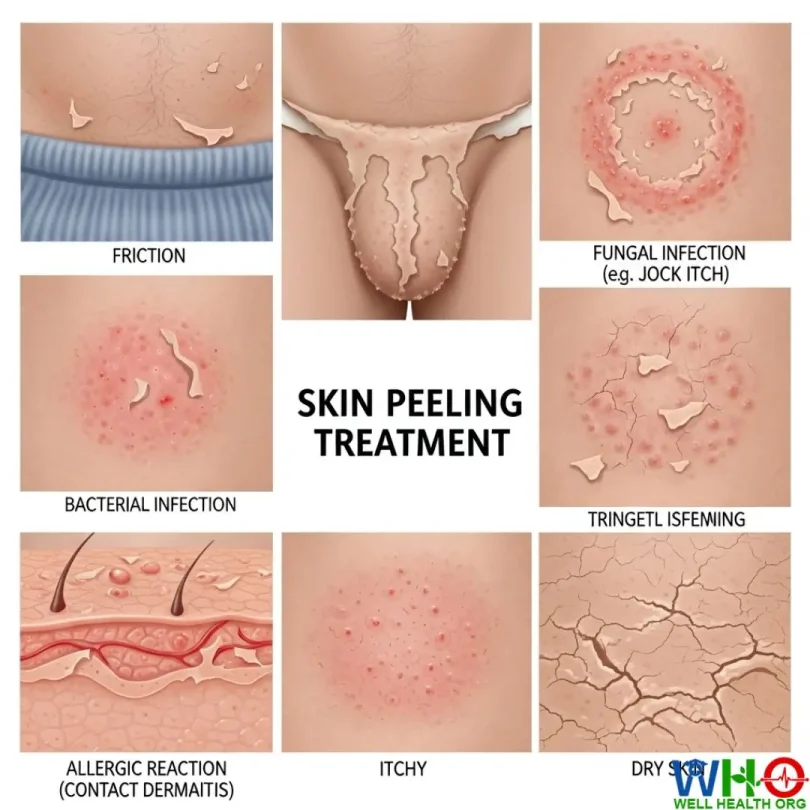
Skin Peeling Around the Male Private Area
Noticing the skin peeling around your private area can trigger instant concern, discomfort, and even embarrassment. It’s not exactly something most men feel comfortable discussing openly — but here’s the truth: it’s far more common than you might think. Whether the issue affects the penis, scrotum, or surrounding groin area, skin peeling can stem from several different causes, ranging from mild irritation to underlying medical conditions.
- Skin Peeling Around the Male Private Area
- Why Is Skin Peeling Around the Male Private Area Happening?
- 1. Friction and Chafing
- 2. Contact Dermatitis (Allergic or Irritant Reaction)
- 3. Jock Itch (Tinea Cruris)
- 4. Yeast Infection (Candidiasis) in Men
- 5. Eczema (Atopic or Seborrheic Dermatitis)
- 6. Psoriasis
- 7. Scabies
- 8. Herpes Simplex Virus (HSV)
- 9. Syphilis
- 10. Lichen Planus and Lichen Sclerosus
- 11. Balanitis, Balanoposthitis, and Posthitis
- 12. Recognizing Related Symptoms
- 13. How Doctors Diagnose Skin Peeling Around the Private Area
- 14. Treatment Options for Peeling Skin on the Penis or Groin
- For Friction or Irritation
- For Allergic Reactions (Contact Dermatitis)
- For Fungal Infections (Jock Itch or Yeast)
- For Bacterial Infections
- For Chronic Skin Conditions (Eczema, Psoriasis, Lichen)
- For Viral Infections (Herpes)
- 15. Preventing Skin Peeling in the Genital Area
- 16. When to See a Doctor
- 17. Practical Self-Care Tips for Faster Healing
- 18. Taking Charge of Your Intimate Health
- Conclusion
- FAQs
Understanding why it’s happening is the key to finding effective relief. Many cases are completely treatable with simple lifestyle adjustments or over-the-counter remedies. However, persistent or severe symptoms might indicate infections or dermatological conditions that need medical attention.
This comprehensive guide covers everything you need to know — from the causes of penis skin peeling to practical treatments, prevention tips, and when to see a doctor. By the end, you’ll have the confidence and clarity to manage and protect your intimate health effectively.
Why Is Skin Peeling Around the Male Private Area Happening?
The skin in your genital region is extremely thin and sensitive. It’s designed to be flexible and protective, but it’s also easily irritated by heat, friction, moisture, or even certain hygiene products. When that delicate balance is disrupted, peeling, dryness, and irritation can appear.
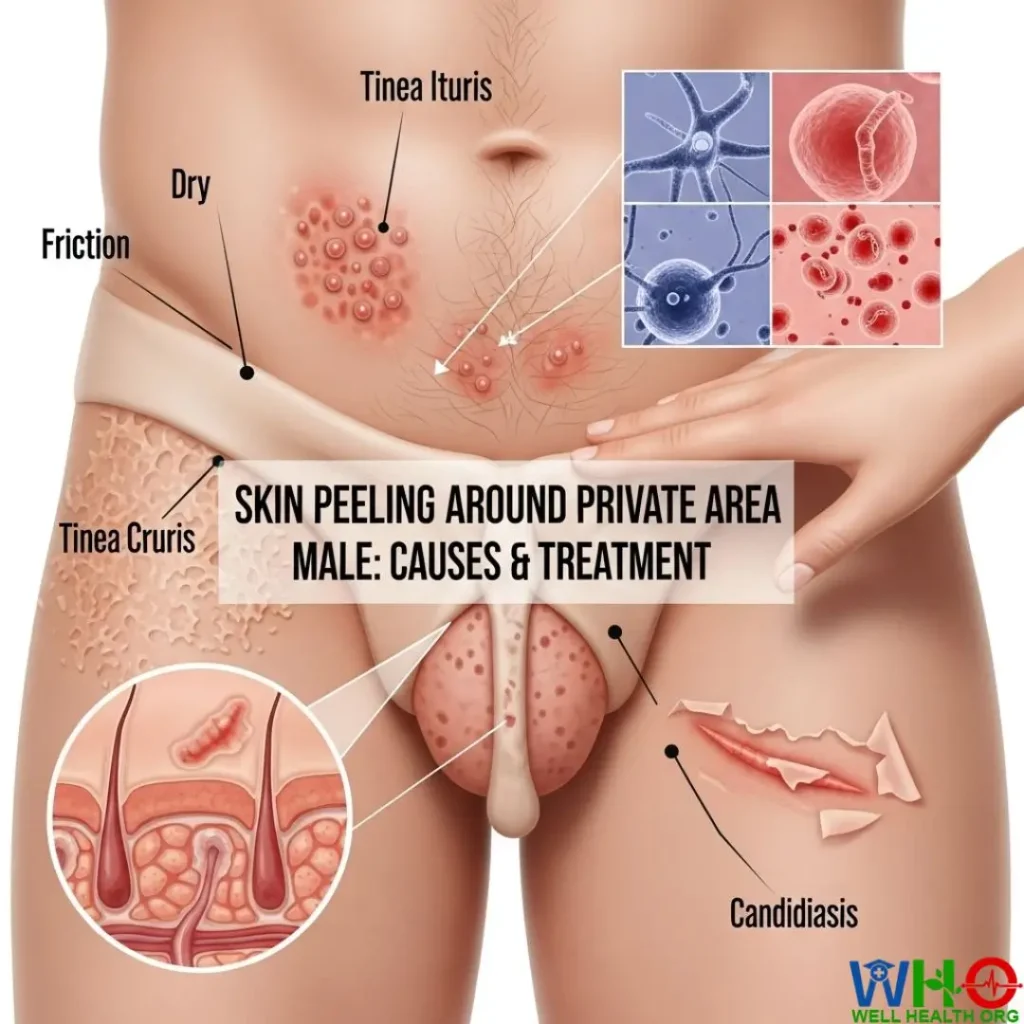
Let’s explore the most common causes — from the simplest to the more serious — so you can better identify what’s happening to your skin.
1. Friction and Chafing
Friction is one of the leading causes of skin peeling in the genital area. It occurs when constant rubbing or pressure irritates the skin, stripping away its natural oils and protective barrier. Over time, this irritation can cause redness, dryness, and eventually peeling.
Common triggers include:
- Tight or synthetic underwear that traps heat and moisture
- Prolonged physical activity like running or cycling
- Masturbation or sexual activity without enough lubrication
- Dry humping or grinding
- Hot, humid weather that increases sweating
When the skin’s outer layer is constantly rubbed, it becomes inflamed and starts to flake or peel. The area may feel sore, tight, or itchy — especially where the friction was most intense.
Simple Fixes:
- Choose breathable, cotton-based underwear that fits comfortably.
- Avoid tight jeans or pants that cause rubbing.
- During sex or masturbation, use a high-quality, water-based lubricant to minimize friction.
- After sweating or exercise, wash gently and change into dry clothing to prevent further irritation.
In most cases, friction-related peeling improves within a few days once the skin is allowed to heal.
2. Contact Dermatitis (Allergic or Irritant Reaction)
If your genital skin suddenly starts peeling or itching after using a new product, contact dermatitis could be the culprit. This reaction happens when the skin comes into contact with an allergen or irritant that triggers inflammation.
Common offenders include:
- Scented body washes, soaps, or lotions
- Laundry detergents with dyes or harsh chemicals
- Latex condoms or certain lubricants
- Spermicides and fragranced wipes
- Deodorant sprays or aftershaves
Symptoms of contact dermatitis include redness, itching, blistering, and peeling — often appearing within hours of exposure, though sometimes the reaction can take a day or two to develop.
What to Do:
- Stop using any new product you recently introduced to your hygiene or laundry routine.
- Cleanse the area gently with lukewarm water and a mild, unscented soap.
- Apply a soothing, fragrance-free moisturizer or a light barrier cream to calm irritation.
- If the reaction is severe or persists for more than a few days, consult a dermatologist.
Your skin should begin to improve once the irritant is removed. For ongoing sensitivity, consider switching to hypoallergenic, dermatologist-tested personal care items.
3. Jock Itch (Tinea Cruris)
Jock itch is a fungal infection that thrives in warm, moist environments — and the groin area is the perfect breeding ground. It’s especially common among men who sweat heavily, wear tight clothing, or share locker rooms or towels.
Symptoms often include:
- Red, scaly rash along the inner thighs and groin
- Persistent itching or burning sensation
- Flaky, peeling skin around the edges of the rash
- Occasional musty odor
Though it’s not usually dangerous, jock itch can spread quickly if not treated properly.
Treatment Options:
- Over-the-counter antifungal creams or powders (like clotrimazole or terbinafine) often clear up mild cases within two weeks.
- Keep the area dry, clean, and cool. Fungi thrive in damp environments.
- Avoid sharing towels or tight athletic gear until the infection resolves.
- For stubborn infections, your doctor might prescribe stronger antifungal medication.
Consistency is key — stopping treatment too early can lead to recurrence.
4. Yeast Infection (Candidiasis) in Men
While often associated with women, men can also develop yeast infections. The fungus Candida albicans naturally lives on the skin, but when it grows excessively — often due to heat, moisture, or poor hygiene — it can cause inflammation and peeling in the genital region.
Symptoms may include:
- Itching, burning, or irritation on the head of the penis (glans)
- Redness or white patches under the foreskin
- Cracked, peeling skin that may bleed slightly
- Clumpy white discharge with a sour odor
Yeast infections can sometimes appear after unprotected sex with an infected partner, prolonged antibiotic use, or uncontrolled diabetes (since high blood sugar promotes fungal growth).
Treatment and Prevention:
- Use over-the-counter antifungal creams such as miconazole or clotrimazole.
- Wash daily with mild soap and ensure the area is completely dry afterward.
- Avoid sugary foods and alcohol, as they can feed yeast growth.
- If you’re uncircumcised, retract the foreskin gently while cleaning.
- Persistent or recurring infections should be evaluated by a doctor, who may prescribe oral antifungal medications.
5. Eczema (Atopic or Seborrheic Dermatitis)
Eczema isn’t limited to your arms or face — it can appear virtually anywhere, including the genital area. When eczema affects the penis, scrotum, or inner thighs, it can cause dryness, intense itching, flaking, and peeling skin that’s easily mistaken for an infection.
Eczema is often linked to genetics, immune sensitivity, or environmental triggers. Even stress can worsen flare-ups. The skin in the genital region is especially delicate, so once it becomes inflamed, symptoms may feel much more intense compared to other parts of the body.
Common Signs of Genital Eczema Include:
- Dry, scaly patches or flaky skin around the penis or groin
- Small fluid-filled blisters that may ooze or crust
- Cracked or thickened skin due to constant scratching
- Burning or stinging sensations after washing or sweating
How to Manage and Soothe Eczema:
- Keep the area clean but avoid over-washing, as that can strip the skin’s natural oils.
- Use fragrance-free soaps and detergents designed for sensitive skin.
- Apply a gentle moisturizer or emollient after bathing to lock in hydration.
- Over-the-counter antihistamines can help reduce itching, while mild hydrocortisone creams ease inflammation.
- Avoid synthetic fabrics and stick to breathable cotton underwear.
If eczema persists or keeps returning, a dermatologist can prescribe stronger corticosteroid creams or non-steroidal topical treatments to manage flare-ups.
6. Psoriasis
Psoriasis is an autoimmune condition where skin cells multiply too rapidly, forming red, scaly patches. When it affects the genitals — known as genital psoriasis — the appearance is usually smoother than on other areas of the body but can still cause irritation, redness, peeling, and pain during sex or urination.
Typical Symptoms of Genital Psoriasis:
- Shiny, inflamed patches on the penis, scrotum, or inner thighs
- Peeling or scaling skin without much flaking
- Itching or soreness, especially when sweating
- Cracking of skin folds
Managing Genital Psoriasis:
- Apply mild topical corticosteroids under medical supervision (stronger formulas can irritate thin genital skin).
- Use gentle moisturizers and avoid fragranced products.
- Avoid tight underwear that traps moisture and heat.
- Reduce stress, as flare-ups often worsen during stressful periods.
Severe cases may require prescription immunosuppressants or biologic therapies. A dermatologist can tailor a safe treatment plan specifically for sensitive skin in this area.
7. Scabies
Scabies is a parasitic infestation caused by microscopic mites (Sarcoptes scabiei) that burrow into the skin to lay eggs. The result is intense itching, redness, and tiny bumps or rashes — often leading to peeling due to scratching and inflammation.
It spreads easily through close physical contact, including sexual activity, shared bedding, or clothing.
How to Identify Scabies:
- Severe itching, especially at night
- Small red bumps or lines where mites burrow
- Crusted, peeling skin from scratching
- Possible presence of thin burrow tracks on the penis, wrists, or between fingers
Treatment Approach:
- Visit a doctor immediately for confirmation.
- Prescription creams containing permethrin or oral ivermectin kill the mites effectively.
- Wash all bedding, clothing, and towels in hot water to prevent re-infestation.
- Avoid close contact with others until treatment is complete.
Scabies is highly contagious but fully curable with prompt, thorough treatment.
8. Herpes Simplex Virus (HSV)
Genital herpes is a viral infection caused by the herpes simplex virus, transmitted through intimate skin-to-skin contact. Many men carry the virus without symptoms, but others experience painful outbreaks that can mimic peeling skin once the blisters rupture.
Symptoms During an Outbreak:
- Itching or tingling around the penis or anus before blisters form
- Clusters of fluid-filled sores that burst and crust over
- Painful urination or discomfort during sex
- Flu-like symptoms such as fatigue or body aches
Once the sores dry up, the skin can appear flaky or peeling as it heals.
Treatment & Management:
- There’s no permanent cure, but prescription antiviral medications like acyclovir or valacyclovir significantly reduce outbreak severity and duration.
- Avoid sexual contact during flare-ups to prevent transmission.
- Keep the affected area clean and dry to aid healing.
- Strengthen your immune system through rest, hydration, and stress reduction.
Even though herpes is lifelong, proper management and medication can help minimize recurrences and discomfort.
9. Syphilis
Syphilis is a sexually transmitted bacterial infection that progresses through distinct stages if left untreated. One of the earliest signs is a small, painless sore called a chancre that appears on the penis, scrotum, or surrounding skin — which may peel or scab as it heals.
Early Signs Include:
- Single or multiple painless sores on the genitals
- Mild peeling or flaking skin where the sore appeared
- Swollen lymph nodes
- Later symptoms may include a body rash, fever, and fatigue
Treatment and Recovery:
- Syphilis is treatable with prescription antibiotics, typically penicillin injections.
- Early treatment ensures full recovery and prevents long-term complications affecting the heart, brain, and nervous system.
- Avoid sexual activity until your doctor confirms you’re no longer infectious.
Because syphilis can resemble other conditions, timely medical diagnosis is crucial.
10. Lichen Planus and Lichen Sclerosus
Both lichen planus and lichen sclerosus are chronic inflammatory skin conditions that can affect the genital region. They cause itching, white patches, thin or shiny skin, and peeling that may resemble scarring or irritation.
- Lichen planus often appears as purplish, flat bumps that itch intensely.
- Lichen sclerosus causes white, patchy skin that feels tight and may tear easily.
Treatment Options:
- Prescription corticosteroid creams or ointments reduce inflammation and itching.
- In more severe cases, doctors may recommend immune-modulating medications, light therapy, or retinoid treatments.
- Keeping the skin moisturized and avoiding irritants are key to preventing flare-ups.
Because these conditions are chronic, long-term management under a dermatologist’s care is essential.
11. Balanitis, Balanoposthitis, and Posthitis
Inflammation around the penis can lead to peeling, redness, swelling, and irritation.
- Balanitis affects the glans (head) of the penis.
- Posthitis affects the foreskin.
- Balanoposthitis involves both areas simultaneously.
These conditions can arise from poor hygiene, infections, tight foreskin (phimosis), or underlying skin disorders like eczema or psoriasis.
Typical Symptoms:
- Red, tender, or shiny skin
- Mild peeling or cracking
- Pain during urination or intercourse
- Foul-smelling discharge under the foreskin
Treatment and Prevention:
- Maintain good hygiene by gently cleaning under the foreskin daily.
- Use mild, unscented soaps or just warm water.
- Apply topical antifungal or antibiotic creams if infection is suspected.
- If inflammation persists, see a urologist or dermatologist for further evaluation.
12. Recognizing Related Symptoms
Skin peeling in the genital area rarely occurs in isolation. Paying attention to associated symptoms can help narrow down the underlying cause and guide proper treatment. Many skin conditions share similar signs, so observing subtle differences is crucial.
Here are some common accompanying symptoms and what they might suggest:
| Symptom | Possible Cause |
|---|---|
| Itching | Fungal infections (like jock itch or yeast), eczema, psoriasis, or scabies |
| Redness or discoloration | Irritation from friction, allergic reactions, or infections |
| Pain or burning sensation | Infection, herpes, or severe irritation |
| Blisters or sores | Herpes, syphilis, or lichen planus/sclerosus |
| Discharge with odor | Yeast or bacterial infection |
| Swelling or tightness | Balanitis, dermatitis, or allergic reaction |
| Fever or malaise | Viral or bacterial infections |
Tip: Keep a short daily record of your symptoms — when they worsen, what products you use, and any sexual activity or new exposure. This information can help your doctor pinpoint the cause more efficiently.
Also, resist scratching. While scratching provides momentary relief, it often worsens irritation, introduces bacteria, and delays healing.
13. How Doctors Diagnose Skin Peeling Around the Private Area
While self-observation is helpful, a professional diagnosis is the only way to know for sure what’s happening. Many conditions — from fungal infections to STIs — can look nearly identical, making self-diagnosis unreliable and sometimes dangerous.
During your appointment, a healthcare provider will typically:
- Review your symptoms and medical history:
They’ll ask about recent sexual activity, hygiene products, new detergents, and past skin conditions. - Perform a physical examination:
The doctor will inspect the affected skin, looking for patterns, rashes, or lesions that indicate specific causes. - Order laboratory tests (if needed):
- Skin swabs or cultures to identify bacterial or fungal growth
- Blood tests for sexually transmitted infections like herpes or syphilis
- Skin biopsy in rare or chronic cases, to rule out autoimmune disorders
Once the underlying issue is identified, your doctor will recommend personalized treatment options to promote healing and prevent recurrence.
14. Treatment Options for Peeling Skin on the Penis or Groin
Treatment depends entirely on the root cause. Below is a breakdown of effective treatments categorized by condition:
For Friction or Irritation
- Switch to loose, breathable cotton underwear to reduce friction.
- Apply a soothing, unscented moisturizer or aloe vera gel to relieve dryness.
- Use lubricants during sexual activity or masturbation to prevent chafing.
- Avoid tight clothing or vigorous activities until the skin heals.
For Allergic Reactions (Contact Dermatitis)
- Identify and remove the triggering product or chemical.
- Wash the area gently with lukewarm water and pat dry.
- Use mild steroid creams (like 1% hydrocortisone) for inflammation — but only short-term.
- Switch to hypoallergenic, fragrance-free hygiene products.
For Fungal Infections (Jock Itch or Yeast)
- Apply antifungal creams, sprays, or powders (clotrimazole, terbinafine, or miconazole).
- Keep the area clean and dry.
- Avoid synthetic underwear or tight gym wear.
- Persistent infections may require oral antifungal medication prescribed by a doctor.
For Bacterial Infections
- Take antibiotics as prescribed and complete the full course.
- Avoid sexual contact until symptoms fully resolve.
- Maintain good hygiene and wear clean, dry underwear daily.
For Chronic Skin Conditions (Eczema, Psoriasis, Lichen)
- Use prescription corticosteroid creams or non-steroidal ointments under medical guidance.
- Take oral antihistamines to relieve itching.
- Apply moisturizers frequently to prevent dryness and cracking.
- Work with a dermatologist for long-term management and trigger identification.
For Viral Infections (Herpes)
- Antiviral medications like acyclovir or valacyclovir help shorten outbreaks.
- Keep the affected area clean and avoid touching the sores.
- Avoid sexual contact during outbreaks.
- Support immune function with adequate rest, hydration, and stress control.
Each treatment plan should be followed exactly as prescribed — stopping too soon may lead to recurrence or resistance.
15. Preventing Skin Peeling in the Genital Area
Prevention is always better (and easier) than cure. Maintaining proper genital hygiene and lifestyle habits can drastically reduce your risk of irritation, infection, and peeling.
Here are expert-backed prevention tips:
- Practice Daily Hygiene:
Wash the area gently with warm water and a mild, unscented cleanser. Avoid scrubbing — the goal is to cleanse, not strip the skin’s protective oils. - Dry Properly:
Moisture is a breeding ground for bacteria and fungi. Pat dry instead of rubbing, and change out of sweaty clothes as soon as possible. - Wear Breathable Fabrics:
Cotton underwear allows air circulation, keeping the area cool and dry. Avoid synthetic materials that trap sweat. - Use Protection:
Condoms reduce your risk of sexually transmitted infections. If you’re allergic to latex, switch to polyurethane or polyisoprene alternatives. - Avoid Harsh Products:
Steer clear of heavily perfumed soaps, sprays, or laundry detergents that can cause allergic reactions. - Stay Hydrated and Eat Well:
Balanced nutrition and hydration promote healthy skin barrier function. - Reduce Friction:
Use lubricants during sex and masturbation, and avoid prolonged activities that cause rubbing. - Manage Stress:
Chronic stress can trigger eczema or psoriasis flare-ups, so relaxation techniques like deep breathing, yoga, or exercise can help. - Check for Underlying Health Issues:
Conditions like diabetes or obesity can increase your risk of skin infections. Regular check-ups can help detect and manage them early.
16. When to See a Doctor
While mild cases of skin peeling often resolve with basic care, some symptoms demand immediate professional attention. Delaying medical evaluation could worsen your condition or lead to serious complications.
Seek medical help if you experience:
- Persistent pain, swelling, or redness
- Peeling accompanied by blisters, sores, or ulcers
- Unusual discharge or foul odor
- Difficulty or pain during urination
- Fever, fatigue, or flu-like symptoms
- Peeling that doesn’t improve after a week of home care
- Suspicion of a sexually transmitted infection
Doctors see these issues regularly — there’s no need for embarrassment. Getting checked early ensures accurate diagnosis and quicker relief.
17. Practical Self-Care Tips for Faster Healing
If your skin is already irritated or peeling, here are some immediate, practical steps to promote faster recovery:
- Use cold compresses: Gently soothe the area to reduce inflammation.
- Avoid scratching or picking: This worsens irritation and can cause infection.
- Apply barrier creams: Products with zinc oxide (like baby rash ointments) can protect healing skin.
- Hydrate from within: Drink plenty of water — skin heals faster when it’s hydrated.
- Wear loose clothing: Give your skin room to breathe and recover.
- Avoid sex until healed: Friction or bodily fluids can delay healing or spread infection.
Healing may take a few days to a couple of weeks depending on the cause. Be patient and consistent with care.
18. Taking Charge of Your Intimate Health
Skin peeling around your private area can be uncomfortable, but it doesn’t have to be a lasting problem. Most causes are treatable with simple care, awareness, and timely intervention.
Start by assessing what’s changed recently — new soaps, tight clothing, or sexual activity without lubrication can all be triggers. Make small adjustments first, and give your skin time to recover. If symptoms persist or worsen, don’t hesitate to consult a healthcare provider.
Your genital health is an essential part of your overall well-being. Treat it with the same attention and respect as any other part of your body.
Conclusion
Peeling skin around the male genital area may feel alarming, but in most cases, it’s manageable and reversible. Whether caused by friction, infection, or an allergic reaction, the key lies in identifying the root cause and following the right treatment plan.
Prioritize hygiene, wear comfortable fabrics, avoid irritants, and keep the area dry. For persistent or recurring symptoms, seek professional guidance. With consistent care and awareness, you can maintain healthy, irritation-free skin — and greater comfort and confidence in your intimate health.
FAQs
1. Is it normal for the skin on my penis to peel after sex?
Yes, minor peeling after intense or prolonged sex can occur due to friction or dryness. Using lubricants and avoiding tight clothing afterward usually resolves it quickly.
2. Can stress cause peeling in the genital area?
Indirectly, yes. Stress can trigger skin conditions like eczema or psoriasis, which may cause peeling or irritation.
3. How long does it take for peeling skin to heal?
Mild irritation may heal within a few days, but fungal or bacterial infections can take one to two weeks or longer, depending on treatment consistency.
4. Should I use antiseptic creams on peeling skin?
Avoid harsh antiseptics unless prescribed by a doctor — they can worsen irritation. Gentle cleansers and moisturizers are safer.
5. Can poor hygiene cause genital skin peeling?
Yes. Failing to wash regularly or dry thoroughly after bathing can lead to infections and irritation that cause peeling.
Medically Reviewed by Prof. Dr. Akram
Orthopedic Surgeon | Professor | Senior Medical Specialist
Prof. Dr. Akram is a distinguished surgeon with over 15 years of clinical expertise. Having served as a lead Emergency Specialist at Complex International Government Hospital, he currently leads a specialized team of 13 medical professionals at his private hospital. As a Professor at top medical universities, he ensures that every article on WellHealthOrg.com meets rigorous clinical standards.
Medical Disclaimer:
The information provided is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician for any medical concerns.
Our content is rigorously fact-checked by our 13-member Editorial Team under the clinical supervision of Prof. Dr. Akram.