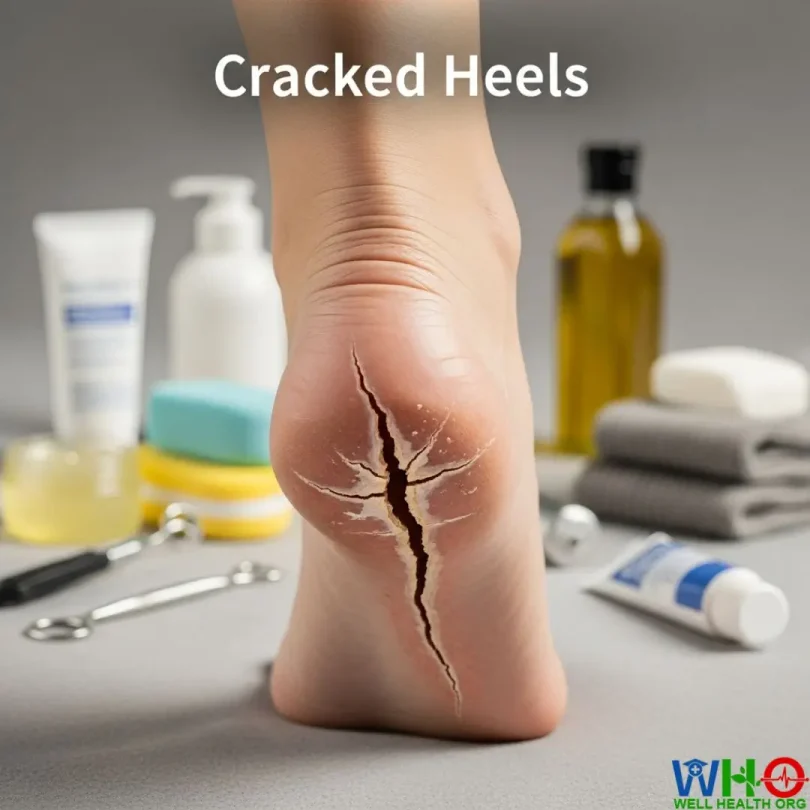
Cracked heels are more than just a cosmetic nuisance—they’re a painful reminder of how much we depend on our feet every single day. That dry, flaky skin on your heels might start as a minor annoyance, but when it deepens into splits or fissures, it can make even the simplest movement uncomfortable. In severe cases, these cracks can bleed, sting, and even lead to infections that require medical attention.
The good news? You don’t have to live with rough, painful heels. With the right treatment routine, consistency, and a bit of self-care, you can restore smooth, healthy skin and prevent cracks from coming back. This complete guide dives deep into what causes cracked heels, the best home and professional treatments, and preventive strategies to keep your feet soft and comfortable all year long.
Understanding Cracked Heels
Cracked heels—often called heel fissures—happen when the skin around your heels becomes excessively dry and thick. The constant pressure from walking or standing pushes the skin downward and outward. When the outer layers lack flexibility, they can split, leading to visible cracks that range from mild to severe.
What Exactly Happens When Heels Crack?
Your feet are covered by a tough layer of skin designed to protect against friction and weight-bearing stress. However, when this skin loses moisture, it becomes hard and inelastic. The pressure from standing and walking causes the dry skin to expand sideways, and since it can’t stretch, it splits instead. These splits may look small at first but can deepen quickly if ignored.
Once cracks form, they can trap dirt and bacteria, which further irritate the area and can lead to infection if untreated. For some people—especially those with underlying health issues like diabetes or poor circulation—cracked heels can become a serious medical problem.
Common Causes of Cracked Heels
Understanding what causes cracked heels is the first step toward preventing and treating them effectively. There isn’t just one cause—rather, it’s usually a combination of lifestyle habits, environmental factors, and health conditions.
1. Prolonged Standing
If your job requires standing for hours, especially on hard surfaces like concrete or tile, your feet take a constant beating. The repetitive pressure forces the fatty tissue under your heel to expand, which can stretch and eventually crack the skin around it.
2. Unsupportive Footwear
Your choice of shoes plays a huge role in heel health. Open-back sandals, flip-flops, and shoes without cushioning don’t support your heel pads properly. When your feet hit the ground, the unsupported heel spreads outward—eventually leading to splits. Walking barefoot, especially on hard or rough surfaces, has the same effect.
3. Dry Air and Hot Showers
Long, hot showers feel relaxing, but they also strip away your skin’s natural oils. Combine that with exposure to dry air from indoor heating or cold weather, and your heels quickly lose moisture and elasticity.
4. Excess Weight
Extra body weight puts more pressure on your feet. The fat pad beneath your heel expands to absorb this pressure, but when the skin above it is dry or thick, it can’t stretch enough, resulting in cracking.
5. Medical Conditions
Certain health conditions increase your risk of cracked heels:
- Diabetes: Reduces sweat and oil production, making the skin dry and slow to heal.
- Hypothyroidism: Can cause general skin dryness.
- Eczema and Psoriasis: Lead to flaking and scaling that can worsen heel fissures.
- Athlete’s Foot: A fungal infection that causes peeling and dryness.
Recognizing the Symptoms

Cracked heels can vary in appearance and discomfort, depending on how deep the fissures go. Here’s what you might notice:
- Dryness and Rough Texture: The skin feels coarse, thick, and flaky.
- Fine Lines or Cracks: These can start as shallow splits and deepen over time.
- Pain or Tenderness: Especially when standing or walking barefoot.
- Peeling or Itchiness: The area around the cracks can itch as it dries out.
- Bleeding or Oozing: In more severe cases, cracks may open enough to bleed.
- Signs of Infection: Redness, swelling, warmth, or pus—these require medical attention.
If you have diabetes, poor circulation, or neuropathy, do not ignore cracked heels. Even a minor wound can turn into a serious infection if left untreated.
Step-by-Step Treatment for Cracked Heels
Healing cracked heels takes a bit of patience, but the process is straightforward. The key lies in softening, exfoliating, moisturizing, and protecting your skin until it fully recovers.

Step 1: Soften and Soak
Start your healing journey by giving your feet a relaxing soak. This simple ritual loosens hard skin, reduces tightness, and preps your feet for exfoliation.
How to Do It:
- Fill a basin with lukewarm water—not hot—and soak your feet for about 15–20 minutes.
- Add a handful of Epsom salt for its soothing and skin-softening effects.
- For an extra antibacterial boost, add a small splash of apple cider vinegar or a few drops of tea tree oil.
- After soaking, pat your feet dry gently with a soft towel. Avoid rubbing, which can irritate already sensitive skin.
Pro Tip: Soak your feet in the evening to relax your muscles and make it easier to follow up with exfoliation and moisturizing before bed.
Step 2: Exfoliate Dead Skin Gently
Once your skin is soft, it’s time to remove the dead cells and calluses that prevent moisture from penetrating deeply.
What You’ll Need:
- A pumice stone or foot file
- A mild foot scrub or homemade exfoliant (mix sugar or salt with olive oil)
How to Exfoliate:
- Using gentle circular motions, rub the pumice stone over rough patches. Focus on the thickened areas around your heel.
- Avoid scrubbing too hard. Over-exfoliating can lead to soreness or worsen cracks.
- Rinse your feet and pat them dry.
Caution:
If you have diabetes or poor circulation, skip home exfoliation. It’s safer to let a podiatrist handle it to prevent cuts or infections.
Step 3: Deep Moisturization—The Heart of Healing
Moisturizing is the cornerstone of cracked heel care. The goal is to rehydrate the skin, restore flexibility, and lock in moisture.
Best Moisturizing Ingredients to Look For:
- Urea (10–25%): Softens and exfoliates thickened skin.
- Salicylic Acid or Lactic Acid: Gently dissolves calluses.
- Glycerin: Attracts and retains moisture.
- Shea Butter and Cocoa Butter: Provide rich, emollient hydration.
- Petroleum Jelly (Vaseline): Creates a barrier that seals moisture overnight.
DIY Moisturizing Remedies:
- Coconut Oil: Naturally antibacterial and rich in fatty acids—perfect for cracked heels.
- Olive Oil and Honey Mix: Hydrates and soothes inflamed skin.
- Glycerin and Rose Water: A time-tested blend that restores suppleness.
The Overnight Healing Method
For maximum results, use the overnight sock treatment:
- Apply a thick layer of moisturizer or heel balm generously.
- Slip on a pair of 100% cotton socks to hold in moisture.
- Leave them on overnight to allow the cream to penetrate deeply.
- In the morning, rinse and gently dry your feet—you’ll notice smoother, softer skin almost immediately.
Repeat this ritual nightly until cracks heal completely, then switch to a maintenance routine of daily moisturizing.
Step 4: Maintain and Protect Your Healed Heels
Once your heels start feeling softer and the painful cracks have closed, it’s crucial to maintain that progress. Without consistent care, dryness can return, bringing back the same old problem in no time.

Here’s how to maintain long-term heel health:
- Moisturize Daily:
Apply a rich, emollient foot cream or balm twice a day—morning and night. The best time to apply moisturizer is right after a shower when your skin is still slightly damp. This helps lock in hydration. - Wear Protective Footwear:
Avoid walking barefoot on hard floors, and stay away from shoes that expose your heels, such as flip-flops or backless sandals. Instead, opt for cushioned shoes with proper arch and heel support. - Keep Feet Clean:
Wash your feet daily with mild soap and lukewarm water. Make sure to dry them completely, especially between the toes, to prevent fungal infections. - Weekly Maintenance:
Give yourself a quick foot soak and gentle exfoliation once or twice a week. This removes buildup and helps your moisturizer penetrate better. - Hydrate Internally:
Drink plenty of water throughout the day. Hydration isn’t just about external creams—your skin’s moisture starts from within.
By turning foot care into a regular routine rather than an occasional fix, you’ll maintain smooth, crack-free heels year-round.
When to Seek Professional Treatment
While mild to moderate cracked heels respond well to home remedies, there are situations where seeing a podiatrist or dermatologist is essential.
You should seek medical care if:
- Your heel cracks are deep, bleeding, or extremely painful
- You notice swelling, redness, or pus (signs of infection)
- You have diabetes, neuropathy, or poor circulation
- Home treatments haven’t helped after 1–2 weeks
- The cracks interfere with walking or daily activity
Ignoring severe fissures can lead to complications like cellulitis, a painful bacterial infection that spreads beneath the skin. In people with diabetes, untreated heel cracks can progress to foot ulcers, which require urgent medical attention.
Professional Treatment Options for Cracked Heels
When home treatments aren’t enough, professionals can offer advanced therapies designed to speed up healing and restore your skin’s health.
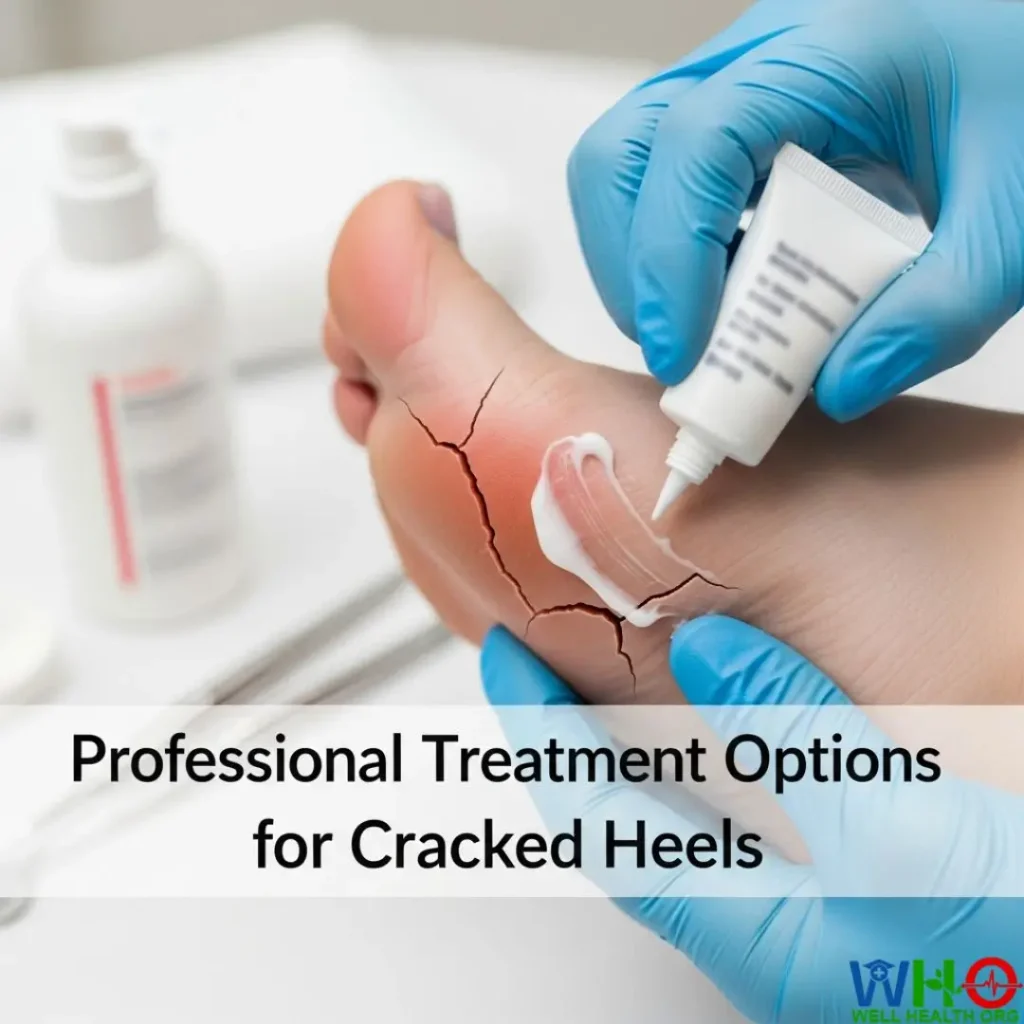
1. Mechanical Debridement
A podiatrist carefully removes hardened calluses and dead skin using a sterile scalpel. This process instantly reduces pressure on the cracks and allows moisturizers to penetrate more effectively.
2. Medical-Grade Foot Creams
These formulations contain higher concentrations of urea, lactic acid, or salicylic acid, offering deeper hydration and exfoliation. They’re particularly effective for chronic or severely dry heels.
3. Pressure Distribution Assessment
Some clinics use advanced pressure mapping to identify how your feet bear weight when walking. This helps tailor custom footwear or orthotic inserts to prevent heel pressure and cracking.
4. Dressings and Bandages
If your cracks are open or painful, your podiatrist may apply protective dressings or heel cups that cushion the area, reduce friction, and promote healing.
5. Laser or Chemical Peels
For persistent dryness, dermatologists may use chemical peels containing glycolic or lactic acid to dissolve rough skin layers, revealing smoother, new skin underneath.
The Hidden Risks of Ignoring Cracked Heels
Cracked heels might seem harmless at first, but when neglected, they can escalate into painful or even serious conditions.
Here’s what can happen if you don’t treat them properly:
- Deep Fissures:
Superficial cracks can deepen over time, leading to bleeding and discomfort with every step. - Infection:
Once bacteria or fungi enter through open skin, they can cause redness, swelling, and oozing. In severe cases, this leads to cellulitis—a painful skin infection that may require antibiotics. - Chronic Pain:
Repeated cracking and inflammation can make walking or standing unbearable, impacting your mobility. - Complications in Diabetes:
Diabetic patients face a higher risk since reduced sensation and slower healing can lead to ulcers or even gangrene in extreme cases.
Simply put, treating cracked heels early prevents pain and complications later. Prevention is always better (and easier) than cure.
Prevention: The Best Defense Against Cracked Heels
Once your heels have healed, prevention becomes the secret to keeping them that way. Cracked heels rarely develop overnight—they’re a result of small habits and neglect that build up over time.
Here’s how to stay one step ahead:
1. Keep Skin Hydrated
Apply a thick, urea-based cream daily. Focus on your heels and soles but avoid applying between the toes, where moisture buildup can cause fungal infections.
2. Choose Supportive Footwear
Invest in shoes with cushioned heels and closed backs. This prevents the fat pad under your heel from expanding outward and splitting the skin. Avoid thin-soled shoes or walking barefoot for long periods.
3. Regular Foot Checks
Make a habit of inspecting your feet each day—especially if you have diabetes or circulatory issues. Catching dryness or redness early allows you to treat it before cracks form.
4. Wear Socks That Breathe
Opt for cotton or moisture-wicking socks. They help your skin retain moisture while preventing excessive sweating that could cause irritation.
5. Limit Prolonged Standing
If you must stand for long hours, try to shift your weight frequently, use anti-fatigue mats, or wear shoes with extra cushioning.
6. Stay Hydrated and Eat Well
Drink plenty of water and include foods rich in omega-3 fatty acids, vitamins E and C, and zinc in your diet. These nutrients support healthy skin from the inside.
Top Recommended Products for Cracked Heels
Building a foot care kit ensures you always have the right tools on hand to prevent or treat cracks quickly.
| Product Type | What It Does | Key Tip |
|---|---|---|
| Urea Cream (10–25%) | Exfoliates and deeply hydrates thick skin | Apply nightly before bed |
| Heel Balm with AHA | Smooths rough skin while moisturizing | Use 2–3 times weekly |
| Petroleum Jelly | Locks in moisture and protects from friction | Best for overnight use |
| Pumice Stone / Foot File | Gently removes dead skin | Use after soaking |
| Cotton Socks | Traps moisture and enhances healing | Ideal for overnight treatment |
| Epsom Salt Foot Soak | Relaxes, softens, and detoxifies | Add to lukewarm water for 15-minute soak |
These simple products, when used consistently, can completely transform the condition of your heels.
Real-Life Tips and Expert Insights
- Rotate Shoes Regularly: Wearing the same pair every day can lead to uneven wear and pressure points.
- Avoid Harsh Soaps: Stick to mild cleansers; harsh soaps strip natural oils from your feet.
- Use a Humidifier: Dry indoor air can sap moisture from your skin—keep a humidifier in your room during winter.
- Massage Your Feet: Regular massages with coconut or olive oil boost circulation and soften tough skin.
- Don’t Peel Skin: If dead skin starts to lift, never pull it off—it can tear healthy skin and cause bleeding.
Small daily actions add up to big results when it comes to healthy, smooth heels.
Your Path to Soft, Healthy Heels
Cracked heels don’t have to be a permanent problem. With consistent care—soaking, exfoliating, moisturizing, and protecting—you can restore even the roughest skin to a soft, pain-free state. The secret is consistency, not complexity.
Start your nightly foot care ritual today. Commit to moisturizing every day, wear supportive shoes, and give your feet the same care you’d give your face or hands. In just a few weeks, you’ll notice smoother, stronger, and healthier heels that make every step more comfortable.
Remember, your feet carry you through life—treat them with kindness, and they’ll reward you with comfort and confidence in return.
Frequently Asked Questions
1. How long does it take for cracked heels to heal?
Mild cracks can improve within a week of consistent care. Deep fissures may take 2–4 weeks, depending on how well you follow your routine and whether you use overnight moisturization.
2. Can I use Vaseline for cracked heels?
Yes. Petroleum jelly is one of the best occlusive agents—it seals in moisture and prevents further cracking. For best results, apply it before bed and wear cotton socks overnight.
3. Is walking barefoot bad for my heels?
Absolutely. Walking barefoot, especially on hard floors, increases heel pressure and dryness. Always wear cushioned shoes or slippers indoors.
4. Are cracked heels a sign of a medical condition?
Sometimes, yes. Conditions like diabetes, eczema, thyroid issues, or psoriasis can make you more prone to dry, cracked skin. If your heels crack frequently, consult a healthcare provider.
5. What’s the best time to apply heel cream?
Right after bathing or before bedtime. Applying moisturizer when your skin is slightly damp helps lock in moisture and accelerate healing.
Medically Reviewed by Prof. Dr. Akram
Orthopedic Surgeon | Professor | Senior Medical Specialist
Prof. Dr. Akram is a distinguished surgeon with over 15 years of clinical expertise. Having served as a lead Emergency Specialist at Complex International Government Hospital, he currently leads a specialized team of 13 medical professionals at his private hospital. As a Professor at top medical universities, he ensures that every article on WellHealthOrg.com meets rigorous clinical standards.
Medical Disclaimer:
The information provided is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician for any medical concerns.
Our content is rigorously fact-checked by our 13-member Editorial Team under the clinical supervision of Prof. Dr. Akram.






![Top 10 Low-Calorie Summer Foods to Shrink Your Waistline [2026 Guide] 17 low-calorie summer foods](https://wellhealthorg.com/wp-content/uploads/2026/05/low-calorie-summer-foods-1-145x100.webp)