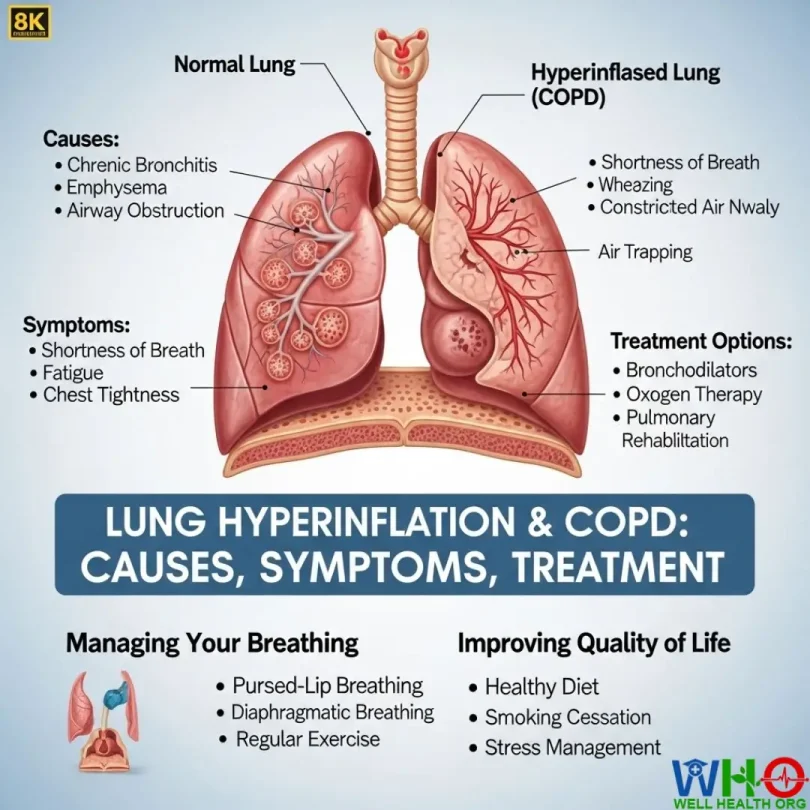
Lung Hyperinflation and COPD
Chronic obstructive pulmonary disease (COPD) is one of the most challenging respiratory conditions, affecting millions of people worldwide. According to the American Lung Association, COPD ranks as the third leading cause of death in the United States, impacting more than 16 million Americans directly and many more indirectly through undiagnosed cases. One of the most significant complications that worsens the daily struggle of COPD patients is lung hyperinflation—a condition where air becomes trapped inside the lungs, causing them to expand beyond their normal size.
- Lung Hyperinflation and COPD
- Understanding COPD: The Root Cause of Hyperinflated Lungs
- What Exactly is COPD?
- The Two Main Types of COPD
- How COPD Leads to Hyperinflated Lungs
- What is Lung Hyperinflation? A Closer Look
- Defining Lung Hyperinflation
- Types of Lung Hyperinflation
- Why Hyperinflation is So Harmful
- Causes and Risk Factors: Why Does Lung Hyperinflation Happen?
- 1. Smoking
- 2. Environmental Exposure
- 3. Genetic Factors
- 4. Aging and Lung Health
- Symptoms of Lung Hyperinflation in COPD Patients
- 1. Shortness of Breath (Dyspnea)
- 2. Decreased Exercise Tolerance
- 3. Barrel Chest Appearance
- 4. Fatigue and Low Energy
- 5. Heart-Related Complications
- Diagnosis and Evaluation: How Doctors Detect Hyperinflated Lungs
- 1. Physical Examination
- 2. Imaging Tests
- 3. Pulmonary Function Tests (PFTs)
- 4. Echocardiogram (if needed)
- Treatment Options: How to Manage Lung Hyperinflation in COPD
- 1. Medications
- Bronchodilators
- Inhaled Corticosteroids
- Oxygen Therapy
- 2. Breathing Therapies
- Pursed-Lip Breathing
- Diaphragmatic Breathing
- 3. Pulmonary Rehabilitation
- 4. Lifestyle Modifications
- Quit Smoking Immediately
- Stay Physically Active
- Maintain a Balanced Diet
- 5. Surgical Options for Severe Cases
- Lung Volume Reduction Surgery (LVRS)
- Bullectomy
- Lung Transplant
- The Role of Pulmonary Rehabilitation: More Than Just Exercise
- Why Pulmonary Rehabilitation is Essential
- Core Components of a Rehab Program
- Prevention Strategies: How to Protect Your Lungs and Slow Disease Progression
- 1. Avoid Smoking and Secondhand Smoke
- 2. Limit Exposure to Lung Irritants
- 3. Stay Up-to-Date with Vaccinations
- 4. Regular Medical Checkups
- 5. Maintain a Healthy Lifestyle
- Living with COPD and Lung Hyperinflation: Daily Challenges and Coping Strategies
- Common Daily Struggles
- Coping Strategies
- The Connection Between Lung Hyperinflation and Heart Health
- How Hyperinflation Affects the Heart
- Real-Life Consequences
- The Emotional and Psychological Impact
- Anxiety and Breathlessness: A Vicious Cycle
- Depression and Social Isolation
- Strategies to Manage Emotional Health
- Diet and Nutrition: Fueling Your Lungs and Body
- Nutrients That Support Lung Function
- Foods to Embrace
- Foods to Limit or Avoid
- Practical Eating Tips
- Exercise and Physical Activity: Moving with Confidence
- Why Exercise Matters
- Best Exercises for COPD and Hyperinflation
- Exercise Safety Tips
- Future Outlook: Advances in COPD and Hyperinflation Treatment
- Emerging Treatments
- Digital Health Tools
- Patient Empowerment and Education
- Taking Control of Your Breathing: Living Well with COPD and Lung Hyperinflation
- FAQs About COPD and Lung Hyperinflation
- 1. Is lung hyperinflation reversible?
- 2. Can exercise make lung hyperinflation worse?
- 3. How can I tell if my lungs are hyperinflated?
- 4. Will quitting smoking help if I already have lung hyperinflation?
- 5. What’s the outlook for someone with COPD and hyperinflation?
- Final Thoughts
While COPD itself is already a difficult disease to live with, hyperinflation adds another layer of discomfort, making breathing even more exhausting. If you’ve ever felt like no matter how deeply you inhale, you can’t get enough air, you may already have experienced what lung hyperinflation feels like.
In this comprehensive guide, we’ll explore the relationship between COPD and lung hyperinflation, diving into their causes, symptoms, diagnosis, and treatment. We’ll also provide practical tips to help you manage your condition, prevent further complications, and maintain a better quality of life.
Understanding COPD: The Root Cause of Hyperinflated Lungs
To fully grasp what lung hyperinflation is, it’s important to first understand COPD itself.
What Exactly is COPD?
Chronic obstructive pulmonary disease (COPD) is a long-term, progressive lung condition that causes airflow blockage and breathing difficulties. Unlike temporary breathing problems caused by a cold or infection, COPD gradually worsens over time, damaging both the airways and the tiny air sacs in the lungs known as alveoli.
When alveoli are damaged, the lungs lose their natural elasticity. This means they can no longer expand and contract efficiently, making it harder to move air in and out. As a result, oxygen struggles to reach your bloodstream, and carbon dioxide removal becomes impaired.
The inflammation caused by COPD also leads to excess mucus production, which clogs the airways further and contributes to chronic coughing and wheezing.
The Two Main Types of COPD
COPD isn’t just one disease—it’s usually a combination of two main conditions:
- Chronic Bronchitis
- This condition is marked by long-term inflammation of the bronchial tubes—the airways that carry air to and from the lungs.
- People with chronic bronchitis often suffer from a persistent cough with thick mucus that lasts for months or even years.
- Over time, the constant irritation narrows the airways, making breathing progressively harder.
- Emphysema
- In emphysema, the delicate alveoli become damaged, stretched, and eventually destroyed.
- Instead of having many small air sacs that provide a large surface area for oxygen exchange, the alveoli merge into larger, less efficient air spaces.
- This reduces the overall lung capacity, limiting how much oxygen can reach the bloodstream.
Many patients suffer from a combination of both conditions, which accelerates lung function decline.
How COPD Leads to Hyperinflated Lungs
The structural damage caused by COPD sets the stage for hyperinflation. When airways are narrowed and alveoli lose their elasticity, the lungs cannot empty fully during exhalation. Instead, air remains trapped inside. Over time, with every breath, more air accumulates—leading to lungs that are over-expanded and unable to function normally.
This is why people with COPD often feel like they are “breathing through a straw”—the lungs are working hard, but airflow remains restricted, and oxygen exchange is compromised.
What is Lung Hyperinflation? A Closer Look
Now that we’ve established the connection between COPD and lung damage, let’s break down what lung hyperinflation really means.
Defining Lung Hyperinflation
Lung hyperinflation—sometimes called pulmonary hyperinflation—occurs when air gets stuck in the lungs, causing them to expand beyond their normal capacity. This makes it harder to take in fresh oxygen with each breath, creating a cycle of shortness of breath and fatigue.
In simple terms, hyperinflated lungs act like a balloon that’s already half-full of air—no matter how hard you try, there’s little room left to inflate it further.
Types of Lung Hyperinflation
Doctors typically classify hyperinflation into two categories:
- Static Hyperinflation
- Occurs when air remains trapped inside the lungs even at rest after a full exhalation.
- The lungs stay partially expanded all the time, reducing space for fresh air.
- Dynamic Hyperinflation
- Happens during physical activity when you inhale again before completely exhaling.
- This is particularly challenging because exercise naturally increases your breathing rate, leaving even less time to expel trapped air.
Both types significantly reduce the efficiency of the lungs and place extra strain on the heart and respiratory muscles.
Why Hyperinflation is So Harmful
The effects of hyperinflated lungs go beyond difficulty breathing:
- Reduced Oxygen Intake: Trapped air means less room for fresh oxygen.
- Increased Heart Strain: The over-expansion of lungs puts pressure on the heart, especially the left ventricle, impairing blood circulation.
- Muscle Fatigue: The body uses much more energy just to breathe, leaving patients feeling exhausted.
- Limited Activity: Even simple tasks like walking or climbing stairs can feel overwhelming.
Causes and Risk Factors: Why Does Lung Hyperinflation Happen?
Lung hyperinflation doesn’t happen in isolation. It’s almost always a consequence of underlying COPD. Let’s look at the main factors that contribute to both conditions.
1. Smoking
- The leading cause of COPD worldwide is cigarette smoking.
- Cigarette smoke contains thousands of toxic chemicals, many of which directly destroy alveolar walls and irritate airways.
- Even long after quitting, some of the lung damage may remain permanent, highlighting the importance of early smoking cessation.
2. Environmental Exposure
- Long-term exposure to air pollution, dust, fumes, or workplace chemicals can also damage the lungs.
- Occupations in mining, construction, or textile industries often report higher COPD cases due to constant inhalation of irritants.
- Secondhand smoke is another hidden risk—non-smokers living with smokers can also develop COPD over time.
3. Genetic Factors
- A rare but serious genetic condition called alpha-1-antitrypsin deficiency can make individuals more prone to COPD.
- This protein normally protects lung tissue from damage. Without enough of it, lungs become highly vulnerable—even in non-smokers.
4. Aging and Lung Health
- As we age, our lungs naturally lose some elasticity.
- For people exposed to smoking or pollutants, aging accelerates lung function decline, making hyperinflation more likely.
Symptoms of Lung Hyperinflation in COPD Patients
One of the challenges with lung hyperinflation is that its symptoms often overlap with those of COPD, making it harder to detect early. However, recognizing these signs can make a big difference in getting timely treatment.
1. Shortness of Breath (Dyspnea)
- The most common symptom, often described as “air hunger.”
- Patients feel as though they cannot take a full breath, even while resting.
- Activities like walking uphill, climbing stairs, or even talking for long periods become exhausting.
2. Decreased Exercise Tolerance
- Physical activity feels harder because the lungs cannot keep up with increased oxygen demand.
- According to clinical studies, up to 70% of severe COPD patients develop lung hyperinflation, significantly limiting their ability to stay active.
3. Barrel Chest Appearance
- Over time, chronically overinflated lungs push the rib cage outward, giving the chest a rounded, barrel-like shape.
- This physical change is often visible and can serve as a clinical indicator of long-standing hyperinflation.
4. Fatigue and Low Energy
- Because breathing itself becomes energy-intensive, patients feel tired even after mild exertion.
- Low oxygen circulation further contributes to ongoing fatigue.
5. Heart-Related Complications
- The pressure from enlarged lungs can squeeze the heart, particularly the left ventricle.
- This strain may weaken the heart’s pumping ability, leading to secondary cardiovascular problems such as arrhythmias or heart failure.
Diagnosis and Evaluation: How Doctors Detect Hyperinflated Lungs
If you suspect that your COPD symptoms are worsening due to hyperinflation, seeking medical evaluation is crucial. Doctors use several methods to confirm the diagnosis.
1. Physical Examination
- A physician listens to the lungs with a stethoscope, often detecting reduced breath sounds or prolonged exhalation.
- They may also look for physical signs such as barrel chest or use an oximeter to measure blood oxygen levels.
2. Imaging Tests
- Chest X-rays can show over-expanded lungs and a flattened diaphragm.
- CT scans provide a more detailed view, allowing doctors to see the extent of lung damage and air trapping.
3. Pulmonary Function Tests (PFTs)
- One of the most important diagnostic tools.
- Measures lung volume, airflow, and residual air left after exhalation.
- Helps determine whether hyperinflation is static or dynamic.
4. Echocardiogram (if needed)
- Since hyperinflated lungs can affect the heart, an echocardiogram may be performed to check for ventricular strain or reduced pumping efficiency.
Treatment Options: How to Manage Lung Hyperinflation in COPD
While there is no cure for COPD or lung hyperinflation, a wide range of treatments can help manage symptoms, improve breathing efficiency, and enhance quality of life. Treatment usually focuses on controlling COPD progression and easing the strain caused by hyperinflated lungs.
1. Medications
Medications play a central role in COPD management. They help open airways, reduce inflammation, and relieve symptoms like shortness of breath.
Bronchodilators
- These are the most commonly prescribed drugs for COPD-related hyperinflation.
- They work by relaxing the muscles around the airways, making it easier to exhale trapped air.
- According to the American Thoracic Society, bronchodilators can improve lung function by up to 15%, providing noticeable relief.
- Types include:
- Short-acting bronchodilators: Provide quick relief during sudden breathlessness.
- Long-acting bronchodilators: Taken daily to maintain consistent airway opening.
Inhaled Corticosteroids
- These reduce airway inflammation, decreasing mucus buildup and irritation.
- Often prescribed in combination with bronchodilators for patients with frequent flare-ups.
Oxygen Therapy
- For patients with low blood oxygen levels, supplemental oxygen can make a dramatic difference.
- Oxygen therapy not only improves breathing but also reduces strain on the heart, preventing further complications.
2. Breathing Therapies
Simple yet effective breathing strategies can help patients gain more control over their lung function.
Pursed-Lip Breathing
- A proven technique to slow down breathing and release trapped air.
- The method: inhale slowly through your nose, then exhale gently through pursed lips (like whistling).
- Benefits include reducing dynamic hyperinflation, calming the body, and improving oxygen intake.
Diaphragmatic Breathing
- Also called “belly breathing,” this exercise strengthens the diaphragm, the main breathing muscle.
- By focusing on expanding the belly rather than the chest, patients maximize air exchange and reduce shallow breathing patterns.
3. Pulmonary Rehabilitation
Pulmonary rehabilitation is one of the most effective treatments for COPD with hyperinflation. These programs are designed to improve overall lung health and patient well-being.
A typical rehab program includes:
- Exercise Training: Builds endurance and strengthens muscles, including those used for breathing.
- Nutritional Counseling: Helps patients maintain a healthy weight—important since both underweight and overweight conditions can worsen symptoms.
- Disease Education: Teaches patients how to manage medications, avoid triggers, and recognize early warning signs of flare-ups.
- Support and Counseling: Addresses the emotional burden of living with a chronic illness.
According to the COPD Foundation, pulmonary rehabilitation can improve quality of life by up to 50%, helping patients remain independent for longer.
4. Lifestyle Modifications
Even the best medical treatments can only go so far without lifestyle changes. Patients who take proactive steps often see the most significant improvements.
Quit Smoking Immediately
- Smoking is the leading cause of COPD and worsens hyperinflation.
- Studies confirm that quitting smoking at any stage slows disease progression significantly.
Stay Physically Active
- Gentle exercises like walking, yoga, or water aerobics help maintain stamina and strengthen respiratory muscles.
- Physical activity also improves circulation, boosts mood, and prevents further deconditioning.
Maintain a Balanced Diet
- Foods rich in antioxidants (fruits, vegetables, whole grains) protect lung tissue from further damage.
- Adequate protein intake supports muscle strength, including breathing muscles.
- Staying hydrated thins mucus, making it easier to clear airways.
5. Surgical Options for Severe Cases
For patients with advanced COPD and extreme hyperinflation, surgery may be considered.
Lung Volume Reduction Surgery (LVRS)
- Surgeons remove up to 30% of diseased lung tissue, allowing the healthier portions of the lungs to expand more efficiently.
- This can reduce hyperinflation, ease pressure on the heart, and improve breathing capacity.
Bullectomy
- In cases of severe emphysema, giant air-filled sacs called bullae may form, occupying space in the chest cavity.
- Removing these bullae creates more room for the remaining lung tissue to function properly.
Lung Transplant
- For end-stage COPD, a lung transplant may be the only viable option.
- While risky, it can significantly improve survival and quality of life in carefully selected patients.
The Role of Pulmonary Rehabilitation: More Than Just Exercise
Pulmonary rehabilitation deserves special attention because it provides far more than just physical training. It’s a comprehensive, holistic program tailored to the unique needs of COPD patients.
Why Pulmonary Rehabilitation is Essential
- Reduces Breathlessness: Teaches breathing control strategies that reduce the feeling of suffocation.
- Boosts Confidence: Many patients fear exercise, worrying it may worsen symptoms. Rehab provides a safe, supervised environment to build trust in their own abilities.
- Improves Emotional Well-being: Living with COPD can lead to anxiety and depression. Rehab programs include mental health support to ease this burden.
- Enhances Longevity: Studies show that patients who regularly attend rehab programs experience fewer hospitalizations and flare-ups.
Core Components of a Rehab Program
- Structured Exercise Training
- Includes treadmill walking, stationary cycling, and resistance training.
- Focuses on improving both cardiovascular endurance and muscle strength.
- Nutritional Guidance
- Patients struggling with weight loss due to COPD may need higher-calorie, nutrient-dense foods.
- Those who are overweight benefit from a balanced plan to reduce excess weight and ease breathing.
- Education and Self-Management
- Patients learn how to take medications properly, handle oxygen therapy equipment, and spot early warning signs of exacerbations.
- Breathing Retraining
- Techniques such as pursed-lip and diaphragmatic breathing are taught and practiced regularly.
Prevention Strategies: How to Protect Your Lungs and Slow Disease Progression
While COPD and hyperinflation cannot be cured, certain preventive strategies can slow down progression and reduce complications.
1. Avoid Smoking and Secondhand Smoke
- The single most important step in prevention.
- If you smoke, seek professional help—nicotine replacement therapy, prescription medications, and counseling can greatly increase success rates.
2. Limit Exposure to Lung Irritants
- Wear protective masks if you work in dusty or chemical-heavy environments.
- Use air purifiers at home if exposed to pollution.
3. Stay Up-to-Date with Vaccinations
- Flu and pneumonia vaccines are essential for COPD patients.
- Respiratory infections can quickly escalate into dangerous flare-ups in hyperinflated lungs.
4. Regular Medical Checkups
- Frequent visits to your pulmonologist help monitor disease progression.
- Early intervention in flare-ups prevents long-term damage.
5. Maintain a Healthy Lifestyle
- A diet rich in fresh fruits, vegetables, and lean proteins keeps the immune system strong.
- Regular, moderate exercise prevents muscle loss and improves circulation.
Living with COPD and Lung Hyperinflation: Daily Challenges and Coping Strategies
Living with COPD and hyperinflated lungs is a daily balancing act—patients must constantly monitor their breathing, activity levels, and environment. But with the right approach, it’s possible to live a fulfilling and independent life.
Common Daily Struggles
- Breathlessness with Simple Tasks: Even dressing, cooking, or showering can leave patients breathless.
- Sleep Difficulties: Lying down may worsen shortness of breath due to pressure on the diaphragm.
- Emotional Stress: Anxiety and depression are common, as the fear of flare-ups looms large.
Coping Strategies
- Energy Conservation Techniques
- Break tasks into smaller steps.
- Sit while cooking or showering to conserve energy.
- Use assistive devices like shower chairs or reach tools.
- Home Adjustments
- Keep essential items within easy reach.
- Install handrails in bathrooms and hallways.
- Ensure proper ventilation and avoid exposure to smoke or strong fumes.
- Breathing Exercises Throughout the Day
- Incorporating pursed-lip breathing during chores or physical activity helps maintain oxygen flow.
- Emotional Support
- Joining COPD support groups can provide encouragement and reduce feelings of isolation.
- Counseling or therapy may be beneficial for those struggling with depression or anxiety.
The Connection Between Lung Hyperinflation and Heart Health
When we think about COPD and hyperinflated lungs, we often focus only on the respiratory system. However, the condition has a significant impact on the cardiovascular system as well. The constant pressure from overexpanded lungs can affect the heart’s ability to pump effectively.
How Hyperinflation Affects the Heart
- Pressure on the Left Ventricle: As lungs expand beyond their normal size, they press against the heart—especially the left ventricle. This chamber is responsible for pumping oxygen-rich blood throughout the body. Compression reduces its efficiency, leading to reduced circulation.
- Right Heart Strain: COPD and hyperinflation often cause low oxygen levels, which increase pressure in the lung’s blood vessels. This forces the right side of the heart to work harder, sometimes leading to a condition called pulmonary hypertension.
- Increased Risk of Arrhythmias: Oxygen deprivation and structural changes in the chest can disrupt the heart’s electrical activity, increasing the risk of irregular heart rhythms.
Real-Life Consequences
Patients often report:
- Feeling faint or dizzy due to poor circulation.
- Swelling in ankles or feet (a sign of right-sided heart strain).
- Increased fatigue beyond what can be explained by breathing problems alone.
This link between hyperinflated lungs and heart health highlights the importance of a comprehensive treatment plan that considers both respiratory and cardiovascular risks.
The Emotional and Psychological Impact
COPD and lung hyperinflation don’t just affect the body—they also take a heavy toll on mental health. Living with constant breathlessness can be emotionally draining.
Anxiety and Breathlessness: A Vicious Cycle
- Shortness of breath often triggers panic and anxiety.
- Anxiety, in turn, makes breathing feel even more difficult, creating a self-reinforcing cycle.
- Many patients avoid physical activity out of fear, which unfortunately leads to muscle weakness and worsening symptoms.
Depression and Social Isolation
- COPD patients may feel embarrassed by constant coughing or oxygen use.
- Fatigue and limited mobility can cause withdrawal from social activities, increasing loneliness.
- Studies suggest that up to 40% of COPD patients experience clinical depression at some point.
Strategies to Manage Emotional Health
- Counseling and Therapy: Cognitive-behavioral therapy (CBT) can help break the cycle of anxiety and breathlessness.
- Support Groups: Talking to others with COPD provides emotional comfort and practical tips.
- Mindfulness Practices: Techniques like meditation and guided breathing reduce stress levels.
- Open Communication: Discussing emotional struggles with family and doctors ensures that mental health is not overlooked.
Diet and Nutrition: Fueling Your Lungs and Body
Nutrition plays a surprisingly big role in managing COPD and lung hyperinflation. What you eat can either support your lungs or make breathing harder.
Nutrients That Support Lung Function
- Protein: Essential for maintaining muscle mass, including respiratory muscles.
- Antioxidants: Found in fruits and vegetables, they reduce oxidative stress that worsens lung damage.
- Omega-3 Fatty Acids: Present in fish and flaxseed, these reduce inflammation.
- Vitamin D: Low levels are common in COPD patients and linked to worse lung function.
Foods to Embrace
- Fresh fruits and vegetables (oranges, berries, leafy greens).
- Whole grains like oats and brown rice.
- Lean proteins such as chicken, eggs, and beans.
- Healthy fats like avocados, nuts, and olive oil.
Foods to Limit or Avoid
- Processed Foods: High in salt, which can cause fluid retention and worsen heart strain.
- Carbonated Drinks: Can make bloating worse, pressing against the diaphragm and making breathing harder.
- Excess Sugar: Promotes inflammation and contributes to weight gain.
Practical Eating Tips
- Eat smaller, more frequent meals to avoid stomach bloating.
- Stay hydrated—water helps thin mucus.
- Keep healthy snacks handy to avoid energy crashes.
Exercise and Physical Activity: Moving with Confidence
Many COPD patients shy away from exercise because it seems overwhelming. Yet, staying active is one of the best ways to combat lung hyperinflation.
Why Exercise Matters
- Strengthens respiratory muscles, making breathing more efficient.
- Improves circulation, delivering oxygen more effectively.
- Boosts mood and reduces anxiety.
- Helps maintain a healthy weight, lowering strain on both lungs and heart.
Best Exercises for COPD and Hyperinflation
- Walking: A low-impact way to build endurance.
- Stationary Cycling: Improves cardiovascular fitness without overexerting.
- Light Resistance Training: Builds muscle strength in arms and legs, making daily activities easier.
- Yoga and Stretching: Promotes flexibility, relaxation, and breathing control.
Exercise Safety Tips
- Always warm up before and cool down after exercise.
- Practice breathing techniques (like pursed-lip breathing) during activity.
- Stop immediately if you feel dizzy, overly short of breath, or experience chest pain.
- Consider supervised exercise in a pulmonary rehabilitation program for added safety.
Future Outlook: Advances in COPD and Hyperinflation Treatment
The future holds promising developments in managing COPD and lung hyperinflation. Researchers are actively seeking new ways to improve lung function and reduce symptoms.
Emerging Treatments
- Endobronchial Valves: Tiny one-way valves inserted into the airways to allow trapped air to escape while preventing new air from entering damaged areas. This minimally invasive treatment is showing success in reducing hyperinflation.
- Stem Cell Research: Early studies suggest stem cells might help regenerate damaged lung tissue, though this remains experimental.
- Targeted Biological Therapies: Medications that specifically target inflammation pathways in COPD are being developed.
Digital Health Tools
- Smartphone apps and wearable devices help track breathing patterns, oxygen levels, and medication use.
- Telemedicine is making it easier for patients to stay in touch with specialists without frequent hospital visits.
Patient Empowerment and Education
- More healthcare providers are focusing on self-management education—teaching patients how to recognize early flare-ups and adjust their care accordingly.
- This approach reduces hospitalizations and empowers patients to take control of their condition.
Taking Control of Your Breathing: Living Well with COPD and Lung Hyperinflation
COPD and lung hyperinflation can make daily life feel like a constant uphill battle. The struggle to breathe, the fatigue, and the emotional weight often leave patients feeling powerless. But here’s the truth—you can regain control. While these conditions cannot be cured, they can be managed effectively with the right strategies, treatments, and lifestyle adjustments.
The key lies in understanding that COPD and hyperinflation are not just medical diagnoses; they are conditions that affect every aspect of life. From how you move, eat, and sleep to how you think and feel—everything is interconnected. Taking small but consistent steps makes a big difference.
- Stay proactive with medical care: Regular checkups, pulmonary function tests, and early treatment of flare-ups help slow disease progression.
- Make breathing strategies part of your daily life: Techniques like pursed-lip breathing and diaphragmatic breathing aren’t just therapy exercises—they’re powerful tools to help you regain control in moments of breathlessness.
- Focus on whole-body health: A balanced diet, safe exercise routine, and proper rest all contribute to stronger lungs and a healthier heart.
- Don’t neglect mental health: Anxiety and depression are as real as physical symptoms. Support groups, therapy, and mindfulness practices can lift much of the emotional burden.
Most importantly, remember that you are not alone. Millions of people around the world live with COPD and hyperinflation. Many find ways to adapt, thrive, and continue enjoying life. By working closely with your healthcare team, making positive lifestyle choices, and embracing support systems, you can breathe easier and live better.
FAQs About COPD and Lung Hyperinflation
1. Is lung hyperinflation reversible?
In most cases, lung hyperinflation caused by COPD is not fully reversible because the underlying damage to lung tissue is permanent. However, with proper treatment—such as bronchodilators, pulmonary rehabilitation, and in some cases surgical interventions—symptoms can be significantly reduced, improving both breathing efficiency and quality of life.
2. Can exercise make lung hyperinflation worse?
It’s a common concern, but the opposite is usually true. When done safely and under guidance, exercise actually helps reduce the effects of hyperinflation. It strengthens respiratory muscles, improves oxygen delivery, and builds endurance. The key is to follow a program tailored for COPD patients, often available through pulmonary rehabilitation.
3. How can I tell if my lungs are hyperinflated?
Some common signs include:
- Persistent shortness of breath, even at rest.
- Barrel-shaped chest appearance.
- Difficulty with physical activity.
- Constant fatigue despite rest.
Only a doctor can confirm hyperinflation through imaging tests (X-ray or CT scan) and pulmonary function tests. If you suspect it, seek medical evaluation early.
4. Will quitting smoking help if I already have lung hyperinflation?
Yes—quitting smoking is the single most effective step you can take, no matter how advanced your condition. While it cannot reverse existing lung damage, it slows down further progression, reduces flare-ups, and improves treatment effectiveness. Many patients notice improved breathing within weeks of quitting.
5. What’s the outlook for someone with COPD and hyperinflation?
COPD is a chronic condition, but with proper management, many people live for years—sometimes decades—after diagnosis. The outlook depends on factors like the severity of lung damage, adherence to treatment, lifestyle habits, and comorbid conditions. Staying engaged in care and making proactive lifestyle changes can dramatically improve long-term outcomes.
Final Thoughts
COPD and lung hyperinflation may feel overwhelming, but they are not a life sentence of suffering. With a deeper understanding of how these conditions work, a commitment to treatment, and the adoption of healthier habits, patients can regain control over their breathing and reclaim much of their independence.
Every breath matters—and with each proactive step, from quitting smoking to practicing pursed-lip breathing, you are giving yourself the chance to breathe a little easier tomorrow.
Medically Reviewed by Prof. Dr. Akram
Orthopedic Surgeon | Professor | Senior Medical Specialist
Prof. Dr. Akram is a distinguished surgeon with over 15 years of clinical expertise. Having served as a lead Emergency Specialist at Complex International Government Hospital, he currently leads a specialized team of 13 medical professionals at his private hospital. As a Professor at top medical universities, he ensures that every article on WellHealthOrg.com meets rigorous clinical standards.
Medical Disclaimer:
The information provided is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician for any medical concerns.
Our content is rigorously fact-checked by our 13-member Editorial Team under the clinical supervision of Prof. Dr. Akram.