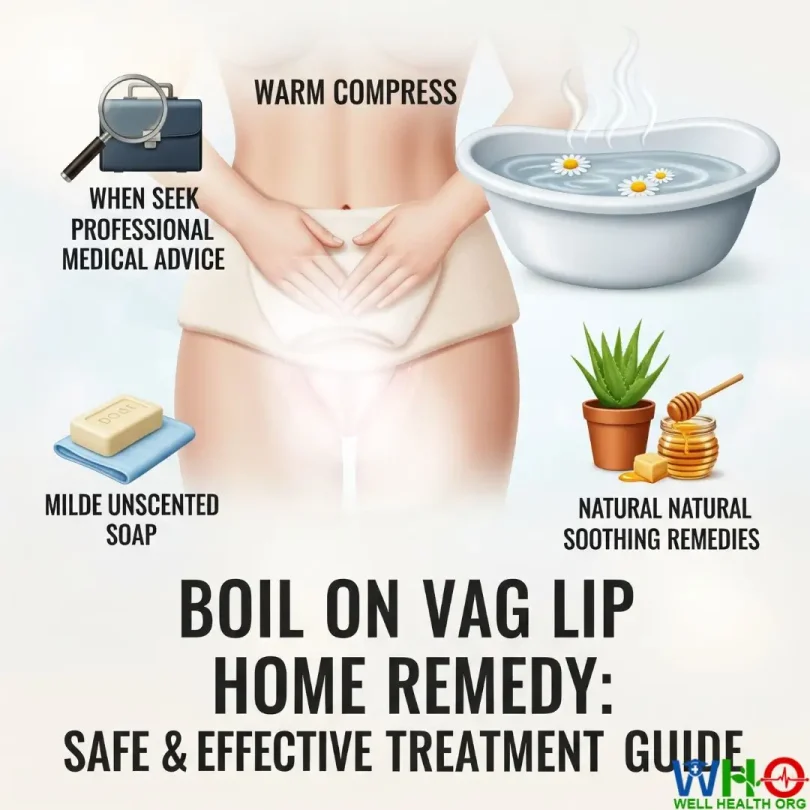
Boils on Vaginal Lips
Discovering a painful, swollen bump on your vaginal lip can be worrying, uncomfortable, and even a little embarrassing. You might immediately wonder — “Is this serious?” or “Can I treat it at home safely?” The truth is, boils on the vaginal lips (also called vulvar abscesses) are relatively common and, in most mild cases, can be managed effectively at home with proper hygiene, care, and patience.
- Boils on Vaginal Lips
- Understanding Vaginal Boils and Why They Develop
- Common Causes of Boils on the Vaginal Lips
- Recognizing the Symptoms Early
- Home Remedies That Help Heal Vaginal Boils Naturally
- 1. Warm Compress Therapy: Nature’s Simple Healer
- 2. Sitz Baths for Gentle Cleansing and Pain Relief
- 3. Maintain Excellent Vulvar Hygiene
- 4. Choose Loose, Breathable Clothing
- 5. Pain and Inflammation Relief
- 6. Healing Through Nutrition and Hydration
- 7. Rest and Avoid Physical Strain
- 8. What NOT to Do When Treating Vaginal Boils at Home
- ❌ Don’t Pop or Squeeze the Boil
- ❌ Avoid Harsh Chemicals and Strong Soaps
- ❌ Don’t Use Unverified Home Remedies
- ❌ Avoid Shaving or Waxing the Area During Healing
- ❌ Don’t Share Towels or Razors
- 9. Natural Remedies and Soothing Alternatives
- Aloe Vera Gel
- Turmeric Paste
- Epsom Salt Compress
- Coconut Oil for Moisture and Protection
- When to Seek Professional Medical Care
- 10. Medical Treatments for Persistent or Severe Boils
- Incision and Drainage (I&D)
- Antibiotic Therapy
- Treatment for Bartholin’s Abscess
- Management for Chronic or Recurrent Boils
- 11. Effective Prevention Strategies
- Practice Good Daily Hygiene
- Opt for Breathable Underwear
- Smart Hair Removal Practices
- Avoid Sharing Personal Items
- Boost Immunity Through Lifestyle
- Monitor for Early Signs
- 12. Emotional Well-Being and Self-Care During Recovery
- 13. When Recurrent Boils Indicate an Underlying Condition
- Your Path Forward: Healing and Prevention with Confidence
- Frequently Asked Questions (FAQs)
- 1. How long do vaginal boils take to heal?
- 2. Can I use antibiotics cream on vaginal boils?
- 3. Are vaginal boils contagious?
- 4. Can stress cause vaginal boils?
- 5. When should I be concerned about a vaginal boil?
- Final Thoughts
This comprehensive guide will walk you through safe and proven home remedies for vaginal boil treatment, explain why these infections occur, help you recognize when to see a doctor, and share preventive strategies to stop them from recurring. With the right knowledge, you can feel confident and comfortable managing this condition from home — while knowing exactly when professional care is necessary.
Understanding Vaginal Boils and Why They Develop
A vaginal boil forms when a hair follicle or oil gland on the vulva becomes infected, usually due to bacteria entering through tiny cuts, ingrown hairs, or clogged pores. The most common culprit is Staphylococcus aureus, a bacterium that naturally lives on our skin but can cause infections when it penetrates deeper layers.
When the infection develops, your body responds by sending white blood cells to fight it. The result? Swelling, redness, tenderness, and the formation of a pus-filled bump that may grow over several days before coming to a head and draining naturally.
While it may sound intimidating, most vaginal boils are localized infections that resolve on their own with supportive care. However, understanding what triggers them is essential to prevent recurrence.
Common Causes of Boils on the Vaginal Lips
Several everyday habits and conditions can increase the likelihood of developing a vulvar boil:
- Hair Removal Practices:
Shaving, waxing, or using depilatory creams can irritate or damage hair follicles, allowing bacteria to enter. Shaving too closely or using dull razors can also lead to ingrown hairs — a common starting point for boils. - Tight or Non-Breathable Clothing:
Synthetic underwear and tight leggings trap heat and moisture, creating a breeding ground for bacteria. Friction from tight clothing can also irritate delicate vulvar skin. - Poor Hygiene or Contamination:
Skipping daily washing or using dirty towels and razors can introduce harmful bacteria to the area. Sharing personal hygiene tools increases the risk further. - Weakened Immune System:
People with diabetes, chronic illnesses, or those undergoing chemotherapy or taking immunosuppressive drugs are more prone to infections, including skin boils. - Bartholin’s Gland Blockage:
When the Bartholin glands — located near the vaginal opening — become blocked, they can form cysts. If bacteria invade, these cysts can develop into abscesses resembling boils.
Recognizing the Symptoms Early
Early detection and care can make a major difference. Typical symptoms of a vaginal boil include:
- A tender, swollen lump near the vaginal lip or groin
- Localized redness and warmth
- Pain that increases when sitting, walking, or wearing tight clothing
- Pus or drainage from the bump as it comes to a head
- In some cases, mild fever or fatigue
If you notice a rapidly enlarging boil, spreading redness, or multiple boils appearing together (a condition called carbuncle), it’s important to seek medical advice.
Home Remedies That Help Heal Vaginal Boils Naturally
When handled properly, most mild boils will heal on their own within one to two weeks. The following evidence-based home treatments can speed up healing and provide comfort during recovery.
1. Warm Compress Therapy: Nature’s Simple Healer
The most effective first-line remedy for vaginal boils is a warm compress. Applying gentle heat increases blood circulation, encourages white blood cells to fight the infection, and helps the boil mature and drain naturally.
How to use it properly:
- Soak a clean, soft washcloth in warm (not hot) water.
- Wring out excess water and gently place the cloth on the affected area for 10–15 minutes.
- Repeat this 3–4 times daily using a freshly cleaned cloth each time.
Avoid reusing the same cloth without washing it, as this can spread bacteria. Within a few days, you may notice the boil forming a soft white or yellow “head,” signaling that drainage may soon occur naturally.
If this happens, let it drain on its own — never squeeze or pop it. Popping a boil can push bacteria deeper into the skin, cause spreading infection, or leave scarring.
2. Sitz Baths for Gentle Cleansing and Pain Relief
A sitz bath is another soothing and effective home remedy. It involves sitting in warm water that covers the vulva and buttocks, which reduces inflammation and relieves pain.
Here’s how to do it safely:
- Fill a clean basin or bathtub with warm water (not scalding).
- Add about one teaspoon of salt per liter of water to create a mild saline solution.
- Sit in the bath for 15–20 minutes, once or twice daily.
Salt has natural antibacterial properties, and the warmth promotes healing. Afterward, gently pat the area dry with a clean towel — never rub. Make sure to disinfect the basin after each use to prevent reinfection.
3. Maintain Excellent Vulvar Hygiene
Cleanliness is key when dealing with boils in intimate areas. However, it’s equally important not to overdo it.
Best hygiene practices include:
- Wash your hands before and after touching the affected area.
- Clean the vulva gently with warm water only — avoid soaps, douches, or perfumed washes that can irritate the skin or disrupt your natural pH balance.
- After washing, pat dry using a clean towel or soft tissue.
- Change your underwear daily and after sweating or exercising.
Avoid bubble baths or harsh feminine hygiene products, which can strip away the good bacteria that naturally protect your vaginal area.
4. Choose Loose, Breathable Clothing
What you wear can dramatically impact your recovery. Tight clothing increases friction and traps heat — both of which can worsen irritation or delay healing.
Opt for loose, cotton underwear and breathable clothing that allows air to circulate. Avoid synthetic fabrics, tight leggings, or shapewear until the area fully heals. Cotton helps absorb moisture, keeping the vulva dry and reducing bacterial buildup.
When resting at home, you may even skip underwear altogether to improve airflow and comfort.
5. Pain and Inflammation Relief
Boils on the vaginal lips can be quite painful, especially when walking or sitting. Over-the-counter medications can help you stay comfortable while your body heals.
Recommended options:
- Acetaminophen (Tylenol): Eases pain and lowers fever.
- Ibuprofen (Advil or Motrin): Reduces both pain and inflammation.
Always follow dosage instructions carefully and consult your doctor if you have existing medical conditions like liver or kidney disease. Applying a clean, warm compress before taking medication can also enhance comfort.
6. Healing Through Nutrition and Hydration
Your diet plays an often-overlooked role in wound healing. To support recovery from an infection, focus on foods that boost your immune system and reduce inflammation:
- Fresh fruits and vegetables (especially leafy greens, citrus, and berries)
- Protein sources like eggs, fish, lean meats, and legumes
- Anti-inflammatory foods like turmeric, ginger, and green tea
- Probiotics such as yogurt and kefir to balance healthy bacteria
Drink plenty of water to stay hydrated — at least 8 glasses a day. Proper hydration helps flush toxins and supports the body’s natural healing mechanisms.
7. Rest and Avoid Physical Strain
It may seem simple, but rest is one of the most powerful remedies. Physical stress, sweating, and friction can worsen swelling and delay healing. Try to minimize prolonged sitting, cycling, or other activities that put pressure on the affected area.
When lying down, consider positioning yourself slightly on your side to avoid direct pressure. Getting enough sleep also enhances immune function, helping your body recover faster.
8. What NOT to Do When Treating Vaginal Boils at Home
While it’s tempting to try quick fixes when in pain or discomfort, some actions can worsen the infection or cause long-term damage. Here’s what you should absolutely avoid:
❌ Don’t Pop or Squeeze the Boil
Trying to pop a boil can push bacteria deeper into the tissue, leading to a more severe infection or even cellulitis (a skin infection that spreads quickly). It can also cause scarring or further swelling. Allow it to rupture and drain naturally.
❌ Avoid Harsh Chemicals and Strong Soaps
The vulvar area is highly sensitive. Avoid products containing alcohol, fragrances, or artificial dyes. These can irritate the skin and alter the natural pH balance, creating an environment where harmful bacteria thrive.
❌ Don’t Use Unverified Home Remedies
The internet is filled with untested suggestions — from applying toothpaste to garlic or vinegar on boils. These methods can cause chemical burns, allergic reactions, or worsening of symptoms, especially in the delicate genital area.
❌ Avoid Shaving or Waxing the Area During Healing
Until the boil has completely healed, avoid any hair removal methods that can further irritate the skin or open new follicles to bacterial infection. Wait at least two weeks after full recovery before resuming hair removal, and always use a clean, sharp razor.
❌ Don’t Share Towels or Razors
These personal items can transfer bacteria to others or reintroduce infection to yourself. Keep separate, freshly washed towels for your use during the healing process.
9. Natural Remedies and Soothing Alternatives
In addition to standard home remedies, a few gentle natural approaches can support healing if used cautiously and correctly. Remember, the vulvar area is delicate, so always do a patch test on another area of your body first and discontinue if irritation occurs.
Aloe Vera Gel
Pure aloe vera gel has anti-inflammatory and cooling properties. Applying a thin layer of 100% natural aloe vera (not mixed with artificial fragrance or alcohol) can soothe burning and itching sensations around the boil. Always ensure hands are clean before application.
Turmeric Paste
Turmeric contains curcumin, a compound with powerful antibacterial and anti-inflammatory benefits. Mix one teaspoon of turmeric powder with a few drops of clean water to form a paste. Apply gently near (but not inside) the affected area, leave for 10–15 minutes, then rinse thoroughly with warm water.
Epsom Salt Compress
Adding Epsom salt to your warm compress or sitz bath can help draw out infection and reduce swelling. Dissolve about one tablespoon in a basin of warm water and apply the compress for 10 minutes daily.
Coconut Oil for Moisture and Protection
Virgin coconut oil contains lauric acid, a natural antibacterial agent. Applying a small amount can help protect the surrounding skin from friction and irritation once the boil begins to heal. Avoid using it on open wounds or active pus-filled boils.
Note: Always ensure that anything applied to the vulva is sterile, natural, and chemical-free. When in doubt, consult a gynecologist or dermatologist before trying new remedies.
When to Seek Professional Medical Care
While most vulvar boils heal at home, some cases require professional evaluation and treatment. Ignoring certain warning signs could allow the infection to worsen or spread.
You should seek medical care if:
- The boil grows larger than ½ inch in diameter
- Pain becomes severe or interferes with sitting and walking
- You develop a fever, chills, or fatigue
- Redness or swelling spreads beyond the immediate area
- The boil doesn’t drain or improve after 10–14 days of home care
- You experience recurrent boils in the same area
Your doctor may perform a minor procedure to safely drain the boil under sterile conditions and prescribe antibiotics if bacteria have spread beyond the local site. In some cases, lab cultures are taken to identify the specific bacteria responsible, ensuring the most effective treatment.
If you have diabetes, compromised immunity, or are pregnant, it’s best to consult your doctor as soon as you notice any boil or unusual swelling in the vulvar region — even if it appears minor.
10. Medical Treatments for Persistent or Severe Boils
When home remedies aren’t enough, doctors can offer several treatment options to accelerate recovery and prevent recurrence.
Incision and Drainage (I&D)
For large or painful boils that won’t drain naturally, a clinician may perform a quick in-office procedure called incision and drainage. The area is numbed, the boil is carefully opened, and pus is removed under sterile conditions. This relieves pressure and pain immediately.
Antibiotic Therapy
If there’s evidence of spreading infection, your doctor may prescribe oral or topical antibiotics. Commonly used antibiotics include cephalexin, dicloxacillin, or clindamycin — depending on the bacterial strain and your medical history.
Treatment for Bartholin’s Abscess
If the boil is due to an infected Bartholin’s gland cyst, drainage may be followed by placing a Word catheter, a tiny tube that helps the gland drain continuously and prevents re-blockage. Occasionally, surgery is required to remove the gland if infections recur frequently.
Management for Chronic or Recurrent Boils
For individuals who get boils repeatedly, your healthcare provider may recommend a decolonization protocol, which involves using topical antibiotic ointments (like mupirocin) in the nostrils and antiseptic body washes (like chlorhexidine) to eliminate bacteria that cause infections.
11. Effective Prevention Strategies
Preventing vaginal boils is just as important as treating them. By adopting a few simple but consistent habits, you can dramatically reduce your risk of future occurrences.
Practice Good Daily Hygiene
- Cleanse the vulvar area with warm water daily.
- Avoid douching or perfumed soaps.
- Pat dry gently after bathing or sweating.
- Change underwear daily and after workouts.
Opt for Breathable Underwear
Cotton underwear is your best friend. It allows airflow, reduces moisture buildup, and keeps your skin healthy. Avoid nylon or polyester fabrics that trap heat and bacteria.
Smart Hair Removal Practices
If you prefer hair removal, use a clean, sharp razor each time. Shave in the direction of hair growth and apply a mild, fragrance-free moisturizer afterward to reduce irritation. Consider trimming instead of shaving for sensitive skin.
Avoid Sharing Personal Items
Towels, razors, or undergarments should never be shared. These items can harbor bacteria and increase your risk of developing boils or other infections.
Boost Immunity Through Lifestyle
Your immune system plays a crucial role in fighting infections. Maintain a balanced diet rich in vitamins, stay hydrated, exercise regularly, and manage stress levels. Chronic stress and fatigue can weaken your immune defenses, making infections more likely.
Monitor for Early Signs
At the first sign of tenderness or redness, start applying warm compresses. Early intervention can often prevent a small bump from turning into a painful boil.
12. Emotional Well-Being and Self-Care During Recovery
Dealing with a vaginal boil can be distressing — not just physically but emotionally. Many women feel embarrassed or anxious about the condition, but it’s important to remember: you’re not alone. Boils are common, natural skin infections that have nothing to do with poor hygiene or sexual activity.
During recovery:
- Be patient with your body. Healing takes time.
- Avoid self-blame — these infections can happen to anyone.
- Use mild relaxation techniques like breathing exercises or meditation to manage stress and pain.
- If recurring boils are affecting your confidence or relationships, consider discussing your concerns with a healthcare provider or counselor.
Taking care of your mental health is just as important as physical healing.
13. When Recurrent Boils Indicate an Underlying Condition
If vaginal boils keep returning despite good hygiene, it may be a sign of an underlying medical condition that needs attention.
Common related factors include:
- Diabetes: High blood sugar levels weaken immunity and increase bacterial infections.
- Hidradenitis Suppurativa (HS): A chronic skin condition causing painful lumps and abscesses in areas with sweat glands, such as the groin.
- Immune Deficiency Disorders: Conditions that reduce your body’s ability to fight infections.
A healthcare provider can perform tests to identify these issues and create a personalized prevention or treatment plan.
Your Path Forward: Healing and Prevention with Confidence
Boils on the vaginal lips can be painful and uncomfortable, but the good news is that most cases are easily manageable at home with warmth, hygiene, and patience. By understanding the underlying causes and knowing when to seek medical help, you can navigate the healing process safely and effectively.
Use warm compresses and sitz baths, maintain cleanliness, wear breathable clothing, and nourish your body with healthy foods. Most importantly, don’t panic or feel ashamed — these infections are common and treatable.
Your body has remarkable healing power. With consistent care and awareness, you can not only recover fully but also prevent future recurrences.
Frequently Asked Questions (FAQs)
1. How long do vaginal boils take to heal?
Most small boils heal within 7–14 days with home care. Larger or infected ones may take longer, especially if professional drainage or antibiotics are needed.
2. Can I use antibiotics cream on vaginal boils?
Topical antibiotics like mupirocin may help mild cases, but they should only be used if recommended by your doctor. Overuse of antibiotics can cause resistance or irritation.
3. Are vaginal boils contagious?
They’re not typically contagious through casual contact, but the bacteria causing them can spread through shared towels, razors, or clothing. Always use personal items only.
4. Can stress cause vaginal boils?
Indirectly, yes. Stress weakens the immune system, which can make you more prone to bacterial infections and delayed healing.
5. When should I be concerned about a vaginal boil?
If the boil is extremely painful, not healing after two weeks, or you develop fever or spreading redness, contact a healthcare provider immediately. These may indicate a more serious infection.
Final Thoughts
Caring for your body, especially in sensitive areas, is an act of self-respect and awareness. By following these evidence-based remedies, maintaining healthy habits, and listening to your body’s signals, you can heal faster, prevent recurrences, and feel comfortable again.
Empower yourself with knowledge — and remember, even the most uncomfortable problems have practical, effective solutions when addressed with care and confidence.
Medically Reviewed by Prof. Dr. Akram
Orthopedic Surgeon | Professor | Senior Medical Specialist
Prof. Dr. Akram is a distinguished surgeon with over 15 years of clinical expertise. Having served as a lead Emergency Specialist at Complex International Government Hospital, he currently leads a specialized team of 13 medical professionals at his private hospital. As a Professor at top medical universities, he ensures that every article on WellHealthOrg.com meets rigorous clinical standards.
Medical Disclaimer:
The information provided is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician for any medical concerns.
Our content is rigorously fact-checked by our 13-member Editorial Team under the clinical supervision of Prof. Dr. Akram.