Introduction: Why Eye Exams Matter More Than You Think
As we grow older, health check-ups become a routine part of life. Many of us diligently schedule visits with our primary care physicians, dentists, and sometimes even specialists. Yet, one vital aspect of health often gets overlooked — our eyes.
- Introduction: Why Eye Exams Matter More Than You Think
- What is Macular Degeneration?
- Types of Age-Related Macular Degeneration
- Symptoms of AMD
- The Role of an Optometrist in Eye Health
- How Optometrists Diagnose Macular Degeneration
- Dilated Eye Exam: The First Step
- Advanced Tests for AMD Diagnosis
- 1. Optical Coherence Tomography (OCT)
- 2. Fluorescein Angiography
- 3. Fundus Photography
- 4. Amsler Grid Test
- When Is a Referral to a Specialist Necessary?
- How Optometrists and Ophthalmologists Work Together
- Treatment Options for Macular Degeneration
- Dry AMD Treatments
- Wet AMD Treatments
- Prevention and Management Strategies
- Nutrition for Eye Health
- Lifestyle Adjustments
- Coping with Vision Loss from AMD
- Low Vision Aids
- Vision Rehabilitation
- Emotional Support
- Your Partner in Preserving Vision
- Conclusion
- Frequently Asked Questions (FAQs)
For millions of people worldwide, the slow but steady decline of vision is not simply a matter of aging. In fact, one of the leading culprits behind severe vision loss in adults over 50 is age-related macular degeneration (AMD). This progressive eye disease can quietly rob a person of their central vision, making everyday activities like reading, driving, or recognizing loved ones increasingly difficult.
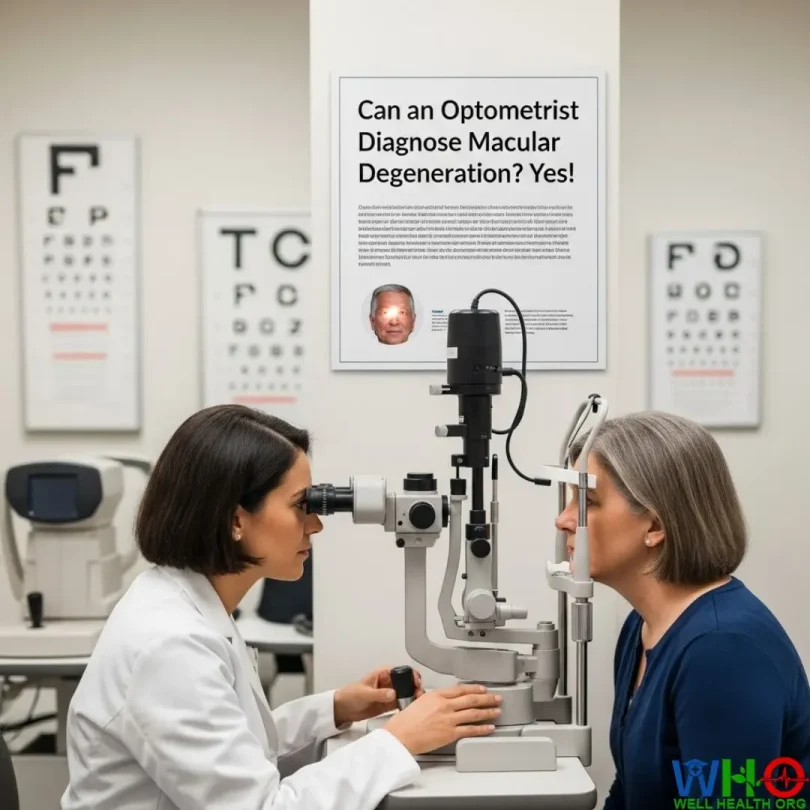
But here’s the good news: optometrists are on the front lines of AMD detection. Many people wonder, Can an optometrist really diagnose something as complex as macular degeneration? The answer is a resounding yes. With advanced training, modern diagnostic tools, and a deep understanding of eye diseases, optometrists are often the first professionals to recognize early warning signs of AMD.
In this comprehensive guide, we’ll explore:
- What macular degeneration is and how it affects your vision
- The different types and stages of AMD
- The crucial role optometrists play in diagnosing AMD
- The advanced tests used to confirm the condition
- When you might need referral to an ophthalmologist
- Lifestyle tips and treatment options to protect your eyesight
By the end, you’ll understand why regular eye exams are one of the most powerful steps you can take to safeguard your vision for years to come.
What is Macular Degeneration?
Macular degeneration, commonly known as age-related macular degeneration (AMD), is a progressive eye disease that damages the macula, a small but incredibly important part of the retina. The macula is responsible for central vision, which allows us to see fine details, read small print, and recognize faces.
When the macula begins to deteriorate, the world can suddenly look less sharp. People with AMD often describe their vision as blurry, wavy, or dim in the center of their visual field, while their peripheral (side) vision remains largely unaffected.
Types of Age-Related Macular Degeneration
There are two main forms of AMD, and understanding the difference is key to understanding both diagnosis and treatment.
1. Dry AMD (Atrophic AMD)
- This is the most common form, accounting for about 80–90% of AMD cases.
- It develops gradually over several years.
- The condition occurs as the macula thins with age, and drusen — tiny yellow protein deposits — build up under the retina.
- AMD progresses through three stages:
- Early stage: No noticeable symptoms, but drusen are present.
- Intermediate stage: Mild vision changes, such as needing more light to read or difficulty seeing in dim environments.
- Late stage: Central vision becomes significantly blurry, faded, or distorted.
2. Wet AMD (Neovascular AMD)
- Less common but far more aggressive and severe.
- Occurs when abnormal blood vessels grow beneath the retina.
- These vessels can leak blood or fluid, causing rapid damage and scarring of the macula.
- Vision loss from wet AMD can occur suddenly and worsen quickly if untreated.
- Importantly, any stage of dry AMD can suddenly advance to wet AMD.
Symptoms of AMD
One of the challenges with AMD is that symptoms may not appear until the disease is already progressing. Still, being aware of early warning signs can make a life-changing difference.
Common symptoms include:
- Blurred or fuzzy central vision
- Straight lines appearing wavy or distorted (known as metamorphopsia)
- A central dark or blank spot in vision
- Difficulty recognizing faces
- Trouble adapting to low light conditions
- Colors appearing less vibrant
It’s worth noting that in the early stages, AMD may have no symptoms at all. This is why routine eye exams are so critical.
The Role of an Optometrist in Eye Health
Optometrists are often thought of simply as “the doctors who prescribe glasses.” While vision correction is certainly part of their work, their role goes far deeper.
An optometrist is a primary eye care provider trained to:
- Perform comprehensive eye exams
- Diagnose and manage a wide range of eye diseases, including AMD, glaucoma, and diabetic retinopathy
- Prescribe medications for certain eye conditions
- Monitor eye health over time
- Co-manage care with ophthalmologists when surgical or advanced treatments are needed
For adults over 50 — and especially those over 65 — annual comprehensive eye exams are strongly recommended. These visits allow optometrists to catch silent eye diseases like AMD before vision loss becomes noticeable.
During a routine exam, an optometrist doesn’t just check your prescription. They carefully examine the internal structures of your eyes, evaluating the retina, macula, optic nerve, and blood vessels. This holistic approach makes them well-positioned to spot the earliest warning signs of AMD.
How Optometrists Diagnose Macular Degeneration
Yes, an optometrist can absolutely diagnose macular degeneration. The process usually starts during a dilated eye exam.
Dilated Eye Exam: The First Step
- Special eye drops are used to widen the pupils.
- This dilation allows the optometrist to get a clear, unobstructed view of the retina and macula using high-powered lenses and lights.
- The doctor looks for:
- Presence of drusen (yellow deposits under the retina)
- Signs of macular thinning
- Abnormal blood vessels or leakage (potential wet AMD)
- Pigmentary changes in the retina
If AMD is suspected, the optometrist may order or perform additional diagnostic tests to confirm the stage and type of the disease.
Advanced Tests for AMD Diagnosis
Optometrists have access to advanced imaging and testing tools that provide precise information about the retina and macula. Here are the most commonly used:
1. Optical Coherence Tomography (OCT)
- A non-invasive imaging technique that uses light waves to capture detailed, cross-sectional images of the retina.
- Think of it like an “ultrasound for the eye,” but with light instead of sound.
- OCT can detect subtle changes in retinal layers, swelling, or fluid buildup — crucial for distinguishing between dry and wet AMD.
- The test is quick, painless, and typically takes 5–10 minutes.
2. Fluorescein Angiography
- Often used when wet AMD is suspected.
- A fluorescent dye (fluorescein) is injected into a vein in your arm.
- As the dye circulates through the retinal blood vessels, a special camera captures images.
- This allows the doctor to see leaky or abnormal vessels, a hallmark of wet AMD.
3. Fundus Photography
- High-resolution images of the back of the eye help document changes in the retina and macula over time.
- These photos act like a visual “health record” for monitoring progression.
4. Amsler Grid Test
- A simple, at-home tool patients can also use.
- It looks like a grid of straight lines with a central dot.
- Patients focus on the dot and report if lines look wavy, blurry, or missing.
- Even subtle distortions can indicate changes in macular function.
When Is a Referral to a Specialist Necessary?
Optometrists are highly trained to detect and monitor macular degeneration, but in some cases, specialized treatment is required. That’s where ophthalmologists — medical doctors specializing in eye surgery and advanced care — come in.
An optometrist will typically refer a patient to an ophthalmologist if:
- Wet AMD is suspected or confirmed: Because this form progresses rapidly, immediate intervention is crucial.
- Late-stage dry AMD is present: While treatment options are limited, specialists may recommend clinical trials, vision rehabilitation, or advanced monitoring.
- Sudden changes in vision occur: Such as a sudden blind spot, rapid distortion of vision, or sudden darkening of central vision.
How Optometrists and Ophthalmologists Work Together
The collaboration between optometrists and ophthalmologists is essential. An optometrist often acts as the first line of defense, detecting AMD during routine exams and managing follow-up care. When intervention such as injections or surgery is needed, an ophthalmologist steps in. Afterward, the optometrist often continues long-term monitoring, ensuring continuity of care.
This co-management model ensures that patients receive both personalized primary eye care and specialized treatment when necessary.
Treatment Options for Macular Degeneration
While there is currently no cure for macular degeneration, treatments can slow progression, preserve vision, and improve quality of life. The type of treatment depends on whether the patient has dry AMD or wet AMD.
Dry AMD Treatments
For dry AMD, treatment primarily focuses on slowing progression and maintaining eye health.
1. Nutritional Supplements (AREDS & AREDS2 Formulas)
- Clinical studies such as the Age-Related Eye Disease Studies (AREDS and AREDS2) showed that a specific combination of vitamins and minerals can slow the progression of intermediate to advanced dry AMD.
- Recommended supplement ingredients include:
- Vitamin C
- Vitamin E
- Zinc
- Copper
- Lutein
- Zeaxanthin
2. Lifestyle Modifications
- Eating a diet rich in leafy greens (spinach, kale), fish high in omega-3 fatty acids, nuts, and colorful fruits supports retinal health.
- Stopping smoking immediately is critical — smoking is one of the strongest risk factors for AMD progression.
- Managing blood pressure and cholesterol levels helps protect retinal blood vessels.
- Regular exercise improves circulation and supports overall eye health.
Wet AMD Treatments
Wet AMD is more aggressive, but modern medicine has made tremendous advances in treating it.
1. Anti-VEGF Injections
- VEGF stands for vascular endothelial growth factor — a protein that promotes the growth of abnormal blood vessels.
- Anti-VEGF medications (such as Lucentis, Eylea, and Avastin) block VEGF, reducing leakage and slowing vision loss.
- These injections are administered directly into the eye (painless with anesthetic drops) and repeated every 4–8 weeks depending on progress.
- Many patients experience stabilization of vision, and some even regain clarity.
2. Photodynamic Therapy (PDT)
- A light-sensitive drug is injected into the bloodstream.
- A special laser activates the drug in the eye, destroying abnormal blood vessels without damaging healthy tissue.
- PDT is less common today but may still be used in select cases.
3. Laser Surgery
- High-energy laser beams are sometimes used to seal leaky vessels.
- This treatment is less common now, as it can also damage healthy retinal tissue.
Prevention and Management Strategies
Even though AMD can’t be cured, you can reduce your risk and slow its progression by adopting smart habits and lifestyle changes.
Nutrition for Eye Health
A healthy diet plays a critical role in maintaining retinal function. Nutrients known to protect eye health include:
- Leafy Greens: Spinach, kale, and collard greens provide lutein and zeaxanthin.
- Fatty Fish: Salmon, tuna, and mackerel are rich in omega-3 fatty acids.
- Colorful Fruits and Vegetables: Carrots, peppers, and oranges contain vitamin C and beta-carotene.
- Nuts and Seeds: Almonds, walnuts, and sunflower seeds provide vitamin E and healthy fats.
Think of this as eating a “rainbow diet” — the more variety of colors on your plate, the better for your eyes.
Lifestyle Adjustments
- Quit Smoking: Smoking increases AMD risk by 2–4 times. Quitting is the single most effective step you can take.
- Exercise Regularly: Physical activity improves circulation, ensuring your retina gets the oxygen and nutrients it needs.
- Maintain Healthy Blood Pressure and Cholesterol: Cardiovascular health is directly linked to eye health.
- Wear Sunglasses: Protecting your eyes from harmful UV light can help preserve macular health.
- Monitor Vision at Home: Using an Amsler grid once a week can help detect subtle changes in central vision early.
Coping with Vision Loss from AMD
For individuals with advanced AMD, coping strategies can make daily life easier and help maintain independence.
Low Vision Aids
- Magnifiers: Handheld or stand magnifiers make reading easier.
- Large-Print Books & Devices: Many resources are now available in larger fonts.
- Electronic Aids: Tablets and e-readers allow customizable text size.
- Screen Readers: Technology that reads text aloud for those with severe vision loss.
Vision Rehabilitation
- Specialized training helps patients use their peripheral vision more effectively.
- Occupational therapists can suggest adjustments at home, such as improved lighting, high-contrast markings, and organization systems.
Emotional Support
Vision loss can take a toll on mental health. Support groups, counseling, and connecting with others experiencing AMD can reduce feelings of isolation and frustration.
Your Partner in Preserving Vision
So, can an optometrist diagnose macular degeneration? Yes — and often, they are the first to detect it. Optometrists are not only trained to recognize the early signs of AMD but also play a central role in its ongoing management.
By scheduling regular comprehensive eye exams, especially after age 50, you give yourself the best chance of catching AMD before it causes irreversible damage. And if advanced treatment is needed, your optometrist will refer you to the right specialist while remaining an active partner in your care.
The key message is clear: Don’t wait until symptoms appear. By the time you notice vision loss, AMD may already be advanced. Proactive care — through regular exams, healthy lifestyle choices, and timely treatment — is your best defense.
Conclusion
Macular degeneration may be one of the leading causes of vision loss worldwide, but early detection changes everything. Optometrists are fully equipped to diagnose AMD, monitor its progression, and guide patients toward effective treatments and preventive strategies.
Protecting your eyesight isn’t just about getting new glasses when things get blurry — it’s about maintaining the health of your eyes throughout life. By working hand in hand with your optometrist and making smart lifestyle choices, you can give your eyes the best chance of staying sharp and clear well into your later years.
Don’t put off your eye exam — your future vision depends on it.
Frequently Asked Questions (FAQs)
1. How often should I see an optometrist if I’m over 50?
Experts recommend a comprehensive eye exam every 1–2 years, but annually is best for adults over 65 or those with risk factors like family history or smoking.
2. Can AMD be reversed once it develops?
No. Current treatments can slow or stop progression and, in some cases, improve vision slightly, but they cannot restore vision already lost.
3. What is the difference between an optometrist and an ophthalmologist?
An optometrist provides primary eye care, diagnoses conditions, and manages ongoing care. An ophthalmologist is a medical doctor who performs surgeries and advanced treatments for eye diseases.
4. If AMD runs in my family, what can I do to reduce my risk?
Adopt a healthy lifestyle: don’t smoke, eat a nutrient-rich diet, exercise regularly, protect your eyes from UV rays, and keep up with yearly eye exams.
5. Is macular degeneration painful?
No, AMD does not cause pain. The main symptom is gradual or sudden vision loss, particularly in the central field of vision.
Medically Reviewed by Prof. Dr. Akram
Orthopedic Surgeon | Professor | Senior Medical Specialist
Prof. Dr. Akram is a distinguished surgeon with over 15 years of clinical expertise. Having served as a lead Emergency Specialist at Complex International Government Hospital, he currently leads a specialized team of 13 medical professionals at his private hospital. As a Professor at top medical universities, he ensures that every article on WellHealthOrg.com meets rigorous clinical standards.
Medical Disclaimer:
The information provided is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician for any medical concerns.
Our content is rigorously fact-checked by our 13-member Editorial Team under the clinical supervision of Prof. Dr. Akram.