VFib vs V-Tach
Heart rhythm disorders, known medically as arrhythmias, can be frightening and sometimes life-threatening. Among them, two of the most dangerous are Ventricular Fibrillation (VFib) and Ventricular Tachycardia (V-Tach). Both conditions arise in the ventricles—the lower chambers of the heart that pump blood throughout the body.
- VFib vs V-Tach
- What is Ventricular Fibrillation (VFib)?
- Causes of VFib: Why Does it Happen?
- Symptoms of VFib: What to Watch Out For
- What is Ventricular Tachycardia (V-Tach)?
- Types of V-Tach
- 1. Nonsustained Ventricular Tachycardia (NSVT)
- 2. Sustained Ventricular Tachycardia (SVT)
- Causes of V-Tach
- Symptoms of V-Tach
- Key Differences Between VFib and V-Tach
- Electrical Activity
- Heart Rate
- ECG Appearance
- Blood Flow
- Immediate Danger
- Diagnosing VFib and V-Tach
- Electrocardiogram (ECG)
- Additional Diagnostic Tools
- Treatment for VFib: Life-Saving Interventions
- Emergency Treatment
- Post-Emergency Management
- Treatment for V-Tach: Stabilization & Long-Term Care
- Emergency Care
- Stable V-Tach
- Long-Term Treatment Options
- Outlook and Long-Term Management
- VFib Prognosis
- V-Tach Prognosis
- Long-Term Management
- Preventing VFib and V-Tach: Can These Arrhythmias Be Avoided?
- Lifestyle Choices for Heart Health
- Medical Prevention
- High-Risk Individuals
- Real-Life Examples: What Patients Experience
- Case Example 1: VFib on the Soccer Field
- Case Example 2: V-Tach in a Heart Attack Survivor
- Case Example 3: Nonsustained V-Tach
- The Importance of AEDs and CPR in Saving Lives
- How AEDs Work
- Why Every Minute Matters
- CPR: The Bridge to Defibrillation
- Lifestyle Tips for Long-Term Heart Health
- Daily Habits
- For Patients With ICDs or Past Arrhythmias
- Conclusion: VFib vs. V-Tach—Different Paths, Same Urgency
- FAQs About VFib and V-Tach
At first glance, VFib and V-Tach might seem similar because both involve abnormal ventricular rhythms. However, they differ significantly in terms of causes, symptoms, severity, diagnosis, and treatment approaches. Understanding these differences is crucial, as both conditions can lead to sudden cardiac arrest if not treated promptly.
This comprehensive guide will break down everything you need to know about VFib and V-Tach, including:
- How they differ in terms of electrical activity
- What symptoms to look out for
- How they appear on an ECG
- What treatments are available today
- What patients and families can do to lower risks
⚠️ Disclaimer: This article is for educational purposes only and should not replace professional medical advice. If you experience chest pain, fainting, dizziness, or palpitations, seek medical attention immediately. Always consult a qualified healthcare provider for diagnosis and treatment.
What is Ventricular Fibrillation (VFib)?
Ventricular Fibrillation is one of the most severe forms of arrhythmia. In VFib, the ventricles don’t beat in a coordinated way—instead, they quiver rapidly and chaotically. This disorganized electrical activity means the heart cannot pump blood effectively, cutting off oxygen supply to vital organs, especially the brain.
When VFib occurs, collapse happens almost instantly. Within seconds, the individual may lose consciousness, stop breathing normally, and enter sudden cardiac arrest. Without immediate treatment, VFib is usually fatal within minutes.
The American Heart Association (AHA) identifies VFib as the leading cause of sudden cardiac death worldwide, emphasizing the need for urgent recognition and rapid defibrillation.
Causes of VFib: Why Does it Happen?
VFib rarely develops in a perfectly healthy heart. Instead, it’s usually triggered by an underlying heart condition or a sudden external factor. The most common causes include:
- Heart Attack (Myocardial Infarction): A sudden blockage in a coronary artery can deprive heart muscle of oxygen, triggering VFib.
- Coronary Artery Disease (CAD): Narrowed or clogged arteries increase long-term risk.
- Cardiomyopathy: Structural damage to the heart muscle weakens electrical stability.
- Congenital Heart Defects: Some people are born with abnormal heart structures or conduction systems.
- Electrolyte Imbalances: Low potassium, calcium, or magnesium can destabilize heart rhythms.
- Major Trauma: A direct blow to the chest (e.g., in sports accidents) can trigger sudden VFib.
- Electrocution or Severe Shock: Electrical currents disrupt the heart’s natural electrical signals.
- Drug Toxicity: Stimulants, illegal drugs, or even certain medications can provoke dangerous arrhythmias.
- Sepsis or Severe Infections: Infections that spread throughout the body strain the heart and may cause rhythm disturbances.
Symptoms of VFib: What to Watch Out For
Unlike some heart conditions that give warning signs, VFib often strikes without any prior symptoms. The hallmark is sudden collapse and unresponsiveness. Other immediate signs include:
- Loss of consciousness within seconds
- No detectable pulse
- Stopped or abnormal breathing (gasping)
- Blue-tinged lips or skin due to lack of oxygen
Since VFib progresses rapidly to cardiac arrest, it’s considered a medical emergency where every second counts. Bystanders who act quickly with CPR and defibrillation can significantly improve survival chances.
What is Ventricular Tachycardia (V-Tach)?
Ventricular Tachycardia is another dangerous arrhythmia, but it differs from VFib in a critical way. Instead of chaotic quivering, the ventricles beat too quickly but still in a somewhat organized manner. Typically, V-Tach means the heart rate exceeds 100 beats per minute and originates from abnormal signals within the ventricles.
Because the beats are so rapid, the heart doesn’t have enough time to fill with blood between contractions. As a result, blood flow to the brain and other vital organs is reduced, which can cause dizziness, fainting, or even cardiac arrest if left untreated.
Unlike VFib, V-Tach can sometimes be self-limiting (nonsustained) or persist dangerously (sustained).
Types of V-Tach
Doctors generally classify V-Tach into two categories:
1. Nonsustained Ventricular Tachycardia (NSVT)
- Lasts less than 30 seconds
- Often resolves spontaneously without intervention
- Usually doesn’t cause severe symptoms but indicates underlying heart problems
2. Sustained Ventricular Tachycardia (SVT)
- Persists for more than 30 seconds
- Causes major circulatory problems, including low blood pressure and fainting
- Can quickly deteriorate into VFib and sudden cardiac arrest
- Always treated as a medical emergency
Causes of V-Tach
V-Tach often arises from structural or electrical abnormalities in the heart. Common causes include:
- Ischemic Heart Disease (IHD): Reduced blood flow due to narrowed arteries
- Heart Attack Scarring: Damaged tissue disrupts normal electrical pathways
- Cardiomyopathy: Weak or enlarged heart muscle increases arrhythmia risk
- Structural Heart Disease: Includes valve disorders and prior heart surgeries
- Genetic Conditions: Such as Long QT Syndrome or Brugada Syndrome
- Electrolyte Imbalances: Especially low potassium or magnesium
- Substance Use: Cocaine, methamphetamines, and stimulants increase arrhythmia risk
Symptoms of V-Tach
Symptoms depend on the heart rate, episode duration, and overall heart health. They may range from mild palpitations to life-threatening collapse:
- Racing heartbeat or fluttering in the chest
- Dizziness or lightheadedness
- Shortness of breath
- Chest pain or tightness
- Fainting (syncope)
- In severe cases: cardiac arrest
Patients with pre-existing heart disease are at the highest risk for serious complications from V-Tach.
Key Differences Between VFib and V-Tach
Although both VFib and V-Tach are dangerous ventricular arrhythmias, they differ significantly in their electrical activity, impact on blood flow, and immediate danger. Understanding these differences can help patients, caregivers, and even bystanders recognize the urgency of each condition.
Electrical Activity
- VFib: The ventricles experience chaotic, uncoordinated electrical signals. Instead of pumping blood, they only quiver weakly, producing no effective circulation.
- V-Tach: The ventricles beat very quickly but in a somewhat organized rhythm. Blood flow may still exist, though it is often inadequate.
Heart Rate
- VFib: So irregular and chaotic that it’s almost impossible to measure a heart rate.
- V-Tach: Typically fast and steady, usually exceeding 100–250 beats per minute.
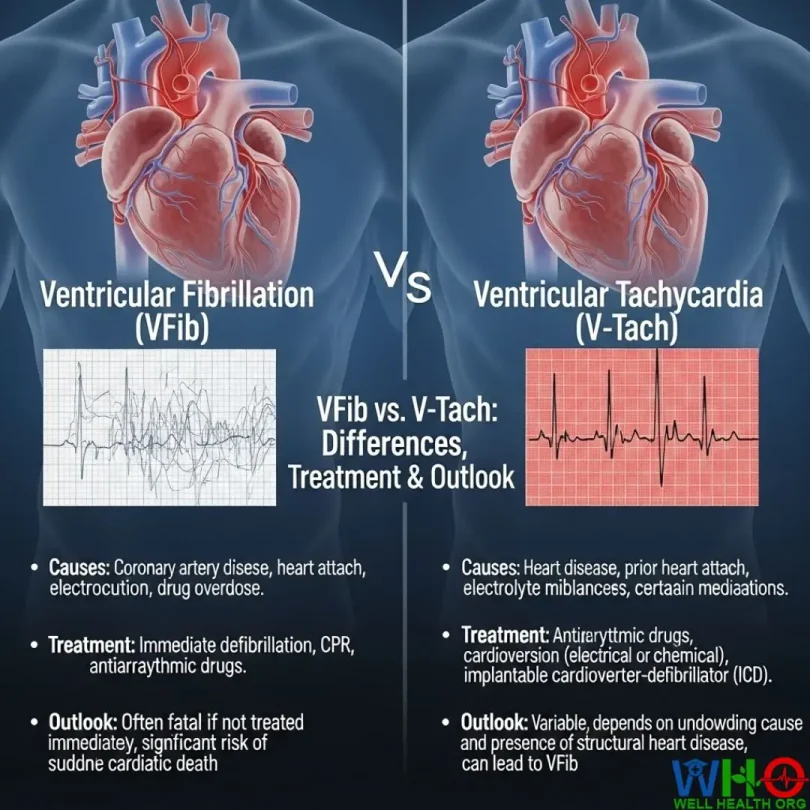
ECG Appearance
- VFib: Displays a completely disorganized, wavy line with no clear P waves, QRS complexes, or T waves.
- V-Tach: Shows wide, abnormal QRS complexes repeating at a rapid, consistent pace.
Blood Flow
- VFib: Virtually no blood is pumped out of the heart, leading to immediate collapse.
- V-Tach: Blood flow may still be present but reduced. If prolonged, it can deteriorate into VFib.
Immediate Danger
- VFib: Always fatal if untreated, requiring instant defibrillation and CPR.
- V-Tach: May be self-limiting in short bursts, but sustained V-Tach is life-threatening and requires urgent intervention.
In simple terms: V-Tach is like a car engine revving too fast, while VFib is like a car engine sputtering out completely. One is unstable, and the other is complete shutdown.
Diagnosing VFib and V-Tach
Because these arrhythmias are often medical emergencies, diagnosis usually occurs in urgent care or emergency settings. The electrocardiogram (ECG or EKG) is the primary tool for distinguishing between VFib and V-Tach.
Electrocardiogram (ECG)
- VFib: Appears as irregular, chaotic waves without identifiable heart cycle patterns.
- V-Tach: Shows wide, fast, repetitive QRS complexes without normal P waves.
Additional Diagnostic Tools
Once the patient is stabilized, doctors may perform further tests to identify underlying causes:
- Blood Tests: To check cardiac enzymes (for heart attack), electrolytes, and thyroid function.
- Echocardiogram (Echo): Uses ultrasound to assess heart structure, pumping efficiency, and valve function.
- Coronary Angiogram: An invasive imaging procedure to detect blockages in coronary arteries.
- Cardiac MRI/CT: Provides detailed images of the heart’s structure and any scarring or damage.
- Electrophysiology Study (EPS): Specialized testing to map the heart’s electrical system.
- Genetic Testing: If there’s suspicion of inherited arrhythmia syndromes like Brugada or Long QT.
Timely and accurate diagnosis helps guide long-term treatment decisions, reducing the risk of recurrence.
Treatment for VFib: Life-Saving Interventions
VFib is a medical emergency where every second counts. Without intervention, death usually occurs within minutes.
Emergency Treatment
- Immediate CPR: Chest compressions keep blood flowing to the brain and vital organs until defibrillation is available.
- Defibrillation: An automated external defibrillator (AED) delivers an electrical shock to reset the heart’s rhythm. AEDs are now widely available in airports, gyms, offices, and public spaces.
- Advanced Cardiac Life Support (ACLS): In a hospital, medical teams may use IV medications such as epinephrine, amiodarone, or lidocaine if VFib persists after shocks.
Post-Emergency Management
Survivors of VFib usually require:
- Implantable Cardioverter-Defibrillator (ICD): Prevents future sudden cardiac death by delivering shocks when VFib or V-Tach is detected.
- Medication: Beta-blockers, antiarrhythmics, or ACE inhibitors may be prescribed.
- Lifestyle Adjustments: Healthy diet, avoiding stimulants, regular exercise (as approved by a cardiologist).
- Treating Underlying Conditions: Coronary artery stenting, bypass surgery, or heart failure management may be necessary.
Without rapid defibrillation, survival rates are extremely low. With quick action, however, survival can exceed 50%.
Treatment for V-Tach: Stabilization & Long-Term Care
The treatment for V-Tach depends on whether the patient is stable or unstable.
Emergency Care
- Unstable V-Tach (with low blood pressure, chest pain, or fainting): Requires immediate cardioversion (a synchronized shock).
- Cardiac Arrest due to V-Tach: Treated like VFib—with CPR, defibrillation, and IV medications.
Stable V-Tach
If the patient is conscious and stable:
- Antiarrhythmic Drugs: Such as amiodarone, procainamide, or lidocaine may restore normal rhythm.
- Observation and Monitoring: Short episodes may not require shock but do need further evaluation.
Long-Term Treatment Options
- Medications: Beta-blockers, calcium channel blockers, or long-term antiarrhythmic therapy.
- Catheter Ablation: A minimally invasive procedure where radiofrequency energy destroys small areas of abnormal heart tissue causing arrhythmias.
- Implantable Cardioverter-Defibrillator (ICD): Recommended for patients at high risk of recurrent V-Tach or VFib.
- Surgery: In rare cases, surgical interventions like ventricular aneurysm resection may be considered.
Modern treatment strategies have significantly improved survival rates, especially with ICDs and ablation therapies.
Outlook and Long-Term Management
The prognosis for VFib and V-Tach varies depending on how quickly treatment is given and what caused the arrhythmia.
VFib Prognosis
- Considered the most dangerous arrhythmia.
- Survival rates drop by 7–10% for every minute defibrillation is delayed.
- Even survivors may face neurological complications due to oxygen deprivation.
V-Tach Prognosis
- Depends heavily on underlying cause.
- Patients with ischemic cardiomyopathy have poorer outcomes without treatment.
- With ICDs, survival rates have greatly improved.
- Idiopathic V-Tach (without structural heart disease) often has an excellent prognosis.
Long-Term Management
- Lifestyle Modifications: Heart-healthy diet, exercise, stress reduction, and quitting smoking.
- Regular Checkups: Ongoing cardiology visits ensure monitoring and early intervention.
- ICD & Ablation: Dramatically reduce risk of sudden cardiac death in high-risk patients.
Preventing VFib and V-Tach: Can These Arrhythmias Be Avoided?
Not every episode of VFib or V-Tach can be prevented—especially when caused by sudden, unpredictable events like trauma or congenital heart defects. However, a large number of cases are linked to modifiable risk factors, meaning proactive steps can dramatically reduce the risk.
Lifestyle Choices for Heart Health
- Eat a Heart-Healthy Diet: Focus on fresh vegetables, fruits, whole grains, lean proteins, and healthy fats. Minimize processed foods, excess sugar, and saturated fats.
- Stay Physically Active: Aim for at least 150 minutes of moderate exercise per week, unless restricted by your doctor. Even brisk walking supports cardiovascular health.
- Maintain a Healthy Weight: Obesity puts strain on the heart and increases the risk of arrhythmias.
- Avoid Tobacco: Smoking damages blood vessels, reduces oxygen delivery, and increases arrhythmia risk.
- Limit Alcohol and Caffeine: Excess alcohol and stimulants can trigger irregular rhythms.
Medical Prevention
- Manage High Blood Pressure & Diabetes: Both conditions increase the risk of structural heart disease and arrhythmias.
- Cholesterol Control: Keeping LDL cholesterol low helps prevent blocked arteries and heart attacks.
- Medication Compliance: If prescribed heart medications, always take them as directed. Skipping doses can destabilize heart rhythms.
- Regular Checkups: Early detection of heart disease can help prevent arrhythmia-related emergencies.
High-Risk Individuals
People with a history of heart attack, cardiomyopathy, or genetic arrhythmia syndromes may need preventive medical devices like an Implantable Cardioverter-Defibrillator (ICD). These devices monitor heart rhythm and deliver life-saving shocks if VFib or V-Tach occurs.
In short: prevention means protecting your heart health daily, and for high-risk individuals, having life-saving technology as backup.
Real-Life Examples: What Patients Experience
Understanding VFib and V-Tach becomes clearer when we look at real-world cases. These examples illustrate how quickly things can change and why awareness is crucial.
Case Example 1: VFib on the Soccer Field
A 40-year-old man with no known history of heart disease suddenly collapsed while playing soccer. Bystanders initially thought it was heat exhaustion. Thankfully, the park had an AED, which was used within 3 minutes. The shock restored his rhythm, and he survived. Later testing revealed he had undiagnosed coronary artery disease. This case highlights how VFib can strike without warning and why public AEDs are lifesaving.
Case Example 2: V-Tach in a Heart Attack Survivor
A 55-year-old woman who previously survived a heart attack started experiencing fluttering in her chest, dizziness, and fainting spells. An ECG confirmed episodes of sustained V-Tach. Doctors implanted an ICD, which later delivered shocks when dangerous arrhythmias recurred. Thanks to this device, she avoided sudden cardiac death.
Case Example 3: Nonsustained V-Tach
A 25-year-old man experienced brief episodes of rapid heartbeats lasting less than 10 seconds. While initially harmless, testing revealed hypertrophic cardiomyopathy, a genetic condition that can cause sudden cardiac arrest. Preventive therapy and lifestyle adjustments greatly lowered his risk.
These cases show us that VFib and V-Tach are not just “medical terms”—they are real, life-changing conditions. Recognition, rapid response, and modern treatments save lives every day.
The Importance of AEDs and CPR in Saving Lives
One of the biggest breakthroughs in fighting sudden cardiac death is the Automated External Defibrillator (AED). These portable devices are now commonly found in airports, malls, schools, gyms, and workplaces.
How AEDs Work
- Designed for anyone to use, even without medical training.
- Provide voice instructions guiding rescuers step by step.
- Analyze the heart rhythm automatically to determine if a shock is needed.
- Deliver a controlled shock to restore normal rhythm.
Why Every Minute Matters
- In VFib, survival chances drop by 7–10% for every minute without defibrillation.
- If CPR is started immediately and an AED is used within 3–5 minutes, survival rates can reach 50–70%.
- Without intervention, survival drops to less than 5%.
CPR: The Bridge to Defibrillation
CPR is not a cure for VFib or V-Tach, but it buys critical time by keeping blood flowing to the brain until a defibrillator is available. Everyone—teenagers, parents, employees—should learn CPR. It’s a skill that can literally double or triple survival chances.
Lifestyle Tips for Long-Term Heart Health
For people with arrhythmias—or those at risk—adopting heart-protective habits can reduce recurrence and improve quality of life.
Daily Habits
- Balanced Diet: Include potassium- and magnesium-rich foods (bananas, spinach, nuts) to support stable heart rhythms.
- Stress Management: Chronic stress and anxiety can trigger arrhythmias. Try meditation, yoga, or deep breathing exercises.
- Sleep Hygiene: Poor sleep and sleep apnea are linked to arrhythmias. Aim for 7–9 hours of quality rest.
- Regular Exercise: Walking, swimming, or cycling strengthens the heart. Avoid excessive or extreme workouts unless cleared by a doctor.
- Moderate Alcohol: Heavy drinking is linked to “holiday heart syndrome,” where binge drinking triggers arrhythmias.
For Patients With ICDs or Past Arrhythmias
- Always carry medical identification noting your device or history.
- Avoid environments with strong electromagnetic interference (like industrial equipment) that could disrupt ICDs.
- Keep up with regular follow-ups for device checks and medication adjustments.
By combining medical care with healthy living, many patients not only survive VFib or V-Tach but also thrive with fulfilling lives.
Conclusion: VFib vs. V-Tach—Different Paths, Same Urgency
VFib and V-Tach may sound like medical jargon, but they represent some of the most serious threats to heart health.
- VFib is chaotic, immediately fatal without defibrillation.
- V-Tach can sometimes be stable, but sustained episodes can deteriorate into VFib.
Both require urgent recognition, fast action, and ongoing management. Thanks to modern medicine—ICDs, catheter ablation, AEDs in public spaces, and advanced medications—survival rates are higher today than ever before.
If you or someone you love has risk factors like heart disease, fainting spells, or unexplained palpitations, take it seriously. Get evaluated by a cardiologist, follow medical advice, and embrace a heart-healthy lifestyle.
When it comes to VFib and V-Tach, knowledge truly is power—power that can save lives.
FAQs About VFib and V-Tach
1. Can stress trigger VFib or V-Tach?
Yes. Stress increases adrenaline levels, which can trigger arrhythmias in susceptible individuals. Managing stress through relaxation techniques helps lower the risk.
2. What’s the difference between an ICD and a pacemaker?
A pacemaker regulates slow heart rhythms, while an ICD detects dangerous fast rhythms (like VFib and V-Tach) and delivers shocks to restore normal rhythm.
3. Can caffeine cause V-Tach or VFib?
In most healthy people, moderate caffeine intake is safe. However, in individuals with existing heart conditions, excessive caffeine may trigger arrhythmias.
4. Is V-Tach always fatal?
Not always. Short, nonsustained episodes may resolve on their own. But sustained V-Tach is dangerous and can lead to VFib if untreated.
5. Can exercise help prevent arrhythmias?
Yes, regular moderate exercise strengthens the heart and lowers risk. However, patients with diagnosed arrhythmias should follow exercise recommendations from their cardiologist.
Medically Reviewed by Prof. Dr. Akram
Orthopedic Surgeon | Professor | Senior Medical Specialist
Prof. Dr. Akram is a distinguished surgeon with over 15 years of clinical expertise. Having served as a lead Emergency Specialist at Complex International Government Hospital, he currently leads a specialized team of 13 medical professionals at his private hospital. As a Professor at top medical universities, he ensures that every article on WellHealthOrg.com meets rigorous clinical standards.
Medical Disclaimer:
The information provided is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician for any medical concerns.
Our content is rigorously fact-checked by our 13-member Editorial Team under the clinical supervision of Prof. Dr. Akram.




![Top 10 Low-Calorie Summer Foods to Shrink Your Waistline [2026 Guide] 7 low-calorie summer foods](https://wellhealthorg.com/wp-content/uploads/2026/05/low-calorie-summer-foods-1-145x100.webp)

![Intermittent Fasting in 45°C: Success Tips [Latest 2026 Guide] 9 Intermittent Fasting in 45°C](https://wellhealthorg.com/wp-content/uploads/2026/05/Intermittent-Fasting-in-45°C-145x100.webp)