Reversible cerebral vasoconstriction syndrome (RCVS): Sudden narrowing of brain blood vessels.
These conditions require urgent hospital care. Delaying treatment can have severe consequences.
When to Contact Your Healthcare Provider
Not every postpartum headache needs urgent care, but it’s important to know when to reach out for help.
Routine Medical Consultation
Schedule a doctor’s appointment if your headaches:
- Occur frequently or persistently, despite rest and hydration.
- Interfere with daily life, including caring for your baby.
- Prevent you from bonding or feeding your newborn.
- Cause emotional distress, anxiety, or postpartum depression symptoms.
Sometimes, even if the headache itself isn’t dangerous, the toll it takes on your well-being and recovery justifies medical attention.
Emergency Medical Care
Go to the ER or call emergency services if you notice:
- Sudden vision loss or double vision.
- Slurred speech or difficulty understanding language.
- Seizures or fainting spells.
- Severe hypertension readings at home.
- Uncontrollable vomiting or inability to keep fluids down.
The rule of thumb: if the headache feels different, worse, or alarming, seek help right away.
Treatment Options for Postpartum Headaches
Treatment depends on the underlying cause, the severity of symptoms, and whether you’re breastfeeding. Doctors carefully consider medications that are safe for both mother and baby.
Medication Management
For most primary headaches, treatment may include:
- Ibuprofen (NSAIDs): Safe for breastfeeding in standard doses and effective against inflammation.
- Acetaminophen (paracetamol): A gentler option for pain relief without anti-inflammatory properties.
- Prescription migraine medications: Such as triptans, prescribed cautiously to avoid passing into breast milk.
Doctors may also suggest caffeine (in small amounts), which constricts blood vessels and eases pain.
Managing Post-Dural Puncture Headaches
Initial treatment is often conservative:
- Lying flat in bed, which reduces pain caused by spinal fluid leakage.
- Hydration, including IV fluids if necessary.
- Caffeine intake, sometimes administered intravenously.
- Pain medications tailored for breastfeeding mothers.
If symptoms last longer than 48 hours, doctors may recommend an epidural blood patch. This procedure involves injecting your own blood into the epidural space, which seals the leak and often provides rapid relief.
Emergency Treatments
Life-threatening headaches are treated aggressively, such as:
- Preeclampsia/eclampsia: Managed with magnesium sulfate and antihypertensives.
- Stroke or blood clots: May require blood thinners, clot-busting drugs, or surgery.
- Meningitis: Treated with urgent IV antibiotics.
In these cases, time is critical—early intervention saves lives.
Preventive Measures and Lifestyle Adjustments
While not every postpartum headache can be prevented, adopting healthy habits and making small changes in your daily routine can significantly reduce their frequency and severity. The postpartum period is already demanding, but a proactive approach to self-care pays off in better recovery, more energy, and fewer health setbacks.
Sleep Optimization
Getting adequate rest may sound impossible with a newborn, but quality sleep is one of the most powerful tools in reducing headaches. Here are practical strategies:
- Sleep when the baby sleeps instead of using that time to catch up on chores. The dishes can wait—your health cannot.
- Share nighttime duties with a partner, family member, or even a trusted friend. Rotating shifts helps ensure both parents get rest.
- Create a sleep-friendly environment by using blackout curtains, eye masks, and white noise machines to block distractions.
- Take short naps during the day. Even 20–30 minutes of rest can refresh your body and reduce headache triggers.
- Avoid screen time before bed. Blue light from phones and TVs interferes with melatonin production, making it harder to fall asleep.
While perfect sleep schedules may not be possible, prioritizing rest whenever you can helps regulate hormones, reduce stress, and stabilize blood pressure—all factors tied to postpartum headaches.
Nutritional Support
Food is more than fuel—it’s a foundation for healing. Unfortunately, many new mothers forget to eat balanced meals or rely on quick snacks due to busy schedules. Skipping meals, however, can trigger headaches by lowering blood sugar levels.
Practical tips include:
- Meal prep in advance during pregnancy or with the help of family. Freezer-friendly meals save time and ensure nourishment.
- Choose nutrient-dense foods like whole grains, lean proteins, leafy greens, and healthy fats. These stabilize energy and reduce inflammation.
- Snack smartly with nuts, yogurt, fruit, or hummus instead of processed junk foods.
- Stay hydrated by keeping water bottles around the house—near the couch, crib, and bedroom. Aim for at least 8–10 glasses of water per day, more if breastfeeding.
- Consider supplements if recommended by your doctor. Iron, magnesium, and B vitamins can reduce headache risk in postpartum women.
Think of nutrition as building blocks for your body’s recovery. Eating well not only prevents headaches but also supports milk production, energy levels, and emotional balance.
Stress Management
Motherhood is rewarding, but it can also be overwhelming. Stress often manifests physically—tight muscles, poor sleep, and yes, headaches. Finding simple stress-relief practices helps both your mind and your body.
- Mindful breathing exercises: Even five minutes of deep breathing can calm your nervous system.
- Gentle meditation or yoga: Focused movement helps ease tension and restore energy.
- New parent support groups: Sharing experiences with others reduces feelings of isolation.
- Journaling or gratitude lists: Writing helps process emotions and shifts focus toward positivity.
- Asking for help: Whether it’s a babysitter, a family member, or a neighbor, never hesitate to ask for support when needed.
By reducing stress, you lower cortisol levels (the stress hormone), which decreases the likelihood of tension headaches and improves overall well-being.
Gradual Return to Physical Activity
Physical activity supports circulation, hormone balance, and mood regulation—all of which can reduce headaches. However, jumping back into exercise too soon after childbirth may strain the body.
Here’s how to return safely:
- Start small with gentle walks, especially outdoors for fresh air and vitamin D.
- Incorporate stretching to release neck and shoulder tension that often contributes to headaches.
- Avoid sudden, high-intensity workouts unless cleared by your doctor.
- Listen to your body: Fatigue, dizziness, or pain are signals to slow down.
- Strengthen gradually with pelvic floor and core exercises recommended for postpartum recovery.
Think of it like rebuilding your strength brick by brick—slow, steady progress ensures long-term wellness without overexertion.
Creating Your Recovery Plan
Recovery after childbirth isn’t linear, and no two women experience it the same way. A personalized recovery plan that addresses both physical and emotional health can make a big difference in preventing and managing postpartum headaches.
Identifying Your Risk Factors
Certain women are more vulnerable to postpartum headaches. Risk factors include:
- A personal or family history of migraines or chronic headaches.
- Older maternal age, which increases vascular and hormonal risks.
- Multiple pregnancies (twins, triplets), which put extra strain on the body.
- Shortened or prolonged labor and the use of epidural anesthesia.
- History of high blood pressure or gestational hypertension.
Knowing your risk profile allows you to prepare ahead of time. For instance, women with a history of migraines may benefit from preventive lifestyle changes and early consultation with their doctors after delivery.
Developing a Care Routine
Think of your postpartum recovery as building a health toolkit. Key elements include:
- Scheduled check-ins with your doctor, not just at the standard 6-week visit.
- Tracking headaches in a journal—note frequency, severity, triggers, and relief methods.
- Balancing rest and activity, allowing for both recovery and gradual strength-building.
- Setting realistic expectations—healing takes time, and it’s okay to prioritize yourself.
By creating structure in your recovery, you’ll be better equipped to manage symptoms before they escalate.
Long-Term Health Considerations
While most postpartum headaches resolve within weeks or months, untreated or recurring headaches may lead to:
- Chronic migraine conditions.
- Delayed return to daily activities, including work.
- Emotional instability, such as anxiety or postpartum depression.
- Economic strain, if medical treatment is delayed or prolonged.
On the positive side, early intervention and comprehensive care improve long-term outcomes dramatically. Women who seek medical help early often recover faster and experience fewer complications.
The Importance of Early Medical Intervention
Timely medical care is not just about easing pain—it’s about preventing serious complications that could threaten your health and quality of life.
Why Early Help Matters
- Improves recovery speed: Early treatment prevents headaches from becoming chronic.
- Reduces emotional burden: Living with constant pain can worsen postpartum depression.
- Protects baby care: A healthy mother is better able to feed, bond with, and care for her newborn.
- Prevents emergencies: Recognizing red flags early avoids strokes, seizures, or severe hypertension crises.
Overcoming Barriers to Care
Many women delay seeking care due to:
- Believing headaches are “normal” after childbirth.
- Prioritizing baby’s needs over their own health.
- Fear of being judged as weak or complaining.
- Limited access to healthcare providers.
Breaking these barriers requires awareness and support from partners, families, and medical professionals. Remember: caring for yourself is part of caring for your baby.
The Fourth Trimester: Why It Deserves Equal Attention
Pregnancy receives plenty of medical focus, but the postpartum period—often called the “fourth trimester”—is just as critical. Unfortunately, many women are sent home after delivery with limited guidance on what to expect beyond physical recovery.
Postpartum headaches highlight why this phase deserves more structured care and attention.
A Period of Intense Change
During the fourth trimester, mothers experience:
- Hormonal rollercoasters as estrogen and progesterone levels drop.
- Physical healing from delivery, C-sections, or stitches.
- Sleep deprivation, which impacts every aspect of health.
- New responsibilities and emotional challenges from adjusting to motherhood.
Headaches are often a symptom of these combined stresses.
Holistic Care Approach
Instead of treating postpartum care as a one-time checkup, healthcare should be continuous and comprehensive. This includes:
- Regular blood pressure monitoring for at least 12 weeks after birth.
- Mental health screenings for depression and anxiety.
- Guidance on safe exercise and nutrition.
- Education on warning signs of complications like headaches.
By treating postpartum care as an extension of pregnancy care, mothers receive the support they need to thrive.
Emotional Impact of Postpartum Headaches
Beyond physical pain, headaches can take a heavy emotional toll. Many women describe feeling frustrated, isolated, or even guilty for being unable to fully enjoy their early days with their newborn.
Link to Postpartum Depression
Studies suggest a strong connection between frequent postpartum headaches and mood disorders. Constant pain drains emotional energy, making it harder to cope with the demands of motherhood. Left untreated, this may spiral into postpartum depression or heightened anxiety.
Breaking the Stigma
It’s important to remind mothers: you are not weak for experiencing headaches. They are a legitimate medical issue, not a sign of poor coping skills. Seeking help shows strength and protects both you and your child.
Practical Tips for Managing Postpartum Headaches at Home
While medical care is essential for severe or persistent headaches, many mothers find relief from simple home remedies and lifestyle adjustments. These techniques are safe, natural, and often effective in easing mild to moderate postpartum headaches.
Hydration and Nutrition Hacks
Dehydration is one of the most common triggers for postpartum headaches, particularly for breastfeeding mothers who lose additional fluids through milk production. To counter this:
- Keep a water bottle nearby at all times—whether in the nursery, living room, or bedroom.
- Infuse water with lemon, cucumber, or berries if plain water feels boring.
- Snack on hydrating foods like watermelon, oranges, and cucumbers.
- Avoid excessive caffeine—while small amounts may help, too much can worsen dehydration and interfere with sleep.
Pair hydration with balanced nutrition:
- Eat smaller, frequent meals instead of large, heavy ones to maintain stable blood sugar.
- Include magnesium-rich foods (spinach, nuts, avocados) which may prevent migraines.
- Boost iron intake through leafy greens and lean meats if you had significant blood loss during delivery.
Relaxation and Pain Relief Methods
Stress and muscle tension contribute to postpartum headaches, so incorporating relaxation techniques into your day can make a difference.
- Warm compresses on the neck or cold packs on the forehead can ease tension.
- Gentle massages, particularly on the shoulders and temples, release tight muscles.
- Aromatherapy with peppermint or lavender essential oils promotes relaxation and can reduce headache intensity.
- Breathing exercises: Try inhaling for 4 seconds, holding for 7, and exhaling for 8. This calms the nervous system.
Even if you only have five spare minutes, these quick strategies can help you feel more in control.
Environmental Adjustments
Your surroundings can either trigger or ease headaches. Consider making your home more “headache-friendly”:
- Dim lights in rooms where you spend time with your baby if you’re sensitive to brightness.
- Use noise-cancelling headphones or white noise machines if household sounds feel overwhelming.
- Declutter and organize to reduce stress from visual chaos.
Sometimes, small adjustments to your environment can significantly improve how you feel day-to-day.
Partner and Family Support in Postpartum Recovery
Recovering from childbirth should never be a solo journey. Family members, especially partners, play a vital role in helping mothers manage postpartum headaches and overall well-being.
Ways Partners Can Help
- Take turns with nighttime baby care to allow the mother longer stretches of uninterrupted sleep.
- Prepare meals and snacks, ensuring the mother stays nourished.
- Encourage hydration by bringing water frequently.
- Help track symptoms, such as noting when headaches occur, their severity, and possible triggers.
- Provide emotional support through reassurance, patience, and active listening.
Sometimes, simply validating the mother’s experience—acknowledging that her headaches are real and difficult—provides immense comfort.
Role of Extended Family and Friends
Family and friends can also help ease the burden by:
- Offering childcare breaks so the mother can rest or attend appointments.
- Assisting with household chores like laundry, cleaning, or grocery shopping.
- Encouraging the mother to seek medical help when needed, rather than dismissing symptoms as “normal.”
Community support makes recovery less isolating and provides the mother with space to prioritize her health.
Long-Term Outlook for Postpartum Headaches
The good news is that most postpartum headaches are temporary and improve as the body stabilizes hormonally and physically. However, some women may face ongoing challenges, especially if they had pre-existing migraine disorders.
Short-Term Outlook
- Primary headaches such as migraines or tension headaches usually improve within a few weeks as sleep patterns normalize.
- Post-dural puncture headaches often resolve within days after treatment (such as an epidural blood patch).
- Hormone-related headaches stabilize as estrogen and progesterone levels even out.
When Headaches Persist
For some women, headaches don’t fully disappear, leading to:
- Chronic migraine conditions if left untreated.
- Heightened risk of recurrence in future pregnancies.
- Increased risk of stroke or vascular disorders, especially in women with a history of hypertension.
In these cases, long-term care under a neurologist or headache specialist may be recommended.
Positive Recovery Outcomes
With early medical intervention and consistent self-care, most women return to their pre-pregnancy baseline within three to six months. Maintaining healthy routines reduces the likelihood of recurrence and supports overall well-being.
Frequently Overlooked Triggers of Postpartum Headaches
Sometimes, postpartum headaches stem from less obvious causes that new mothers or even doctors may overlook. Understanding these hidden triggers can prevent unnecessary suffering.
Hormonal Birth Control
Some women begin hormonal contraception shortly after birth, either as pills, injections, or IUDs. While effective, these can:
- Trigger migraines due to added hormone fluctuations.
- Cause vascular changes that mimic postpartum headache symptoms.
If headaches worsen after starting birth control, consult your doctor about non-hormonal alternatives.
Breastfeeding Posture
Long hours spent breastfeeding can lead to:
- Neck strain from leaning forward.
- Shoulder tension from holding the baby in awkward positions.
- Eye strain if using screens while nursing.
Using supportive pillows, changing positions, and practicing good posture can reduce these physical stressors.
Caffeine Dependence
Many mothers turn to coffee for an energy boost, but caffeine can be a double-edged sword:
- Too little caffeine after habitual intake can trigger withdrawal headaches.
- Too much caffeine may cause rebound headaches, dehydration, and anxiety.
Moderation is key—limit intake to safe levels (about 200–300 mg daily for breastfeeding mothers).
Emotional Exhaustion
Mental fatigue can be as draining as physical fatigue. Mothers juggling sleep deprivation, hormonal shifts, and constant caregiving may experience tension headaches linked to emotional stress. Therapy, counseling, or support groups can help.
Empowering Mothers Through Education and Awareness
One of the most effective ways to reduce the impact of postpartum headaches is education. When mothers, partners, and families understand what to expect, they are better equipped to take action.
Shifting the Narrative
Too often, mothers are told: “It’s just part of motherhood—deal with it.” This dismissive attitude leads many women to ignore red flags until it’s too late. Education empowers mothers to:
- Recognize what’s normal versus what’s dangerous.
- Advocate for themselves during doctor visits.
- Prioritize their health without guilt.
Healthcare Providers’ Role
Doctors, nurses, and midwives must do more than treat—they must inform. Postpartum education should include:
- Clear explanations of possible headache types.
- Guidance on safe medications during breastfeeding.
- Instructions on when to seek emergency care.
By making maternal health education a routine part of postpartum care, fewer complications slip through the cracks.
Mothers Supporting Mothers
Peer-to-peer support also matters. Online communities, local parenting groups, and postpartum meetups provide safe spaces for women to share experiences, exchange tips, and encourage one another.
Knowledge shared is strength multiplied. The more women know about postpartum headaches, the fewer will suffer in silence.
Conclusion
Postpartum headaches are far more common than most women realize, affecting nearly half of new mothers at some point after childbirth. While many headaches are mild and manageable, others can signal life-threatening conditions such as preeclampsia, stroke, or infection.
The key takeaway is this: never ignore your symptoms. Whether the pain is dull and persistent or sharp and sudden, your health matters. Sleep, nutrition, hydration, stress management, and partner support all play a role in reducing headaches, but medical care remains crucial for serious cases.
Motherhood is not about suffering in silence—it’s about thriving while caring for your baby. By staying informed, recognizing red flags, and prioritizing self-care, you can navigate postpartum headaches with confidence and resilience.
FAQs About Postpartum Headaches
1. How long do postpartum headaches usually last?
Most mild headaches resolve within days to weeks after delivery. However, hormone-related migraines may last longer, and headaches caused by medical complications require treatment to resolve.
2. Can I take headache medication while breastfeeding?
Yes. Options like acetaminophen and ibuprofen are generally safe. Stronger medications may be prescribed, but only under medical supervision. Always consult your doctor before taking anything.
3. Are postpartum headaches more common after C-sections?
Yes. Women who receive spinal or epidural anesthesia during a C-section are at higher risk of post-dural puncture headaches, which occur due to spinal fluid leakage.
4. Can stress alone cause postpartum headaches?
Absolutely. Stress, combined with sleep deprivation and physical strain, is a leading cause of tension headaches in new mothers. Stress management techniques can help significantly.
5. When should I worry about my postpartum headache?
Seek immediate medical care if your headache is sudden, severe, or accompanied by symptoms like vision changes, high blood pressure, seizures, or confusion.
Medically Reviewed by Prof. Dr. Akram
Orthopedic Surgeon | Professor | Senior Medical Specialist
Prof. Dr. Akram is a distinguished surgeon with over 15 years of clinical expertise. Having served as a lead Emergency Specialist at Complex International Government Hospital, he currently leads a specialized team of 13 medical professionals at his private hospital. As a Professor at top medical universities, he ensures that every article on WellHealthOrg.com meets rigorous clinical standards.
Medical Disclaimer:
The information provided is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician for any medical concerns.
Our content is rigorously fact-checked by our 13-member Editorial Team under the clinical supervision of Prof. Dr. Akram.