Pregnancy is often described as one of the most beautiful and transformative journeys in a woman’s life. But alongside the joy and anticipation, pregnancy also brings health challenges that must be carefully managed to protect both mother and baby. Among these challenges, eclampsia stands out as one of the most serious medical emergencies a pregnant or postpartum woman can face.
- What is Eclampsia?
- When does eclampsia occur?
- How common is eclampsia?
- Understanding the Causes and Risk Factors
- 1. First-time pregnancy
- 2. Previous history of preeclampsia or eclampsia
- 3. Maternal age
- 4. Multiple gestations
- 5. Pre-existing medical conditions
- 6. Family history and genetics
- 7. Race and socioeconomic factors
- 8. Obesity and lifestyle
- Recognizing the Key Symptoms of Eclampsia
- Warning signs to watch for:
- Diagnosis and Immediate Management
- How is eclampsia diagnosed?
- Emergency management goals:
- Long-Term Treatment and Postnatal Care
- 1. Medical follow-up
- 2. Emotional and psychological recovery
- 3. Family planning discussions
- 4. Breastfeeding considerations
- 5. Lifestyle adjustments
- Postpartum Care: Why It Matters More Than You Think
- Why postpartum monitoring is critical
- Key elements of postpartum care
- Long-Term Health Outlook After Eclampsia
- Potential long-term complications
- How to reduce long-term risks
- Prevention Strategies: Can Eclampsia Be Avoided?
- 1. Consistent prenatal care
- 2. Home monitoring
- 3. Aspirin therapy
- 4. Healthy lifestyle choices
- 5. Early delivery when necessary
- Safeguarding Your Health During Pregnancy
- Tips for protecting yourself
- Living With the Aftermath of Eclampsia
- 1. Physical recovery
- 2. Emotional impact
- 3. Family and relationship adjustments
- 4. Future pregnancies
- Expert Advice: What Doctors Want You to Know About Eclampsia
- 1. Don’t ignore high blood pressure
- 2. Be honest about symptoms
- 3. Know the emergency signs
- 4. Partner involvement is vital
- 5. Postpartum vigilance is just as important
- Real-Life Experiences: Voices of Eclampsia Survivors
Eclampsia is rare, but when it does occur, it can be devastating. It represents the final and most dangerous progression of preeclampsia, a pregnancy complication marked by high blood pressure and organ stress. The defining feature of eclampsia is the sudden onset of seizures, which can be life-threatening if not treated immediately.
Even though modern medicine has reduced the risks of maternal death compared to decades ago, eclampsia still claims lives every year. The condition does not discriminate—it can occur in otherwise healthy women, during a first pregnancy, or even after delivery when most families think the danger has passed. Because of this, raising awareness about eclampsia is not just important; it can literally save lives.
This guide dives deep into what eclampsia is, why it develops, who is at risk, how to recognize the warning signs, and what treatment and recovery look like. Whether you are pregnant, planning a pregnancy, or supporting someone through motherhood, understanding eclampsia empowers you to act quickly and effectively if warning signs appear.
What is Eclampsia?
Eclampsia is classified as a hypertensive disorder of pregnancy, but its seriousness goes far beyond high blood pressure alone. It occurs when a woman with preeclampsia—a condition characterized by elevated blood pressure, protein in the urine, and potential organ damage—progresses to having seizures. These seizures are usually generalized tonic-clonic seizures, the kind most people associate with epilepsy, involving convulsions, muscle stiffness, and loss of consciousness.
Unlike epilepsy, however, these seizures are directly tied to the stress pregnancy places on the mother’s body, particularly the cardiovascular and nervous systems.
When does eclampsia occur?
- During pregnancy (after 20 weeks): Most cases arise in the later stages of pregnancy when blood pressure tends to peak.
- During labor: The physical stress of labor can trigger seizures in someone with severe preeclampsia.
- After childbirth (postpartum eclampsia): Surprisingly, nearly one-third of cases happen after the baby is born, often within the first week but sometimes up to a month later. Many new mothers mistakenly believe the risks vanish after delivery, which is why postpartum monitoring is just as critical.
How common is eclampsia?
While preeclampsia affects around 5–10% of pregnancies worldwide, eclampsia is less common, with an estimated 1.5–10 cases per 10,000 deliveries in developed countries. In lower-resource regions, the numbers are significantly higher due to limited access to prenatal care.
Despite being relatively rare, eclampsia accounts for up to 14% of maternal deaths globally. In the U.S. alone, it remains one of the top causes of maternal mortality. These statistics highlight why prompt recognition and treatment are essential.
Think of eclampsia as the body’s final warning signal that things are dangerously out of balance. Without intervention, the risk of complications like stroke, organ failure, and even death becomes extremely high for both mother and baby.
Understanding the Causes and Risk Factors
One of the most frustrating realities for both doctors and expectant mothers is that the exact cause of eclampsia remains a mystery. Scientists believe it results from abnormal development of the placenta, which in turn affects blood vessels, circulation, and the body’s ability to regulate blood pressure. This dysfunction may lead to inflammation, blood clotting problems, and organ stress—all of which create the perfect storm for seizures.
While we don’t yet have all the answers, researchers have identified several risk factors that make eclampsia more likely. Let’s break them down:
1. First-time pregnancy
Women experiencing their first pregnancy are at higher risk, possibly because their bodies are adjusting to pregnancy-related changes for the first time.
2. Previous history of preeclampsia or eclampsia
If you had preeclampsia or eclampsia in a previous pregnancy, your risk in future pregnancies increases significantly. Doctors often recommend closer monitoring in these cases.
3. Maternal age
Teen mothers (under 20) and older mothers (over 35) face higher risks. For teenagers, the body may not yet be fully mature, while for older mothers, pre-existing conditions like high blood pressure or diabetes often play a role.
4. Multiple gestations
Carrying twins, triplets, or more puts greater strain on the circulatory system, raising the likelihood of complications.
5. Pre-existing medical conditions
Women with chronic hypertension, kidney disease, diabetes, or autoimmune conditions such as lupus are more vulnerable.
6. Family history and genetics
If your mother or sister experienced preeclampsia, your own risk is higher. This points to a possible genetic link.
7. Race and socioeconomic factors
Studies show African American women have a three times higher mortality rate from preeclampsia-related complications compared to white women. Limited access to quality healthcare, systemic disparities, and stress may contribute to this inequality.
8. Obesity and lifestyle
Obesity increases the risk of preeclampsia and eclampsia because it is often associated with insulin resistance, hypertension, and inflammation—all conditions that strain the cardiovascular system.
👉 Important Note: Having risk factors does not mean you will definitely develop eclampsia. Many women with risk factors never experience it, while others without any known risks do. However, awareness is crucial for early detection.
Recognizing the Key Symptoms of Eclampsia
Pregnancy brings a long list of symptoms—swelling, headaches, fatigue—that can feel overwhelming and sometimes misleading. This is where eclampsia becomes particularly dangerous: many of its early warning signs mimic ordinary pregnancy discomforts.
However, there are specific red flag symptoms that should never be ignored. These usually appear during severe preeclampsia and serve as the body’s alarm system before seizures occur.
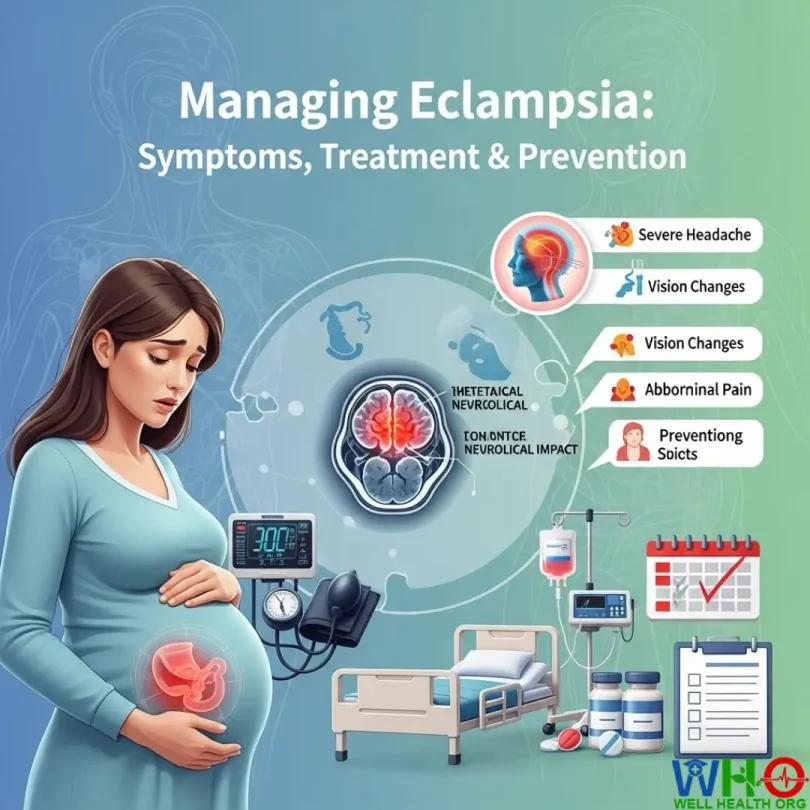
Warning signs to watch for:
- Severe, persistent headaches that don’t improve with rest or medication
- Vision disturbances, including blurred vision, seeing flashing lights or spots, and heightened sensitivity to light
- Upper abdominal pain (especially on the right side, near the liver)
- Nausea and vomiting not explained by normal morning sickness
- Sudden swelling in the face, hands, or around the eyes (beyond mild pregnancy swelling)
- Difficulty breathing or a sensation of chest tightness
- Confusion or altered mental state before seizures
What makes these symptoms dangerous is how easy it is to dismiss them. A pregnant woman might chalk up headaches to stress, swelling to salt intake, or vision changes to exhaustion. But when combined with high blood pressure, these symptoms demand urgent medical evaluation.
If a seizure occurs, it often happens suddenly, with no time for preparation. That’s why recognizing and acting on these warning signs is key to preventing full-blown eclampsia.
Diagnosis and Immediate Management
Once a woman shows symptoms of severe preeclampsia or experiences a seizure, doctors must act fast. Eclampsia is always treated as a medical emergency, and immediate stabilization becomes the top priority.
How is eclampsia diagnosed?
- Blood pressure checks: Regular prenatal visits include blood pressure screening. Readings above 140/90 mmHg raise concern.
- Urine tests: Detect protein in urine (proteinuria), a hallmark of preeclampsia.
- Blood tests: Evaluate kidney and liver function, clotting ability, and overall organ stress.
- Symptom assessment: Headaches, vision changes, or swelling guide clinical suspicion.
Emergency management goals:
- Control seizures: The gold standard treatment is magnesium sulfate, administered intravenously. It not only stops ongoing seizures but also prevents new ones. However, dosage must be carefully managed because too much magnesium can cause toxicity, leading to breathing difficulties or cardiac issues.
- Lower blood pressure: Safe antihypertensive medications such as labetalol, hydralazine, or nifedipine are commonly used. These reduce the risk of stroke or brain hemorrhage.
- Supportive care: Oxygen is given if breathing is compromised, and medical staff ensure the airway remains clear during seizures to prevent aspiration.
- Monitor mother and baby: Continuous monitoring of the mother’s vital signs and the baby’s heart rate ensures any signs of distress are detected early.
- Delivery of the baby: Ultimately, the only definitive treatment for eclampsia is delivery of the baby and placenta. Depending on how far along the pregnancy is and the condition of both mother and baby, doctors may induce labor or perform an emergency C-section.
Imagine this scenario: A pregnant woman in her third trimester arrives at the hospital with a severe headache, blurred vision, and high blood pressure. Within minutes, she has a seizure. The medical team administers magnesium sulfate, stabilizes her breathing, and prepares for an urgent delivery. Thanks to swift intervention, both mother and baby survive. This is why rapid recognition and treatment are so critical.
Long-Term Treatment and Postnatal Care
Surviving eclampsia is only the first step. Recovery doesn’t happen overnight, and the journey can be physically, mentally, and emotionally demanding. Many women assume that once the baby is born and seizures are controlled, everything returns to normal. The reality is that eclampsia can leave behind lingering health effects that require ongoing care.
1. Medical follow-up
After experiencing eclampsia, women need close monitoring for weeks and sometimes months postpartum. Blood pressure may stay elevated for several weeks, and some women develop chronic hypertension that persists long-term. Follow-up visits usually involve:
- Regular blood pressure checks
- Blood tests to monitor kidney and liver function
- Assessment for lingering neurological symptoms, such as headaches or vision issues
2. Emotional and psychological recovery
Eclampsia is a traumatic event. Many women describe feelings of fear, helplessness, or even guilt afterward. It’s common to experience anxiety about future pregnancies or even post-traumatic stress disorder (PTSD). Counseling, therapy, and support groups can be incredibly beneficial for healing mentally and emotionally.
3. Family planning discussions
Healthcare providers often recommend spacing out future pregnancies to allow the body time to recover. They may also suggest safe birth control methods until the mother is medically stable. This is particularly important for women who had severe complications or who are at risk of recurrence.
4. Breastfeeding considerations
Most women who experience eclampsia can breastfeed safely. Magnesium sulfate used during treatment does not harm the baby when passed through breast milk. However, women on certain blood pressure medications should consult their doctor to confirm which drugs are safe while nursing.
5. Lifestyle adjustments
Long-term health management often involves changes such as:
- Maintaining a healthy weight
- Reducing salt intake
- Engaging in safe physical activity
- Managing stress levels
These adjustments not only reduce the risk of high blood pressure but also support overall cardiovascular health.
In short, recovery doesn’t end at the hospital doors. Ongoing medical care and emotional support are essential for regaining health and confidence after eclampsia.
Postpartum Care: Why It Matters More Than You Think
For many new mothers, postpartum care tends to take a backseat as attention shifts to the baby. However, for women recovering from eclampsia, the postpartum period can be just as dangerous—sometimes even more so—than pregnancy itself.
Why postpartum monitoring is critical
- One-third of eclampsia cases occur after delivery. This means the risk doesn’t end once the baby is born.
- High blood pressure may linger for weeks, and if unmanaged, it can trigger complications such as stroke or organ damage.
- Emotional health may be compromised due to the traumatic experience, increasing the risk of postpartum depression or anxiety.
Key elements of postpartum care
- Scheduled follow-up visits – Women recovering from eclampsia usually need check-ups at 1–2 weeks postpartum, 6 weeks, and sometimes beyond if blood pressure remains high.
- Medication management – Some mothers may need antihypertensive medications temporarily or even long-term.
- Monitoring for late seizures – Although rare, seizures can still happen weeks after birth, which is why awareness of warning signs remains important.
- Nutritional support – A balanced diet rich in lean protein, whole grains, and fresh fruits and vegetables helps recovery and supports breastfeeding.
- Mental health care – Counseling, journaling, or joining a support group can make a significant difference in emotional healing.
Think of postpartum care as a bridge: it connects the emergency of eclampsia with a long-term path to health and stability. Skipping this step leaves women vulnerable to complications that could otherwise be prevented.
Long-Term Health Outlook After Eclampsia
Surviving eclampsia is a victory, but it often leaves women facing increased long-term health risks. Doctors now recognize eclampsia not just as a pregnancy complication, but also as a red flag for future cardiovascular disease.
Potential long-term complications
- Chronic hypertension: Many women continue to experience high blood pressure long after pregnancy.
- Increased risk of heart disease and stroke: Studies show women with a history of preeclampsia or eclampsia are twice as likely to develop cardiovascular problems later in life.
- Kidney disease: The stress eclampsia places on the kidneys can lead to lasting damage in some cases.
- Diabetes risk: Some women may develop type 2 diabetes years later, especially if obesity or insulin resistance is present.
How to reduce long-term risks
- Regular health screenings: Annual blood pressure, cholesterol, and blood sugar tests help detect problems early.
- Lifestyle changes: Prioritizing heart-healthy habits such as exercise, balanced eating, and weight management lowers the risk of future illness.
- Medical guidance: Partnering with a healthcare provider ensures personalized care and ongoing monitoring.
👉 In essence, eclampsia should be seen as a warning light on the dashboard of health. Paying attention to it now can prevent more serious conditions years down the road.
Prevention Strategies: Can Eclampsia Be Avoided?
One of the most pressing questions expectant mothers ask is: “Can eclampsia be prevented?” Unfortunately, the answer isn’t simple. While there is no guaranteed way to prevent it entirely, there are effective strategies to reduce the risk.
1. Consistent prenatal care
Attending every scheduled prenatal visit is the most important prevention step. Blood pressure checks, urine tests, and routine monitoring allow doctors to detect preeclampsia early before it progresses.
2. Home monitoring
Women at high risk may be advised to check their blood pressure at home. Keeping a daily log helps both the patient and doctor spot trends that may signal trouble.
3. Aspirin therapy
Low-dose aspirin (usually 81 mg daily) is often recommended for women at high risk of preeclampsia. Research shows it can lower the likelihood of developing the condition when started in the second trimester.
4. Healthy lifestyle choices
- Eat a nutrient-rich diet with plenty of vegetables, fruits, lean proteins, and whole grains.
- Limit processed foods high in salt and sugar.
- Exercise regularly, as approved by a doctor.
- Avoid smoking and alcohol.
5. Early delivery when necessary
In some cases, if preeclampsia becomes severe, doctors may recommend inducing labor early to prevent progression to eclampsia. While this may seem drastic, it can be life-saving for both mother and baby.
While prevention isn’t always possible, these strategies greatly improve the chances of catching preeclampsia before it escalates. The key is awareness and proactive care.
Safeguarding Your Health During Pregnancy
Pregnancy is a delicate balance between the needs of the mother and the developing baby. For women at risk of eclampsia, safeguarding health means being proactive and informed every step of the way.
Tips for protecting yourself
- Don’t skip prenatal appointments – Even if you feel well, regular check-ups catch problems early.
- Know your numbers – Familiarize yourself with your normal blood pressure, and don’t ignore changes.
- Track symptoms – Keep a journal of headaches, swelling, vision changes, or other unusual symptoms.
- Ask questions – Never hesitate to bring up concerns with your healthcare provider.
- Build a support system – Share your knowledge with your partner, family, or friends so they can recognize warning signs too.
Pregnancy can sometimes feel like walking a tightrope, but with the right tools and awareness, you can cross safely. Remember, early detection saves lives. The sooner you act on potential warning signs, the better the outcome for both you and your baby.
Living With the Aftermath of Eclampsia
For many women, eclampsia is more than just a medical emergency—it’s a life-changing event. Even after the crisis has passed, survivors often carry the physical, emotional, and psychological effects long into the future. Understanding how to live with and manage these after-effects is an important part of recovery.
1. Physical recovery
After eclampsia, fatigue is common, especially if seizures or an emergency cesarean section occurred. Some women may also experience lingering headaches, blurred vision, or high blood pressure. Doctors typically recommend rest, but not in isolation—gradual reintroduction of physical activity, like gentle walking, can help restore energy levels and support cardiovascular health.
2. Emotional impact
The trauma of seizures, hospitalization, and fears for the baby’s safety often leave emotional scars. Many women report feeling anxious, depressed, or even guilty about what happened, despite it being out of their control. Postpartum depression and post-traumatic stress disorder (PTSD) are not uncommon. Recognizing these struggles and seeking therapy or support groups can make a profound difference in emotional healing.
3. Family and relationship adjustments
Eclampsia affects not only the mother but also her family. Partners may feel helpless or fearful, while relatives often struggle with understanding the severity of the condition. Open conversations and counseling for the family can foster stronger emotional support systems.
4. Future pregnancies
One of the most pressing concerns women have is whether they can safely get pregnant again. The answer is usually yes—but with closer monitoring. Doctors may recommend preconception counseling, low-dose aspirin in future pregnancies, and more frequent prenatal check-ups.
Living with the aftermath of eclampsia requires resilience. While the journey is challenging, many women emerge stronger, more informed, and more determined to prioritize their health.
Expert Advice: What Doctors Want You to Know About Eclampsia
Doctors, midwives, and obstetricians often emphasize the same message: eclampsia is preventable in many cases, but only if warning signs are taken seriously. Their advice usually focuses on proactive care and awareness.
1. Don’t ignore high blood pressure
Even mild hypertension during pregnancy should never be brushed off. Consistently elevated readings—even if not extremely high—can indicate early preeclampsia. Doctors stress that blood pressure should be monitored regularly and reported immediately if it rises.
2. Be honest about symptoms
Some women hesitate to report headaches, swelling, or vision changes because they don’t want to seem overly worried. Doctors strongly advise against this. In pregnancy, “better safe than sorry” truly applies.
3. Know the emergency signs
If you experience severe headaches, vision disturbances, intense abdominal pain, or sudden swelling, seek medical care right away. These are not normal pregnancy symptoms—they’re red flags.
4. Partner involvement is vital
Healthcare providers often encourage partners to learn about eclampsia, too. In emergencies, partners may be the first to notice seizures or call for help. Educated partners can make life-saving decisions.
5. Postpartum vigilance is just as important
Doctors repeatedly warn that many women let their guard down after delivery. But with one-third of eclampsia cases occurring postpartum, ongoing monitoring is non-negotiable.
The takeaway? Listen to your body, communicate with your healthcare team, and act quickly if something feels wrong. That’s the advice doctors wish every expectant mother would follow.
Real-Life Experiences: Voices of Eclampsia Survivors
Hearing from women who have lived through eclampsia offers powerful insights. Their stories highlight both the dangers and the resilience required to overcome the condition.
- Maria’s story: At 32 weeks pregnant, Maria began experiencing severe headaches and swelling in her hands. She brushed it off as “just pregnancy.” One night, she collapsed from a seizure. Thanks to quick medical intervention, both she and her baby survived. Today, she shares her story to remind women never to ignore symptoms.
- Amara’s story: Amara, a first-time mother, developed postpartum eclampsia just three days after giving birth. She was home when she suddenly had a seizure. Her husband rushed her to the hospital, where doctors administered magnesium sulfate. She emphasizes the importance of partners knowing the warning signs.
- Lina’s story: Lina experienced eclampsia with her first pregnancy. For years afterward, she struggled with anxiety about having another baby. With close monitoring and preventive care, her second pregnancy was safe and complication-free. Her story shows that eclampsia does not always prevent future healthy pregnancies.
These real-life accounts underscore the importance of awareness, quick action, and emotional recovery. They also prove that while eclampsia is terrifying, survival and healing are possible.
Medically Reviewed by Prof. Dr. Akram
Orthopedic Surgeon | Professor | Senior Medical Specialist
Prof. Dr. Akram is a distinguished surgeon with over 15 years of clinical expertise. Having served as a lead Emergency Specialist at Complex International Government Hospital, he currently leads a specialized team of 13 medical professionals at his private hospital. As a Professor at top medical universities, he ensures that every article on WellHealthOrg.com meets rigorous clinical standards.
Medical Disclaimer:
The information provided is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician for any medical concerns.
Our content is rigorously fact-checked by our 13-member Editorial Team under the clinical supervision of Prof. Dr. Akram.