Medically Verified by Prof. Dr. Akram | Chief Medical Content Strategist & Senior Neurologist | Status: Online
The Golden Hour: A Tale of Two Emergencies
It was exactly 2:14 PM on a blistering July afternoon when the emergency department doors blew open. Paramedics wheeled in two different patients, separated by minutes, both collapsing at a local summer festival. Patient A was a 58-year-old male, clutching his chest, his skin pale and slick with a cold sweat. Patient B was a 22-year-old marathon runner, incoherent, combative, his skin radiating heat like an open oven, completely dry. As the attending physician, I had seconds to direct my trauma teams. One patient’s heart was suffocating from a blocked artery; the other’s brain was boiling in its own skull.
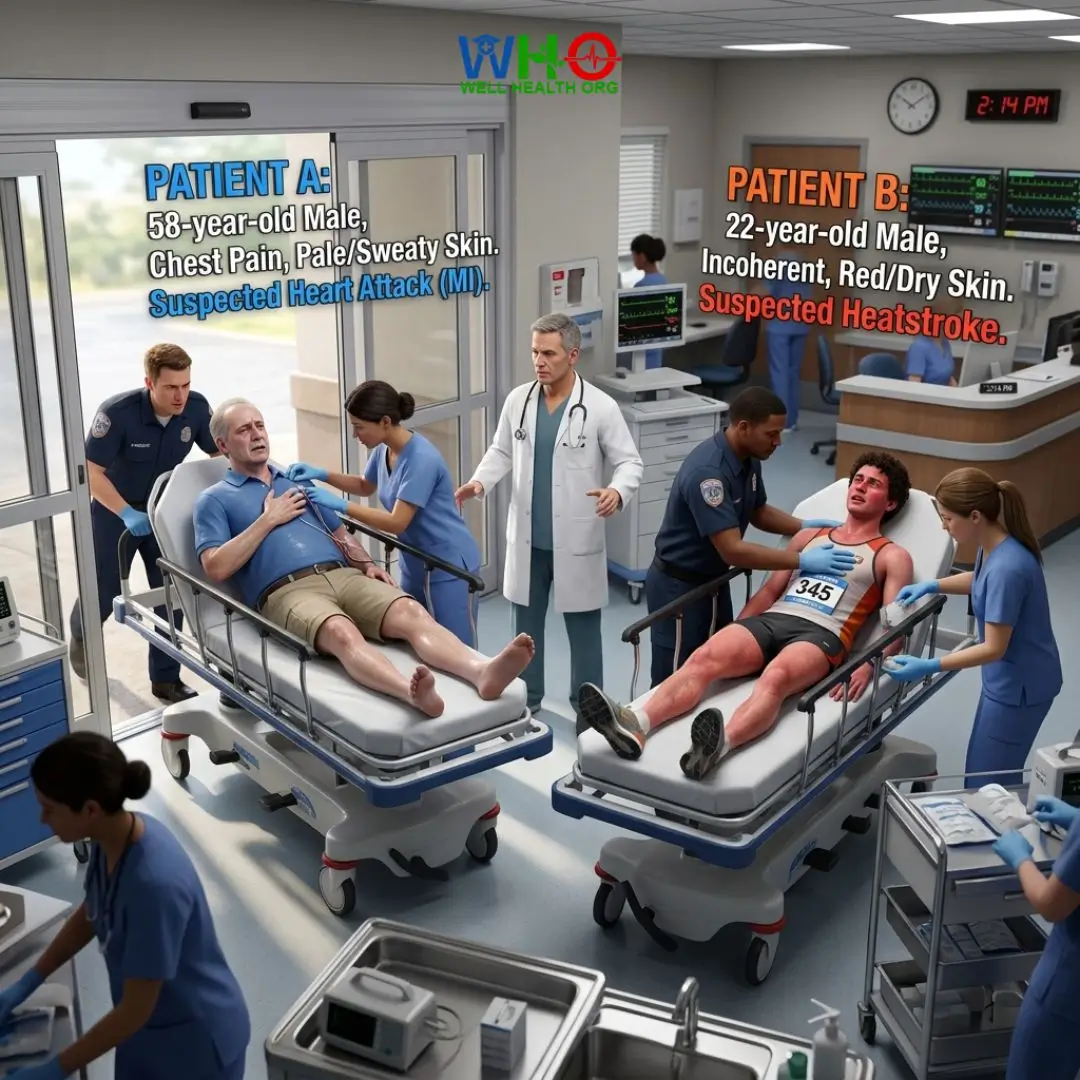
Understanding Heatstroke vs. Heart Attack: How to Tell the Difference in an Emergency can mean the line between a full recovery and irreversible cellular death. In the chaos of a collapse, bystanders often freeze, misinterpreting the body’s warning signals. Both conditions represent catastrophic failures of the human machine, but their immediate treatments are diametrically opposed. Wrap a heart attack patient in ice, and you might induce fatal arrhythmias. Wait to cool a heatstroke patient, and brain death begins in minutes.
💡 Shareable Insight: “A heart attack starves the pump; a heatstroke boils the processor. Know the difference, save a life.”
As a neurologist with over three decades of acute trauma and stroke management, I have witnessed the devastating neurological deficits left behind by delayed interventions. We are going to strip away the medical jargon. We will examine the exact biological triggers, the visual triage signs, and the uncompromising emergency protocols required to stabilize the human body when it stands on the precipice of death.
Interactive Clinical Index
The Pathophysiology of Heatstroke: Cellular Meltdown
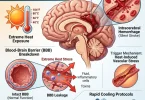
Heatstroke is not merely “being too hot.” It is a profound, life-threatening failure of the hypothalamus—the brain’s internal thermostat. When a patient is exposed to extreme environmental heat or generates massive internal heat through severe exertion, the body attempts to cool itself via vasodilation (sending blood to the skin) and diaphoresis (sweating).
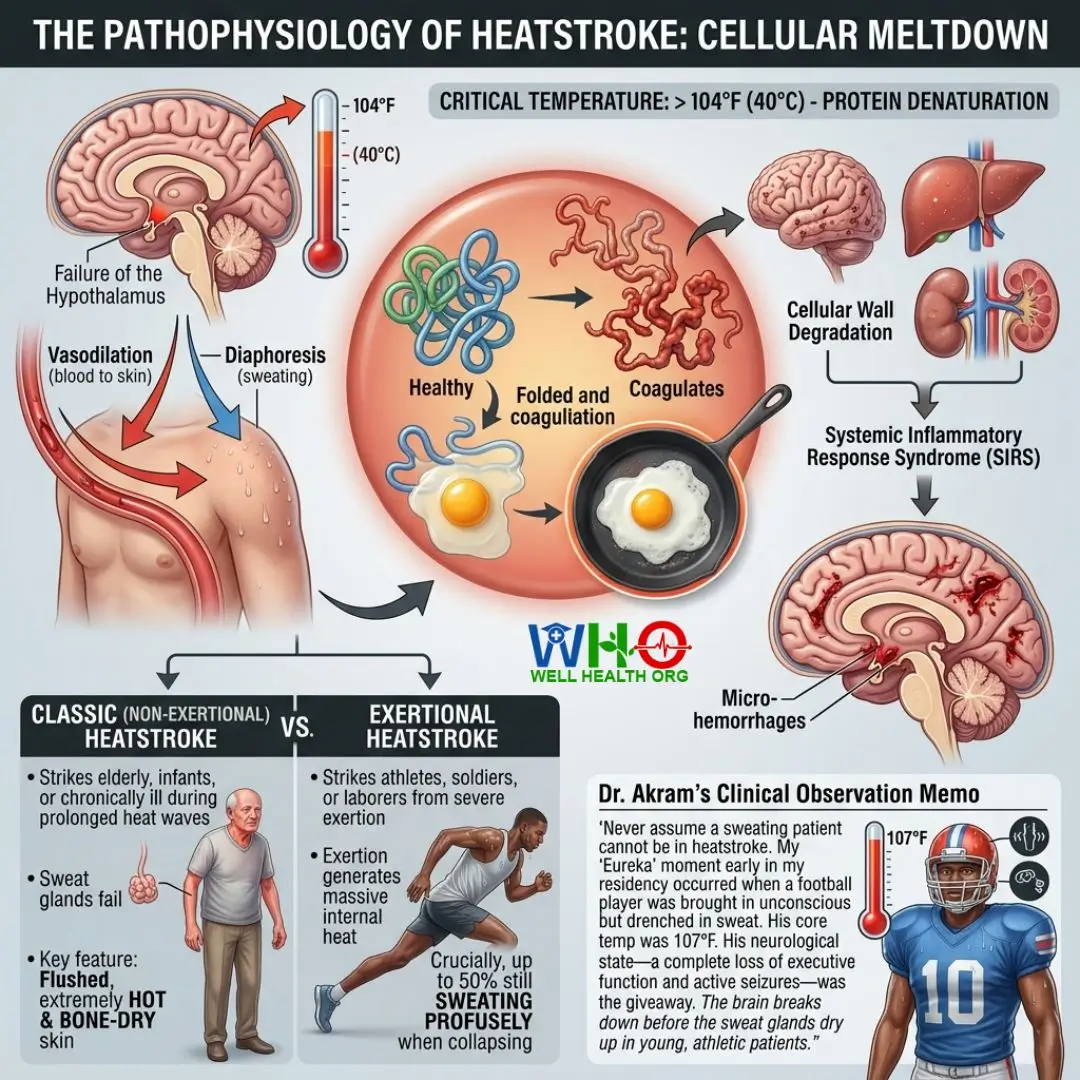
When these compensatory mechanisms fail, the core body temperature rockets past 104°F (40°C). At this precise temperature threshold, the molecular structure of human proteins begins to denature. Picture dropping a raw egg into a hot frying pan; the clear albumin turns irreversibly white and solid. A similar structural degradation happens to the cellular walls in the brain, liver, and kidneys. This triggers a systemic inflammatory response syndrome (SIRS), leading to micro-hemorrhages throughout the neurological architecture.
Classic vs. Exertional Heatstroke
To accurately discern Heatstroke vs. Heart Attack: How to Tell the Difference in an Emergency, we must split heatstroke into its two primary clinical variants:
- Classic (Non-exertional) Heatstroke: Typically strikes the elderly, infants, or the chronically ill during prolonged heat waves. Their sweat glands simply fail. The hallmark is deeply flushed, extremely hot, and bone-dry skin.
- Exertional Heatstroke: Strikes athletes, soldiers, or laborers. The body generates heat faster than sweat can evaporate it. Crucially, up to 50% of exertional heatstroke victims are still sweating profusely when they collapse. Their skin will be hot and wet, which confuses first responders.
Dr. Akram’s Clinical Observation Memo
“Never assume a sweating patient cannot be in heatstroke. My ‘Eureka’ moment early in my residency occurred when a football player was brought in unconscious but drenched in sweat. His core temp was 107°F. His neurological state—a complete loss of executive function and active seizures—was the giveaway. The brain breaks down before the sweat glands dry up in young, athletic patients.”
The Mechanics of Myocardial Infarction: The Starving Muscle
If heatstroke is an issue of hyperthermic toxicity, a heart attack (Myocardial Infarction) is an issue of plumbing and oxygen starvation. The human heart operates via an intricate network of coronary arteries. Over decades, cholesterol, calcium, and inflammatory cells form atherosclerotic plaques along the intimal walls of these arteries.

A heart attack occurs when one of these unstable plaques ruptures. The body, perceiving a microscopic tear in the blood vessel, sends platelets to clot the area. This clot (thrombus) grows in seconds, entirely occluding the vessel. Blood flow stops. The cardiac tissue downstream from the blockage immediately begins to die from ischemia (lack of oxygen). This cellular death releases lactic acid and biochemical markers (like Troponin) into the bloodstream, triggering intense nerve fibers.
Referred Pain and Autonomic Shock
Unlike the brain, the heart does not have localized pain receptors that can pinpoint exact damage. Instead, the pain signals travel up the spinal cord and cross wires with nerves feeding the chest wall, the left arm, the jaw, and the back. This is why a heart attack manifests as heavy, squeezing pressure—often described as “an elephant sitting on the chest”—rather than a sharp internal stab.
Simultaneously, the shock of a failing heart triggers the sympathetic nervous system (the fight-or-flight response). This dumps massive amounts of adrenaline into the blood, causing the peripheral blood vessels to constrict tightly. Blood is drawn away from the skin to protect the core organs. This leaves the patient’s skin looking pale, ashen, and feeling cold and clammy—a stark contrast to the boiling heat of a heatstroke victim.
💡 Shareable Insight: “Heatstroke sets the skin on fire; a heart attack turns it to cold ash. Your hands are your first diagnostic tool.”
The 10-Second Visual Triage: Heatstroke vs. Heart Attack
When someone collapses, you do not have time to Google symptoms. You must rely on immediate physical cues. Learning Heatstroke vs. Heart Attack: How to Tell the Difference in an Emergency requires you to become a rapid clinical observer. Here is my 10-second triage protocol.
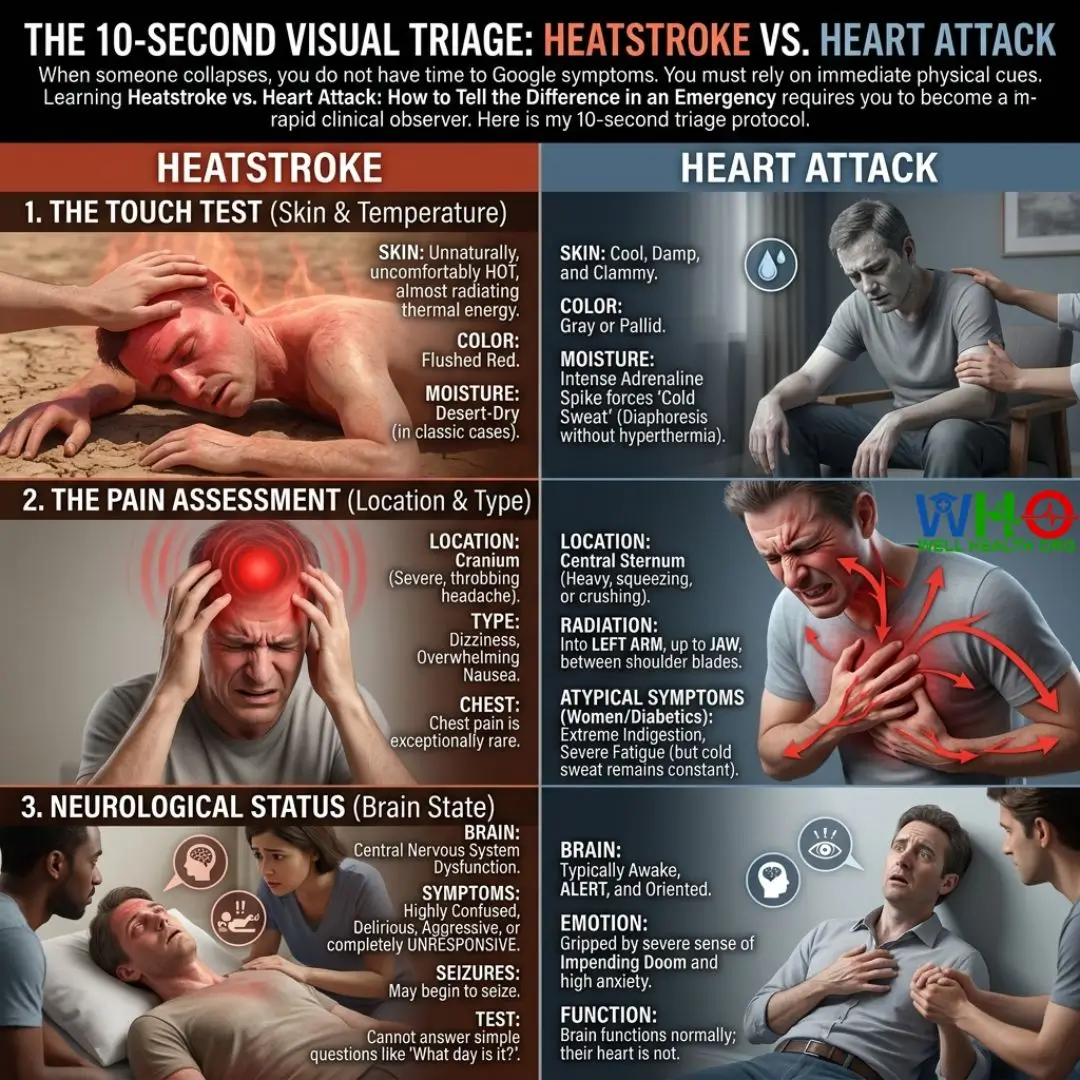
1. The Touch Test (Skin & Temperature)
- Heatstroke: Place the back of your bare hand on their forehead or chest. A heatstroke victim will feel unnaturally, uncomfortably hot, almost radiating thermal energy. The skin will often be flushed red. In classic heatstroke, it will be desert-dry.
- Heart Attack: The skin will feel cool, damp, and clammy. The intense adrenaline spike forces a “cold sweat” (diaphoresis without hyperthermia). The patient’s face may appear gray or pallid.
2. The Pain Assessment (Location & Type)
- Heatstroke: Chest pain is exceptionally rare. The patient will complain of a severe, throbbing headache, overwhelming dizziness, and profound nausea. The pain is isolated to the cranium.
- Heart Attack: The pain is centralized in the sternum. It is heavy, squeezing, or crushing. Critically, ask if the pain is radiating into the left arm, up into the jaw, or between the shoulder blades. Women and diabetics may present with atypical symptoms like extreme indigestion or severe fatigue without the crushing chest pain, but the cold sweat remains a constant.
3. Neurological Status (Brain State)
- Heatstroke: The hallmark of heatstroke is central nervous system dysfunction. The patient will be highly confused, delirious, aggressive, or completely unresponsive. They may begin to seize. They cannot answer simple questions like “What day is it?”
- Heart Attack: The patient is typically awake, completely alert, and oriented, though they will be gripped by a severe sense of impending doom and high anxiety. Their brain is functioning normally; their heart is not.
Clinical Remedial Ecosystem
Once you have answered the question of Heatstroke vs. Heart Attack: How to Tell the Difference in an Emergency, you must immediately activate the corresponding survival protocol. Below are the electronic data cards detailing the exact medical methodologies for stabilizing these life-threatening events. Read them carefully; this data dictates the mechanics of human survival.
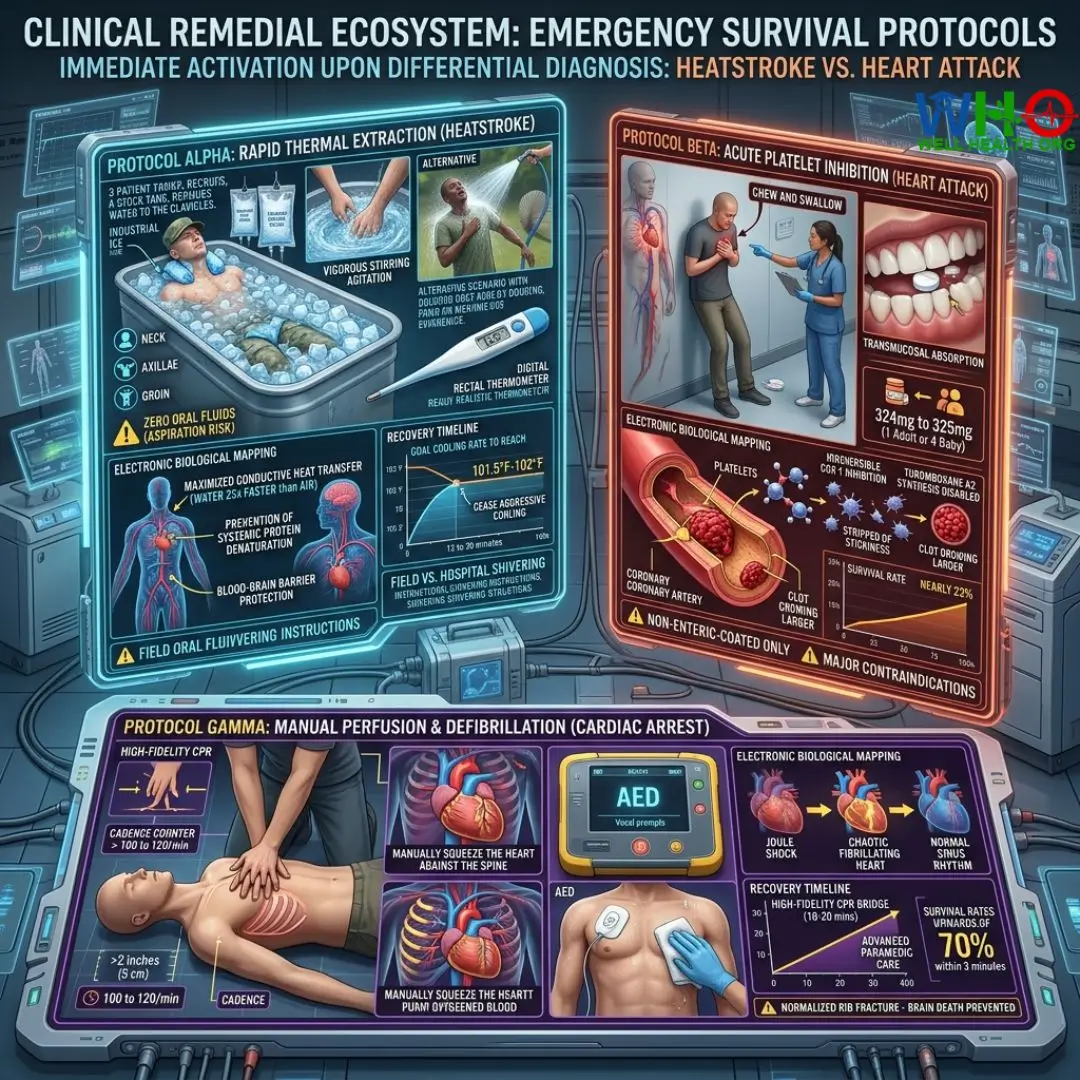
Protocol Alpha: Rapid Thermal Extraction (Heatstroke)
⚡ How to Use (Clinical Application): Immediately strip the patient of outer clothing and equipment. Submerge the patient up to the clavicles (collarbones) in a tub of ice water. If a tub is unavailable, aggressively douse the patient with water from a hose while vigorously fanning them, or apply ice packs strictly to the neck, axillae (armpits), and groin.
⚖️ Dosage & Quantity (Clinical Measurement): Water temperature should be maintained between 35°F and 59°F (2°C – 15°C). Continuously agitate (stir) the water to break the thermal boundary layer that forms around the hot skin. Provide zero oral fluids if the patient is confused or unconscious due to aspiration risks.
🔬 Mechanism of Action (Electronic Biological Mapping): Ice water immersion maximizes conductive heat transfer. Water conducts heat 25 times faster than air. Rapidly pulling thermal energy out of the vascular system prevents the denaturation of systemic proteins and halts the inflammatory cascade destroying the blood-brain barrier.
📈 Recovery Timeline (Projected Outcome): The goal is a cooling rate of 0.35°F per minute. You must lower the core body temperature to 101.5°F-102°F within 15 to 30 minutes to prevent permanent neurological deficits. Once this target is hit, cease aggressive cooling to prevent hypothermic overshoot.
🛠️ Preparation Guide (Laboratory Method): In high-risk environments (marathons, military drills), pre-stage a 100-gallon stock tank filled half with water and half with industrial ice bags. Keep a digital rectal thermometer ready, as oral and axillary temperatures are uselessly inaccurate in acute hyperthermia.
⚠️ Reaction & Bio-Safety (Emergency Protocol): The patient may begin violently shivering. Shivering generates metabolic heat, which is counterproductive. In a hospital setting, we administer intravenous benzodiazepines (like Diazepam) to paralyze the shivering response while we cool. In the field, ignore the shivering and continue aggressive cooling until EMS arrives.
Protocol Beta: Acute Platelet Inhibition (Heart Attack)
⚡ How to Use (Clinical Application): First, ensure the patient is seated safely on the floor leaning against a wall to minimize cardiac workload. Command the patient to chew and swallow the aspirin. Do not allow them to swallow it whole with water; it must be chewed to initiate rapid transmucosal absorption.
⚖️ Dosage & Quantity (Clinical Measurement): Administer exactly 324mg to 325mg. This translates to one adult regular-strength aspirin (325mg) or exactly four low-dose “baby” aspirins (81mg each).
🔬 Mechanism of Action (Electronic Biological Mapping): Aspirin is an irreversible cyclooxygenase-1 (COX-1) inhibitor. Within minutes of chewing, it enters the bloodstream and disables the synthesis of Thromboxane A2. This chemically strips platelets of their “stickiness.” It does not dissolve the existing clot blocking the coronary artery, but it absolutely prevents the clot from growing larger, buying the exact minutes needed to reach a cath lab.
📈 Recovery Timeline (Projected Outcome): Chewed aspirin begins working in the bloodstream within 4 to 5 minutes. Survival rates increase by nearly 23% when aspirin is administered pre-hospital during a myocardial infarction.
🛠️ Preparation Guide (Laboratory Method): Ensure your emergency medical kit contains non-enteric-coated aspirin. Enteric-coated aspirin is designed to dissolve slowly in the intestines, which delays the critical absorption time required during an active cardiac event.
⚠️ Reaction & Bio-Safety (Emergency Protocol): Do not administer if the patient has a known, severe anaphylactic allergy to aspirin, or if they are actively suffering from massive gastrointestinal bleeding. Ignore minor contraindications; the immediate threat to life is the dying heart muscle. Do not substitute with Ibuprofen or Acetaminophen; they do not possess the required anti-platelet properties.
Protocol Gamma: Manual Perfusion & Defibrillation (Cardiac Arrest)
⚡ How to Use (Clinical Application): If a heatstroke or heart attack patient loses consciousness and stops breathing normally (gasping does not count as breathing), immediately begin CPR. Place the heel of one hand on the center of the chest (lower half of the sternum). Interlock your other hand. Push hard and fast. If an AED is available, turn it on immediately and follow the vocal prompts.
⚖️ Dosage & Quantity (Clinical Measurement): Compress the chest to a depth of at least 2 inches (5 cm). Maintain a strict cadence of 100 to 120 compressions per minute. Allow the chest to fully recoil between compressions to allow the heart chambers to refill with blood.
🔬 Mechanism of Action (Electronic Biological Mapping): Chest compressions manually squeeze the heart between the sternum and the spine, forcing oxygenated blood out into the vascular system to keep the brain alive. An AED delivers a highly calculated joule shock to depolarize the entire cardiac electrical matrix, essentially “rebooting” a chaotically fibrillating heart back into a normal sinus rhythm.
📈 Recovery Timeline (Projected Outcome): High-fidelity CPR sustains cellular viability for 10-20 minutes, serving as a mechanical bridge until Advanced Cardiac Life Support (ACLS) paramedics arrive with epinephrine and intubation gear. Early defibrillation (within 3 minutes) yields survival rates upwards of 70%.
🛠️ Preparation Guide (Laboratory Method): Rip the patient’s shirt completely open. The skin must be bare and relatively dry for AED pad adhesion. If the patient is profusely sweating or was in a pool, rapidly wipe the chest down with a towel before applying the adhesive pads.
⚠️ Reaction & Bio-Safety (Emergency Protocol): You will likely hear ribs crack or separate from the cartilage during proper compressions. This is normal and biologically acceptable. A broken rib is a treatable injury; brain death is permanent. Do not halt compressions because of bone fractures.
Rapid Multilingual Briefings
To ensure this critical knowledge penetrates diverse communities, I have synthesized the fundamental rules of Heatstroke vs. Heart Attack: How to Tell the Difference in an Emergency into highly actionable, localized modules.
🇮🇳 Hindi Translation: Heatstroke vs Heart Attack (15-Bullet Summary)
- 1. Heatstroke (लू लगना) शरीर के तापमान के बेकाबू होने के कारण होता है।
- 2. Heart Attack (दिल का दौरा) दिल की नसों में खून के रुकने के कारण होता है।
- 3. हीटस्ट्रोक में मरीज की त्वचा बहुत गर्म, लाल और अक्सर सूखी होती है।
- 4. हार्ट अटैक में मरीज की त्वचा ठंडी, पीली और पसीने से चिपचिपी (cold sweat) होती है।
- 5. हीटस्ट्रोक में सीने में दर्द नहीं होता, बल्कि भयानक सिरदर्द और चक्कर आते हैं।
- 6. हार्ट अटैक में सीने में भारीपन या दर्द होता है जो बाएं हाथ या जबड़े तक जाता है।
- 7. हीटस्ट्रोक का मरीज मानसिक रूप से भ्रमित (confused) हो जाता है या बेहोश हो जाता है।
- 8. हार्ट अटैक का मरीज अक्सर होश में रहता है लेकिन बहुत घबराया हुआ होता है।
- 9. हीटस्ट्रोक अक्सर तेज धूप या भारी शारीरिक मेहनत के बाद होता है।
- 10. हार्ट अटैक अचानक होता है, यह आराम करते समय या ठंडी जगह पर भी हो सकता है।
- 11. हीटस्ट्रोक का इलाज: मरीज को तुरंत ठंडी जगह पर ले जाएं और शरीर पर बर्फ या ठंडा पानी डालें।
- 12. हार्ट अटैक का इलाज: मरीज को आराम से बैठाएं और एम्बुलेंस को कॉल करें।
- 13. हार्ट अटैक में अगर मरीज होश में है और उसे एलर्जी नहीं है, तो तुरंत एस्पिरिन (Aspirin) चबाने को दें।
- 14. हीटस्ट्रोक के बेहोश मरीज को कभी भी पानी या कुछ भी पीने को न दें, पानी फेफड़ों में जा सकता है।
- 15. अगर किसी भी स्थिति में मरीज की सांस रुक जाए, तो तुरंत CPR शुरू करें।
🇮🇳 Hinglish Breakdown: Heatstroke vs Heart Attack (15-Bullet Summary)
- 1. Heatstroke tab hota hai jab body apni cooling capacity kho deti hai aur temp 104°F cross kar jata hai.
- 2. Heart Attack tab hota hai jab heart ki artery block ho jati hai aur blood flow ruk jata hai.
- 3. Heatstroke mein patient ki skin aag ki tarah garam, red, aur mostly dry lagti hai.
- 4. Heart Attack mein skin thandi, pale, aur clammy (chipchipa cold sweat) feel hoti hai.
- 5. Heatstroke mein chest pain nahi hota; isme severe headache aur extreme nausea hota hai.
- 6. Heart Attack mein chest par heavy pressure feel hota hai, jaise koi weight rakha ho.
- 7. Heart attack ka pain left arm, neck, ya jaw ki taraf radiate kar sakta hai.
- 8. Heatstroke ka hallmark sign confusion hai—patient ajeeb behave karega ya faint ho jayega.
- 9. Heart attack mein patient fully awake aur alert rehta hai, par usko severe anxiety hoti hai.
- 10. Heatstroke Action: Patient ko turant shade mein le jayein aur ice water se aggressively cool karein.
- 11. Heart Attack Action: Patient ko floor par bitha dein aur movement bilkul band karwa dein.
- 12. Heart attack mein turant 325mg Aspirin chaba kar khane ko dein (agar allergy na ho).
- 13. Heatstroke mein agar patient confused hai, toh use peene ke liye kuch bhi na dein. Choking risk hai.
- 14. 10-Second Test: Skin touch karein. Garam aur sookhi = Heatstroke. Thandi aur paseene wali = Heart Attack.
- 15. Dono cases medical emergencies hain. Turant ambulance bulao aur saans rukne par CPR chalu karo.
High-Frequency Emergency FAQs
To further solidify our understanding of Heatstroke vs. Heart Attack: How to Tell the Difference in an Emergency, I have compiled 25 of the most pressing clinical questions asked by first responders, EMTs, and concerned citizens. These answers contain critical medical nuances.
1. Can extreme heat actually trigger a heart attack?
Yes. Extreme heat forces the heart to beat faster and pump harder to push blood to the skin for cooling. In individuals with pre-existing compromised coronary arteries, this intense cardiovascular workload can rupture a plaque, leading directly to a myocardial infarction. The heat is the trigger, but the event is cardiac.
2. If someone is sweating heavily, does that completely rule out heatstroke?
Absolutely not. This is a dangerous myth. Exertional heatstroke victims (athletes, laborers) often collapse while still profusely sweating because their core temperature rises faster than evaporation can handle. Always check mental status; if they are profoundly confused and burning hot, it is heatstroke, regardless of sweat.
3. Why does a heart attack cause a “cold sweat”?
A heart attack triggers a massive surge of adrenaline as a stress response. Adrenaline causes profound vasoconstriction (narrowing of blood vessels) in the skin to preserve blood for the core. This draws warmth away from the skin, while simultaneously stimulating sweat glands, resulting in a cold, clammy feeling.
4. Is it safe to put a heatstroke victim in a freezing ice bath?
Yes, it is the gold standard of care. Despite older myths about “shocking the system,” rapid cooling via ice water immersion is the scientifically proven method to rapidly lower core temperatures and save the brain from thermal destruction.
5. Should I give water to a heart attack patient?
No. A heart attack is not caused by dehydration. Giving water risks aspiration if the patient suddenly vomits or loses consciousness, which is common during severe cardiac events. The only oral intervention should be chewed aspirin.
6. How do women’s heart attack symptoms differ from men’s?
Women frequently experience atypical presentations. Instead of crushing chest pain, they may suffer from intense shortness of breath, unexplained extreme fatigue, profound nausea, or sharp pain between the shoulder blades. However, the cold sweat and sudden onset remain consistent indicators.
7. What is the difference between heat exhaustion and heatstroke?
Mental status is the divider. Heat exhaustion features heavy sweating, cramps, and weakness, but the brain functions normally. Heatstroke occurs when thermoregulation fails entirely, leading to neurological collapse—confusion, delirium, seizures, or coma. Heat exhaustion requires rest and fluids; heatstroke requires immediate emergency cooling.
8. Why must aspirin be chewed during a heart attack?
Swallowing a pill whole forces it through the slow digestive tract, taking 30-45 minutes to enter the bloodstream. Chewing breaks the pill down and allows rapid transmucosal absorption directly through the buccal capillaries in the mouth, acting on platelets within 5 minutes.
9. Can heatstroke cause permanent brain damage?
Absolutely. Temperatures above 104°F rapidly denature cellular proteins. If not cooled immediately, cerebellar damage occurs, which can lead to permanent ataxia (loss of motor coordination), cognitive deficits, or a persistent vegetative state.
10. Should I perform CPR if the patient is still breathing?
No. CPR is strictly for individuals who are unconscious and completely lack normal breathing (or only have agonal gasps). If they are breathing, their heart is still beating. Monitor them closely and be ready to start CPR if breathing stops.
11. What is silent ischemia?
Silent ischemia is a heart attack that occurs with little to no chest pain. It is incredibly common in diabetic patients whose neuropathy (nerve damage) masks the pain signals from the dying heart muscle. They may present only with sudden weakness and a cold sweat.
12. Why do we avoid oral fluids for an unconscious heatstroke victim?
An unconscious or deeply confused person lacks a reliable gag reflex. Pouring fluids into their mouth will likely result in aspiration—fluid entering the trachea and lungs—causing chemical pneumonitis, drowning, or fatal airway obstruction.
13. Is Ibuprofen effective for a heart attack?
No, it is dangerous. Ibuprofen and NSAIDs do not possess the specific rapid anti-platelet binding properties of aspirin. In fact, taking NSAIDs during a cardiac event can increase mortality by interfering with vascular healing and exacerbating hypertension.
14. What is the role of an AED in these emergencies?
An Automated External Defibrillator analyzes the heart’s rhythm. If a heart attack causes ventricular fibrillation (a chaotic, non-pumping quiver), the AED delivers a shock to reset the electrical system. It is useless for heatstroke unless the heatstroke has progressed to secondary cardiac arrest.
15. Why does heatstroke cause the skin to turn red or flushed?
The body attempts to radiate heat away from the internal organs by massively dilating the peripheral blood vessels in the skin. This flooding of superficial capillaries with hot blood turns the skin bright red, similar to a radiator dispersing engine heat.
16. Can a younger person suffer a heart attack?
Yes. While more common in older adults, heart attacks in people under 40 are rising steeply due to hyperlipidemia, obesity, undiagnosed congenital anomalies, and substance abuse (like cocaine, which induces profound coronary vasospasm).
17. Can I drive someone to the hospital for a heart attack?
It is highly discouraged. EMS vehicles are essentially rolling emergency rooms. Paramedics can administer oxygen, nitroglycerin, begin ECG tracking, and defibrillate en route. If the patient goes into cardiac arrest in your passenger seat, you cannot perform CPR while driving.
18. What temperature indicates clinical heatstroke?
A core body temperature of 104°F (40°C) or higher, coupled with central nervous system dysfunction (altered mental state), is the clinical diagnostic threshold for heatstroke.
19. Why apply ice packs to the neck, groin, and armpits specifically?
These areas house massive, superficial blood vessels (carotid, femoral, and axillary arteries). Placing ice directly over these arterial highways cools the blood rapidly as it flows back into the body’s core and up to the brain.
20. Do heart attacks always happen suddenly?
Not always. Many patients experience “stuttering” symptoms or prodromal angina (intermittent chest pressure that comes and goes) for hours, days, or even weeks before the final plaque rupture completely occludes the artery.
21. Are energy drinks safe during extreme heat?
No. Energy drinks are packed with massive amounts of caffeine, a diuretic that speeds up dehydration. Furthermore, high caffeine doses stress the cardiovascular system, increasing the risk of arrhythmias during heat stress.
22. Can a person have a heart attack without high blood pressure or cholesterol?
Yes. Stress, severe inflammation, genetic predispositions, and endothelial dysfunction can precipitate a myocardial infarction even in individuals with pristine lipid panels and normal blood pressure.
23. What happens if I misdiagnose them in the field?
If you are uncertain, activate EMS immediately. In an ambiguous collapse, check breathing and pulse. If both are present, ensure they are in a safe, cool environment and keep them completely at rest until paramedics assess vital signs via telemetry.
24. How fast does brain tissue die without oxygen?
During cardiac arrest, irreversible hypoxic brain damage begins within 4 to 6 minutes without CPR. By 10 minutes, biological death of the neurological matrix is nearly certain.
25. Can medications increase heatstroke risk?
Yes. Anticholinergics (allergy meds), beta-blockers (heart meds), and diuretics fundamentally inhibit the body’s ability to sweat or dilate blood vessels, making the patient highly susceptible to classic heatstroke during heat waves.
© 2026 Dr. Akram Medical Strategy Group. All Rights Reserved.
Medically Reviewed by Prof. Dr. Akram
Orthopedic Surgeon | Professor | Senior Medical Specialist
Prof. Dr. Akram is a distinguished surgeon with over 15 years of clinical expertise. Having served as a lead Emergency Specialist at Complex International Government Hospital, he currently leads a specialized team of 13 medical professionals at his private hospital. As a Professor at top medical universities, he ensures that every article on WellHealthOrg.com meets rigorous clinical standards.
Medical Disclaimer:
The information provided is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician for any medical concerns.
Our content is rigorously fact-checked by our 13-member Editorial Team under the clinical supervision of Prof. Dr. Akram.


![Best Ayurvedic Summer Drinks for Belly Fat Loss [Updated for 2026] 8 Drinks for Belly Fat Loss](https://wellhealthorg.com/wp-content/uploads/2026/05/Drinks-for-Belly-Fat-Loss-145x100.webp)
![7-Day Summer Fat Burn: How to Lose 5kg Fast [Latest 2026 Guide] 10 7-Day Summer Fat Burn](https://wellhealthorg.com/wp-content/uploads/2026/05/7-Day-Summer-Fat-Burn-145x100.webp)


